Journal of Nutritional Medicine and Diet Care
Nutritional Intake and Cardiovascular Risk Factors in Saudi Subjects with Different Degrees of Atherosclerosis: A Case Control Study
Eman M Alissa1* and Nabeel A Alama2
1Department of Clinical Biochemistry, Faculty of Medicine, King Abdulaziz University, Jeddah, Saudi Arabia
2Department of Internal Medicine, Faculty of Medicine, King Abdulaziz University, Jeddah, Saudi Arabia
*Corresponding author:
Eman M Alissa, Faculty of Medicine, King Abdulaziz University, PO Box 12713, Jeddah 21483, Kingdom of Saudi Arabia, Tel: (966)-2-6400000 Ext. 23432, Fax: (966)-2-6643499, E-mail: em_alissa@yahoo.com
J Nutri Med Diet Care,
JNMDC-1-008, (Volume 1, Issue 2),
Original Article
Received: August 31, 2015: Accepted: October 12, 2015: Published: October 14, 2015
Citation: Alissa EM, Alama NA (2015) Nutritional Intake and Cardiovascular Risk Factors in Saudi Subjects with Different Degrees of Atherosclerosis: A Case Control Study. J Nutri Med Diet Care 1:008
Copyright: © 2015 Alissa EM. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Coronary heart disease (CHD) is related to a large number of environmental and lifestyle factors including an unhealthy dietary pattern, physical inactivity and a positive smoking habit. Dietary modification has been involved in managing and reducing the risk of CHD.
We aimed to assess the dietary intake of Saudi population with various degrees of atherosclerosis, and to examine the relationship between specific nutrient intakes with some classical cardiovascular risk factors.
The study comprised 450 subjects (150 men and 300 women), aged between 40-88 years, randomly selected from the medicine clinics at the King Abdulaziz University Hospital in Jeddah, Saudi Arabia, in a case-control study design. One hundred and fifty controls were matched for age and sex with 150 patients with subclinical atherosclerosis and 150 patients with clinical atherosclerosis. A standardized questionnaire was used to determine socio-demographics variables, general health, and lifestyle habits. Anthropometric measurements were taken for all study subjects.
Overall and central obesity was highly prevalent among the study participants. Daily intakes of all macronutrients were significantly lower in patients with clinical and subclinical atherosclerosis than their matched controls (p < 0.05). Except for vitamin C and β-carotene, atherosclerotic patients reported the lowest consumption levels of all vitamins than patients with subclinical atherosclerosis and matching controls (p < 0.05). Concerning minerals, the lowest consumption levels were reported by patients with subclinical atherosclerosis as compared to atherosclerotic patients and matching controls except for calcium (p < 0.05).
Increasing public awareness of healthy lifestyle patterns, including increasing physical activity and a reduction in smoking, to enhance the prevention of CHD and associated risk factors.
Key words
Dietary pattern, Atherosclerosis, Cardiovascular risk factors
Introduction
Cardiovascular disease (CVD) is the leading cause of death globally [1]. Coronary heart disease (CHD) is the most common type of heart disease [2]. Many hospital-based studies have shown a rise in the occurrence of CHD in the Kingdom of Saudi Arabia [3,4] and the overall prevalence was estimated to be 5.5% in a community-based study [5]. The major underlying cause of CHD is atherosclerosis. Atherosclerosis is as an inflammatory process that leads to plaque build-up in the arterial wall, stenosis and eventually plaque rupture, heart attack, or stroke [6]. CHD is related to a large number of environmental and lifestyle factors including an unhealthy dietary pattern, physical inactivity and a positive smoking habit [7]. Dietary modification has been involved in managing and reducing the risk of CVD [8,9]. Unhealthy dietary practices can synergize with underlying genetic tendencies, predisposing to atherosclerosis. Several dietary factors have been associated with a reduced rate of atherosclerosis progression in subjects with established CHD; these include increased whole grains, fewer refined carbohydrates, and a high content of oily fish [10,11]. Diets rich in combinations of these components as well as dietary antioxidants have also shown inverse associations with subclinical atherosclerosis markers [12,13].
Progression of coronary atherosclerosis, as assessed by quantitative angiography, is a well-established marker of clinical risk that allows direct investigation of effects of risk factors on atherogenesis [14]. Therefore, modifications of dietary components are thought to restrict the progression of atherosclerosis and facilitate the regression of cardiovascular risk factors. In the present study we aimed to assess the dietary intake of Saudi population with various degrees of atherosclerosis, and to examine the relationship between specific nutrient intakes with some classical cardiovascular risk factors.
Methods
Study design
The study comprised 450 subjects (150 men and 300 women), aged between 40-88 years, attending the department of internal medicine clinics at the King Abdulaziz University Hospital (KAUH) in Jeddah, Saudi Arabia between January 2013 and January 2015. Subjects were randomly selected in a case-control study design. All participants provided informed consent to a protocol approved by the local Ethical Review board of KAUH.
