International Archives of Nursing and Health Care
Self-Perceived Competency-Based Training Needs of Registered Nurses: A Cross-Sectional Exploratory Study
Lap Fung Tsang1*, So Yuen Alice Sham1, Sheung Lan Winnie Law1, Shuk Chun Irene Ho1, Siu Keung Tang2, Ching Yan Kong3, Suk Ying Peggy Wong4 and A Marie Tarrant5
1Nursing Services Division, United Christian Hospital, China
2Department of Medicine & Geriatrics, United Christian Hospital, China
3Orthopaedics & Traumatology department, United Christian Hospital, China
4Nursing Services Department, Hong Kong Special Administrative Region, China
5School of Nursing, The University of Hong Kong, China
*Corresponding author: Lap Fung Tsang, Nursing Services Division, United Christian Hospital, Rm. 5B, 5/F, Block L, 130 Hip Wo Street, Kwun Tong, KLN, Hong Kong Special Administrative Region, China, Tel: 852-52153340, Fax: 852-39495540, E-mail: tsanlf1@ha.org.hk
Int Arch Nurs Health Care, IANHC-3-062, (Volume 3, Issue 1), Review Article; ISSN: 2469-5823
Received: October 19, 2016 | Accepted: February 22, 2017 | Published: February 25, 2017
Citation: Tsang LF, Sham SYA, Winnie SL, Shuk CIH, Tang SK, et al. (2017) Self-Perceived Competency-Based Training Needs of Registered Nurses: A Cross-Sectional Exploratory Study. Int Arch Nurs Health Care 3:062. 10.23937/2469-5823/1510062
Copyright: © 2017 Tsang LF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The aim of this study is to explore a competency-based training need of registered nurses working in United Christian Hospital (UCH) in Hong Kong. This cross-sectional questionnaire study included 876 registered nurses from 3 to 23 August 2015. Data were analyzed using Statistical Package for the Social Sciences® Version 23.0 for Windows®. The response rate of the study was 82.4%. The mean of functional, personal, people & team and organizational effectiveness competency were 2.62, 2.63, 2.49 and 2.48 respectively. The mean of training needs under functional, people & team, personal and organizational effectiveness competency were 6.65, 6.62, 6.23 and 5.95 respectively. Nurses with less self-perceived competency required a higher training needs on care management (r = - 0.9, p = 0.008). A professional development and training framework based on competency for registered nurse was developed. This study sheds light on the strength and direction of training needs and the significantly correlated perspective from senior level managers and RNs.
Keywords
Competency, Training needs, Registered nurse, Personal growth, Professional and Service development
Introduction
An increasing demand for quality of clinical service and safety of clinical procedures in hospitals has become a burden to healthcare staff. Nursing knowledge is growing exponentially and is constantly evolving. Senior level managers are responsible to work out strategies for improving the nurse' competency and work performance. Staff is critical to the continued health of the organization due to being its greatest asset [1]. Obviously, nurses are the biggest party in a hospital. In order to develop nurses to reach the achievable competency at different levels, Nursing Services Division (NSD), thus, emphasizes on staff training and their professional development.
However, allocation of resources specifically for training is always not adequate to fulfill nurses' actual needs. Training activities are time consuming and expensive to develop and deliver [2]. Senior level managers, therefore, make informed decision regarding prioritization of what and how education should be provided for their sub-ordinates. It is crucial to meet the specialized needs of the organization and the individual trainees through tailor-made trainings [3]. Furthermore, it is an essential step in the planning process to perform a training needs assessment because it can help ascertain that educational activities are designed for the purpose of enhancing learning outcomes, improving patient outcomes, and optimizing cost-effectiveness of organizational resources [2].
Training needs analysis (TNA) is commonly used to identify training needs. It is an effective method to determine who and what should be trained based on the perspective of users when planning in training and development [4]. The use of a TNA exercise can support the development of fit-for-purpose programmes of information skills training [5]. It is usually associated with skill development for the workplace [6].
Many of these trainings and educational needs were traditionally based on the perspective of the senior level managers instead of frontline nurses [7]. If organizations develop and organize training without recognizing a needs assessment, it may result in over training, under training or just missing the point all together [1]. Therefore, the TNA is a primary step to provide important information in the development of training programme in order to meet the demands from nurses [8]. Hence, it can facilitate to establish a structural training framework that guides senior level managers to organize appropriate training programmes.
Background
Hospital Authority (HA) has constructed a core competency framework for registered nurses (RNs) to review their competency development. A functional competency, personal competency, people and team competency, and organization effectiveness are specific to assess the competence of the RNs along with progressive to the career ladder [9]. Nurses' professional competence is described as 'a framework of skills reflecting knowledge, attitudes and psycho-social and psycho-motor elements' by World Health Organization (WHO) in 2009 [10]. It is evidently associated with clinical incidence in relation to the safety and quality of patient care [11]. Therefore, the competency is widely accepted to assess the capability of nurses [12].
