Journal of Infectious Diseases and Epidemiology
A Meta-Analysis of Directly Observed Treatment vs. Self- Administered Therapy Outcomes in Pulmonary Tuberculosis Patients
Ardigleusa Alves Coêlho1,2, Ricardo Ney Oliveira Cobucci1,3*, Emannuela Maria Nunes Freitas2, Paulo Henrique Lima1, Ewerton Willian Gomes Brito1, Tânia Maria Ribeiro Monteiro de Figueiredo2, Ana Katherine da Silveira Gonçalves1 and Severina Alice da Costa Uchoa1
1Universidade Federal do Rio Grande do Norte, Natal, Brazil
2Universidade Estadual da Paraíba, Campina Grande, Brazil
3Universidade Potiguar, Natal, Brazil
*Corresponding author:
Ricardo Ney Oliveira Cobucci, PhD, Universidade Federal do Rio Grande do Norte and Universidade Potiguar, Natal, Brazil, E-mail: rncobucci@hotmail.com
J Infect Dis Epidemiol, JIDE-3-027, (Volume 3, Issue 1), Research Article; ISSN: 2474-3658
Received: October 17, 2016 | Accepted: March 07, 2017 | Published: March 10, 2017
Citation: Coêlho AA, Cobucci RNO, Freitas EMN, Lima PH, Brito EWG et al. (2017) A Meta-Analysis of Directly Observed Treatment vs. Self- Administered Therapy Outcomes in Pulmonary Tuberculosis Patients. J Infect Dis Epidemiol 3:027. 10.23937/2474-3658/1510027
Copyright: © 2017 Coêlho AA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A systematic review and meta-analysis were conducted in order to compare the effectiveness of directly observed therapy, short-course (DOTS) with self-administered treatment (SAT) in people with pulmonary tuberculosis. PubMed, Embase, ISI Web of Science, and the Scielo/Lilacs were searched for studies published between 1 January 1965 and 31 December 2013. Eleven studies were selected, including 14390 people with the following outcomes: cure, treatment completion or abandonment, and death. Results showed that approximately 22% more healing and completed treatment occurred among patients who underwent SAT (OR 1.22, 95% CI 1.07 to 1.40), while a lower treatment dropout rate was found in the group receiving DOTS (OR 0.68, 95% CI 0.56 to 0.83). Results did not detect a significant difference in the risk of death when comparing SAT and DOTS (OR 0.82, 95% CI 0.64 to 1.05). In the discussion, a reflection is made on what kind of treatment regimen is best suited to those infected by Mycobacterium tuberculosis and a discussion ensues on how to achieve better cure rates and less abandonment and mortality. It is concluded that when choosing a treatment regimen for patients, public programs are key to considering the dynamics of health services as well as the conditions and lifestyle of patients. The latter must also provide prevention, treatment and monitoring of infection, and have sufficient funding to train a health team and ascertain follow up of patients and families in order to attain the best success rates possible.
Keywords
Tuberculosis, Pulmonary tuberculosis, Treatment
Introduction
Tuberculosis (TB) still represents a serious problem in public health, expressed by approximately nine million new cases and 1.5 million deaths each year [1-3]. Studies also point to the fact that TB cure and disease control are seriously compromised by drop-out rates, as can be deduced by statistics on re-treatment, relapse, treatment dropout, drug resistance and death by TB [4-6]. Such to better TB treatment and control its spread, especially in countries with a high incidence, the WORLD HEALTH ORGANIZATION (WHO) has recommended a strategy since 1993 called Directly Observed Treatment Short-Course (DOTS). The latter involves four components: politically committed governments, improvement of laboratory diagnosis, supervised treatment with continuous supply of drugs and an information system to monitor and record appropriate treatment progress of patients and programs [2].
Treatment administered under the supervision or direct observation of a trained professional from initiation of treatment to cure, has become a key element leading to successful DOTS [3]. Studies show that by adopting DOTS more than 30 million TB patients have been treated, resulting in cure rates above 80% as well as reducing dropout rates by about 10% [4].
In 2006 the Global Plan to Stop TB recommended that DOTS become "standard treatment" under appropriate conditions. This treatment method has been shown to reduce the risk of drug resistance as well as support patients, thus resulting in increased adherence to treatment, and consequently, the possibility of cure [1]. Several studies support this statement [7-14].
