Journal of Infectious Diseases and Epidemiology
Lemierre's Syndrome without Internal Jugular Vein Thrombophlebitis: A Diagnostic Conundrum
Gbolahan O Ogunbayo*, Josephine Adunse, Odunayo Olorunfemi and Nashwa Abdulsalam
Department of Internal Medicine, Rochester General Hospital, Rochester, NY, USA
*Corresponding author:
Gbolahan Ogunbayo, Department of Internal medicine, Rochester General Hospital, 1425 Portland Avenue, Rochester, NY 14621, USA, Tel: +17735017532, E-mail: Gbolahan.ogunbayo@rochesterregional.org
J Infect Dis Epidemiol, JIDE-2-017, (Volume 2, Issue 2), Case Report; ISSN: 2474-3658
Received: April 25, 2016 | Accepted: August 13, 2016 | Published: August 16, 2016
Citation: Ogunbayo GO, Adunse J, Olorunfemi O, Abdulsalam N (2016) Lemierre's Syndrome without Internal Jugular Vein Thrombophlebitis: A Diagnostic Conundrum. J Infect Dis Epidemiol 2:017. 10.23937/2474-3658/1510017
Copyright: © 2016 Ogunbayo GO, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
In 1936 André Lemierre described a disease entity with septicemia that occurs days after a sore throat, pyrexia and rigors along with pulmonary infarcts and arthritic manifestations [1]. Over the years many authors have included internal jugular vein thrombosis or septic thrombophlebitis as an integral part of this disease entity now known as Lemierre's syndrome [2-4]. We report a case that typifies Lemierre's syndrome but without clinical or radiographic evidence of internal jugular vein pathology.
Case Report
A previously healthy 23-year-old male presented with fever and shortness of breath. His illness initially started six days before presentation with a sore throat. Two days later he developed fevers with associated chills, rigors, and night sweats. He also complained of myalgias, non-productive cough, a right-sided chest pain, and shortness of breath on exertion, as well as nausea, vomiting, abdominal pain, and diarrhea. His symptoms continued to worsen until he became dyspneic at rest and was brought to our medical center.
On examination he was ill-looking, his temperature was 100.9°F, blood pressure 99/54 mmHg, heart rate 101 beats per minute, and respiratory rate was 28 breaths per minute. He appeared anxious and his peripheral capillary oxygen saturation by pulse oximetry was 97% on room air. He was jaundiced, with an erythematous oropharynx, cervical lymphadenopathy, and right chest tenderness, with bilateral rales and right upper quadrant abdominal tenderness.
His initial labs were significant for a white blood cell count of 20,500/uL, with neutrophilic predominance and a platelet count of 58,000/uL. He was also had a sodium of 129 mEq/L, creatinine of 1.9 mg/dL, lactate of 6.4 mmol/L and elevated liver enzymes: AST of 91 U/L; ALT of 64 U/L and APLP of 177 U/L and a total bilirubin of 6.7 mg/dL with a direct bilirubin of 5.8 mg/dL. His arterial blood gas about three hours after initial presentation revealed hypoxemia of 77 mmHg (normal 80-100 mmHg) and his chest radiograph revealed bilateral pulmonary nodules likely representing septic emboli (Figure 1). A computed tomography with contrast enhancement further characterized these lesions as cavitary (Figure 2). Work up for infective endocarditis with transthoracic and transesophageal echocardiograms were negative.
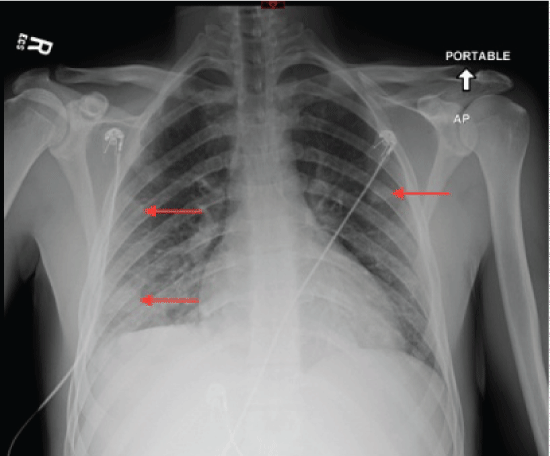
.
Figure 2: CT scan: Computed Tomography of chest showing pulmonary lesions with cavitation.
