Journal of Otolaryngology and Rhinology
Eosinophilic Airway Inflammation: The Effectiveness of Nasal Steroids
Peirolo Anna1*, Simoncini Daniela1, Macchi Alberto2, Graziani Daniela1, Porcu Stefania1 and Nespoli Luigi1
1Department of Clinical and Experimental Medicine, University of Insubria c/o Ospedale Filippo del Ponte, Varese, Italy
2Otorhinolaringology Clinic University of Insubria Varese, AICNA, c/o Ospedale di Circolo, Varese, Italy
*Corresponding author:
Dr. Peirolo Anna, Department of Clinical and Experimental Medicine, University of Insubria c/o Ospedale Filippo del Ponte, Varese, via Cristoforo Colombo 10, 22077 Olgiate Comasco, COMO, Italy, E-mail: anna.peirolo@hotmail.it
J Otolaryngol Rhinol,
JOR-1-009, (Volume 1, Issue 2),
Research Article
Received: November 23, 2015: Accepted: December 22, 2015: Published: December 24, 2015
Citation: Anna P, Daniela S, Alberto M, Daniela G, Stefania P, et al. (2015) Eosinophilic Airway Inflammation: The Effectiveness of Nasal Steroids. J Otolaryngol Rhinol 1:009
Copyright: © 2015 Anna P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background:An increasing proportion of patients have coexisting upper and lower airway disease. Therefore, the historic perspective of these allergen-induced disorders as distinct and separate entities is being displaced by current thinking that they are better described as a continuum of inflammation involving one common airway [1].
Objectives:The aim of this study was to investigate the role that upper airway inflammation and therapy plays on lower airway situation.
Methods:This study was performed on 84 children, aged 4 to 17 years, with asthma with/without rhinitis. Skin prick-test, FeNO (fractional exhaled nitric oxide) and nasal cytology were analyzed in all patients; upper and lower airways symptomatology was assessed by ACT or C-ACT (Asthma Control Test; Childhood Asthma Control Test) and SNOT (Sino Nasal Outcome Test) questionnaires [Appendix A].
To examine the direct effect of rhinitis therapy on lower airway inflammation, all these tests were performed before and after treatment with oral antihistamines and nasal steroids (Fluticasone).
Results:The study group consisted of 84 children, 72 allergic and 12 non-allergic patients; 26 children with asthma and 58 children with asthma and rhinitis. FeNO was higher in subjects with asthma and rhinitis than in asthmatic patients without rhinitis. In all subjects, atopic sensitization and nasal eosinophilia were associated with elevated FeNO levels. Nasal corticosteroids improved severity of rhinitis and asthma symptoms and insignificantly reduced FeNO and upper airway inflammation.
Conclusions:Asthma and rhinitis are different manifestations of a common pathogenic phenomenon; therefore treatments for one condition could potentially alleviate the coexisting disease.
Keywords
Asthma, Eosinophilic airway inflammation, FeNO, Nasal steroids, Nasal cytology, Rhinitis
Abbreviations
FeNO: fractional exhaled nitric oxide, eNO: exhaled nitric oxide, ACT: Asthma Control Test, C-ACT: Childhood Asthma Control Test, SNOT: Sino Nasal Outcome Test, DPP: Dermatophagoides pteronyssinus, DPF: Dermatophagoides farina, ppb: parts per billion, E: eosinophils, M: mast-cells, EM: eosinophils and mast-cells, ALL: allergic children, NON-ALL: non-allergic children
Main Text
The prevalence of asthma and rhinitis is on the increase and these conditions are frequently associated, thus leading to the concept that these two conditions are different aspects of the same disease: "one airway, one disease" [2]. Most of patients with allergic (80%) and non-allergic asthma (75%) have concomitant rhinitis, while, approximately 34% of patients with allergic rhinitis and 25% of patients with non-allergic have concomitant asthma [2,3]. Although upper and lower airway diseases commonly occur together, clinicians have yet to determine the exact nature of the association between these two chronic conditions and to test the hypothesis that treating rhinitis reduces health care utilization for co-morbid asthma [4].
In the present study, we used FeNO and nasal cytology to investigate upper and lower airway inflammation and the clinical benefits of nasal treatment in children with asthma.