This being said, the systematic review conducted by Volmink and Garner [15] showed no significant evidence supporting the routine use of DOTS over SAT when aiming to cure patients or at least complete the chosen treatment. In a recent meta-analysis, Karumbi and Garner [16] concluded that DOTS did not provide a solution to poor adherence in TB treatment. Several studies have not found DOTS to be the most efficient regimen for TB management [17,18]. DOTS has recently been questioned because its resulting completion rates seem equivalent to those of SAT. DOTS has been criticized as a passive model within public health services since it often only delivers the appropriate drugs without taking into account some important social components of the disease which may lead to a low success rate, social stigma, and lack of moral support by family members unwilling to modify living conditions and habits [18].
The fact that the literature boasts few studies or meta-analyses which result in significant levels of evidence to prove that one type of TB therapy is more effective than any other also leads to the importance of further investigating the comparative effectiveness of DOTS and other pulmonary TB management strategies. This systematic review and meta-analysis intends to compare the effectiveness of DOTS with SAT in the fight against pulmonary TB.
Methods
We followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [19]. We searched PubMed, Embase, ISI Web of Science, and the Scielo/Lilacs for studies published between 1 January 1965 and 31 December 2013. There was no exclusion of articles by language. Bibliographies of original articles, key reviews, and consensus statements were also searched for additional relevant studies. The following Medical Subject Heading terms and strategy was used: directly observed therapy or supervised therapy or directly observed treatment strategy or DOT or DOTS and self-administered therapy or self-supervised therapy OR unsupervised therapy and tuberculosis.
Inclusion criteria
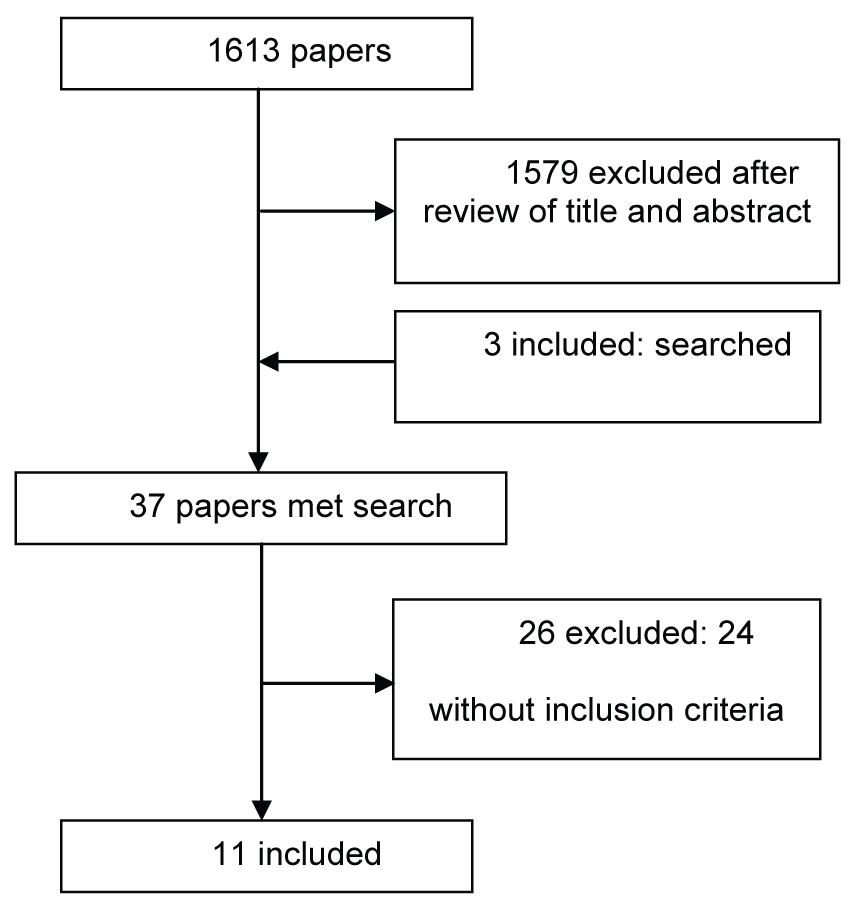
Three researchers (AAC, EWB and EMNF) began the process of selecting relevant studies by examining titles and abstracts using the following inclusion criteria: the studies were observational studies comparing pulmonary TB patients following the DOTS, or SAT regimens until the treatment was concluded or interrupted, the patients were healed, or died of TB. Studies that exclusively addressed extra pulmonary tuberculosis as well as qualitative studies were excluded. After evaluating titles and abstracts, 1579 articles were excluded (Figure 1). The outcomes cited above were classified according to the WHO definitions [20]:
.
