Journal of Infectious Diseases and Epidemiology
Factors Associated with Changes in HIV-Testing Uptake among Young Women (15-24 Years) in Tanzania: Analysis of 2003-04, 2007-08 and 2011-12 Tanzania HIV/AIDS and Malaria Indicator Survey
Michael J. Mahande* Habib O Ramadhani and Rune N Phimemon
Kilimanjaro Christian Medical Centre, Tanzania
*Corresponding author:
Michael Mahande, Department of statistics, Kilimanjaro Christian Medical Centre, Tanzania, E-mail: jmmahande@gmail.com
J Infect Dis Epidemiol, JIDE-1-001, (Volume 1, Issue 1), Research Article; ISSN: 2474-3658
Received: June 28, 2015 | Accepted: July 14, 2015 | Published: July 16, 2015
Citation: Mahande MJ, Ramadhani HO, Phimemon RN (2015) Factors Associated with Changes in HIV-Testing Uptake among Young Women (15-24 Years) in Tanzania: Analysis of 2003-04, 2007-08 and 2011-12 Tanzania HIV/AIDS and Malaria Indicator Survey. J Infect Dis Epidemiol 1:001. 10.23937/2474-3658/1510001
Copyright: © 2015 Mahande MJ. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
HIV counselling and testing (HTC) is an integral component of HIV preventive strategies. Despite an increase in the number of HTC sites, HIV testing uptake among young women in Tanzania is relatively low compared to other countries in Sub-Saharan Africa. This study aimed to explore the factors associated with changes in HIV testing uptake using Tanzania HIV/AIDS and Malaria Indicator Surveys of 2003-04, 2007-08 and 2011-12.
This was a secondary data analysis using the 2003-04 Tanzanian HIV/AIDS Indicator Survey (THIS), and the 2007-08 and 2011-12 Tanzanian HIV/AIDS and Malaria Indicator Surveys (THMIS). The study population consisted of young women 15 - 24 years old at the time of each survey. Using a pooled logistic regression we identified factors associated with HIV testing uptake during the study period. Multivariate decomposition analysis was used to assess factors associated with the changes in HIV testing uptake over the survey period.
HIV testing uptake among this population was 6.6%, 30.8% and 39.8% for 2003-04, 2007-08 and 2011-12 surveys respectively. Independent of other covariates, the time period of the survey has an important effect on uptake of HIV testing. Women's age (20-24 years), education level (primary & secondary), ever married, number of life sex partners (1 or more),having STI or symptoms of STI and attendance to antenatal care were significantly associated with higher odds of HIV testing across both sets of pooled surveys. Changes in characteristics of the sub-populations (endowments) in 2003-04 vs 2007-08 surveys would have resulted in low HIV testing uptake (-5.26%) in the absence of the changes in effects of these characteristic which contributed most of the changes in HIV testing uptake; (105.26%). In 2007-08 vs 2011-12 surveys, the changes in endowments contributed to 21.1% of the changes in HIV testing uptake, while 77.9% of the changes were attributed to coefficients. Both endowments and coefficients were statistically significant in both of the multivariate decomposition models.
HIV testing has been greater among women with high risk factors, and thus has become more targeted. Until testing is universal, an effective expansion strategy would be to prioritize those most likely to be infected.
Keywords
HIV testing, Uptake
Introduction
Approximately 35.3 million people were estimated to be HIV infected by 2012 [1]. Increased Anti-Retroviral Therapy (ART) coverage led to the decline in morbidity and mortality related to HIV and its associated opportunistic infections [2-4]. Reports showed a global decline in HIV epidemics among general populations [5]. Despite these successes, variation in HIV testing uptake across the regions exists [6]. For example in 2010, in Burundi, Tanzania and Rwanda, HIV testing uptake among men and women was 37%, 55% and 75% respectively [7], suggesting that the context in which the person lives may have an influence on HIV testing uptake.