A professional development is referred to constant commitment to maintain specific skill levels and career paths, and to ensure that a nurse's skills and knowledge are updated and relevant [13]. Nurse should commit professional development to deliver a safe and effective health care [14] although the effectiveness of professional development relies on self-motivating and is valued by nurses [15]. In addition, when organization offers opportunities for providing professional development training for nurses, it may increase nurse retention to some extent [16]. As a result, a professional development is one of the important components to be studied in the TNA because it is able to determine the trainings which aim to strengthen nursing knowledge, skills and attitude towards their job [17].
Personal growth is defined as a journey by which people change and develop throughout the life span [18]. During the growth process, it involves various parts of self, such as cognitions, behaviors and/or emotions [19]. Nurse perceives these changes from work, family and whenever possible affects their capabilities to perform well. According to the core competency constructed by HA, personal growth is no longer addressed. It is deemed necessary to master new athletic skills, and to manage stressors and challenges encountered throughout life [19]. A review stated that a personal growth can facilitate health care providers' ability to consider and respond to concerns around meaning within palliative care when nurses are aware of it [20]. A retrospective study found that the inter-relationship between personal growth and professional development was the strongest [21]. Therefore, when nurse receives appropriate professional training, they become more confident to perform patient care effectively and safely, and that, in turn, leads to personal growth.
Aims of this Research
The aim of this study was to explore the competency-based training needs of registered nurses working in United Christian Hospital (UCH), a district public HA hospital in Hong Kong. The main objectives of this study were: (1) to explore the self-perceived competency level of registered nurses; (2) to explore the self-perceived training needs of registered nurses using a direction of professional development, personal growth, and services development; (3) to explore the training needs from the perspective of their supervisors; and (4) to formulate a competency-based professional development and training framework in UCH.
Methods
Research design
This is a cross-sectional exploratory study from 1200 registered nurses, who were invited to complete a self-administered questionnaire from 3rd to 23rd August 2015 in UCH.
Participants
All nurses in full-time employment were invited to take part in the study. Nurses who were part-time employment, and on leave including maternity leave, annual leave, study leave or no payment leave during the period of data collection were excluded. A 20-minute briefing session about the design of the study and instruction to fill in the questionnaire for senior management was given by LSL and TLF prior to the period of data collection in order to seek their support. Over 20 briefing sessions, in addition, were delivered to other nurses in various departments.
Ethical considerations
The study was approved by the Research Ethics Committee (Kowloon Central/Kowloon East) (KC/KE-15-0050/ER-2). Consent was implied by completion of the questionnaire. All participants were voluntary and had every right to participate or refuse without any reason. Anonymity was preserved for questionnaire distribution and collection. The protocol was complied with the ICH-GCP. To protect the privacy of respondents, all study data were handled in line with HA/Hospital's policy in handling/storage/destruction. Electronic data should be saved in secured computer of the hospital with restricted access. All the raw data will be destroyed after 3 years of the completion of the study.
Procedures
From December 2013 to March 2014, three sessions of focus group composed of general manager (nursing), senior nursing officers (SNOs), nurse consultants (NCs), department operation managers (DOMs) and advanced practice nurses (APNs) were held which identified three directions of nursing training: professional development, personal growth and clinical services development. They were incorporated into the core competency framework and training needs programmes organized in the past two years to develop the questionnaire for the study. The core competencies include functional, personal, people & team, and organizational effectiveness that are further categorized into 11 sub-category competencies including therapeutic and caring relationship, care management, knowledge & skill application, quality and risk management, holistic health, teamwork, people development, personal qualities & attribute, holistic health, operation and resources management, service development, and legal and ethical practice.
The focus of the study was to explore the competency and training needs from registered nurses directly. Therefore, the questionnaire was composed of three parts including demographic data, self-perceived competency level, and self-perceived training needs. DOMs and ward managers (WMs) were invited to evaluate training needs of registered nurses in a separable questionnaire.
Demographic data included gender, age, academic qualification, working unit, number of year in present unit, number of year in present rank and number of year in UCH. Ten sub-competency categories including a total of 32 items of therapeutic and caring relationship, care management, knowledge and skill application, quality and risk management, personal qualities, professional attribute, teamwork, people development, service development, and legal and ethical practice were focused. The participants was instructed to rate from 1 (sometimes meets and needs improvement) to 4 (consistently exceeds the competency requirement).
A self-designed questionnaire of perceived training needs was employed for RN with 56-items. These training needs based on the trainings organized by NSD and HA were framed against three major domains including professional development, personal growth, and service development. The participants identified the training needs using a 10-point Likert Scale (from 1 indicated "No Need" to 10 indicated "Greatest Need") and participants might write down corresponding training needs if there is no mention in the questionnaire. Similarly, fifty-six training needs rated by senior level managers on RN stratified by 5 years of experience of present rank were expressed in a dichotomous (yes/no) response format.