Figure 1: Pubmed, Embase, ISI Web of science and the Scielo/Lilacs were searched for observational studies comparing pulmonary tuberculosis treatment.
View Figure 1
• Healed: Patient whom completed TB treatment which resulted in negative culture at the end of the treatment.
• Treatment completed: Patient completed treatment but did not meet the criteria for cure or failure. This definition applies to patients with pulmonary TB smear-positive and smear-negative cultures.
• Abandonment: Patient who took anti TB drugs for one month or more and interrupted treatment for two months or more.
• Death: Patient who died for any reason during anti TB treatment.
Thirty seven articles were read by the following researchers, AAC, PHL and SACU .It was determined that only studies which followed adult patients with pulmonary TB under DOTS or SAT with the following regimens would be considered: the first two months daily doses of four drugs were administered (isoniazid (INH), rifampin (RMP), pyrazinamide and ethambutol) followed by a four month maintenance phase of INH and RMP during which individuals were followed by a health professional. The outcomes included in the review were treatment completion, abandonment, cure and death.
Data extraction
The data was extracted independently by three researchers (AAC, PHL and SACU). In case of disagreement between the authors, a fourth researcher (RNOC) was consulted. The following data was extracted from the eleven selected studies (Figure 1): first author, year of publication, country where the study was conducted, period, the number of patients with pulmonary TB, number of losses, type of treatment and outcome (Table 1).
![]()
Table 1: Characteristics of studies selected for meta-analysis.
View Table 1
Analysis
The odds ratio (OR) was calculated by means of the Mantel-Haenszel method, using a confidence interval of 95%, while a chi-square test with a significance level of 5% was used to determine the heterogeneity between studies. All calculations were made with Review Manager 4.2.
Results
Eleven studies met the inclusion criteria [21-31]. The characteristics of the selected studies are listed in table 1. The outcome measures for comparison between DOTS and SAT were: cure, treatment completion or abandonment and death.
Cure and treatment completion
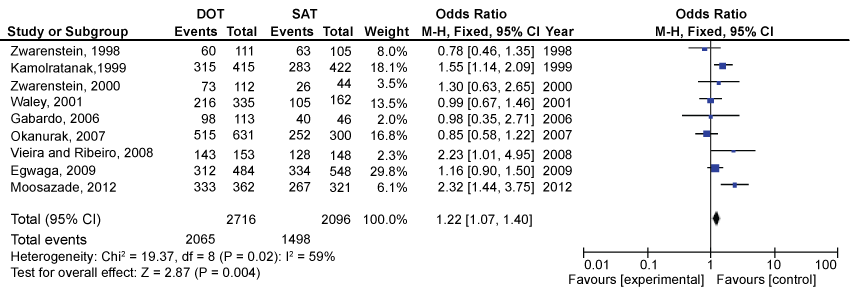
Of all the TB patients considered for this review, 2716 were followed within the DOTS regimen to measure cure rate and treatment completion, while 2096 were followed within the SAT regimen. From the DOTS group 2065 patients were considered cured or had completed the treatment, while in the SAT group 1498 subjects were assigned the same outcome. Data analysis revealed that approximately 22% more of the SAT patients were considered healed and completed treatment (OR 1.22, 95% CI 1.07 to 1.40) (Figure 2).
.
Figure 2: DOT versus SAT Odds Ratio for cure or complete treatment of tuberculosis.
