Journal of Hypertension and Management
Noninvasive Tools Used Nowadays in both, Clinical Practice and Trials in Order to Assess Blood Pressure
Martyna Zaleska1, Olga Mozenska1, Katarzyna Nikelewska1, Magdalena Chrabaszcz1, Weronika Rygier1, Jan Gieraltowski2, Monika Petelczyc2 and Dariusz A Kosior1,3*
1Department of Cardiology and Hypertension, Central Research Hospital, the Ministry of the Interior, Poland
2Warsaw University of Technology, Faculty of Physics, Poland
3Department of Applied Physiology, Mossakowski Medical Research Centre, Poland
*Corresponding author:
Dariusz A Kosior, MD, PhD, FACC, FESC, Head of Department of Cardiology and Hypertension, Wołoska 137, 02-507 Warsaw, Poland, Tel: 48-22-508-16-70, Fax: +48-22-508-16-80, E-mail: s.iadariusz@upcpoczta.pl
J Hypertens Manag, JHM-2-009, (Volume 2, Issue 1), Short Review; ISSN: 2474-3690
Received: March 05, 2016 | Accepted: March 31, 2016 | Published: April 02, 2016
Citation: Zaleska M, Mozenska O, Nikelewska K, Chrabaszcz M, Rygier W, et al. (2016) Noninvasive Tools Used Nowadays in both, Clinical Practice and Trials in Order to Assess Blood Pressure. J Hypertens Manag 2:009. 10.23937/2474-3690/1510009
Copyright: © 2016 Zaleska M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Hypertension affects currently around 1 billion people worldwide and cardiovascular disease remains the most frequent cause of mortality worldwide. Hypertension societies publish cyclically recommendations how to diagnose and manage this illness. Some of them describes tools used to diagnose this disease, others do not. However nowadays many new methods are introduced to assess blood pressure (BP) values. Some of them allow only to obtain central or systolic BP, others are used currently only in animal studies. Some studies proved that they may be a useful tool to assess BP values noninvasive in the future. Here we present a short review regarding methods described in literature to assess BP.
Keywords
Hypertension, Noninvasive assessment, Blood pressure, Clinical research, Animal studies
Abbreviations
ABPM: Ambulatory blood pressure monitoring; ACC: American college of cardiology; AHA: American heart association; AP: Arterial pressure; BP: Blood pressure; CVD: Cardiovascular disease; DBP: Diastolic blood pressure; ESC: European society of cardiology; HBPM: Home blood pressure monitoring; JNC 8: Eight joint national committee; PPG: Photoplethysmography; PTNT: Polish society of hypertension; PTT: Pulse transit time; PWV: Pulse wave velocity; SBP: Systolic blood pressure
Introduction
Cardiovascular diseases (CVD) remain the most frequent cause of mortality worldwide. One of the key risk factors for CVD is hypertension [1]. Although good blood pressure (BP) control may decrease incidence of related deaths and effective treatment is available, first correct hypertension diagnosis has to be made as well as assessment of treatment effectiveness is needed [2]. Both of the above-mentioned goals may be achieved with the aid of different non-invasive tools to assess BP.
Devices Used for Everyday Blood Pressure Measurement
Nowadays the most frequently used method to assess BP is office BP measurement with auscultatory or oscillometric semiautomatic sphygmomanometers [3]. Due to ban on mercury now sphygmomanometers base on aneroid devices, which proved to be accurate [4]. Although this method has certain limitations, i.e. white coat hypertension, auscultatory gap and influence of cuff inflation and deflation time on BP values [5].
For home use oscillometric devices are recommended, due to its ease to use and satisfactory accuracy [6]. Though, patients should be advised to use devices validated according to standard international protocols [5]. Wrist devices may be very useful in severely obese patients, but their measurements are influenced by wrist position [7].