Study subjects
None of the study subjects had a past history of cardiovascular events (unstable angina, myocardial infarction, and stroke), heart failure, peripheral vascular diseases, or a history of cardiovascular surgery. Individuals with any major co-morbidity such as cancer, autoimmune, chronic kidney disease, hepatic dysfunction, infectious, and inflammatory diseases were also excluded.
One hundred and fifty controls were matched for age and sex with 150 patients with subclinical atherosclerosis and 150 patients with clinical atherosclerosis. The latter patient group was subdivided into 3 subgroups according to the number of occluded coronary vessels: single, double and multi vessel disease. Subclinical stages of atherosclerosis was determined by measuring the intima-media thickness of the carotid arteries (CIMT) using a non-invasive ultrasound techniques. The presence of one or more CIMT ≥ 0.8 mm in one major area was considered to be evidence of significant CIMT atherosclerosis [15].
Overt or clinical stages of atherosclerosis was scored by the severity of angiographically defined disease > 50% occlusion of the luminal diameter in ≥ 1 coronary artery [16]. A diagnosis of a myocardial infarction was made in accordance with Joint European Society of Cardiology/American College of Cardiology Committee criteria [17]. None of the patients had suffered a heart attack within 6 months of recruitment into the study.
The control subjects were drawn from the outpatients clinics of the same hospital populations with disorders not normally associated with metabolic abnormalities (e.g., orthopedic conditions).
Each subject was interviewed to complete a standardized questionnaire to determine socio-demographics variables, lifestyle habits (including smoking status, physical exercise and dietary pattern), family history of chronic diseases, past medical history and medication use. Family history of early CHD was present when a first-order relative had developed cardiac death, myocardial infarction, or coronary revascularization at < 65 years of age for women and < 55 years of age for men.
Dietary assessment
A 96-item semi-quantitative pre-validated food frequency questionnaire (FFQ) was used to assess dietary habits among the study participants. The reliability and validity of the FFQ have been evaluated previously among participants of a population that is comparable to our present study subjects attending health examination clinics [18]. Participants were questioned about their average intake and the specified serving portion size for each food over the past year. For each food item on the questionnaire, five responses were possible, ranging from "almost never" to "2-4 times a day." Frequencies and portions for the individual food items were converted to average daily intake of macro and micronutrients for each participant including carbohydrates, total fat, proteins, saturated fat, monounsaturated fatty acids, polyunsaturated fatty acids, fiber, cholesterol, vitamin E, vitamin C, β-carotene, vitamin D, vitamin B12, folic acid, calcium, selenium, zinc and copper.
To control for total energy intake, all nutrients were adjusted for total energy intake by using the regression residual method [19]. Implausible energy intakes (i.e., < 500 kcal/day or > 4500 kcal/day) were excluded. The nutrient database used was based on UK food composition tables [20] together with food composition tables for use in East Asia and the US handbook of food composition [21]. The composition of traditional local foods, not included in the above tables, was derived from another local study [22]. The estimated dietary intake of all nutrients was calculated in terms of percentage recommended nutritional intake for US adults for each individual, because there are no published data on recommendations for a Saudi population. The most recent version of the dietary guidelines for Americans [23] was used to standardize the pattern of nutrient intake. Information on multivitamin supplement use was also requested on the FFQ, but data on nutrient intake from supplements were not included in the analyses.
Anthropometric assessment
For all individuals, anthropometric parameters including weight, height, and waist and hip circumferences were measured using standard protocols. Body weight and weight were measured with subjects dressed in very light clothing after an overnight fast. Body weight was measured with standard scales to an accuracy of ± 0.1 kg and height was measured to an accuracy of ± 0.1 cm (a stadiometer was used for measuring height). BMI was calculated as weight (kg) divided by height squared (m2). Waist circumference was measured at the level of the umbilicus (at the level midway between the lower rib margin and the iliac crest). Blood pressure was measured twice while patients were seated and rested for 15 min, using a standard mercury sphygmomanometer.
CIMT assessment
The subjects underwent B-mode ultrasonography of the extracranial carotid arteries by use of a high-resolution ultrasound instrument (iU22 xMatrix ultrasound system, Philips Medical Systems, USA) with a linear array multi-frequency transducer. Both common (CCA) and internal carotid arteries were evaluated. The IMT, defined as the distance between the intimal-luminal and the medial-adventitial interfaces, was measured. Briefly, in posterior approach and with the sound beam perpendicular to the arterial surface, 1 cm from the bifurcation, three longitudinal IMT measurements were completed on both common carotid arteries far-wall, at sites without plaques. The measurement followed a standardized scanning protocol [24].
According to these criteria, subjects were considered as normal if no lesion was detected, or having carotid atherosclerosis when a plaque, stenosis or occlusion was detected in at least one segment of common, bifurcation or internal carotid artery.
Coronary artery stenosis assessment
Coronary angiography was performed at the catheterization laboratory at the cardiac care unit, KAUH. Subjects with suspected or known CHD were admitted to verify the presence of the disease.