View Figure 2
Abandonment
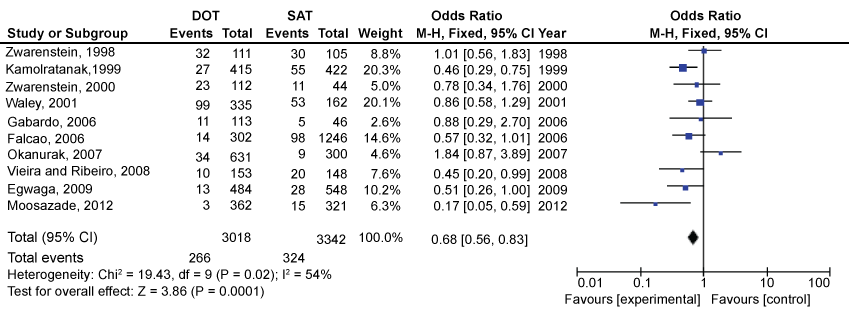
From the subjects included in this review, 3018 were followed within the DOTS regimen to measure the treatment abandonment rate and 3342 were followed within the SAT regimen. Results showed that 266 patients dropped out of DOTS while 324 left SAT. By comparison, the group receiving DOTS had a lower dropout rate, approximately 32% lower (OR 0.68, 95% CI 0.56 to 0.83) (Figure 3).
Death
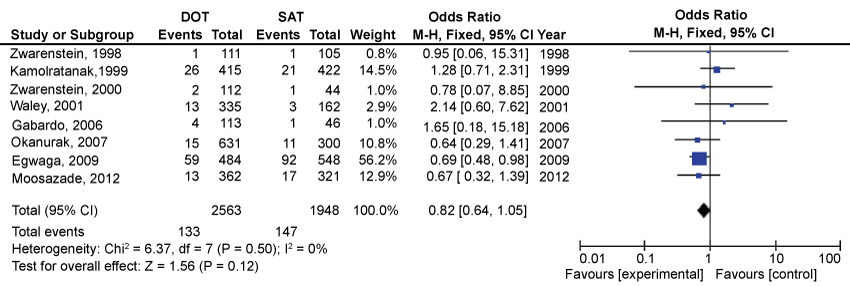
Of all the TB patients making up the sample, 2563 received the DOTS regimen and were followed to measure mortality rate, while 1948 received the SAT regimen under the same conditions. We found that among the DOTS group 133 deaths occurred, while 147 were counted in the SAT group. No significant difference was found in risk of mortality when both regimes were compared (OR 0.82, 95% CI 0.64 to 1.05) (Figure 4).
Discussion
DOTS, has long been defended as a highly effective strategy in the cure of pulmonary TB. It is said that patients adhere more easily to the regimen which consequently increases success rates in treatment [3,6].
However, DOTS has not clearly shown an increase in cure rates, reduced dropout rates or lower mortality, factors which would prove the efficiency of this type of therapy. Furthermore, few studies compare DOTS to SAT, blurring the picture even more.
The findings of this meta-analysis showed that treatment success, found only in the healed and completed treatment group, was more significant among patients under the SAT regimen (OR 1.22, 95% CI 1.07 to 1.40). Similar findings were also published by Volmink and Garner [15], who did not find that DOTS was significantly more effective than SAT, regarding cure or completed treatment (OR 1.06, 95% CI 1.00 to 1.13). Karumbi and Garner [16] showed that TB cure was low with SAT across all studies and direct observation did not substantially improve this (OR 1.08, 95% CI 0.91 to 1.27), while treatment completion showed a similar pattern, ranging from 59% to 78% in the self-treatment groups, and DOTS did not improve this (RR 1.07, 95% CI 0.96 to 1.19).
Even though these meta-analyses, has shown DOTS not to be more effective than SAT, several studies have done so. Charokopos, et al. [32], compared both regimens and found that patients receiving DOTS had the higher cure rate of the two. Elkomy, et al. [33], also published results supporting DOTS as the most effective treatment (P < 0.005). Steffen, et al. [34] supported DOTS as well by finding that DOTS treatments were completed more frequently than SAT. The favorable findings for DOTS in these studies may be explained by small sample sizes. Other factors may help increase the cure rate and treatment completion in the groups that received supervised therapy. It is important to note that treatment supervision is one of the pillars of the DOTS strategy; there may be differences in the quality of the supervision provided, considerably influencing the result represented by complete healing.