Methods and Study Population
Study population
A total of 84 patients, 4-17 years of age, 53 males and 31 females, coming from the allergology outpatient "Filippo del Ponte", were clinically examined from 1 November 2013 to 31 July 2014. All participants were interviewed about respiratory symptoms thanks to ACT (Asthma Control Test) or C-ACT (Childhood-Asthma Control Test) and SNOT (Sino-Nasal Outcome Test); lung function and airway inflammation were measured using HyPAIR FeNO and nasal cytology in children free of treatment (systemic antihistamine and/or nasal steroids) for at least 10 days' time.
Furthermore the allergic sensitization to common aeroallergens (birch, core, olive tree, grasses, ragweed, parietaria, dog, cat, house dust mite: DPP and DPF1, mould: alternaria) and foods (cow lactalbumin, cow casein, egg white and yolk, peanuts) was evaluated by skin prick-test and used to classify patients in two groups: allergic (72, 47 males and 25 females) and non-allergic (12, 6 males and 6 females). Histamine hydrochloride, 10 mg/mL, and phenolated glycerol-saline served as positive and negative controls. The reaction was regarded as positive if the mean wheal diameter was at least 3 mm greater than negative control [5].
1DPP: Dermatophagoides pteronyssinus, DPF: Dermatophagoides farinae
In order to investigate if a rigorous treatment of upper airway, could result in less lower airway inflammation, 38 of patients were treated with nasal saline (NaCl 0.9%) while, 46 with nasal Fluticasone. At the end of 2 months treatment, 70 of children coming to the follow-up were evaluated from the same tests completed during the first visit.
Methods
Study design and participants:A stratified (by gender, age, allergies, clinician diagnosis and ongoing therapy), multistep defined sample was used. In a first phase, the inclusion criteria of participants were defined:
1. Subjects previously diagnosed with asthma, with or without rhinitis, by allergists
2. Subjects aged 4 or above
3. Children with positive skin-prick tests
4. Children free of treatment (systemic antihistamine and/or nasal steroids) for at least 10 days' time
In a second phase, patients were assigned into one of the 4 therapy groups (ongoing therapy due to subject's diseases): leukotriene antagonists, inhaled corticosteroids, leukotriene antagonists and inhaled corticosteroids, no therapy.
In the final phase, considering the sensitization to different allergens as well, each of the participants in the 4 groups was randomly assigned into one of two study arms, including nasal saline or nasal steroids group.
FeNO: FeNO is recognized as a reliable surrogate marker of airway inflammation and offers the advantage of being completely non-invasive and very easy to obtain [6].
According to the study by Buchvald et al. [7] we report that the upper normal level (no airway inflammation) of FeNO in children from 4 to 17 years ranges from 15 ppb (parts per billion) in the young children to 25 ppb in adolescents; FeNO was higher in patients with airway inflammation.
FeNO was measured by using the online single breath method with HyPAIR FeNO according to ERS/ATS guidelines.
The subject seated comfortably and with the nose clip, inserted the mouthpiece and inhaled NO-free air to total lung capacity over a period of 2 to 3 seconds through the mouthpiece of the instrument. The subject then started exhalation with a flow rate of 50 ml/sec. Children younger than 10 years performed a 6-second exhalation, and FeNO was calculated during the last 2 seconds of the exhalation. Children ≥ 10 years performed an exhalation of 10 seconds, and FeNO was calculated during the last 3 seconds of the exhalation. FeNO values were recorded if the reliability index was higer than 60%. Each subject performed no more than a total of 6 exhalations. The interval between exhalations was at least 30 seconds. FeNO was calculated as the mean of 3 correct exhalations. All measurements were performed in parts per billion (ppb) [8,9].
Nasal cytology: Nasal cytology represents a valid method in the diagnosis of nasal inflammation as it is easy to perform, non-invasive, and able to detect both the cellular modification of the nasal epithelium caused by either allergen exposure or irritative stimuli or inflammation. Such a consideration suggests the quality of a systemic use of nasal cytology in the diagnostic work-up of upper and lower airways disorders, in order to reach a proper defined diagnosis and to study the airway inflammation: the diagnosis of nasal disorders through nasal cytology is based on the consideration that, in healthy subjects, the nasal mucosa is composed of 4 normal subsets of cells, which commonly characterize the pseudo-stratified epithelium; besides neutrophils, no other cells are detected in healthy individuals. Therefore, on a rhinocytogram, the presence of eosinophils, mast cells, bacteria, spores and fungi has to be considered as a clear sign of nasal pathology.