Statistical analysis
All results are expressed as mean ± SEM or n (%) as appropriate. Data were assessed for normality using the Kolomogorov-Smirnov test. Chi-square test was implemented when necessary for categorical variables comparison. Statistical analyses were performed using ANOVA test for normally distributed parameters or Kruskall-Wallis test for non-normally distributed parameters to compare mean values of repeated measures of non-normally distributed parameters. Multiple comparisons of the mean differences among the variables were done using the Bonferroni post-hoc test. Correlation analysis was undertaken with Pearson's correlation coefficient for parametric data and Spearman's rho coefficient for nonparametric data. Macronutrients intake was adjusted for energy according to the method of Willett and Stampfer [19]. Statistical analysis was performed using the SPSS (version 20.0) software. A p-value < 0.05 (2-tailed) was considered to be significant.
Results
Demographic and anthropometric variables distribution
Four hundred and fifty subjects were categorized into three groups; 150 controls without atherosclerosis, 150 patients with subclinical atherosclerosis, and 150 patients with clinically evident atherosclerosis. Female: male distribution was 100:50 in each subgroup. The mean age of subjects were 59.9 ± 0.6, 60.0 ± 0.6, and 62.0 ± 0.7 years in the three groups respectively (p > 0.05).
Table 1 presents the socio-demographic characteristics of the study population. The majority of the subjects were nonsmokers, married, illiterate, unemployed or retired, with 5 children or more and living in rented apartments. Two thirds of the atherosclerotic patients and those with subclinical atherosclerosis reported physical activity 1-2 times per week while physical inactivity (as defined by exercising < 1 time per week) was prevalent among two thirds of their matching controls.
![]()
Table 1: Clinical characteristics of the study population (N = 450).
View Table 1
Atherosclerotic patients were more likely to be shorter, had lower waist and hip circumferences measurements than patients with subclinical atherosclerosis and matching controls (p < 0.01 in all). Compared to patients with subclinical atherosclerosis and matching controls, atherosclerotic patients had higher SBP readings and reported less family history of CVD (p < 0.01).
Figure 1 shows high prevalence of overall and central obesity among the study participants as estimated by three anthropometric indices; BMI, WHR and waist circumference. Ninety seven percent of atherosclerotic patients had central obesity vs. 87% of patients with subclinical atherosclerosis and 87% of matched controls (p < 0.05).
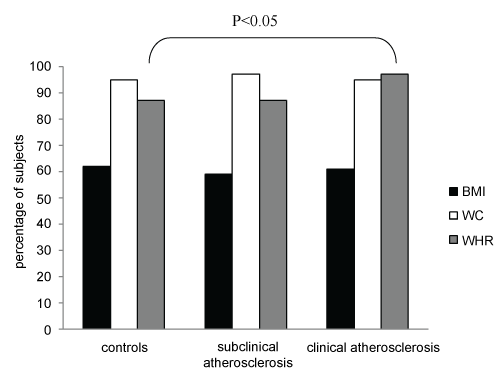
.
Figure 1: Obesity distribution among the study population (N = 450) as defined by the values of: BMI ≥ 30 Kg/m2, waist circumference > 80 cm in females and 94cm in males, and WHR ≥ 0.80 in females and ≥ 0.95 in males. The only significant difference was in WHR value between atherosclerotic patients vs. patients with subclinical atherosclerosis and matching controls as tested by χ 2 test (p < 0.05).
View Figure 1
Dietary intake levels
Table 2 summarizes levels of dietary covariates in the study population. Daily intakes of all macronutrients were significantly lower in patients with clinical and subclinical atherosclerosis than their matched controls (p < 0.05). Figure 2a illustrates that the percentage of energy intake from carbohydrate was significantly higher among patients with subclinical atherosclerosis in comparison with their matched controls and atherosclerotic patients (p < 0.0001). Conversely the percentage of energy intake from fat was significantly lower among patients with subclinical atherosclerosis in comparison with their matched controls and atherosclerotic patients (p < 0.0001). The percentage of energy intake from protein was significantly lower among controls in comparison with clinical and subclinical atherosclerotic patients (p < 0.0001). Figure 2b shows significantly higher percentage of energy intake from PUFA among controls in comparison with clinical and subclinical atherosclerotic patients (p < 0.0001). The percentage of energy intake from SFA and MUFA were significantly lower among patients with subclinical atherosclerosis in comparison with their matched controls and atherosclerotic patients (p < 0.0001 in both).
![]()
Table 2: Nutrients intake levels of the study population (N = 450).
View Table 2
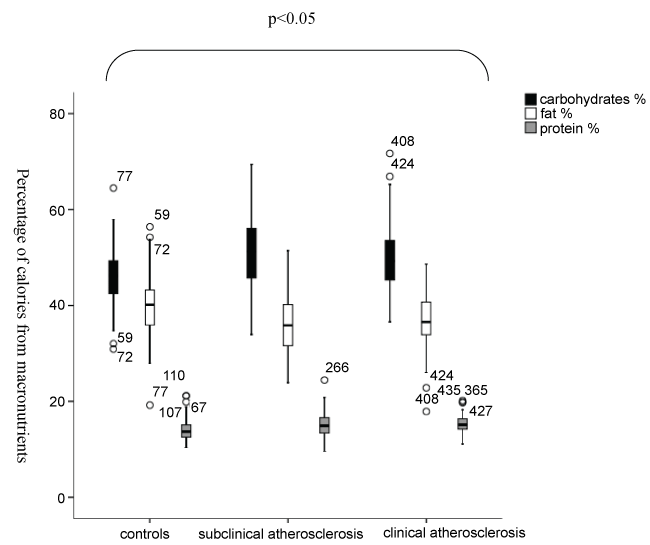
.