All countries where the studies included in this review were conducted have high incidence rates of TB. Two studies in particular observed better results in relation to healing when comparing DOTS with SAT [24,25], which leads us to seek an explanation for the increased success in the two countries Brazil and Thailand. The Brazilian Health System (Unified Health System - SUS) ensures universal access and public funding of health programs and services. Regarding TB control, a government program called the Family Health Strategy has decentralized diagnosis and supervised treatment in order to facilitate access and encourage patient adherence to TB treatment. In Thailand, the government invested in the public health system through disease prevention programs. Among these, the TB Control Program is well organized and effective. These results may be explained by the fact that the DOTS regimen has been efficiently implemented in these two countries, reinforcing the importance of government involvement. Studies carried out in Pakistan [21] and South Africa [22] showed no difference between SAT and DOTS regimens in terms of efficiency. Thus, it can be said that DOTS is only the most effective method when government funding is sufficient, casting a slight shadow over the WHO recommendation. This makes the DOTS regimen an expensive choice, especially in developing countries where government funding doesn't usually permit such extensive health programs. Quite possibly, DOTS is not economically feasible for developing countries, casting a favorable light on SAT, and a less expensive alternative.
A likely explanation for the limited effectiveness of DOTS is its lack of routine execution in regular health services in developing countries. Unlike the SAT, in which the patient takes responsibility for their treatment, implementation of DOTS depends on the commitment of the health professionals involved in the supervision of the TB patient. Often, there is lack of preparation, interest, and professionalism in health staff supervising the intake of drugs, due to work overload in the clinic and insufficient number of employees [35]. These situations contribute to undermine DOTS, neither prioritizing it nor making it effectively systematic, especially when performed in the patient's home. In addition, hardship can often reduce the possibility that patients will go to the clinic on a daily basis for DOTS, which does not favor adherence to treatment.
The higher rate of cure and complete treatment under unobserved regimen found in this meta-analysis suggests that SAT is more effective than DOTS. The factors mentioned above may explain this finding, even though WHO has recommended treatment under supervision as the best option for TB control.
In this study, a lower dropout rate for TB treatment was observed for the DOTS group (OR 0.68, 95% CI 0.56 to 0.83), confirming the findings of other studies that have shown reduced dropout treatment among patients with pulmonary TB and supervised therapy [36-38].
Treatment dropout is still one of the barriers to the effectiveness of TB treatment, especially in unsupervised patients [37]. Studies report the following risk factors associated with non-adherence in patients under supervised treatment: being of male gender, unaware of the importance of regular treatment, uses illicit drug, and of low economic status [36-38].
No significant difference in mortality was found when TB deaths between the two treatment groups (DOTS versus SAT) were analyzed (OR 0.82, 95% CI 0.64 to 1.05). However, the heterogeneity between studies was significant, possibly resulting from the inclusion of deaths from other causes in the calculation of mortality rates from TB.
A study in Taiwan [39], showed a reduction in all causes of mortality among patients with TB from 2006 to 2008, a period that corresponds to the increase of the DOTS regimen in Taiwan, and after controlling for confounding factors, the odds ratio of death among patients who received DOTS was 40% lower (OR 0.60, 95% CI 0.5 to 0.80) than for SAT. Bloss, et al. [40], contradicted the results of this systematic review when his 2012 study analyzed the risk of TB death during observed and unobserved treatment, and showed that in the unobserved group the risk of death increased significantly when compared to the observed group, OR 53.9, 95% CI 43.0-67.4 and OR 10.9, 95% CI 8.7-13.6 respectively. Again, these types of results are inconclusive since the inclusion of deaths from other causes entered in the calculation of mortality rates from TB, obscuring the picture, and preventing any definitive conclusion from being drawn.
We understand that DOTS is a relevant strategy for TB control, however, its relevance and effectiveness is greatly diminished if not implemented in a government program as WHO originally intended. Investment becomes necessary to train health professionals involved in the supervision of treatment as well as from their train of thought about TB treatment. Clinic and hospital staff should use common sense when considering the dynamics of health services as well as patient style and quality of life to give good advice on the most appropriate treatment regimen. Furthermore, the technical and financial health care resources allotted to TB control, together with the effective participation of the community and patients, can make a difference regardless of the treatment regimen used.
Our results incite reflection about whether we should simply be focusing on the type of therapy to be adopted by those infected with Mycobacterium TB to obtain better cure rates and less abandonment and mortality. However, further studies are needed, controlling for these potential biases, to determine the best strategy to increase patient adherence to treatment and achieve the effective results promised by DOTS, as recommended by WHO.
References
-
World Health Organization (2012) Global Tuberculosis Control-Report. Geneva, Switzerland.