In our study, nasal cytology was assessed in all patients, free of treatment (systemic antihistamine and/or nasal steroids) for at least 10 days' time, using these following steps:
• Sampling and processing: scraping the middle portion of the inferior turbinate by using Rhino-probe; placed the material on a glass slide, fixed by air drying and stained by May-Grünwald-Giemsa method.
• observation through a light microscopy able to magnify up to 1000x
For the rhinocytogram analysis, the slide, divided into 10 microscopic fields, have to be read in order to detect eosinophils, mast cells, neutrophils, bacteria, spores and calculate their percentages comparing to the number of total leukocytes (Table 1).
![]()
Table 1: Rhinocytogram analysis.
View Table 1
Statistical analysis: Frequencies were calculated for the entire study group and differences were assessed by chi-squared tests for categorical data and by t-tests for normally distributed data. Logistic regression analysis with backward elimination was performed with FeNO as the dependent variable. Demographics variable (age, sex and BMI), concurrent rhinitis, exposure to allergens and medication taken within the last 4 weeks (inhaled corticosteroids and leukotriene antagonists) were included as independent variables in the model [10,11]. A P-value < 0.05 was considered to be statistically significant.
Results
According to the clinician diagnosis, 58 of children were affected by asthma and rhinitis (53 allergic patients and 5 non-allergic patients), 26 of children by asthma (19 allergic subjects and 7 non-allergic subjects).
Among asthmatic patients, 16% of subject was monoallergic (33% female and 67% male), while 84% was polyallergic (19% female and 81% male).
Among children with asthma and rhinitis, 8% of patient was monoallergic (25% female and 75% male), while 92% was polyallergic (41% female and 59% male) (Table 2).
![]()
Table 2: Distribution of the study population.
View Table 2
Nasal cytology before and after treatment
To examine the direct effect of rhinitis therapy on upper airway inflammation, nasal cytology was performed before and after treatment in 2 groups of patients: one (34 subjects) treated with topical nasal saline and the other one (36 subjects) with topical nasal steroids (Fluticasone).
• In 70% of allergic children and 67% of non-allergic children treated with Fluticasone, nasal inflammation was absent or lower than before therapy. The same result was obtained in 12% of allergic children treated with saline (Table 3a and Table 3b).
![]()
Table 3a: Nasal cytology before and after treatment with nasal steroid (Fluticasone).
View Table 3a
![]()
Table 3b: Nasal cytology before and after treatment with nasal saline (NaCl 0, 9%).
View Table 3b
• 10% of allergic subjects treated with nasal steroids showed no differences in upper airway inflammation before and after treatment. The same result was recorded in 24% of allergic and 40% of non-allergic subjects treated with saline (Table 3a and Table 3b).
• In 20% of allergic children and 33% of non-allergic children treated with Fluticasone, nasal inflammation was higher than before therapy. The same result was obtained in 64% of allergic and 60% of non-allergic children treated with saline (Table 3a and Table 3b).
FeNO and nasal cytology before treatment
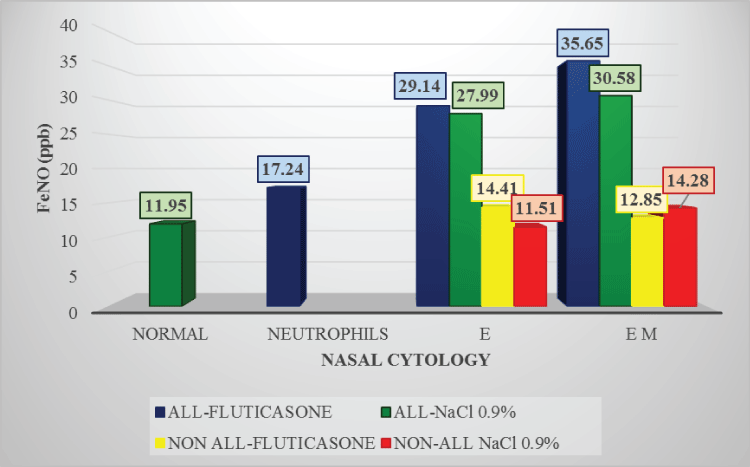
In general, patients with eosinophils, with or without mast cells, had higher FeNO levels compared with other patients (Figure 1a). In subgroup with eosinophils, FeNO levels (ppb) were associated with the increase of nasal inflammation (Figure 1b).