View Figure 2
He subsequently decompensated, developing respiratory failure and septic shock and was incubated and started on vasopressors: Norepinephrine, Phenylephrine and Vasopressin with good effect. He also received broad-spectrum intravenous antibiotics including Vancomycin, Cefepime and Flagyl. Based on the chronology of his symptoms and clinical findings, Lemierre's disease was suspected but an ultrasound and computed tomography of his neck and soft tissue were negative for internal jugular vein pathology. His blood cultures later grew Fusobacterium necrophorum in both anerobic bottles for which he completed three weeks Ceftriaxone and Flagyl. His clinical course was complicated by empyema requiring thoracentesis and Video-Assisted Thoracoscopic Surgery (VATS) where lung decortication and evacuation of empyema and pleural fluid was performed. He clinically improved, was extubated, and weaned off all vasopressors. He was discharged in good health thirty-one days after admission.
Discussion
The incidence of Lemierre's disease in different populations is quoted to be between 0.55 cases per 100,000 to 14.4 cases per million per year [5,6]. It occurs most frequently in young healthy adults and has an overall mortality of 9 to 11% [5,6]. Although the definition of Lemierre's disease was set in the 1930s, a variety of interpretations continue to exist on whether internal jugular vein presenting as either thrombosis or thrombophlebitis should be required to make a diagnosis [1,2,4,5,7,8]. F. necrophorum is generally not considered a normal flora in the oropharynx, therefore it is generally believed that F. necrophorum septicemia in the setting of angina illness or compatible clinical findings and septic emboli or metastatic lesions can be considered as Lemierre's disease [2,8,9]. There have been sparse reports of Lemierre's disease without internal jugular vein pathology on ultrasound, computed tomography or magnetic resonance imaging in literature [10-14].
To our knowledge the reason for this variation remains unclear although literature has ascribed a change in presentation and incidence to the advent of antibiotics [15]. The prognosis of Lemierre's disease with or without evidence of thrombosis or thrombophlebitis is comparable [16]. As such, absence of internal jugular vein pathology as in our patient should not preclude making the diagnosis and initiating appropriate treatment for this condition, as therapeutic inertia may be fatal.
Funding
None.
Conflict of Interest
None.
Authorship
All authors had access to the data and a role in writing this manuscript.
References
-
Lemierre A (1936) On Certain Septicæmias due to Anaerobic Organisms. Lancet 227: 701-703.
-
Riordan T (2007) Human infection with Fusobacterium necrophorum (Necrobacillosis), with a focus on Lemierre's syndrome. Clin Microbiol Rev 20: 622-659.
-
Karkos PD, Asrani S, Karkos CD, Leong SC, Theochari EG, et al. (2009) Lemierre's syndrome: A systematic review. Laryngoscope 119: 1552-1559.
-
Goldenberg NA, Knapp-Clevenger R, Hays T, Manco-Johnson MJ (2005) Lemierre's and Lemierre's-Like Syndromes in Children: Survival and Thromboembolic Outcomes. Pediatr 116: e543-e548.
-
Hagelskjaer Kristensen L, Prag J (2008) Lemierre's syndrome and other disseminated Fusobacterium necrophorum infections in Denmark: a prospective epidemiological and clinical survey. Eur J Clin Microbiol Infect Dis 27: 779-789.
-
Afra K, Laupland K, Leal J, Lloyd T, Gregson D (2013) Incidence, risk factors, and outcomes of Fusobacterium species bacteremia. BMC Infect Dis 13: 264.
-
Jones JW, Riordan T, Morgan MS (2001) Investigation of postanginal sepsis and Lemierre's syndrome in the South West Peninsula. Commun Dis Public Health 4: 278-281.
-
Ramirez S, Hild TG, Rudolph CN, Sty JR, Kehl SC, et al. (2003) Increased diagnosis of Lemierre syndrome and other Fusobacterium necrophorum infections at a Children's Hospital. Pediatrics 112 : e380.
-
Huggan PJ, Murdoch DR (2008) Fusobacterial infections: clinical spectrum and incidence of invasive disease. J Infect 57: 283-289.
-
De Vos AI, van Rossem RN, van Elzakker EP, Nijhuis-Heddes JM, Maartense E (2001) Lemierre's syndrome. Sepsis complicating an anaerobic oropharyngeal infection. Neth J Med 59: 181-183.
-
Yousem DM, Scatarige JC, Gayler BW, Siegelman SS (1985) CT demonstration of postanginal sepsis. J Otolaryngol 14: 333-335.
-
http://www.icm.tn.gov.in/caseround/caseround2.htm.
-
Hirschel B, Allaz AF, Siegrist CA (1983) Anaerobic septicemia following oropharyngeal infections (Lemierre's postanginal septicemia): a forgotten syndrome. Schweiz Med Wochenschr 113.
-
Brocard H, Guibe C (1957) Septicemias caused by Bacillus funduliformis. Rev Prat 7: 1285-1286.
-
Eilbert W, Singla N (2013) Lemierre's syndrome. Int J Emerg Med 6: 40.
-
Boharas S (1943) Postanginal Sepsis. Arch Intern Med 71: 844.