HIV counselling and testing (HTC) is an integral component of HIV preventive strategies. Studies using mathematical models revealed that about 50 percent of the new HIV infections are from HIV infected persons unaware of their HIV status, making it difficult combating the infection [8]. While early diagnosis and treatment is associated with good treatment outcomes [7], delayed diagnosis and treatment increases disease burden and represents missed opportunity for prevention [9,10]. Knowing one's HIV status may influence change in personal behavior, a critical piece in HIV preventive efforts [11,12]. Individuals tested positive for HIV are likely to be linked to HIV care and treatment. Among the benefits of linking patients in HTC includes reduction of mother to child transmission, preventing uninfected partners, improving quality of life, reducing morbidity and mortality related to opportunistic infections and reduction in the frequency of hospitalizations [13]. High cost associated with the management of HIV infected patients underscores the importance of addressing HIV preventive efforts [14]. The concept of test and treat has been explored and it was documented that receiving HIV treatment was associated with 96% reduction in the new infections among sero-discordant couples; these findings highlight the need to increase HIV testing uptake and treatment [15]. Furthermore, one of the prevailing concepts of HIV prevention effort is through increasing the number of patients being tested and treated. Increasing those receiving ART in the population reduces community viral load (CVL). The idea behind reducing CVL is that as the number of individuals being tested and receive ART increases, greater numbers of HIV-infected persons will be virologically suppressed, leading to reduced CVL, and consequently, reduced incidence of HIV infection in the general population [16].
Tanzania is one of the sub-Saharan countries heavily affected by the HIV epidemic. According to the HIV/AIDS and Malaria Indicator survey 2007-08, the HIV prevalence was reported to decline from 7.0% in 2004 to 5.8% in 2008. Decreases were greatest among men in the urban areas but the overall change in HIV prevalence was not statistically significant [17]. A more recent survey 2011-12indicated an overall decline in the national HIV prevalence from 5.8% in 2007-08 survey to 5.1% though this decline was also not statistically significant [18]. Despite the success in the decline of HIV prevalence by the year 2012, only 62% and 47% women and men aged 15-49 years respectively have ever tested for HIV and received their results, leaving a large proportion of persons unaware of their HIV status [19]. Higher levels of HIV testing uptake are needed in a test and treat models if reduction in HIV incidence is to be realized [20-22].
The principal focus of this paper is among young women at high risk of HIV acquisition in Tanzania. While previous surveys indicated a consistent decline in HIV prevalence among boys aged 15 - 24 years, the decline is notable among girls aged 15 - 19 but not among women aged 20 - 24 years [19]. Among other factors, difference in HIV prevalence in this subgroup of the population could be attributed by early age at sexual debut and early marriages among young women compared to young men. Early age at sexual debut was also noted to be associated with increased risk of HIV infection among young women in Kenya [23]. It is particularly critical for young women at the debut of their sexual and reproductive lives to have access to information about their HIV status through routine HIV testing.
The Tanzanian Government in collaboration with international donors have significantly expanded and decentralized centers for HIV testing care and treatment. Since 2004 to 2007 Tanzania made changes in national HIV/AIDS policy to increase availability and access to care and treatment services, meanwhile building capacity of health care workers [17]. In 2004, the government started to provide care and treatment services such as free anti-retroviral drugs (ARVs). In 2007, the government rolled out the care and treatment services closer to the community (health centres and dispensaries). During the same year, a new approach Provider Initiated Testing and Counseling (PITC) was adopted to complement with voluntary counseling and testing approach to allow more people who come into contact with health care providers to be offered HIV testing to determine their HIV sero-status. In addition, the national HIV counseling and testing campaign was launched in 2007 by the president of Tanzania as an effort to mobilize more people to undergo HIV testing to determine their HIV sero-status and to establish linkages between prevention, care, treatment, social support. Furthermore, in 2008 Tanzania established a law against stigma and discrimination for people living with HIV/AIDS (PLWHA) to intensify community actions [17].
Despite all these extensive efforts, HIV testing uptake in young women is relatively low. Understanding factors associated with HIV testing uptake in this population is critical. Realizing potential benefits of HIV testing, first, we explored trend in HIV testing uptake among young women (15-24) years between 2003-04 and 2011-12. Secondly, we evaluated individual and contextual factors associated with the changes in HIV testing uptake using 2003-04 THIS, 2007-08 and 2011-12 THMIS.