.
Figure 1a: FeNO levels in rhinitis before treatment
FeNO in allergic children without inflammation: 11.95ppb in allergic children subsequently treated with NaCl 0.9% (ALL-NaCl 0.9%);
FeNO in allergic patient with neutrophils: 17.24ppb in the allergic patient subsequently treated with Fluticasone (ALL-FLUTICASONE);
FeNO in children with eosinophils: 29.14ppb in allergic (ALL-FLUTICASONE) and 14.41ppb in non-allergic children subsequently treated with Fluticasone (NON ALL-FLUTICASONE); 27.99ppb in allergic (ALL-NaCl 0.9%) and 11.51 in non-allergic children subsequently treated with NaCl 0.9% (NON ALL-NaCl 0.9%);
FeNO in patients with eosinophils and mast cells: 35.65ppb in allergic (ALL-FLUTICASONE) and 12.85ppb in non-allergic patients subsequently treated with Fluticasone (NON ALL-FLUTICASONE); 30.85ppb in allergic (ALL-NaCl 0.9%) and 14.28 in non-allergic patients subsequently treated with NaCl 0.9% (NON ALL-NaCl 0.9%);
View Figure 1a
.
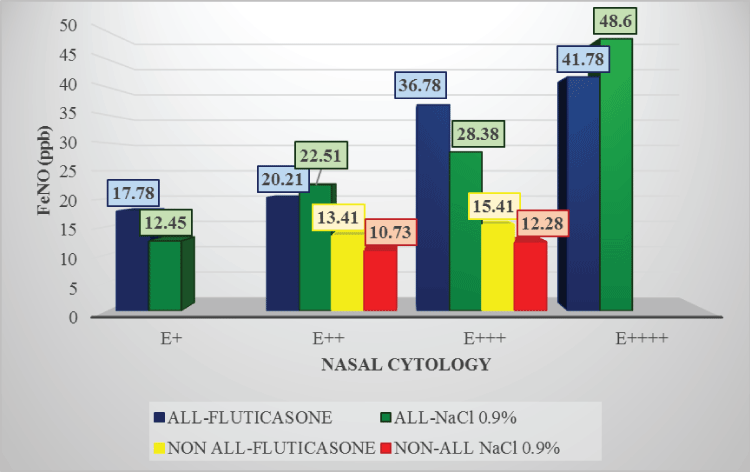
Figure 1b: FeNO levels in children with nasal eosinophils before treatment
FeNO in allergic children with eosinophils + : 17.78ppb in allergic children subsequently treated with Fluticasone; 12.45ppb in the allergic child subsequently treated with NaCl 0.9%;
FeNO in patients with eosinophils ++ : 20.21ppb in allergic patients and 13.41ppb in the non-allergic patient subsequently treated with Fluticasone; 22.51ppb in allergic and 10.73 in non-allergic patients subsequently treated with NaCl 0.9%;
FeNO in subjects with eosinophils +++ : 36.78ppb in allergic and 15.41ppb in non-allergic subjects subsequently treated with Fluticasone; 28.38ppb in allergic subjects and 12.28 in the non-allergic subject subsequently treated with NaCl 0.9%;
FeNO in allergic children with eosinophils ++++ : 41.78ppb in allergic children subsequently treated with Fluticasone; 48.6ppb in the allergic child subsequently treated with NaCl 0.9%;
View Figure 1b
FeNO and nasal cytology after treatment
.