Figures 2a: Percentage of calories from macronutrients of the total daily energy intake of study subjects in the 3 groups. Box and whisker plots illustrate median and interquartile ranges of % of calories supplied by carbohydrates, total fat and protein in controls, patients with subclinical atherosclerosis and atherosclerotic patients. Open circles show outliers. Statistical significance was tested by Kruskall-Wallis test for non-normally distributed parameters with Bonferroni adjustment for multiple testing.
View Figures 2a
Except for vitamin C and β-carotene, atherosclerotic patients reported the lowest consumption levels of all vitamins than patients with subclinical atherosclerosis and matching controls (p < 0.05). Concerning minerals, the lowest consumption levels were reported by patients with subclinical atherosclerosis as compared to atherosclerotic patients and matching controls except for calcium (p < 0.05).
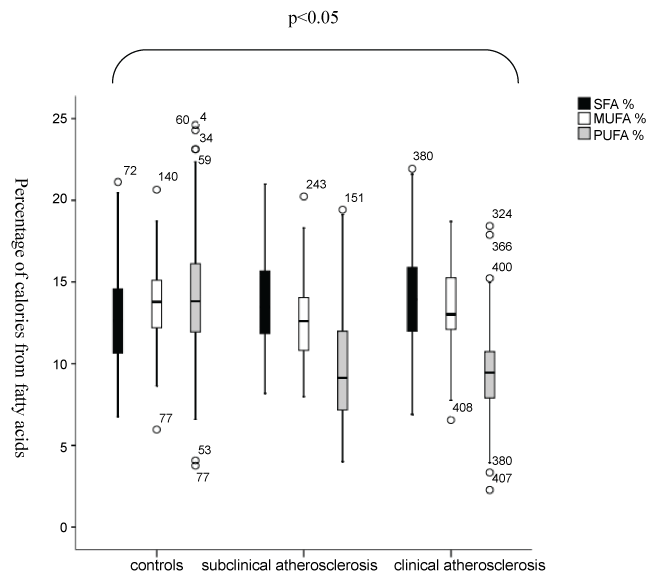
.
Figures 2b: Percentage of calories from fatty acids of the total daily energy intake of study subjects in the 3 groups. Box and whisker plots illustrate median and interquartile ranges of % of calories supplied by SFA, MUFA and PUFA in controls, patients with subclinical atherosclerosis and atherosclerotic patients. Open circles show outliers. Statistical significance was tested by Kruskall-Wallis test for non-normally distributed parameters with Bonferroni adjustment for multiple testing.
View Figures 2b
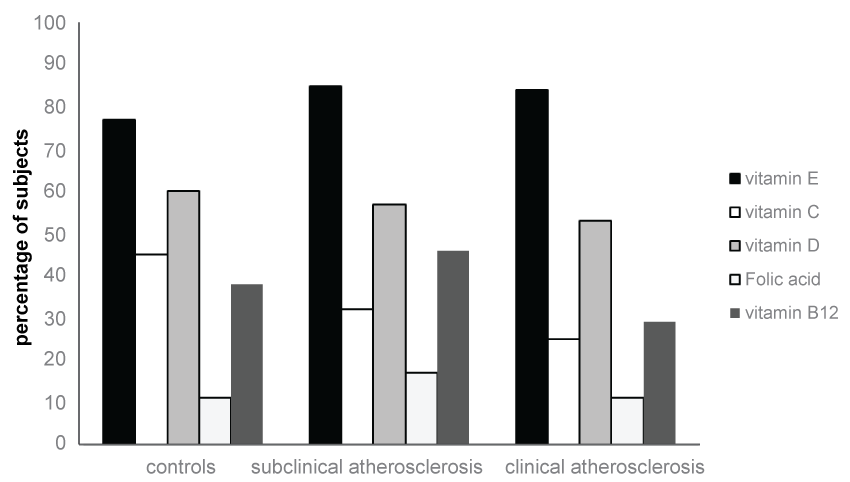
Overall, levels of intake were below the recommended values for optimal health for energy, carbohydrates, vitamin D, vitamin E, calcium, selenium and zinc in all study groups. Conversely, intake levels of total fat, saturated fat and MUFA were above recommendations in all study groups. Figure 3a and Figure 3b display the percent of subjects in each study group with suspected micronutrients inadequacies as determined by consuming micronutrients in amounts below their corresponding EAR values. Inadequacy of dietary selenium was highly prevalent among 84%, 90% and 86% of the study groups: controls, subclinical atherosclerosis and clinical atherosclerosis respectively. Dietary calcium and zinc inadequacy was prevalent among almost half of the study participants. Finally, dietary copper inadequacy was prevalent among almost quarter of the study participants. With regards to vitamins, vitamin E inadequacy was highly prevalent among 77%, 85% and 84% of the study groups: controls, subclinical atherosclerosis and clinical atherosclerosis respectively. Vitamin D inadequacy was prevalent among two thirds of the study population followed by vitamin C inadequacy which was prevalent among one third of the study population whereas folic acid inadequacy was merely prevalent among one tenth of the study population.