Ambulatory BP monitoring (ABPM) is obtained with the use of portable BP measuring devices on non-dominant arm for the period of 24 hours. The patient wears a standard cuff and a computer, which weights around 500 g and is worn on a belt or over the shoulder, during the whole time of the study. It provides BP values during patients' normal, daily activity and reduces risk of white coat hypertension [8]. Although, in ABPM measurements arm position may influence obtained BP values [9].
Everyday BP Measurement and Hypertension Definition according to International Guidelines
American College of Cardiology (ACC)/American Heart Association (AHA) and Eight Joint National Committee (JNC 8) guidelines do not discuss methods of BP assessment [10,11]. European Society of Cardiology (ESC), Polish Society of Hypertension (PTNT) as well as ACC/AHA and JNC 8 guidelines define hypertension as BP values above 140 or 90 mmHg for systolic (SBP) and diastolic (DBP), respectively, if office BP measurements are used [3,10,11]. Some conditions must be fulfilled in order to make proper BP measurement, for example patient must be seated, at least 2 measurements must be taken, cuff and bladder dimensions must be adapted to the arm circumference. Additionally during the first visit BP should be measured on both arms [3]. Those conditions are given in both, ESC and PTNT guidelines [3,12].
Lower BP values are defined as hypertension when ABPM or home BP monitoring (HBPM) are used. They provide numerous BP measurements taken outside of the clinical environment, which are expected to be more reliable than office BP values [3,10-12]. American guidelines do not relate to ABPM value in hypertension diagnosis [10]. Regarding ESC guidelines patient should be instructed to stop talking or moving during cuff infiltration and to remain engaged in normal daily activities, though he should provide dairy with symptoms or actions which may potentially influence BP values. Normal BP values are defined as: SBP under 135 mmHg and DBP under 85 mmHg during awake hours, SBP under 120 mmHg and DBP under 70 mmHg during nighttime. Mean BP values calculated from all available values assessed during measurement should be under 130 and 80 mmHg for SBP and DBP respectively [3]. In PTNT guidelines there are no instructions for patients, but other data are in agreement with ESC guidelines [12]. This method provides additionally data such as circadian blood pressure profile, BP load or morning surge. Though, those additional data is still considered as experimental, since their predictive value has not been fully cleared yet [3]. Although, studies proved that ABPM outcomes are more sensitive as clinical risk predictor for cardiovascular outcomes, morbidity and mortality [3,13,14].
Table 1 summarizes indications, advantages, limitations and instructions for correct use of ABPM.
![]()
Table 1: Indications, advantages, limitations and instructions for correct use of ambulatory blood pressure monitoring.
View Table 1
Home BP monitoring involves patients' self-measurement of BP, sometimes with support of family member or trained health provider. Again JNC 8 guidelines do not state conditions to diagnose hypertension with HBPM [10]. Regarding ESC guidelines measurement should be obtained for 7 days, at least 3 to 4 days, both in the mornings and in the evenings. We should bear in mind that special conditions should be kept, such as 5 minutes rest before measurement and 2 measurements taken each time. Some authors reported that HBPM outcomes have better predictive value of cardiovascular morbidity and mortality than office measurements [3,14]. Polish Hypertension Society gives the same conditions to obtain proper home BP value [12]. Table 2 summarizes advantages, limitations and indications for correct use of HBPM.
![]()
Table 2: Limitations, advantages and instructions for correct use of home blood pressure monitoring.
View Table 2
Devices for BP Measurement Used in Clinical Trials and Studies Conducted on Animals
Central SBP measurement
One of the non-invasive methods to assess central BP is carotid artery pressure measurement. Due to proximity of carotid artery we assume that the pressure values measured on the carotid artery can surrogate values in the aorta. To obtain carotid pressure values we use applanation tonometry and then analysis of the carotid waveforms. We scale them to DBP and mean BP values measured on brachial artery, since they do not vary markedly in the arterial tree [15]. However, this method is highly observer-dependent and is not often used in routine clinical practice [16]. We could also register brachial waveforms, what may be easier and less operator-dependent, but then we need generalized transfer function, identification of the late systolic shoulder of the peripheral pressure waveform, or a proprietary algorithm to obtain central BP due to factors moulding pulse wave shape remote to aorta [16]. It may be easier to obtain radial waveform, but due to brachial-to-radial amplification it should not be calibrated to the brachial mean and diastolic BP [16,17].