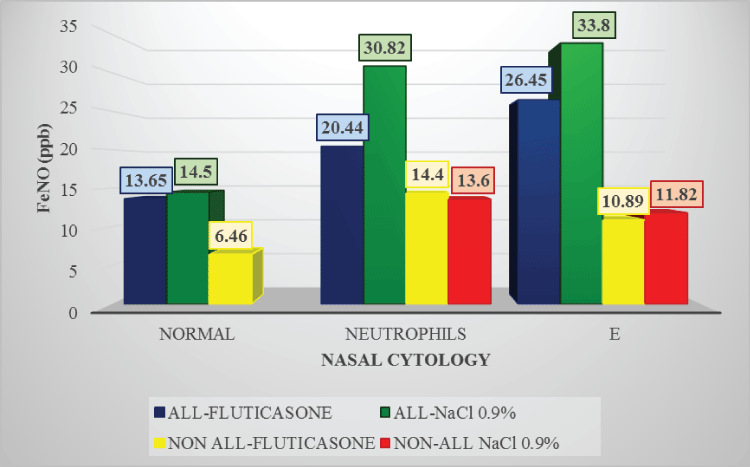
Figure 2a: FeNO levels in rhinitis after treatment
Children treated with Fluticasone:
FeNO in patients without inflammation: 13.65ppb in allergic and 6.46ppb in non-allergic patients.
FeNO in children with eosinophils: 20.44ppb in allergic and 14.4ppb in non-allergic children;
FeNO in patients with eosinophils and mast cells: 26.45ppb in the allergic patient and 10.89ppb in non-allergic patients.
Children treated with NaCl 0.9%:
FeNO in patients without inflammation: 14.5ppb in allergic patients.
FeNO in subjects with eosinophils: 30.82ppb in allergic and 13.6ppb in non-allergic subjects;
FeNO in children with eosinophils and mast cells: 33.8ppb in allergic and 11.82ppb in non-allergic children.
View Figure 2a
.
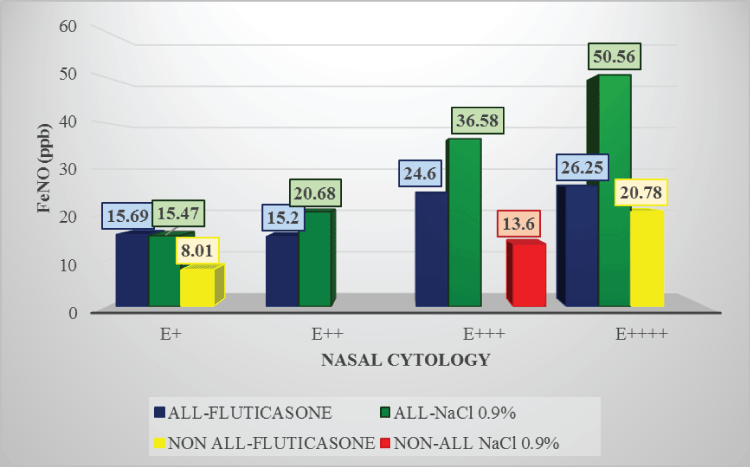
Figure 2b: FeNO levels in children with nasal eosinophils after treatment
Children treated with Fluticasone:
FeNO in patients with eosinophils + : 15.69ppb in allergic patients and 8.01ppb in the non-allergic patient;
FeNO in allergic patients with eosinophils ++ : 15.2ppb;
FeNO in allergic subjects with eosinophils +++ : 24.6ppb;
FeNO in patients with eosinophils ++++ : 26,25ppb in the allergic patient and 20.78ppb in the non-allergic patient.
Children treated with NaCl 0.9%:
FeNO in the allergic patient with eosinophils + : 15.47ppb;
FeNO in allergic patients with eosinophils ++ : 20.68ppb;
FeNO in subjects with eosinophils +++ : 36.58ppb in allergic and 13.6 in non-allergic subjects;
FeNO in allergic children with eosinophils ++++ : 50,56ppb.
View Figure 2b
Questionnaires
ACT (C-ACT) and SNOT-20 were used for determining the presence and severity of upper and lower airway disorders. Each subject completed the questionnaires before and after nasal treatment.
Our results (Table 4a and Table 4b) indicated that nasal steroid caused a higher level of improvement than nasal saline:
![]()
Table 4a: ACT before and after treatment.
View Table 4a
![]()
Table 4b: SNOT-20 before and after treatment.
