Journal of Infectious Diseases and Epidemiology
Legionella's Pneumoniae: A New Outbreak in Spain and Urinary Antigen Test Review
Soraya Jodra Sánchez1*, Jacinto Ramos González1, María Teresa Santos Jiménez2, Rosa Cordovilla Pérez1, Jose María González Ruíz1, Ana María Sánchez Hernández1, Sergio Cadenas Menéndez1 and Miguel Barrueco Ferrero1
1Department of Pneumology, Salamanca University Hospital, Spain
2Department Data Documentation, Salamanca University Hospital, Spain
*Corresponding author:
Soraya Jodra Sánchez, Department of Pneumology, Salamanca University Hospital, Biomedical Research Institute of Salamanca (IBSAL), Paseo de San Vicente 58, 37007 Salamanca, Spain, Tel: 923 29 11 00, Fax: 923 29 11 39, E-mail: sorayajodra_9@hotmail.com
J Infect Dis Epidemiol, JIDE-2-007, (Volume 2, Issue 1), Short Review; ISSN: 2474-3658
Received: January 21, 2016 | Accepted: February 25, 2016 | Published: February 27, 2016
Citation: Sánchez SJ, González JR, Jiménez MTS, Pérez RC, Ruíz JMG, et al. (2016) Legionella's Pneumoniae: A New Outbreak in Spain and Urinary Antigen Test Review. J Infect Dis Epidemiol 2:007. 10.23937/2474-3658/1510007
Copyright: © 2016 Sánchez SJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Precedent: Legionella pneumophila pneumonia is an endemic disease which it can presents as recurrent outbreaks.
Methods: Descriptive retrospective analysis which included all patients with Legionaire's disease (LD) diagnosed due to an outbreak in Salamanca between February (just one patient in September) to March 2015.
Results: We analysed 14 hospitalized patients, 8 patients (57%) were males. Middle age 64.71 ± 16.31 years. Seven patients (50%) presented two or more associated comorbidities. The insolated fever was the principal consulting in Emergency Department in 8 patients (57%). The principal radiological finding was bilateral pneumonia in 5 patients (35.7 %).
Conclusions: LD dueto the Legionella pneumophila species constitutes a common pneumonia cause although many times underdiagnosed. A better investigation of this disease will do an exactly epidemiological knowledge.
Keywords
Legionella pneumophila, Legionaire's disease (LD)
Introduction
Since the microorganism Legionella pneumophila (Lp) was identified during an American Legion Convention in Philadelphia in 1976, it has been recognised as a common cause of both extra- and intra-hospital pneumonia [1]. The incidence of community-associated pneumonia (CAP) due to Lp varies widely from one area to another, hovering around 1% in subjects treated on an outpatient basis and 15-28% in hospitalised patients. Of these, approximately a quarter require admission to an intensive care unit (ICU) [2].
In the latest guidelines of the American Thoracic Society on CAP, Lp is highlighted as the fifth most common cause of hospitalisation, and the third most common cause of admission to the ICU. These guidelines establish that different diagnostic tests are needed to identify the specific causal agents of pneumonia. This is due to the changes in antibiotic coverage and the epidemiological implications involving some etiologies, as in the case of Lp, where the “sentinel case” is of paramount importance for an early detection of an epidemic outbreak, , but the guidelines do not establish a need for routine employment of p urinary antigen test [3,4].
This is a retrospective study in which we have analysed the clinical and radiologic features and the results of laboratory tests of all patients who presented with CAP secondary to Lp infection during the outbreak in the province of Salamanca (Spain) between September 2014 and March 2015.Salamanca University Hospital attends 300,000 habitants and has a total of 989 beds. We have also reviewed the urinary antigen test indications and considered it benefit as a routine test for the cases of Lp pneumonia.
Methods
The variables analysed for each patient were: demographics (age, sex), toxic habits (smoking and drinking), comorbidities, reason for going to the Emergency Department (ER), vital signs at the ER, chest involvement in X-ray and laboratory results (leukocytes, C-reactive protein (CRP), procalcitonin (PCT), serum sodium, partial pressure of oxygen- PO2), microbiological results (urinary antigen test, sputum and blood cultures), and clinical outcome. Statistical analysis was performed using SPSS version 20.0.
Results
From September 2014 to March 2015 14 patients with pneumonia or Legionaire's disease (LD) were hospitalised. Of these, 8 (57%) were men and 6 (43%) were women, with a mean age of 64.71 ± 16.31 years (range: 31-92). Eight patients were smokers (57%) and one (7.1%) had a drinking habit. The main comorbidities were Systemic Arterial Hypertension (6 patients; 42.85%), Atrial Fibrillation (3 patients; 21.4%), Diabetes Mellitus (2 patients; 14.28%), Hypothyroidism (2 patients; 14.28%), and Chronic Obstructive Pulmonary Disease (2 patients; 14.28%). Seven patients (50%) presented two or more comorbidities, three (21.42%) only one comorbidity, and four (28.57%) none.