It is worth mentioning that central SBP is usually measured on carotid site and should not be confused with peripheral SBP, measured on brachial artery, since it may be overestimated in young subjects. It may be due to higher peripheral artery stiffness, which increase with age and other conditions diagnosis, such as hypercholesterolemia or hypertension [18]. Central BP values are becoming more interesting for physicians firstly due to their higher than brachial BP values' predictive value for cardiovascular events [19-22]. Secondly, in latest research differential effects of antihypertensive drugs on central BP are starting to be described [23,24].
Photoplethysmography
The photoplethysmogram, which allows to estimate skin blood flow, and measures not only BP, but also cardiac output and oxygen saturation, consists of light source and sensor system (Figure 1) [25]. This method includes waveform measurement and from those parameters we can obtain blood volume pulse and then BP. Photoplethysmography (PPG) allows to measure BP on such issues as finger, toe or even ear lope [26]. However, those outcomes may be influenced by temperature and sympathetic activity [27,28]. On the other hand, it is worth emphasizing that this method is inexpensive and convenient, even if imprecise in some cases [29].
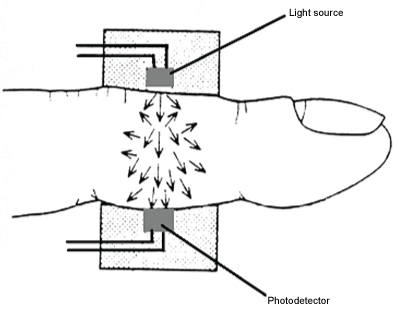
.
Figure 1: Photoplethysmography.
(Source: http://sashpsg.blogspot.com/2015/02/photoplethysmography.html)
View Figure 1
Volume clamping
Above-mentioned limitations of PPG may be omitted since in 1973 Penaz introduced his novel method to assess BP [30]. It includes additionally to PPG fingertip cuff occlusion (Figure 2). In this method the blood flow oscillations are detected and the finger cuff keeps the volume in the finger arteries constant. From the values of pressure needed to keep the volume in the finger arteries constant obtained by cuff arterial pressure can be calculated indirectly [31,32]. In 1998, after reviewing 43 papers regarding this method's accuracy Imholz et al. stated, that this method is an accurate tool to assess mean and diastolic BP, and despite the fact that differences in SBP reached statistical significance, they remained clinically irrelevant [33]. Recently Wagner et al. proved those outcomes in their study [32]. Additionally beat-to-beat BP changes and BP variability measured with volume clamping method proved to be accurate and reliable comparing to invasive methods [33]. It is worth mentioning that this method has no risk of infection or bleeding in contrast to invasive tools [32].
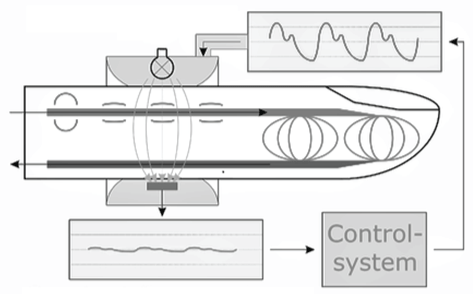
.
Figure 2: Volume clamping.
(Source:https://en.wikipedia.org/wiki/Continuous_noninvasive_arterial_pressure)
View Figure 2
Pulse transit time
Another method now being considered for use in “real-life” is pulse transit time (PTT). It is defined as time between R-wave on the electrocardiogram and peripheral pulse-wave (obtained mainly with the use of PPG). Further from the PTT we calculate pulse wave velocity (PWV) and after that on the base of PWV and BP relation software can calculate BP [34]. Authors also reported that PTT may be used in order to obtain absolute SBP, when an ndividual correction for the offset of the relation between PWV and BP is performed [35].