View Table 4b
• Nasal steroid→87% and 77% of patients showed an improvement in asthma and rhinitis total symptom score of baseline, pre-medical treatment values.
• Nasal saline→42% and 40% of patients showed an improvement in asthma and rhinitis total symptom score of baseline
Rhinitis and the quality of life
In our analysis, it was apparent that clinical diagnosis of rhinitis and "rhinitis" scores on the survey were not associated. SNOT-20:
• No problem to mild problem: 12 of children
• Moderate problem: 57 of children
• Severe to "as bad as it can be": 15 of children
Clinical diagnosis:
• No problem to mild problem: 30 of children
• Moderate problem: 49 of children
• Severe to "as bad as it can be": 5 of children
Discussion
Epidemiological evidence consistently demonstrates the frequent coexistence of asthma and rhinitis in the same patients, thus leading to the concept that these two conditions are different aspects of the same disease (United Airway [6]). Rhinitis is present in the majority of patients with asthma (74% of patients with allergic asthma and 42% of patients with non-allergic asthma), and a significant minority (20-50%) of patients with rhinitis have concomitant asthma [2,3,6].
This consideration relates to important implications in the clinical management of these diseases: patients with rhinitis should be evaluated for a possible concomitant asthma; conversely, it is necessary to assess the presence of asthma in patients with nasal disease [12]. Even though this connection seems clear, upper airway symptoms are often under diagnosed. According to this statement, in our study, 69% of asthmatic children with concomitant rhinitis didn't receive a correct diagnosis and medications treating nasal diseases. In these asthmatic patients, "occult" (clinically unrecognized) rhinitis was associated with a worse respiratory involvement and therefore worse healthcare costs and quality of life.
We investigated the impact of rhinitis on asthma in airway inflammation and FeNO levels in patients with rhinitis of different etiology (allergic versus non-allergic), as well as the influencing factors. We also evaluated whether improved control of upper airway in a child with asthma also means improving lower airway symptoms and inflammation [13-15].
Generally, FeNO was higher in children with both asthma and rhinitis than in asthmatic patients without rhinitis; in all subjects, atopic sensitization appeared to be an important cause of elevated FeNO levels (Figure 3).
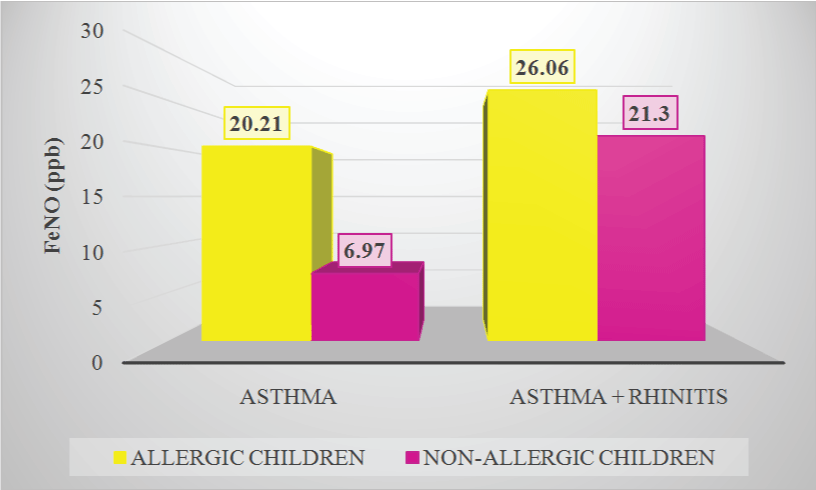
.
Figure 3: FeNO in allergic and non-allergic asthmatic children with or without rhinitis
View Figure 3
It is hypothesized that the local immune response to the allergen leads to the recruitment of eosinophils [16], which may induce NO-synthase in bronchial epithelial cells. Among patients with rhinitis, FeNO was higher in children with eosinophils, with or without mast cells, than other patients (Figure 1a and Figure 2a). In subgroup with eosinophils, the increase of FeNO was associated with the increase of nasal inflammation (Figure1b and Figure 2b).