Isolated fever was the reason for going to the ER in 8 of the 14 patients (57%). The other motives for consultation are summarised in table 1. Seven patients (50%) had already been administered some type of antibiotic treatment (either at the ER or as an outpatient at their Primary Care Centre), and three (21.3%) had already visited the ER in the days just before hospitalisation.
![]()
Table 1: Motive for consultation.
View Table 1
The vital signs in Emergency were: medium axilar temperature 37.87 ± 1.18°C (range: 36.2-39.8°C) and oxygen saturation with pulse oximetry: 90.62 ± 3.94 % (range: 83-96%).
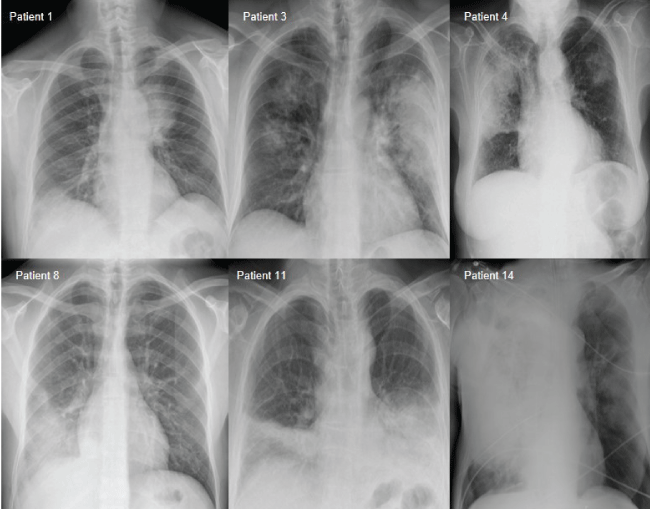
The radiological findings were: 5 patients (35.7 %) presented a bilateral pneumonia, 3 (21.4%) bilobar unilateral pneumonia, 4 (28.6%) right lower lobe pneumonia lobar and 2 (14.3%) in right upper lobe. The figure 1 shows different radiographs corresponding to the 1, 3, 4, 8, 11 and 14 patients.
The medium analytics parameters were: leukocytes 16,602.50 ± 10,016.61 μL (range: 7,000-46,220), natremy 133.21 ± 4.6 mmol/L (range: 122-140), CRP 44.36 ± 8.9 mg/dl (range: 26.6-61.2) and PCT (requested in 11 of the 14 patients) 4.02 ± 5.10 ng/ml (range: 0.4-17.42) and medium PO2 (requested in 9 of the 14 patients): 58.56 ± 15.18 mmHg (range: 40-92).
Four patients (28.5%) were assessed in the ER by the ICU team, two of whom were immediately admitted to the Unit due to the severity of their condition. Both required endotracheal intubation.
In the first intention, the most common antibiotic coverage was defined: ceftriaxone and levofloxacin (5 patients; 35.7%) and amoxicillin-clavulanic (2 patients; 14.3%). After microbiological confirmation of Lp, levofloxacin was prescribed for all patients.
The presence of Lp antigen in urine test was confirmed in all patients. Among the six (42.8%) for whom a sputum sample was taken, presence of the germ was confirmed in only one (7.1%) with no isolation of other germs. The average stay in hospital was 15.64 ± 27.98 days (range: 3-112). Outcome was favourable for all patients.
Conclusions
We believe it is of interest to describe the hospitalised cases of LD that occurred in our province. Sanitary Authorities were finally successful in detecting the source of the outbreak (a cooling tower) in one main street of the city and were able to take appropriate measures to prevent new infections. (How source of the outbreak was detected? Same Legionella pneumophila strain in all patients and in the cooling tower? What method was used? It is important for prevention services and doctors to know the quickest and most suitable method. (i) the right to request samples; (ii) to be sure of the origin of the epidemic.). Note: We have no information about this.
The clinical features and results from additional tests that we report are similar to those described in the literature [5-8]. From a radiological point of view, bilateral pneumonia was the most common finding. It is true that while there is no typical radiological feature for pneumonia caused by Lp patchy unilobar involvement that progresses to consolidation and the ground-glass pattern are often characteristic. However, in our revision, bilateral pneumonia prevailed [9,10].