Methods
Study design and population
We used a cross-sectional study design to evaluate trends in HIV testing uptake and factors associated with the changes in HIV testing uptake among young women 15 - 24 years from Tanzanian Mainland using THIS and THMIS data. Secondary data analyses using 2003-04 THIS as well as 2007-08 and 2011-12 THMIS was performed. Tanzania Demographic Health Survey (DHS) collects nationally representative data at five year intervals through cross sectional surveys. Three such surveys including HIV testing have been conducted: 2003-04, 2007-08 and 2011-12.
Selection of the study participants and data sources
The study population was restricted to young women (15 - 24) years as this group is considered as one of the potentially high risk for HIV infection. After exclusion of those ineligibles, the final sample size was 9,252 subjects from three successive surveys (Figure 1).
Data collection
During the original surveys, after obtaining informed consent, standardized questionnaires designed based on AIDS and Malaria indicator surveys were administered to participating individuals. The questionnaires were developed in English and translated into Kiswahili. Among other things, questionnaires captured information on socio-demographic characteristics (age, gender, marital status, education, residence, religion, employment, asset ownership); biological (ever had STI in the last 12 months, received HIV test results) and antenatal care for recent births.
Variables and definitions
The outcome variable is the proportion of young women who report that they were tested for HIV and received test results within two years preceding the surveys. The independent variables explored in this study are summarized in table 1. These include the following:
![]()
Table 1: Percentage distribution of socio-demographic characteristics of the respondent for Tanzania HIV/AIDS and Malaria Indicator Survey (2003, 2007 and 2011)
View Table 1
Socio-demographic variables: Participants' age (15 - 19, 20 - 24), place of residence (rural, urban), administrative zones (Central, Lake, Northern, Eastern, Western, South West Highlands Southern Highlands, and Southern), and employment status (employed, not employed), number of sexual life partners (0, 1, 2 and >2). Those with missing value on number of sexual life partners were assumed >2).
Zones were used rather than administrative regions in order to have consistency across the surveys. Between 2003 and 2012, some of the regions were split to form new districts and regions thus the 2011-12 survey has more administrative regions than the 2003-04 survey. All the regions however (new and old) belong to the same zones and the geographical coverage of the zones has remained consistent throughout the surveys. Composition of the administrative regions in their respective zones is follows; Eastern (Morogoro, Dar essalaam), Northern (Kilimanjaro, Tanga, Arusha), Lake (Mwanza, Geita, Mara, Simiyu, Shinyanga), Central (Dodoma, ManyaraSingida), Western (Kigoma, Tabora), South-west highlands (Katavi, Rukwa, Mbeya), Southern highland (Iringa, Njombe, Ruvuma) and Southern (Lindi, Mtwara).
Biological variables: reported having had an STI in the last 12 months or not. The three consecutive surveys asked respondents who had ever had sex whether they had had a disease that they got through sexual contact in the past 12 months preceding the surveys. They were also asked whether, in the past 12 months, they had had any genital discharge and whether they had experienced a genital sore or ulcer. For this paper we chose to report whether participant ever had STI or not.
Birth and Antenatal clinic visit in the past two years preceding the surveys. Women who had a birth in the two years prior to the survey were asked whether they received any antenatal care (any number of visits) from any provider for their most recent birth. Respondents were grouped accordingly; those who did not give birth in the past two years, those who gave birth and received any ANC, those who gave birth but did not attend any ANC.
HIV testing
Three dry blood spot (DBS) specimen were collected for each participant and sent to Muhimbili University of Health and Allied Sciences (MUHAS) laboratory for testing. Standard HIV testing algorithm was used across the surveys. The algorithm used two HIV enzyme-linked immunosorbent assays (ELISA) based on different antigens. Discordant samples from the two ELISA tests were retested using the same ELISA tests. All discordant samples from the second round of HIV testing were retested using western blot confirmatory test, the result of which was considered final. Internal and external quality assurance and quality control (QA & QC) were done with external assurance using external reference laboratory.