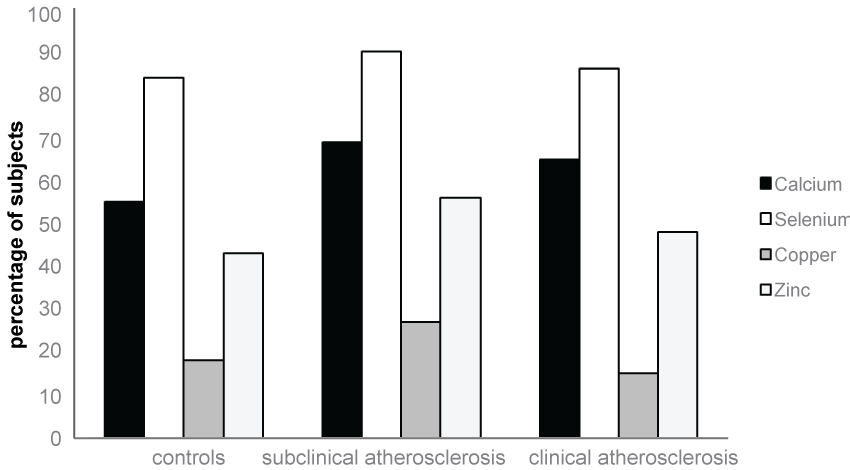
.
Figures 3a: Frequency of study subjects within the 3 groups with minerals inadequacies as defined by dietary consumption levels below their corresponding estimated average requirement values and they are as follow: calcium < 769.2 mg/d, selenium < 57.7 μg/d, copper < 0.92 μg/d, zinc < 7.4 mg/d.
View Figures 3a
.
Figures 3b: Frequency of study subjects within the 3 groups with vitamins inadequacies as defined by dietary consumption levels below their corresponding estimated average requirement values and they are as follow: vitamin E < 11.5 mg/d, vitamin C < 30.8 mg/d, vitamin D < 7.7 μg/d, vitamin B12 < 1.15 μg/d, folic acid < 153.9 μg/d.
View Figures 3b
Correlation between nutrients intakes and cardiovascular risk factors
Table 3 shows univariate associations between macro-and micronutrients intakes with obesity indices in the study population as categorized into obese and non-obese individuals. More significant relationships were documented by central obesity measures, namely waist circumference and WHR.
![]()
Table 3: Correlation between indices of adiposity and nutrient intake levels. Significant relationships are shown in bold font Obesity is defined by BMI ≥ 30 Kg/m2. Non-obesity is defined by 25-29.9 Kg/m2.
View Table 3
In addition, further testing for the relationship between nutrients intakes and blood pressure readings in the study population as categorized into hypertensive and pre-hypertensive patients are listed in table 4. Negative association between SBP and % of energy supplied by MUFA (r = -0.177, p < 0.05) was found in pre-hypertensive patients and negative correlations between SBP and both of % of energy supplied by PUFA (r = -0.168, p < 0.05) and vitamin C (r = -0.182, p < 0.01) among hypertensive patients. On the other hand, DBP was inversely correlated with % of energy supplied by MUFA (r= -0.172, p < 0.05) and with selenium (r=- 0.253, p < 0.01) in pre-hypertensive patients. DBP was negatively correlated with % of energy supplied by PUFA (r = -0.182, p < 0.01) in hypertensive patients.
![]()
Table 4: Correlation between blood pressure and nutrients intake levels. Significant relationships are shown in bold font.
View Table 4
Discussion
Although the prevalence of chronic diseases like CVD are on the rise worldwide [25], the available information on sub-optimal dietary patterns among atherosclerotic Saudi population is relatively limited [26]. Dietary composition is likely to influence the development of atherosclerosis in a causal manner [27], yet investigators have failed to find concomitant associations with specific dietary measures.
Thus, the aim of the current study was to assess dietary intake of Saudi population with various degrees of atherosclerosis, by pre-validated semi-quantitative food frequency questionnaire, and to examine the relationship between nutrients intakes with some classical cardiovascular risk factors. Considering the high prevalence of cardiovascular risk factors in our study sample and the influence of socio-demographic variables, it can be postulated that diet has a key role in developing CAD. Older age, female gender, adiposity, and physical inactivity are powerful determinants of atherosclerosis, and thus may alter the relations between diet and cardiovascular risk.
There are many epidemiological data showing the relationships between and unhealthy dietary habits, notably, low intake of fibers and anti-oxidants, high intake of animal fat and refined sugar [28-30].