One question that remains is that one patient presented with this infection in September 2014, while the rest of the cases occurred between February and March 2015. This individual required admission to the ICU for 49 days, and the diagnosis of Lp infection was reached during their stay. This could have been an isolated case, unrelated to the outbreak, or there could have been other cases that might have gone unnoticed (Pontiac fever) prior the peak of incidence, prompting urinary antigen test to be routinely tested in all pneumonia cases in our hospital when the outbreak was recognised has enabled the detection of new cases. This is, however, only a hypothesis.
(In our hospital, for each patient with pulmonary signs, a urinary antigen test, a Legionella culture and a qPCR are routinely made from sputum or bronchoalveolar lavage).
Note: "reference 3": clinical indications for UAT: ICU admission, failure of outpatient antiobiotic therapy, active alcohol abuse, recent travel and/or pleural effusion The guidelines not establish this routinely test, so in our hospital don´t apply the test out of these cases.
In a publication from our working group that was recently accepted for publication as an editorial in the journal Medicina Clínica (in press), we discussed the indications of urinary antigen test (there are already a number of publications about this!, NO: [Epub ahead of print].). The article discusses whether p antigen test should routinely be tested for (provided there is availability) for all cases of pneumonia, taking into account the cost-effectiveness ratio of the analysis (in our hospital it costs 5.80 euros). The test would assist in the diagnosis of Lp pneumonia which may otherwise go unnoticed, and would improve the administration of antibiotics, increase compliance, and reduce costs. In addition, it would have importance as a "sentinel" for early detection of outbreaks [11,12].
In conclusion, LD can present epidemically by sporadic outbreaks. This would prevent or delay the raising of a health alarm, a process that would avoid new cases by immediately prioritising the search for the source of the infection. Although only a hypothesis, this is probably what happened in Salamanca from September 2014 to February 2015, leading to us considering the routine testing for Lp urinary antigen test a in any incidence of CAP.
References
-
McDade JE, Shepard CC, Fraser DW, Tsai TR, Redus MA, et al. (1977) Legionnaires' disease: isolation of a bacterium and demonstration of its role in other respiratory disease. N Engl J Med 297: 1197-1203.
-
Rodríguez de Castro F, Zalacaín Jorge R (2010) Neumología adquirida en la comunidad En Álvarez-Sala Walther JL. In: Casan Clará P, Rodriguez de Castro F, Rodríguez Hermosa J.L, Villena Garrido V, Neumología Clínica. Barcelona, Elsevier.
-
Mandell L, Wunderink R, Anzueto A, Bartlett J, Douglas G, et al. (2007) Infectious Diseases Society of America/American Thoracic Society Consensus Guidelines on the Management of Community-Acquired Pneumoniain Adults. Clin Infect Dis 44: S27-S72.
-
Dirou S, Cazanave C (2015) [Urine antigen testing: Indication and contribution to the treatment of community-acquired pneumonia]. Rev Mal Respir 32: 845-849.
-
Ramon Duch F, Ruiz de Porras L, Elizalde G, Abellà M (1997) [Description and study of the etiology of a community outbreak of atypical pneumonia in L'Espluga de Francolí, Tarragona]. Med Clin (Barc) 108: 490-494.
-
Álvarez J, Oyaga N, Escofet A, Codony F, Orcau A, et al. (2001) Community-acquired legionellosis in the Barcelona region between 1992 and 1999: epidemiological characteristics and diagnostic methods. Med Clin (Barc) 117: 495-496.
-
Fernández JA, López P, Orozco D, Merino J (2002) Clinical study of an outbreak of Legionnaire's disease in Alcoy, Southeastern Spain. Eur J Clin Microbiol Infect Dis 21: 729-735.
-
Jericó Alba C, Nogués Solán X, Santos Martínez M.J, Félez Florb, M, Garcés Jarquea, et al. (2004) Legionella pneumophila pneumonia community epidemic outbreak in Barcelona: " The Barceloneta outbreak". Effect of the early diagnosis and treatment. Rev Clin Esp 204: 70-74.
-
Kim KW, Goo JM, Lee HJ, Lee HY, Park CM, et al. (2007) Chest computed tomographic findings and clinical features of legionella pneumonia. J Comput Assist Tomogr 31: 950-955.
-
Tan MJ, Tan JS, Hamor RH, File TM Jr, Breiman RF (2000) The radiologic manifestations of Legionnaire's disease. The Ohio Community-Based Pneumonia Incidence Study Group. Chest 117: 398-403.
-
Jodra Sánchez S, Barrueco Ferrero M (2015) Legionella's pneumonia. When is useful the urinary antigen test? Med Clin (Barc).
-
National Institute for Health and Care Excellence (2014) Pneumonia: Diagnosis and management of community- and hospital-acquired pneumonia in adults.