Statistical analysis
Statistical analyses were conducted using STATA version 12. To evaluate trend in HIV testing uptake across three consecutive surveys, descriptive analyses of HIV testing stratified by selected variables was performed. Analyses were done separately for the periods between 2003-2007, 2007-2011 and 2003-2011. Pooled logistic regression models were performed to determine factors associated with HIV testing uptake between 2003-04 vs. 2007-08 and 2007-8 vs. 2011-12 surveys.
Because each survey sampled a different group of people, change in HIV testing uptake between the three surveys can be attributed to the change in the distribution of selected characteristics (compositional changes or endowments) as well as the change in the effects of the selected characteristics (effects changes or differences in coefficients). Multivariate decomposition models, which are used for portioning changes over time into components attributable to changing effects and changing composition or characteristics, were used to determine factors associated with changes in HIV testing uptakes across the survey periods. The difference observed in HIV testing uptake was decomposed into components attributable to differences in characteristics between surveys (i.e., compositional differences or endowment) and group differences in effects of characteristics (i.e., differences in coefficients or behavioral responses). For example, change in HIV testing can be due to differences in distribution of employment status as well as due to the effects of employment between surveys. All analyses performed in this paper were weighted for probability sampling and non-response using factor as is standard in all surveys that are part of the DHS Program. Because we restricted our outcome to respondents who had HIV serostatus results, we used HIV weight. All associations were deemed statistically significant at cut off p-value of 0.05. Complex sampling (multi-stage sampling and stratification) and 95% confidence intervals were considered and SVY- STATA command was used to control for complex sampling.
Ethical consideration
THIS and THMIS received approval by the Tanzania National Institute of Medical Research (NIMR), the Institutional Review Board (IRB) of ICF International, and the Center for Disease Control (CDC). All adult respondents gave informed consent. As part of DHS fellowship, authors submitted a proposal to DHS Program/ICF International and permission was granted to download and use the data for this study. The DHS Program authorized data access; and the data was used solely for the purpose of the current study.
Results
Trends in HIV testing uptake
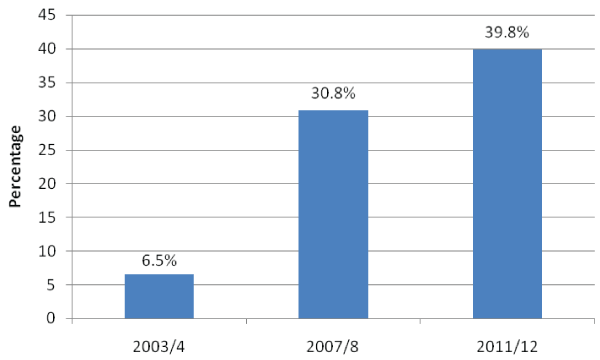
Figure 2 depicts trends in the uptake for HIV testing and receiving results in 2 years preceding the survey for three consecutive surveys among the study population. HIV testing uptake increased remarkably from 6.6% to 30.8% and on to 39.8% for 2003-4, 2007-8 and 2011-12 surveys respectively.
.
Figure 2: Percentage of women who tested for HIV and received results over the 3 successive surveys
View Figure 2
Characteristics of the study participants
The sociodemographic characteristics of the study participants have been shown in table 1. In all the three surveys, participants aged 15-19 years out numbered participants aged 20-24 years, and over 65% were living in rural areas. The majority of the participants had primary education (71.3% in 2003-04, 70.4% in 2007-08 and 59.5% in 2011-12 surveys). Across the three surveys, most of the women had not had birth in the past two years, 66.4%, 68.2% and 68.1% for 2003-04, 2007-08 and 2011-12 surveys respectively. The proportion of women reporting having had 0, 1, or 2 sexual partners in their lifetime was fairly consistent with approximately 31% reporting no sexual partners, 34% reporting 1 lifetime sexual partner, and around 19% reporting 2 lifetime sexual partners. The 2003-04 survey seemed to have a higher proportion reporting more the 2 lifetime sexual partners (18.1%) compared to the 2007-08 and 2011-12 surveys both had approximately 14% of respondents in this category. The majority were employed (63.0% in 2003-04, 59.7% in 2007-08 and 63.8% in 2011-12). The percent who were HIV positive declined from 4% in 2003-4 to 2.8% in 2011-12. About 31% of women reported to have birth and attended ANC within two years preceding the surveys and this proportion remained fairly consistent across the surveys.