Elevated levels of eNO are thought to result from increased expression and activity of inducible form of nitric oxide synthase in airway epithelial and inflammatory cells. These findings suggest that eNO provides information about the degree of eosinophilic airway inflammation and that the correlations between eNO and pulmonary function test characteristics are probably caused by the impact of eosinophils on pulmonary functions [17].
Measurement of FeNO in this group of patients may be helpful in identifying those with ongoing airway eosinophilia that is a hallmark of bronchial asthma [18].
Consistent with the observation that corticosteroids inhibit the expression of inducible NOS (iNOS) in epithelial cells, [19] we aimed to demonstrate that nasal steroids are effective not only in controlling upper airway inflammation, but also in lower airway inflammation.
According to ACT and SNOT20, 88% and 77% of patients treated with nasal steroid showed an improvement in asthma and rhinitis total symptom score of baseline; nasal saline irrigation caused the same result in 42% and 40% of subjects (Table 4a and Table 4b).
At the same time, treatment of patients with nasal steroids leads to a fall in airway eosinophilia measured by nasal cytology and FeNO.
The comparison of NO exhalation and nasal cytology before and after saline irrigation or Fluticasone application suggests that the decrease in upper airway inflammation is associated with the decrease in lower airway inflammation (Figure 1a, Figure 1b, Figure 2a and Figure 2b).
The correlation was more pronounced after nasal steroids treatment (in all patient groups, nasal steroids caused an higher reduction in FeNO levels than nasal saline, but with no statistical significance), therefore it remains unclear whether, in this group of children, the occasional increase of exhaled NO and nasal inflammation was due to incorrect execution of therapy.
These results should be interpreted in context and are subject to limitations.
It is still possible that this study includes individuals who were taking medications for rhinitis without our prescription. Another limitation that should be considered is the possibility that those who were prescribed nasal steroid were different from those who were treated with saline, in ways that could not be observed in claims data. These unobserved differences may be explanatory factors associated with differences in the degree of airway inflammation. In conclusion, the distribution of different subpopulations (72 allergic children vs. 12 non allergic children -Table1) is not homogeneous concerning the number of patients [5].
Conclusions
In summary, this study provides evidence of a relationship between upper and lower airway inflammation, therefore, a rigorous treatment of comorbid factors of asthma, such as rhinitis, could result in less asthma exacerbations, which will greatly improve the quality of life [12].
Although it is not known whether this inflammation leads to irreversible airway remodelling, it seems reasonable, approaching an asthmatic child, to evaluate the possible nasal involvement.
FeNO and nasal cytology are easy-to-perform and helpful in identifying patients with [18] a "subclinical" inflammation that may need a closer follow-up and, possibly, anti-inflammatory medications [19].
Key Messages
1. Asthma and rhinitis are different manifestations of a common pathogenic phenomenon involving one airway, therefore treatments for one condition could potentially alleviate the coexisting disease.
2. We used FeNO and nasal cytology to investigate upper and lower airway inflammation and the clinical benefits of nasal treatment in children with asthma.
3. Nasal steroids leads to a fall in airway eosinophilia measured by nasal cytology and FeNO: the decrease in upper airway inflammation is associated with the decrease in lower airway inflammation
Capsule Summary
According to the renewed interest in the role that upper airway plays as biomarker of lower airway inflammation, in this study we investigate the role that rhinitis inflammation and therapy plays on lower airway situation.
References
-
Grossman J (1997) One airway, one disease. Chest 111: 11S-16S.
-
Bousquet J, Vignola AM, Demoly P (2003) Links between rhinitis and asthma. Allergy 58: 691-706.
-
Peroni DG, Piacentini GL, Alfonsi L, Zerman L, Di Blasi P, et al. (2003) Rhinitis in pre-school children: prevalence, association with allergic diseases and risk factors. Clin Exp Allergy 33: 1349-1354.
-
Morjaria JB, Caruso M, Rosalia E, Russo C, Polosa R (2014) Preventing progression of allergic rhinitis to asthma. Curr Allergy Asthma Rep 14: 412.
-
Kalpaklioglu AF, Kalkan IK (2012) Comparison of orally exhaled nitric oxide in allergic versus nonallergic rhinitis. Am J Rhinol Allergy 26: e50-54.
