Journal of Otolaryngology and Rhinology
Laryngeal Tuberculosis: About 3 Cases from Morocco
Abou-elfadl M*, Benzaouia A, Abada R, Rouadi S, Roubal M and Mahtar M
Department of Otorhinolaryngology and Neck Surgery, 20August Hospital, Casablanca, Morocco
*Corresponding author:
Dr. Abou-elfadl Maryame, Resident of the Otorhinolaryngology and Neck Surgery department, 20August Hospital, PO Box 9619 Moulay Rchid, Casablanca, Morocco, Tel: +212-6679-32692, E-mail: maryameabouelfadl@gmail.com
J Otolaryngol Rhinol, JOR-2-026, (Volume 2, Issue 4), Clinical Study
Received: July 25, 2016; Accepted: November 30, 2016; Published: December 03, 2016
Citation: Abou-elfadl M, Benzaouia A, Abada R, Rouadi S, Roubal M, et al. (2016) Laryngeal Tuberculosis: About 3 Cases from Morocco. J Otolaryngol Rhinol 2:026.
Copyright: © 2016 Abou-elfadl M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Summary
Introduction: Tuberculosis is a public health problem in developing countries; pulmonary localization is the most common and contagious. Laryngeal localization is rare; it can be primary or secondary often.
Materials and methods: Presents three cases of laryngeal tuberculosis revealed by atypical clinical and endoscopic tables, of which only the histology was confirmed diagnosis.
Discussion: Laryngeal tuberculosis (TL) is often taken for laryngeal cancer or a specific or nonspecific laryngitis, which delayed diagnosis, a source of danger for the health public because of the contagiousness. Only histology confirms the diagnosis and allows initiating adapted antituberculosis drugs treatment that ensures healing.
Keywords
Dysphonia, Tuberculosis, Larynx, Biopsy, Antituberculosis drugs
Introduction
The laryngeal tuberculosis incidence decreased significantly since the development of antituberculosis drugsand early detection of new cases. Currently, it represents less than 1% of cases of extrathoracic tuberculosis. As tuberculosis is endemic in Morocco, we continue to see this rare localization. Its clinical presentation is atypical and endoscopic aspects are polymorphic, hence the difficulty of diagnostic. The aim of the study is to report three different observations of the laryngeal localization of tuberculosis.
Materials and Methods
We collected during the year 2014, 3 cases of laryngeal tuberculosis diagnosed in service and treated in the specialized center for tuberculosis.
Results
Observation n°1: laryngeal tuberculosis revealing a miliary tuberculosis
A thirty year old male, 10 pack year smoking, presented a chronic dysphonia, isolated, without cough or dyspnea, or dysphagia with weight loss notion.
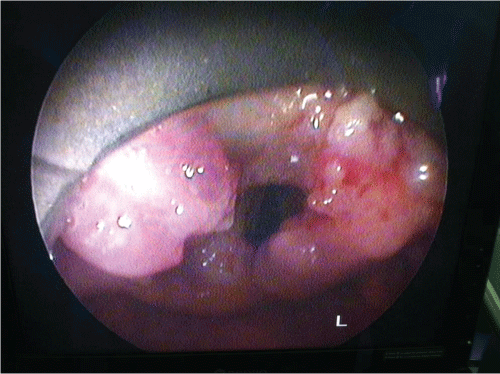
Clinical examination revealed, in nasofibroscopie, tumor in the larynx. There was no neck stiffness or enlarged lymph nodes or signs of meningeal irritation or localising neurological deficit. Chest radiography revealedwide spread small (2-4 mm) nodular opacities distributed throughout both lungs (Figure 1). Direct laryngoscopy revealed a tumor taking all the epiglottis, the two ventricular bands and the two arytenoid (Figure 2), the piriform sinus, the sub-glottis and esophageal mouth are free, basic language is flexible. The biopsy with histological examination revealed chronic inflammation with epithelioid granuloma giant cell without necrosis.
.