-
World Health Organization (1999) What is DOTS? A Guide to Understanding the WHO-recommended TB Control Strategy Known as DOTS. Geneva, Switzerland.
-
World Health Organization (2002) An expanded DOTS frame work for effective tuberculosis control: Stop TB Communicable Diseases. Geneva, Switzerland.
-
Frieden TR, Sbarbaro JA (2007) Promoting adherence to treatment for tuberculosis: the importance of direct observation. Bull World Health Organ 85: 407-409.
-
Gazetta CE, Vendramini SH, Ruffino-Netto A, Oliveira MR, Villa TC (2007) Descriptive study of the implementation and impact of the directly observed treatment, short-course strategy in the São Josédo Rio Preto municipal tuberculosis control program (1998-2003). J Bras Pneumol 33: 192-198.
-
Chaulk CP, Kazandjian VA (1998) Directly observed therapy for treatment completion of pulmonary tuberculosis: Consensus Statement of the Public Health Tuberculosis Guidelines panel. JAMA 279: 943-948.
-
Siemion-Szcześniak I, Kuś J (2009) Treatment outcomes in culture positive pulmonary tuberculosis. Pneumonol Alergol Pol 77: 11-22.
-
Rusen ID, Aït-Khaled N, Alarcón E, Billo N, Bissell K, Boillot F, et al. (2007) Cochrane systematic review of directly observed therapy for treating tuberculosis: good analysis of the wrong outcome. Int J Tuberc Lung Dis 11: 120-121.
-
Van der Werf TS, Dade GK, Van der Mark TW (1990) Patient compliance with tuberculosis treatment in Ghana: factors influencing adherence to therapy in a rural service programme. Tubercle 71: 247-252.
-
Irurzun RN, Hasper I, Garcia LE (1990) Re-treatment from tuberculosis, non-compliance with previous treatment and its relationship with the same. Rev Argentinadel Torax 51: 17-30.
-
Moralez EMM, Montes VS, Perez GC, et al. (1993) Main causes of noncompliance with tuberculosis pulmonary treatment. Gaceta Medicade Mexico 129: 57-62.
-
Almeida SAD, Honer MR (2006) Non compliance with tuberculosis treatment in to the reference units in Campo Grande, MS-2002 e 2003. Bol Pneumol Sanit 14: 167-171.
-
Xu W, Lu W, Zhou Y, Zhu L, Shen H, et al. (2009) Adherence to anti-tuberculosis treatment among pulmonary tuberculosis patients: a qualitative and quantitative study. BMC Health Serv Res 9: 169.
-
Bagchi S, Ambe G, Sathiakumar N (2010) Determinants of Poor Adherence to Anti-Tuberculosis Treatment in Mumbai, India. Int J Prev Med 1: 223-232.
-
Volmink J, Garner P (2007) Directly observed therapy for treating tuberculosis. Cochrane Database Syst Rev CD003343.
-
Karumbi J, Garner P (2015) Directly observed therapy for treating tuberculosis. Cochrane Database Syst Rev CD003343.
-
Pasipanodya JG, Gumbo T (2013) A meta-analysis of self-administered vs directly observed therapy effect on microbiologic failure, relapse, and acquired drug resistance in tuberculosis patients. Clin Infect Dis 57: 21-23.
-
Mangura B, Napolitano E, Passannante M, Sarrel M, McDonald R, et al. (2002) Directly observed therapy (DOT) is not the entire answer: an operational cohort analysis. Int J Tuberc Lung Dis 6: 654-661.
-
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339: b2535.
-
http://whqlibdoc.who.int/publications/2010/9789241547833_eng.pdf.
-
Walley JD, Khan MA, Newell JN, Khan MH (2001) Effectiveness of the direct observation component of DOTS for tuberculosis: a randomised controlled trial in Pakistan. Lancet 357: 664-669.
-
Zwarenstein M, Schoeman JH, Vundule C, Lombard CJ, Tatley M (2000) A randomised controlled trial of lay health workers as direct observers for treatment of tuberculosis. Int J Tuberc Lung Dis 4: 550-554.
-
Zwarenstein M, Schoeman JH, Caesar V, Lombard CL, Tatley M (1998) Randomised controlled trial of self-supervised and directly observed treatment of tuberculosis. Lancet 352: 1340-1343.