Doppler assessment of BP
Using Doppler machine we as well may obtain BP values, though due to sensitivity of the method it is more likely used in case of low pressures' measurement (Figure 3) [36]. After inflating the cuff to values above SBP we begin to deflate it. The first sound heard by the Doppler machine over the brachial artery is considered SBP [37]. Some authors reported that SBP measured by the Doppler technique agree more closely with directly obtained BP than values assessed by other techniques, such as palpation and auscultation [37]. Some newer devices may measure also DBP, though those measurements correlated less satisfactory with direct measurements than SBP, authors described, that they correlated well [38].
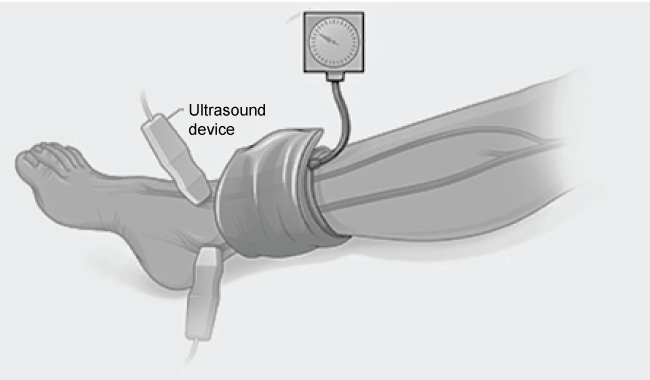
.
Figure 3: Doppler assessment of blood pressure. (Source: https://www.gbhealthwatch.com/pericardialdisorders-details.php)
View Figure 3
A modification of Doppler method is laser Doppler assessment of BP. This method is more accurate than PPG in case of low BP values, i.e. in case of critical leg ischemia. In laser Doppler moving blood cells cause changes in frequency shift of the reflected light, what is obtained by this method. In order to assess SBP with this method we have to inflate the cuff and then deflate it slowly. The SBP is defined as the moment when signal reappears or rises from the baseline. Additionally minute microcirculatory blood perfusion in the skin is detectable in laser Doppler [39].
Electrical impedance tomography
This modern technology is a non-invasive tool to analyze bioimpedance signals. It measures intra-thoracic impedance changes in relationship to cardiovascular activity [40]. This method relies on the fact that pulse pressure propagates along arteries, what causes increase of blood volume what is associated with decrease in local impedance. Based on mathematical models others proved that this method is useful in obtaining arterial pulsatility in descending aorta, what may lead to continuous central BP assessment [41]. To the best of our knowledge, currently it is used in order to assess BP only in clinical trials and animal studies. An MRI-based 3D hemodynamic thorax model was built, on which Braun et al. investigated the possibility to measure mean aortic BP using this method, though studies in humans are needed for detailed evaluation [40].
High definition oscillometry
Conventional oscillometry measures mean arterial pressure (AP) and from this parameter systolic AP and diastolic AP are calculated. In high definition oscillometry pulse amplitudes are based on real-time analysis of artery oscillations. Additionally this method allows to measure AP by heart frequencies up to 500 beats per minute and to maintain linearity during deflation [42]. This method is used mainly in animal studies regarding pharmacology. The newest approach in oscillometry is based not on the mathematical algorithm to calculate systolic and diastolic BP from mean BP. It allows to accomplish direct, both DBP and SBP measurements [43].
Radiofrequency ultrasound wall tracking of the carotid artery
This method measures carotid pressure changes from calibrated distension waveforms [44]. Carotid wall tracking measurements should be calibrated to the mean and diastolic BP (obtained by for example sphygmomanometry on brachial artery). It allows measuring only central SBP. Outcomes of this method proved to be well correlated with directly measured BP [45].