It is noteworthy that the mean total energy intake in the control group was more than that in the other two case groups. The contrasting findings in this study could be the result of heart patients being aware of the effect of diet modification on their disease. Also, it could be due to underreporting as case-control study design relies on the respondents' memory and their capabilities to interpret those questions.
Epidemiological studies and controlled trial data have long indicated that variations in the relative amounts of dietary fatty acids influence the risk of CVD in part by influencing lipid metabolism [31,32]. Indeed the amount of energy supplied by total fat and PUFA in the control group was more than that in the other two case groups, but energy contribution by SFA was lower than that in the other two case groups. Our study extends previous studies [33,34] by showing that increasing total fat and saturated fat consumption are directly associated with obesity among non-obese individuals while controlling for potential confounders (Table 3).
Indeed consumption of fish, a major source of dietary omega-3 fats, was associated with significantly reduced progression of coronary atherosclerosis [11]. Nonetheless, omega-6 fats are largely consumed from vegetable oils such as corn, sunflower, safflower, and soybean oils and studies have shown inconsistent findings about their cardiovascular benefits.
Although several studies have observed protective associations of n-6 PUFA on progression of coronary atherosclerosis [35], others have found no association [36] or even trends toward higher risk [37]. Nevertheless, contribution to energy by dietary carbohydrates and protein intake in the control group was less than that in the other two case groups. In this respect, it should be noted that high levels of consumption of animal protein have been shown to increase the risk for heart disease. Health effects of high-carbohydrate and high-starch diets, whether beneficial or detrimental, vary due to various types and sources of carbohydrates consumed and have been discussed in literature [29,38]. It was not surprising to find an inverse correlation between dietary fiber level and waist circumference among obese subjects (Table 3). According to previous studies, the findings on the level of fiber intake were predictable [9,39,40].
Micronutrients are vitamins and minerals that are required in small quantities for specific functions such as essential coenzymes and cofactors for metabolic reactions and required to maintain energy production and life. The present study dietary vitamins showed diverse pattern, but essentially a negative correlation with obesity measures (Table 3) and blood pressure readings (Table 4). There is a substantial body of data supporting the biological plausibility of cardiovascular benefits of certain micronutrients [41]. Protective effects of micronutrients may impart anti-inflammatory and anti-thrombotic characteristics to such a dietary pattern [42].
With the exception of vitamin C and copper, dietary levels of the remaining micronutrients were below recommended levels. Micronutrients inadequacy are long suspected to be involved in atherosclerotic lesions development and the protection provided by their supplementation are extensively studied [42]. Yet, the exact mechanism by which a particular micronutrient may affect heart disease risk are unclear, but it is likely that they involve effects on enzymes, hormones and messenger molecules.
Our current data and previous study results support the hypothesis that micronutrients inadequacy promotes atherosclerosis development, at least in part, through its influence on oxidant antioxidant balance [26]. It has been postulated that higher intakes of antioxidants may attenuate oxidative stress, an etiology common among CVD [43]. Despite these plausibly biological mechanisms, single nutrients have been inconsistently associated with disease outcomes. Some of this inconsistency may be due to differences in food sources of these nutrients across unique populations, particularly when predominant food sources of a single nutrient show opposite associations with disease. It is possible that some constituents of the food matrix interact with single nutrients, altering their bioavailability and influencing mechanisms that underlie disease development [44].
Although our study cannot be used to infer causality, but it might be safe to say that dietary modification and exercise are associated with lower prevalence of coronary atherosclerosis. Another potential limitation of the study was its retrospective design though this design is not uncommon in descriptive studies. Although FFQ is usually used to investigate long-term dietary intakes in epidemiological studies, this method has its limitations. As a result of its closed structure, the flexibility and the degree of between-person variation is limited compared with open methods like 24 hr dietary recalls. However, important strengths of FFQ are its low respondent burden and cost and the fact that it gives information about respondents' usual or habitual dietary intake [45]. Moreover, FFQs have been shown to accurately rank the relative intake of micronutrients among individuals and are therefore an adequate, albeit not perfect, instrument for measuring relative dietary intake.
Conclusion
Our region has witnessed large changes in dietary patterns resulting from the marked shifts in socioeconomic status and demographics, as well as rapid urbanization and modernization during the last few decades [46]. Adopting the Western dietary pattern is known to be associated with cardiovascular risk factors, including an increased risk of obesity, hyperlipidemias, hypertension, diabetes and metabolic syndrome [47,48].
Therefore, increasing awareness of the high prevalence of cardiovascular risk factors among the public is crucial. In addition, there is an urgent need for nutrition education programs among all Saudi population to increase awareness regarding healthy diets and diet-related chronic diseases. This should be combined with encouragement of healthy lifestyle patterns, including increasing physical activity and a reduction in smoking, to enhance the prevention of CVD and associated risk factors.
Nevertheless, the influence of dietary components on oxidative status remains an active field of research, especially relating to age-associated diseases. Further studies on the graded relationship between coronary severity and dietary pattern would enhance our understanding of the relationships described in the current study.