-
Kamolratanakul P, Sawert H, Lertmaharit S, Kasetjaroen Y, Akksilp S, et al. (1999) Randomized controlled trial of directly observed treatment (DOT) for patients with pulmonary tuberculosis in Thailand. Trans R Soc Trop Med Hyg 93: 552-557.
-
Falcao AB (2006) Estudo comparativodo tratamento supervisiona doda tuberculose comoauto administrado. Bol Pneumol Sanit 14: 21-25.
-
Gabardo BMA (2006) Assessement of the effectiveness of supervised treatment in the control of pulmonary tuberculosis in Curitiba-PR. Bol Pneumol Sanit 14: 91-97.
-
Vieira AA, Ribeiro SA (2008) Noncompliance with tuberculosis treatment involving self-administration of treatment or the directly observed therapy, short-course strategy in a tuberculosis control program in the city of Carapicuíba, Brazil. J Bras Pneumol 34: 159-166.
-
Okanurak K, Kitayaporn D, Wanarangsikul W, Koompong C (2007) Effectiveness of DOT for tuberculosis treatment outcomes a prospective cohort study in Bangkok, Thailand. Int J Tuberc Lung Dis 11: 762-768.
-
Anuwatnonthakate A, Limsomboon P, Nateniyom S, Wattanaamornkiat W, Komsakorn S, et al. (2008) Directly Observed Therapy and Improved Tuberculosis Treatment Outcomes in Thailand. PLoS One 3: e3089.
-
Egwaga S, Mkopi A, Range N, Haag-Arbenz V, Baraka A, et al. (2009) Patient-centred tuberculosis treatment delivery under programmatic conditions in Tanzania: a cohort study. BMC Med 7: 80.
-
Moosazade M, Jamshidi M, Amiresmaili M, Nezammahalleh A (2012) A Comparison of Directly Observed Therapy and Self-Administered Therapy Strategies in Treatment of Pulmonary Tuberculosis: A Cohort Study in North of Iran. Middle-East Journal of Scientific Research 11: 873-880.
-
Charokopos N, Tsiros G, Foka A, Voila P, Chrysanthopoulos K, et al. (2013) Modified directly observed treatment for tuberculosis versus self-administered therapy: an observational study in rural Greece. Rural Remote Health 13: 2114.
-
Elkomy H, Awad M, El-Shora A, Elsherbeni B (2013) Assessment of the efficacy of Directly Observed Treatment with shortcourse (DOTS) for pulmonary tuberculosis in Sharkia governorate, Egypt. J Chest Dis Tuberc 62: 257-261.
-
Steffen R, Menzies D, Oxlade O, Pinto M, de Castro AZ, et al. (2010) Patients costs and cost-effectiveness of tuberculosis treatment in DOTS and non-DOTS facilities in Riode Janeiro, Brazil. PLoS One 5: e14014.
-
Queiroz EM, De-La-Torre-Ugarte-Guanilo MC, Ferreira KR, Bertolozzi MR (2012) Tuberculosis: limitations and strengths of Directly Observed Treatment Short-Course. Rev Lat Am Enfermagem 20: 369-377.
-
Paz LN, Ohnishi MD, Barbagelata CM, Bastos Fde A, Oliveira JA 3rd, et al. (2012) Effectiveness of tuberculosis treatment. J Bras Pneumol 38: 503-510.
-
Thiam S, LeFevre AM, Hane F, Ndiaye A, Ba F, et al. (2007) Effectiveness of strategy to improve adherence to tuberculosis treatment in are source poor setting. JAMA 297: 380-386.
-
Kulkarni P, Akarte S, Mankeshwar R, Bhawalkar J, Banerjee A, et al. (2013) Non-Adherence of New Pulmonary Tuberculosis Patients to Anti-Tuberculosis Treatment. Ann Med Health Sci Res 3: 67-74.
-
Yen YF, Rodwell TC, Yen MY, Shih HC, Hu BS, et al. (2012) DOT associated with reduced all-cause mortality among tuberculosis patients in Taipei, Taiwan, 2006-2008. Int J Tuberc Lung Dis 16:178-184.
-
Bloss E, Chan PC, Cheng NW, Wang KF, Yang SL, et al. (2012) Increasing directly observed therapy related to improved tuberculosis treatment outcomes in Taiwan. Int J Tuberc Lung Dis 16: 462-467.