Changes in HIV testing in relation to participants characteristics
Change in HIV testing uptake in relation to participant's characteristics is summarized in table 2. In order to assess change in HIV testing uptake, analysis of HIV testing was divided into two phases: Phase 1, between 2003-04 survey to 2007-08 survey, and phase 2, between the2007-08 survey and the 2011-12 survey. Overall, change in HIV testing uptake was 24.2 percentage points between the 2003-04 survey and the 2007-08 survey and 9 percentage points between the 2007-08 survey and the 2011-12 survey, reflecting a higher change in the former phase than in the latter. HIV testing uptake increased for both women aged 15 - 19 and 20 - 24; however, a greater change was notable among those aged 20 - 24 years. Among women residing in urban areas, the change in HIV testing uptake increased by 26.9 percentage points in 2003 - 2007, nearly six times the change seen in 2007 - 2011, 4.7 percentage points. Within the surveys, the change in HIV testing uptake was higher among those who were married compared to those who were not married and it was also higher among those who were HIV positive compared to those who were HIV negative. Compared to women who had no birth within two years preceding the surveys, the change in HIV testing was higher among those who had birth and attended ANC visit (45.8 percentage points vs. 14.3 percentage points) in phase 1 and (20.4 percentage points vs. 3.9 percentage points) in phase 2. The change in HIV testing uptake varies from 5.1 percentage points in phase 1 among women with no sexual partners to 37.5 percentage points among women with two or more lifetime sexual partners.
![]()
Table 2: Trend in HIV testing among women who tested and receive results by socio-graphic characteristics for TMHIS 2003, 2007 and 2011
View Table 2
Factors associated with HIV testing uptake across the surveys
Table 3 shows the results from the pooled logistic regression models for the factors associated with HIV testing uptake across the two survey phases (Phase 1 and Phase 2). Of the factors examined, factors that were found to be associated with women's likelihood to test for HIV and receive results included having an education (primary or secondary), ever being married, having had one or more life sexual partners, attendance to antenatal care within the 2 years preceding the survey. Having had an STI was also associated with HIV testing uptake, but the association was not statistically significant.
![]()
Table 3: Pooled Multivariate logistic regression for factors associated with HIV testing uptake among women aged 15-24 years across 2 surveys
View Table 3
The results from multivariate decomposition regression models are shown in table 4a & 4b. According to the model, in 2003-04 vs 2007-08 surveys, changes in population characteristics (endowments) would have resulted in a decline in overall HIV testing (-5.26%) in the absence of any changes of the effects of these characteristics on the likelihood of being tested. Changes in composition factors such as increased proportion of women residing in rural areas and decreased proportion of women with primary education would have contributed to decreased odds in HIV testing uptake among women in the absence of the effects of these characteristics. In addition, some compositional factors such as, increased in proportion of those ever married, having one or more lifetime sexual and attendance to antenatal care within 2 years preceding the survey, were significantly associated with changes in HIV testing uptake (Table 4a). Our findings also revealed that 105.26% of the changes in HIV testing uptake in 2003-04 vs 2007-08 surveys was due to differences in the effects of compositional factors (coefficients).
![]()
Table 4A: Decomposition changes in HIV testing among women of reproductive (15-24 years) in TMHIS 2003 to 2007
View Table 4A
![]()
Table 4B: Decomposition changes in HIV testing among women of reproductive (19-49 years) in TMHIS 2007 to 2011
View Table 4B
In the 2007-08 vs. 2011-12 surveys, the changes in endowments contributed to 22.1% of the changes in HIV testing uptake, where as 77.9% of the changes in HIV testing uptake was attributed to differences in the effects of characteristics (coefficients). Both endowments and coefficients were statistically significant in both multivariate decomposition models. Increased education level of women (having any level of education vs. having none) made it much more likely for them to test. The increase in women with primary education should have made it more likely for women to be tested regardless of any changes in effects.