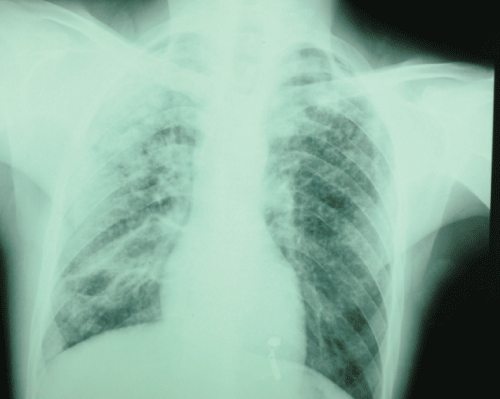
Figure 1: Chest radiography revealed wide spread nodular opacities distributed throughout both lungs.
View Figure 1
The assessment completed by a cervicothoracic scanner that shows a glotto-sus-glottic tumor associated with macronodules of both lung fields (Figure 3). The tuberculin skin test (TST) and search of Mycobacterium tuberculosis (BK) in sputum were positive.The patient hasanantibacillaire treatment in specialized center for tuberculosis with monitoring and testing the entourage.
.
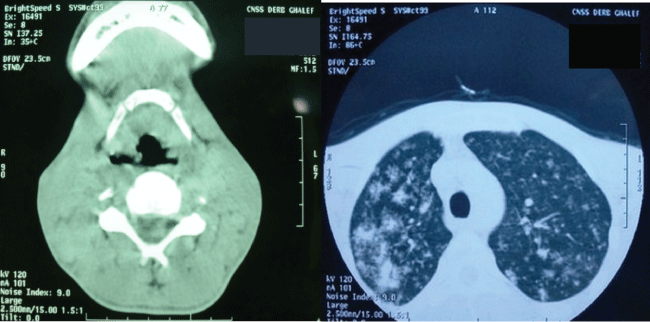
Figure 3: Cervicothoracic scanner that shows a glotto-sus-glottic tumor associated with macronodules of both lung fields.
View Figure 3
Observation n°2: isolated laryngeal tuberculosis
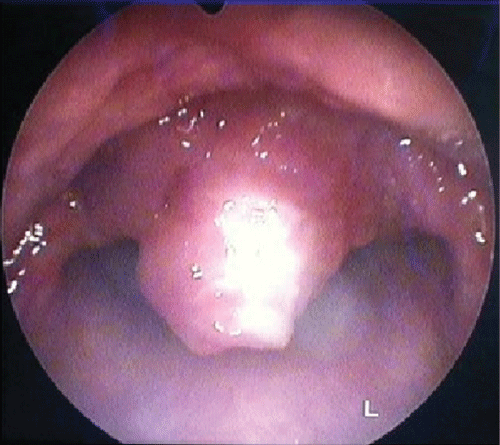
Forty six years old male, 12 pack year smoking and chronic alcoholic, consults for isolated and permanent dysphonia, evolving since 9 months, in a context of impaired general condition. We found in nasofibroscopie an irregular and inflammatory laryngeal mucosa. There was no cervical lymphadenopathy or other defects.
Direct laryngoscopy showed an irregular and inflamed aspect of laryngeal mucosa, ventricular band, epiglottis and arytenoid. The biopsy with histological examination revealed chronic inflammation with epithelioid granuloma giant cell without caseous necrosis. The TST was positive (20 mm), the chest radio was normal and 3 sputum BK were negatives. The patient has anantibacillary treatment.The lesions was completely regressed.
Observation 3: Concomitant laryngeal and pulmonary tuberculosis
Forty one years old male, 30 pack years smoking, consulted for dysphagia, dysphonia, and a productive cough evolving for three months in a context of fever, night sweats and weight loss without dyspnea. Clinical examination found a febrile patient with bilateral lung sounding rales and swelling at the level of the epiglottis in Nasofibroscopy (Figure 4). There was no neck enlarged lymph nodes. Chest radiography showed a bilateral interstitial infiltrate, TST and 3BKsputum were positives.