Acknowledgments
The authors thank all of the patients who participated in or collaborated with the present study. The authors declare no conflict of interest. The authors wish to thank Professor Gordon Ferns (Brighton and Sussex Medical School, University of Brighton, UK) for critical review of the manuscript.
References
-
World Health Organization (2011) Global status report on non-communicable diseases. Geneva.
-
Mendis S, Puska P, Norrving B. World Health Organization (2011) Global atlas on cardiovascular disease prevention and control. Geneva.
-
Gaziano TA, Bitton A, Anand S, Abrahams-Gessel S, Murphy A (2010) Growing epidemic of coronary heart disease in low- and middle-income countries. Curr Probl Cardiol 35: 72-115.
-
BeLue R, Okoror TA, Iwelunmor J, Taylor KD, Degboe AN, et al. (2009) An overview of cardiovascular risk factor burden in sub-Saharan African countries: a socio-cultural perspective. Global Health 5: 10.
-
Al-Nozha MM, Arafah MR, Al-Mazrou YY, Al-Maatouq MA, Khan NB, et al. (2004) Coronary artery disease in Saudi Arabia. Saudi Med J 25: 1165-1171.
-
Ross R1 (1999) Atherosclerosis--an inflammatory disease. N Engl J Med 340: 115-126.
-
Levenson JW, Skerrett PJ, Gaziano JM (2002) Reducing the global burden of cardiovascular disease: the role of risk factors. Prev Cardiol 5: 188-199.
-
Mann JI (2002) Diet and risk of coronary heart disease and type 2 diabetes. Lancet 360: 783-789.
-
Srinath Reddy K, Katan MB (2004) Diet, nutrition and the prevention of hypertension and cardiovascular diseases. Public Health Nutr 7: 167-186.
-
Erkkila AT, Herrington DM, Mozaffarian D, Lichtenstein AH (2005) Cereal fiber and whole-grain intake are associated with reduced progression of coronary-artery atherosclerosis in postmenopausal women with coronary artery disease. Am Heart J 150: 94-101.
-
Erkkila AT, Lichtenstein AH, Mozaffarian D, Herrington DM (2004) Fish intake is associated with a reduced progression of coronary artery atherosclerosis in postmenopausal women with coronary artery disease. Am J Clin Nutr 80: 626-632.
-
Luedemann J, Schminke U, Berger K, Piek M, Willich SN, et al. (2002) Association between behavior-dependent cardiovascular risk factors and asymptomatic carotid atherosclerosis in a general population. Stroke 33: 2929-2935.
-
Millen BE, Quatromoni PA, Pencina M, Kimokoti R, Nam BH, et al. (2005) Unique dietary patterns and chronic disease risk profiles of adult men: the Framingham nutrition studies. J Am Diet Assoc 105: 1723-1734.
-
Vigen C, Hodis HN, Selzer RH, Mahrer PR, Mack WJ, et al. (2005) Relation of progression of coronary artery atherosclerosis to risk of cardiovascular events (from the Monitored Atherosclerosis Regression Study). Am J Cardiol 95: 1277-1282.
-
Riccioni G, D'Orazio N, Palumbo N, Bucciarelli V, Ilio Ed, et al. (2009) Relationship between plasma antioxidant concentrations and carotid intima-media thickness: The Asymptomatic Carotid Atherosclerotic Disease in Manfredonia Study. Eur J Cardiovasc Prev Rehabil 16: 351-357.
-
Judkins MP (1967) Selective coronary arteriography. I. A percutaneous transfemoral technic. Radiology 89: 815-824.
-
Alpert JS, Thygesen K, Antman E, Bassand JP (2000) Myocardial infarction redefined-a consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction. J Am Coll Cardiol 36: 959-969.
-
Alissa EM, Bahjri SM, Al-Ama N, Ahmed WH, Starkey B, et al. (2005) Dietary vitamin A may be a cardiovascular risk factor in a Saudi population. Asia Pac J Clin Nutr 14: 137-144.
-
Willett W, Stampfer MJ (1986) Total energy intake: implications for epidemiologic analyses. Am J Epidemiol 124: 17-27.
-
McCance RA, Widdowson EM, Holland B: (2002) "McCance and Widdowson's: The Composition of Foods." 6th (edn). Her Majesty's Stationery Office, London, UK.
-
Food Composition Tables for Use in East Asia (1972) US Department of Health, Education and Welfare and Food and Agriculture Organization of the United Nations.
-
Abalkhail BA, (1998) Hypercholesterolemia and susceptibility to cardiovascular diseases among white and blue collars in Jeddah. Saudi Med J 19:123-129.
-
http://www.dietaryguidelines.gov/
-
Stein JH, Korcarz CE, Hurst RT, Lonn E, Kendall CB, et al. (2008) Use of carotid ultrasound to identify subclinical vascular disease and evaluate cardiovascular disease risk: a consensus statement from the American Society of Echocardiography Carotid Intima-Media Thickness Task Force. Endorsed by the Society for Vascular Medicine. J Am Soc Echocardiogr 21: 93-111.