In terms of coefficients, ANC attendance (43.5%) and age group 20 - 24 years (35.3%) appear to have statistically significant contribution to the uptake of HIV testing. Despite having large contributions to the uptake of HIV testing based on coefficient, both rural residence (with a coefficient of 36.38%) and having primary education (with a coefficient of 13.6%), do not appear to have a statistically significant contribution toward the uptake of HIV testing.
Discussion
Trends in HIV testing uptake
The present study demonstrated a rapid increase in HIV testing uptake over the past eight years between the surveys. Nearly 40 percent of the included women in the 2011-12 survey had been tested for HIV and received test results, a proportion that is 7.5 times that seen in the 2003-04 survey. Greater increase in HIV testing uptake is noted between 2003-04 and 2007-08 than that seen between 2007-08 and 2011-12, however, the proportion of HIV testing is similar to that seen in general population of women aged 15-49 [17].
The increase in HIV testing uptake could be attributable to the wider availability of rapid HIV testing kits (lowering cost of testing), the rolling out of free antiretroviral therapy which started in December 2004, as well as national campaigns to promote testing [17,24]. The increase in HIV testing uptake may as well be due to the presidential mass campaign for HIV testing 2007 as well as enactment of the law for anti-discrimination for people living with HIV (PLWH) in 2008. Increased testing translates to increased proportion of those aware of their status and possibly behavior modification towards HIV preventive efforts.
Determinants of HIV testing uptake
Numerous factors were associated with HIV testing uptake. The odds of HIV testing uptake was higher among women with primary and secondary education or higher as compared to those without formal education. This finding is in agreement with a previous study conducted among Ghanaian women which showed that higher education was strongly correlated with HIV testing uptake [25]. The possible explanation for this could be that higher education attainment provides opportunities to clearly understand HIV infection.
Moreover, those with higher education are more likely to be employed and therefore have better access to VCT services than those without formal education as most VCT centers would charge clients up to around the year 2004.
Marital status also showed to be related to HIV testing uptake with women who were married being more likely to undergo HIV testing than those who were not married. Similar findings were documented by others where women who were not married were less likely to be tested for HIV [25,26]. Higher odds of HIV testing uptake among married women in our study could be due to advocacy of faith based institutions on the importance of having HIV testing prior to marriage in Tanzania.
Compared to women without sexual partners, the odds of HIV testing uptake were higher in those who had one or more life time sexual partners which is consistent with the previous findings from Tanzania [27]. Higher odds of HIV testing uptake among those who engaged in sexual practices may be due to the fear of being infected or infecting others as HIV infection in this region is predominantly transmitted sexually.
Attending ANC was also an important determinant for HIV testing in the current study. Women who had birth within two years preceding the surveys and attended ANC had increased odds of HIV testing as compared to those who did not have birth. No association of HIV testing uptake was noted among women who had birth and did not attend ANC. Increased uptake of HIV testing has been previously reported among Vietnamese women attending ANC [28]. As part of prevention of mother to child transmission of HIV, women are required to test in order to receive ART for prevention and also make decision on breast feeding for newborn and family planning practices. This could explain the higher HIV testing uptake amongst women who attended ANC. Analysis showed a significant difference in HIV testing uptake in relation to participant STI status. Having an STI or symptoms of an STI was associated with increased odds of HIV testing compared to those who did not have. Association between STI and HIV testing uptake has also been reported previously [29]. STIs are one of the risk factors for HIV infection acquisition and are often transmitted along with HIV. Individuals attending STI clinics are thus more likely to be counselled and eventually tested for HIV, which could explain higher odds of HIV testing uptake among this group.
This study also revealed that HIV testing uptake changes with age. Women aged 20 - 24 years had increased odds of HIV testing uptake compared to those who were 15 - 19 years. Older age has been reported to be associated with an increased likelihood of being tested for HIV [30]. This could be due to the fact that older women are more likely to be sexually active, more likely to be married and economically empowered than younger ones.