-
Compalati E, Ridolo E, Passalacqua G, Braido F, Villa E, et al. (2010) The link between allergic rhinitis and asthma: the united airways disease. Expert Rev Clin Immunol 6: 413-423.
-
Buchvald F, Baraldi E, Carraro S, Gaston B, De Jongste J, et al. (2005) Measurements of exhaled nitric oxide in healthy subjects age 4 to 17 years. J Allergy Clin Immunol 115: 1130-1136.
-
Cobos Barroso N, Pérez-Yarza EG, Sardón Prado O, Reverté Bover C, Gartner S, et al. (2008) Exhaled nitric oxide in children: a noninvasive marker of airway inflammation. Arch Bronconeumol 44: 41-51.
-
Olin AC, Bake B, Torén K (2007) Fraction of exhaled nitric oxide at 50 mL/s: reference values for adult lifelong never-smokers. Chest 131: 1852-1856.
-
Malmberg LP, Petäys T, Haahtela T, Laatikainen T, Jousilahti P, et al. (2006) Exhaled nitric oxide in healthy nonatopic school-age children: Determinants and height-adjusted reference values. Pediatr Pulmonol 41: 635-642.
-
Bergmann-Hug K, Wirth R, Henseler M, Helbling A, Pichler WJ, et al. (2009) Effect of natural seasonal pollen exposure and repeated nasal allergen provocations on elevation of exhaled nitric oxide. Allergy 64: 1629-1634.
-
Caimmi D, Marseglia A, Pieri G, Benzo S, Bosa L, et al. (2012) Nose and lungs: one way, one disease. Ital J Pediatr 38: 60.
-
Ferreira de Magalhaes MJ, Pereira AM, de Sa E Sousa Santos AI, Morais-Almeida M, Azevedo I, et al. (2015) Asthma control in children is associated with nasal symptoms, obesity and health insurance: a nationwide survey. Pediatr Allergy Immunol.
-
de Groot EP, Nijkamp A, Duiverman EJ, Brand PL (2012) Allergic rhinitis is associated with poor asthma control in children with asthma. Thorax 67: 582-587.
-
Crystal-Peters J, Neslusan C, Crown WH, Torres A (2002) Treating allergic rhinitis in patients with comorbid asthma: the risk of asthma-related hospitalizations and emergency department visits. J Allergy Clin Immunol 109: 57-62.
-
Di Cara G, Marcucci F, Palomba A, Milioni M, Pecoraro L, et al. (2015) Exhaled nitric oxide in children with allergic rhinitis: a potential biomarker of asthma development. Pediatr Allergy Immunol 26: 85-87.
-
Strunk RC, Szefler SJ, Phillips BR, Zeiger RS, Chinchilli VM, et al. (2003) Relationship of exhaled nitric oxide to clinical and inflammatory markers of persistent asthma in children. J Allergy Clin Immunol 112: 883-892.
-
Payne DN, Adcock IM, Wilson NM, Oates T, Scallan M, et al. (2001) Relationship between exhaled nitric oxide and mucosal eosinophilic inflammation in children with difficult asthma, after treatment with prednisolone. Am J Respir Crit Care Med 164: 1376-1381.
-
Silvestri M, Spallarossa D, Frangova Yourukova V, Battistini E, Fregonese B, et al. (1999) Orally exhaled nitric oxide levels are related to the degree of blood eosinophilia in atopic children with mild-intermittent asthma. Eur Respir J 13: 321-326.
-
Pynnonen MA, Kim HM, Terrell JE (2009) Validation of the Sino-Nasal Outcome Test 20 (SNOT-20) domains in nonsurgical patients. Am J Rhinol Allergy 23: 40-45.
-
Thomas M, Kay S, Pike J, Williams A, Rosenzweig JR, et al. (2009) The Asthma Control Test (ACT) as a predictor of GINA guideline-defined asthma control: analysis of a multinational cross-sectional survey. Prim Care Respir J 18: 41-49.
-
Koolen BB, Pijnenburg MW, Brackel HJ, Landstra AM, van den Berg NJ, et al. (2011) Comparing Global Initiative for Asthma (GINA) criteria with the Childhood Asthma Control Test (C-ACT) and Asthma Control Test (ACT). Eur Respir J 38: 561-566.