Self BP measurements and telemonitoring system
Currently it is emphasized that despite hypertension diagnosis many patients fail to achieve their treatment goals [46]. Some authors reported that telemonitoring systems of HBPM may be helpful to improve hypertension treatment's management [47,48]. Telemonitoring is a technology used to monitor patients' status from a distance [49]. Notifications are sent to physicians when i.e. BP values are outside of normal range, so they can consult this patient immediately if needed [50]. This can reduce patients' both, travel and off-work time and allow better patients' compliance [50].
Conclusions
Although multiple noninvasive methods to assess BP values are described and proposed in multiple studies, they are nowadays mainly used in research and animal studies. They are not evaluated by international societies and their diagnostic value remains unclear. Multiple new devices to obtain noninvasive continuous BP values are proposed. They may be very useful in case for example of cardiac surgery and postoperative monitoring of BP. They may limit the number of infections associated with invasive BP monitoring. Table 3 gives a brief summarization of novel methods' advantages as well as disadvantages.
![]()
Table 3: Methods used in clinical trials and animal studies.
View Table 3
Additionally the availability of ABPM may become better during next years. Its predictive value is better than predictive value of standard office BP measurements. It also allows to monitor drug effectiveness during the whole day and that may improve timing of drugs' administration.
Home BP monitoring is highly patient dependent. It may be influenced by patients' device and, sometimes, their inability to obtain proper BP values. Although this method in long-term may help to include patient's into the treatment process and may allow better compliance.
Due to limited availability and also lack of data regarding evaluation by international societies authors of this paper consider new methods interesting and perhaps useful in the future. A limitation in their introduction to standard medical use may be high costs and need to invest in new equipment.
References
-
(2013) A global brief on hypertension: silent killer, global public health crisis. World Health day, Organization WHO.
-
He FJ, MacGregor GA (2003) Cost of poor blood pressure control in the UK: 62,000 unnecessary deaths per year. Journal of human hypertension 17: 455-457.
-
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, et al. (2013) ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens: 1281-357.
-
Ma Y,Temprosa M, Fowler S, Prineas RJ, Montez MG, et al. (2009) Evaluating the accuracy of an aneroid sphygmomanometer in a clinical trial setting. American journal of hypertension 22: 263-266.
-
Ogedegbe G, Pickering (2010) T. Principles and techniques of blood pressure measurement. Cardiologyclinics 28: 571-586.
-
O'Brien E, Waeber B, Parati G, Staessen J (2001) Blood pressure measuring devices: recommendations of the European Society of Hypertension. British Medical Journal 322: 531-536.
-
Mitchell PL, Parlin RW, Blackburn H (1964) Effect of vertical displacement of the arm on indirect blood-pressure measurement. New England Journal of Medicine 271: 72-74.
-
Health Quality Ontario (2012) Twenty-Four-Hour Ambulatory Blood Pressure Monitoring in Hypertension: An Evidence-Based Analysis. Ont Health Technol Assess Ser 12: 1-65.
-
Netea R, Lenders J, Smit P, Thien T (2003) Both body and arm position significantly influence blood pressure measurement. Journal of human hypertension 17: 459- 462.
-
James PA, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb, et al. (2014) evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). Jama 311: 507-520.
-
Go AS, Bauman MA, King SMC, Fonarow GC, Lawrence W, et al. (2014) An effective approach to high blood pressure control: a science advisory from the American Heart Association, the American College of Cardiology, and the Centers for Disease Control and Prevention. Journal of the American College of Cardiology 163: 1230-1238.
-
Tykarski A, Narkiewicz K, Gaciong Z, Januszewicz A, Litwin M, et al. (2015) Zasady postępowania w nadciśnieniu tętniczym-2015 rok. Nadciśnienie Tętnicze w Praktyce 1: 1-70.
-
Staessen JA, Thijs L, Fagard R, O'Brien ET, Clement D, et al. (1999) Predicting cardiovascular risk using conventional vs ambulatory blood pressure in older patients with systolic hypertension. Jama 282: 539-546.