In addition, women who lived in urban areas were more likely to test for HIV than those who lived in rural areas. Those who live in urban areas have greater access to VCT services than those who live in rural areas and this may explain higher odds of HIV testing uptake among those in urban areas. We also found zonal variations in HIV testing uptake across the surveys. This could be explained by the regional variation in HIV testing across the countries due to differences in availability of VCT services between zones.
Decomposition of the changes of HIV testing uptake
Decomposition analyses discerned the sources in the changes of HIV testing uptake. Changes in the composition of the population with different levels of education, attending ANC visits and place of residence contributed to observable changes in HIV testing uptake. For example during the first phase a decrease in the proportion of women with primary education or an increase in the proportion of women residing in rural areas would have resulted in a decrease in HIV testing uptake in the absence of the effects of these compositional characteristics. Although changes in the population composition contributed to the change in the increase in HIV testing uptake, most of the HIV testing uptake was due to the changes in the effects of the population characteristics. For example, attending ANC visit significantly contributed to the changes in HIV testing uptake in both first and second phases.
Strengths and limitations of the study
Unlike the standard logistic regression-based approaches that rely on individual level observational data, multivariate regression decomposition in HIV testing provides opportunity for detailed explanations for the differences in the changes in HIV testing across the surveys. We were also not able to assess the true effect of HIV interventions performed across the survey periods which also might have influenced the observed changes in HIV testing.
Conclusions
The uptake of HIV testing has remarkably increased over the three surveys. The differences in HIV testing uptake across surveys is to a large extent explained by the differences in coefficients with attending ANC visit, place of residence and having primary education or higher playing major role. Knowing one's HIV status is the gateway to HIV treatment and prevention however the expansion in HIV testing has been greater among women with high risk characteristics, and thus has become more targeted. Until testing is universal, an effective expansion strategy would be to prioritize those most likely to be infected.
Acknowledgments
We are grateful to the USAID for funding the research project through the program implemented by ICF International. Our gratitude appreciations extend to all reviewers for their constructive comments to help improving our manuscript. We thank Sarah, Wenjuan and other DHS facilitators for their endless support throughout the DHS training period.
References
-
(2013) Global report: UNAIDS report on the global AIDS epidemic 2013. UNAIDS: 198.
-
Ivers LC, Kendrick D, Doucette K (2005) Efficacy of antiretroviral therapy programs in resource-poor settings: a meta-analysis of the published literature. Clin Infect Dis 41: 217-224.
-
Ferradini L, Jeannin A, Pinoges L, Izopet J, Odhiambo D, et al. (2006) Scaling up of highly active antiretroviral therapy in a rural district of Malawi: an effectiveness assessment. Lancet 367: 1335-1342.
-
Barth RE, Van Der Meer JTM, Hoepelman a. IM, Schrooders P a., Van De Vijver D a., et al. (2008) Effectiveness of highly active antiretroviral therapy administered by general practitioners in rural South Africa. Eur J Clin Microbiol Infect Dis 27: 977-984.
-
Beyrer C, Abdool Karim Q (2013) The changing epidemiology of HIV in 2013. Curr Opin HIV/AIDS 8: 306-310.
-
(2013) Demographic and Health Survey. Demographic Patterns of HIV Testing Uptake in Sub-Saharan Africa. DHS Comoparative Reports 30: 1-95.
-
Gianella S, Von Wyl V, Fischer M, Niederoest B, Battegay M, et al. (2011) Effect of early antiretroviral therapy during primary HIV-1 infection on cell-associated HIV-1 DNA and plasma HIV-1 RNA. Antivir Ther 16: 535-545.
-
Hall HI, Holtgrave DR, Maulsby C (2012) HIV transmission rates from persons living with HIV who are aware and unaware of their infection. AIDS 26: 893-896.
-
Siegfried N, Uthman OA, Rutherford GW (2010) Optimal time for initiation of antiretroviral therapy in asymptomatic, HIV-infected, treatment-naive adults. Cochrane Database Syst Rev 3: CD008272.
-
Miro JM, Manzardo C, Mussini C, Johnson M, d'Arminio Monforte A, et al. (2011) Survival outcomes and effect of early vs. deferred cART among HIV-infected patients diagnosed at the time of an AIDS-defining event: A cohort analysis. PLoS One 6: 4-11.