Direct laryngoscopy objectified a lesion in the epiglottis which biopsies were incomes for a gaseous necrosis tuberculosis of larynx. A quadruple tuberculosis is introduced in specialized center. The outcome was favorable with regression of symptoms, negativity of Koch’s Bacillus sputum and disappearance of laryngeal lesions.
Discussion
Laryngeal tuberculosis (LT) is a specific chronic laryngitis caused by mycobacterium tuberculosis. Centers for Disease Control and Prevention ranked laryngeal TB as "a highly contagious form of tuberculosis, including erosive and exudative invasion of the larynx" [1].
LT represents 1% of all TB localizations [2] and the most common location in the ENT [3]. It can be seen at any age, but especially in young adults between 20 and 50 years [2].
Tuberculosis is an airborne disease, transmitted from person to person. Koch's bacillus can reach the larynx by two differents ways: directly from the external environment, realizing the primary laryngeal tuberculosis or indirectly from another focus and realizing the secondary laryngeal tuberculosis [1,3].
Clinically, it is difficult to differentiate tuberculosis and malignant tumors of the larynx [2,3]. The symptoms are atypical: hoarseness, weight loss, fatigue, persistent dry cough, fever, sweats, and sleep apnea, in an often chronic alcohol and tobacco subject [2].
In the literature, no asphyxiant form has been described justifying resuscitation measures such as intubation or a tracheostomy [4]. Physical examination may find cervical lymph nodes in 10% of cases [5]. Laryngoscopy are also contributive, with an aspect that may primarily evoke cancer or chronic laryngitis, but also other granulomatous diseases such as syphilis, sarcoidosis, Wegener's granulomatosis [2,3,5-7].
Gallasand, et al. study show that the laryngeal tuberculosis is essentially glottic with a predominant involvement of the vocal cords (64.8% of cases) followed by vestibular folds (34.9% cases) [5]. According to Lim et al, the proportions were 46 and 18% respectively [5].
More rarely, tuberculous granulomas concern the arytenoid, the posterior commissure and epiglottis [5].
Once the diagnosis is confirmed by histological and bacteriological studies, the search for other focus point of tuberculosis, especially lung disease. The adequate management and startingantituberculosis drugs ensure healing without sequelae [4,5] (Table 1).
![]()
Table 1: Different cases of laryngeal tuberculosis from the literature.
View Table 1
Conclusion
Laryngeal tuberculosis is rare. Often it is not isolated and can sometimes reveal clinically unrecognized pulmonary tuberculosis. A few specific symptoms and endoscopic semiology can refer to wrongly malignancy until bacteriological results. The latest techniques of cultivation and genomic diagnostics allow rapid diagnosis of tuberculosis. The standard tuberculosis treatment allows complete mucosal healing of the larynx and quickly stops any risk of human transmission.
References
-
Hans L Rieder (2009) La contagiosite de la tuberculose laryngee: action de sante publique appropriee basee sur des premices inexactes. Int J Tuberc Lung Dis 13: 4-5.
-
Mandal A, Ray S, Ganguly (2014) Study to evaluate clinicopathological profile of laryngeal tuberculosis. BBB 2: 742-747.
-
Bhuyan N, Das AK (2014) Primary laryngeal tuberculosis: a rare cause of chronic laryngitis. Int J Adv Med 1: 279-281.
-
Margery J, Grassin F, Lecoules S, Dot JM, Guigay J, et al. (2004) Atteinte laryngée révélatrice d’une tuberculose pulmonaire méconnue. Rev Pneumol Clin 60: 39-42.
-
Saroul N, Vellin JF, Baud O, Nohra O, Kemeny JL, et al. (2008) Tuberculose epilaryngée: considérations épidémiologiques, cliniques et sanitaires, annales d'otolaryngologie et chirurgie cervico-faciale. 125: 155-159.
-
Kumar A, Singh DK, Arpit S, Singha S (2014) Tubercular Laryngitis Simulating Laryngeal Carcinoma. J Pulm Respir Med 5.
-
Chen HK, Thornley P (2012) Laryngeal tuberculosis: A case of a non-healing laryngeal lesion. Australas Med J 5 : 175-177.