-
Alwan A (2011) Global status report on noncommunicable diseases 2010. Geneva: World Health Organization.
-
Alissa EM, Bahijri SM, Ferns GA (2005) Dietary macronutrient intake of Saudi males and its relationship to classical coronary risk factors. Saudi Med J 26: 201-207.
-
Davis N, Katz S, Wylie-Rosett J (2007) The effect of diet on endothelial function. Cardiol Rev 15: 62-66.
-
Hu FB, Willett WC (2002) Optimal diets for prevention of coronary heart disease. JAMA 288: 2569-2578.
-
Diehr P, Beresford SA (2003) The relation of dietary patterns to future survival, health, and cardiovascular events in older adults. J Clin Epidemiol 56: 1224-1235.
-
Artinian NT, Schim SM, Vander Wal JS, Nies MA. (2004) Eating patterns and cardiovascular disease risk in a Detroit Mexican American population. Public Health Nurs 21: 425-434.
-
Katan MB, Grundy SM, Willett WC (1997) Should a low-fat, high-carbohydrate diet be recommended for everyone? Beyond low-fat diets. N Engl J Med 337: 563-566.
-
He K, Liu K, Daviglus ML, Mayer-Davis E, Jenny NS, et al. (2008) Intakes of long-chain n-3 polyunsaturated fatty acids and fish in relation to measurements of subclinical atherosclerosis. Am J Clin Nutr 88:1111-1118.
-
Djousse L, Arnett DK, Carr JJ, Eckfeldt JH, Hopkins PN, et al. (2005) Dietary linolenic acid is inversely associated with calcified atherosclerotic plaque in the coronary arteries: the National Heart, Lung, and Blood Institute Family Heart Study. Circulation 111: 2921-2926.
-
Oh K, Hu FB, Manson JE, Stampfer MJ, Willett WC, (2005) Dietary fat intake and risk of coronary heart disease in women: 20 years of follow-up of the nurses' health study. Am J Epidemiol 161: 672-679.
-
Harris WS, Mozaffarian D, Rimm E, Kris-Etherton P, Rudel LL, et al. (2009) Omega-6 fatty acids and risk for cardiovascular disease: a science advisory from the American Heart Association Nutrition Subcommittee of the Council on Nutrition, Physical Activity, and Metabolism; Council on Cardiovascular Nursing; and Council on Epidemiology and Prevention. Circulation 119: 902-907.
-
Xu J, Eilat-Adar S, Loria C, Goldbourt U, Howard BV, et al. (2006) Dietary fat intake and risk of coronary heart disease: the Strong Heart Study. Am J Clin Nutr 84: 894-902.
-
de Oliveira Otto MC, Wu JH, Baylin A, Vaidya D, Rich SS, et al. (2013) Circulating and dietary omega-3 and omega-6 polyunsaturated fatty acids and incidence of CVD in the Multi-Ethnic Study of Atherosclerosis. J Am Heart Assoc 2: 000506.
-
Abbasi F, McLaughlin T, Lamendola C, Kim HS, Tanaka A, et al. (2000) High carbohydrate diets, triglyceride-rich lipoproteins, and coronary heart disease risk. Am J Cardiol 85: 45-48.
-
Rimm EB, Ascherio A, Giovannucci E, Spiegelman D, Stampfer MJ, et al. (1996) Vegetable, fruit, and cereal fiber intake and risk of coronary heart disease among men. JAMA 275: 447-451.
-
Pereira MA, O'Reilly E, Augustsson K, Fraser GE, Goldbourt U, et al. (2004) Dietary fiber and risk of coronary heart disease: a pooled analysis of cohort studies. Arch Intern Med 164: 370-376.
-
Fung TT, Rimm EB, Spiegelman D, Rifai N, Tofler GH, et al. (2001) Association between dietary patterns and plasma biomarkers of obesity and cardiovascular disease risk. Am J Clin Nutr 73: 61-67.
-
Evans P, Halliwell B (2001) Micronutrients: oxidant/antioxidant status. Br J Nutr 2: S67-74.
-
Asplund K (2002) Antioxidant vitamins in the prevention of cardiovascular disease: a systematic review. J Intern Med 251: 372-392.
-
Jacobs DR Jr, Tapsell LC (2007) Food, not nutrients, is the fundamental unit in nutrition. Nutr Rev 65: 439-450.
-
Willett WC, (1998) Nutritional Epidemiology. Oxford University Press: New York, NY.
-
Al-Nuaim AR, (1997) Serum total and fractionated cholesterol concentration distribution and prevalence of hypercholesterolemia in urban and rural communities in Saudi Arabia. Int J Cardiol 58: 141-149.
-
Lutsey PL, Steffen LM, Stevens J (2008) Dietary intake and the development of the metabolic syndrome: the Atherosclerosis Risk in Communities study. Circulation 117: 754-761.
-
Centers for Disease Control, National Center for Chronic Disease Prevention and Health Promotion, (2003) Physical activity and good nutrition: essential elements to prevent chronic diseases and obesity 2003. Nutr Clin Care 6:135-138.