-
(2005) Scaling-up HIV Testing and Counselling services. WHO
-
Cock KM De, Marum E, Mbori-ngacha D (2003) Viewpoint A serostatus-based approach to HIV / AIDS prevention and care in Africa. Lancet 362: 1847-1849.
-
Mabuto T, Latka MH, Kuwane B, Churchyard GJ, Charalambous S, et al. (2014) Four models of hiv counseling and testing: Utilization and test results in South Africa. PLoS One 9: e102267.
-
Ng'ang'a A, Waruiru W, Ngare C, Ssempijja V, Gachuki T, et al. (2014) The status of HIV testing and counseling in Kenya: results from a nationally representative population-based survey. J Acquir Immune Defic Syndr 1: S27-S36.
-
Cohen MS, Chen YQ, McCauley M, Gamble T, Hosseinipour MC (2011) Prevention of HIV-1 Infection with Early Antriretroviral Therapy. N Engl J Med 365: 493-505.
-
Das M, Chu PL, Santos GM, Scheer S, Vittinghoff E, et al. (2010) Decreases in community viral load are accompanied by reductions in new HIV infections in San Francisco. PLoS One 5: e11068.
-
(2008) HIV/AIDS and Malaria Indicator Survey 2007-08. TACAIDS.
-
(2013) HIV/AIDS and Malaria Indicator Survey 2011-12. TACAIDS.
-
(2001) The United republic of Tanzania prime minister's office national policy on HIV / AIDS. Dar es Salaam. TACAIDS.
-
Granich RM, Gilks CF, Dye C, De Cock KM, Williams BG (2009) Universal voluntary HIV testing with immediate antiretroviral therapy as a strategy for elimination of HIV transmission: a mathematical model. Lancet 373: 48-57.
-
Dodd PJ, Garnett GP, Hallett TB (2010) Examining the promise of HIV elimination by "test and treat" in hyperendemic settings. AIDS 24: 729-735.
-
Alsallaq RA, Baeten JM, Celum CL, Hughes JP, Abu-Raddad LJ, et al. (2013) Understanding the Potential Impact of a Combination HIV Prevention Intervention in a Hyper-Endemic Community. PLoS One 8: 1-13.
-
Gitonga M, Sinyard M, Gachuiri G (2012) Alcohol and substance use vis a vis HIV sexual risk behaviours among freshman students at a Kenyan University College; focus for interventions. J Biol Agric Healthc 2: 8-12.
-
Isingo R, Wringe A, Todd J, Urassa M, Mbata D, et al. (2012) Trends in the uptake of voluntary counselling and testing for HIV in rural Tanzania in the context of the scale up of antiretroviral therapy. Trop Med Int Heal 17: 15-25.
-
Tenkorang EY, Owusu GA (2010) AIDS Care?: Psychological and Socio-medical Aspects of AIDS / HIV Correlates of HIV testing among women in Ghana?: some evidence from the Demographic and Health Surveys. AIDS Care 22: 296-307.
-
Ziraba AK, Madise NJ, Kimani JK, Oti S, Mgomella G, et al. (2011) Determinants for HIV testing and counselling in Nairobi urban informal settlements. BMC Public Health 11: 663.
-
Charles MP, Kweka EJ, Mahande AM, Barongo LR, Shekalaghe S, et al. (2009) Evaluation of uptake and attitude to voluntary counseling and testing among health care professional students in Kilimanjaro. BMC Public Health 9: 1-9.
-
Hanh NT, Gammeltoft TM, Rasch V (2011) Number and timing of antenatal HIV testing?: Evidence from a community-based study in. BMC Public Health 11: 8-10.
-
Swenson RR, Rizzo CJ, Brown LK, Payne N, DiClemente RJ, et al. (2009) Prevalance and Correlates of HIV Testing among Sexualy Active African American Adolescents in Four U.S. Cities. Sex Transm Dis 36: 584-591.
-
Peltzer K, Matseke G, Peltzer K (2013) Determinants of HIV testing among young people aged 18 - 24 years in South Africa. Afr Health Sci 13: 1012-1020.