-
Sega R, Facchetti R, Bombelli M, Cesana G, Corrao G, et al. (2005) Prognostic value of ambulatory and home blood pressures compared with office blood pressure in the general population follow-up results from the Pressioni Arteriose Monitorate e Loro Associazioni (PAMELA) Study. Circulation 111: 1777-17783.
-
Kroeker EJ, Wood EH (1955) Comparison of simultaneously recorded central and peripheral arterial pressure pulses during rest, exercise and tilted position in man. Circulation research 3: 623-632.
-
McEniery CM, Cockcroft JR, Roman MJ, Franklin SS,Wilkinson IB (2014) Central blood pressure: current evidence and clinical importance. European heart journal 35: 1719-1725.
-
Verbeke F, Segers P, Heireman S, Vanholder R, Verdonck P, et al. (2005) Noninvasive assessment of local pulse pressure importance of brachial-to-radial pressure amplification. Hypertension 46: 244-248.
-
Wilkinson IB, Franklin SS, Hall IR, Tyrrell S, Cockcroft JR (2001) Pressure amplification explains why pulse pressure is unrelated to risk in young subjects. Hypertension 38: 1461-1466.
-
Roman MJ, Devereux RB, Kizer JR, Lee ET, Galloway JM, et al. (2007) Central pressure more strongly relates to vascular disease and outcome than does brachial pressure the strong heart study. Hypertension 50: 197-203.
-
Safar ME, Blacher J, Pannier B, Guerin AP, Marchais SJ, et al. (2002) Central pulse pressure and mortality in end-stage renal disease. Hypertension 39: 735-738.
-
Pini R, Cavallini MC, Palmieri V, Marchionni N, Di Bari M, et al. (2008) Central but not brachial blood pressure predicts cardiovascular events in an unselected geriatric population: the ICARe Dicomano Study. Journal of the American College of Cardiolog 51: 2432- 2439.
-
Jankowski P, Kawecka-Jaszcz K, Czarnecka D, Brzozowska-Kiszka M, Styczkiewicz K, et al. (2008) Pulsatile but not steady component of blood pressure predicts cardiovascular events in coronary patients. Hypertension 51: 848-855.
-
Williams B, Lacy PS, Thom SM, Cruickshank K, Stanton A, et al. (2006) Differential impact of blood pressure-lowering drugs on central aortic pressure and clinical outcomes principal results of the Conduit Artery Function Evaluation (CAFE) Study. Circulation 113: 1213-1225.
-
Asmar RG, London GM, O'Rourke ME, Safar ME (2001) Coordinators RP, Investigators. Improvement in Blood Pressure, Arterial Stiffness and Wave ReflectionsWith a Very-Low-Dose Perindopril/Indapamide Combination in Hypertensive Patient A ComparisonWith Atenolol. Hypertension 38: 922- 926.
-
Tamura T, Maeda Y, Sekine M, YoshidaM (2014) Wearable photoplethysmographic sensors-past and present. Electronics 3: 282-302.
-
Zneid BA, Al-zidi M, Al-kharazi T (2014) Non-invasive blood pressure remote monitoring instrument based microcontroller. IEEE.
-
Hertz man AB, Roth LW (1942) The vasomotor components in the vascular reactions in the finger to cold. American Journal of Physiology-Legacy Content 136: 669- 679.
-
Heyman F, Ahlberg NE (1968) Effect of rapid distension of large arteries and veins on the vascular tone of the fingers. Acta medica Scandinavica 183: 337-340.
-
Elgendi M (2012) On the analysis of fingertip photoplethysmogram signals. Current cardiology reviews 8: 14.
-
Penaz J (1973) Photoelectric measurement of blood pressure, volume and flow in the finger. Digest of the 10th international conference on medical and biological engineering. International Federation for Medical and Biological Engineering, New York.
-
Fortin J, MarteW, Grüllenberger R, Hacker A, Habenbacher W, et al. (2006) Continuous non-invasive blood pressure monitoring using concentrically interlocking control loops. Computers in biology and medicine 36: 941-957.
-
Wagner JY, Negulescu I, Schöfthaler M, Hapfelmeier A, Meidert AS, et al. (2015) Continuous noninvasive arterial pressure measurement using the volume clamp method: an evaluation of the CNAP device in intensive care unit patients. J Clin Monit Comput 29: 807-813.
-
Imholz BP, Wieling W, van Montfrans GA, Wesseling KH (1998) Fifteen years experience with finger arterial pressure monitoring. Cardiovascular research 38: 605-616.
-
Patzak A, Mendoza Y, Gesche H, Konermann M (2015) Continuous blood pressure measurement using the pulse transit time: Comparison to intra-arterial measurement. Blood Press 24: 217-221.
-
Gesche H, Grosskurth D, Küchler G, Patzak A (2012) Continuous blood pressure measurement by using the pulse transit time: comparison to a cuff-based method. Eur J Appl Physiol 112: 309-315.
-
Ward M, Langton JA (2007) Blood pressure measurement. Continuing Education in Anaesthesia, Critical Care & Pain 7: 122-126.
-
Elseed A, Shinebourne E, Joseph M (1973) Assessment of techniques for measurement of blood pressure in infants and children. Arch Dis Child 48: 932-936.
-
Savage J, Dillon M, Taylor J (1979) Clinical evaluation and comparison of the Infrasonde, Arteriosonde, and mercury sphygmomanometer in measurement of blood pressure in children. Arch Dis Child 54: 184-189.
-
de Graaff JC, Ubbink DT, Legemate DA, de Haan RJ, Jacobs MJ (2000) The usefulness of a laser Doppler in the measurement of toe blood pressures. J Vasc Surg 32: 1172-1179.
-
Braun F, Proença M, Rapin M, Lemay M, Adler A, et al. (2015) Aortic blood pressure measured via EIT: investigation of different measurement settings. Physiol Meas 36: 1147-1159.
-
Solà J, Adler A, Santos A, Tusman G, Sipmann FS, et al. (2011) Non-invasive monitoring of central blood pressure by electrical impedance tomography: first experimental evidence. Med Biol Eng Comput 49: 409-415.
-
Wernick M, Doherr M, Howard J, Francey T (2010) Evaluation of high‐definition and conventional oscillometric blood pressure measurement in anaesthetised dogs using ACVIM guidelines. J Small Anim Pract 51: 318-324.
-
Meyer O, Jenni R, Greiter-Wilke A, Breidenbach A, Holzgrefe HH (2010) Comparison of telemetry and high-definition oscillometry for blood pressure measurements in conscious dogs: effects of torcetrapib. J Am Assoc Lab Anim Sci 49: 464- 471.
-
Palombo C, Kozakova M, Guraschi N, Bini G, Cesana F, et al. (2012) Radiofrequency-based carotid wall tracking: a comparison between two different systems. J Hypertens 30: 1614-1619.
-
Milne L, Keehn L, Guilcher A, Reidy JF, Karunanithy N, et al. (2015) Central Aortic Blood Pressure From Ultrasound Wall-Tracking of the Carotid Artery in Children Comparison With Invasive Measurements and Radial Tonometry. Hypertension 65: 1141-1146.
-
Glynn LG, Murphy AW, Smith SM, Schroeder K, Fahey T (2010) Interventions used to improve control of blood pressure in patients with hypertension. Cochrane Database Syst Rev.
-
Parati G, Omboni S (2010) Role of home blood pressure telemonitoring in hypertension management: an update. Blood press monit15: 285-295.
-
Logan AG, Irvine MJ, McIsaac WJ, Tisler A, Rossos PG, et al. (2012) Effect of home blood pressure telemonitoring with self-care support on uncontrolled systolic hypertension in diabetics. Hypertension 60: 51-57.
-
Field MJ (1996) Telemedicine: A guide to assessing telecommunications for health care. National Academies Press.
-
Meystre S (2005) The current state of telemonitoring: a comment on the literature. Telemedicine Journal & e-Health 11: 63-69.