Data analysis
Statistical analysis was performed using the Statistical Package for the Social Sciences® Version 23.0 for Windows [22]. The data files were checked for discordant values and contraindications by a statistician who was not involved in the study. Descriptive data analysis was used for nominal variables and ordinal variables that were expressed in means and standard deviations reported for continuous variables, frequencies and per cents reported for categorical variables. The t-test and ANOVA test were used for evaluating the difference of self-perceived performance and training needs in terms of year of experience of less than 5 from equal to or more than 5. A correlation statistical test was used to determine any association on competency and training needs. A Chi-square test was used to compare two groups when data were categorized. The level of significance was set at P < 0.05. A sample size of 854 was estimated using a confidence level at 95% in a confidence interval of 1.8% in an exact population size of 1200 RNs [23].
Validity and reliability
It is indispensable to measure and report the content validity of questionnaires because of a creation of confidence in measurements of the variables of interest [24]. The questionnaires had undergone a content validity by three senior nurses to ensure a satisfactory level of content validity scale, rating from 1 (irrelevant), 2 (somewhat relevant), 3 (relevant), to 4 (very relevant) [25,26]. The degree of relevance among the domains, the competencies and the training needs in the questionnaire were indicated by a former principal of Institute of Advanced Nursing School, a Chief Nursing Officer (Nursing Education) and MT. Mean relevance scores of each training need was calculated. It was compromised amongst researchers that the mean score of a training need should be at least 3.0 to justify inclusion into the questionnaire. CVI was calculated for each item under various competencies and for the overall questionnaire. Regarding conciseness, design, information, content and understandability of the two questionnaires, the results from the expert panel yielded an overall CVI of 3.9. The three senior nurses and another seven nurses who worked in NSD as an executive partnership (EP) were invited to conduct face validity so that the questionnaire appeared to be appropriate to the study purpose and content [26]. Test-retest reliability was estimated by completing the same tool by TLF and SCY in an interval of one week. A Cronbach's alpha of more than 0.70 was considered good consistency [27]. The Cronbach's alpha for the functional, people & team, personal, and organizational effectiveness competency were 0.89, 0.92, 0.93, and 0.96 respectively.
Results
The response rate from RN of the study was 82.4%. All questionnaires from the above ranks were valid for the purposes of the study. The working experience in present rank of RN was distributed as less than 2 years [202 (23.1%)], between 2 and 5 years [193 (22.0%)], between 5 and 8 years [99 (11.3%)], and more than 8 years [382 (43.6%)].
Self-perceived Competency
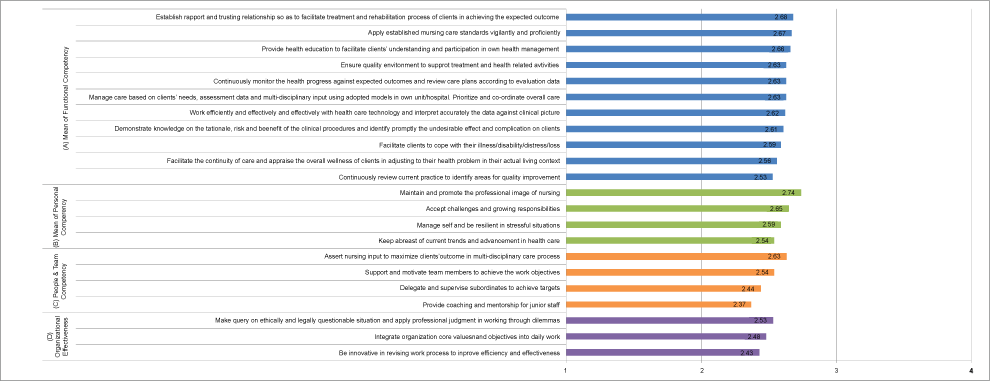
A demographic data was shown in table 1. The overall mean of self-perceived competency was 2.58. The mean of functional, personal, people & team and organizational effectiveness competency were 2.62, 2.63, 2.49 and 2.48 respectively (Figure 1).
.
Figure 1: Mean of self-perceived functional, personal, people & team, and organizational effectiveness competency.
View Figure 1
![]()
Table 1: Demographic data of the participants.
View Table 1
Under different self-perceived competencies, the following areas should be addressed using a mean of each sub-competency as a cutoff.
Functional competency
• Continuously review current practice to identify areas for quality improvement.
• Facilitate the continuity of care and appraise the overall wellness of clients in adjusting to their health problem in their actual living context.
• Facilitate clients to cope with their illness/disability/distress/loss.
• Demonstrate knowledge on the rationale, risk and benefit of the clinical procedures and identify promptly the undesirable effect and complication on clients.
Personal competency
• Manage self and be resilient in stressful situations.
• Keep abreast of current trends and advancement in health care.
People & team competency
• Delegate and supervise subordinates to achieve targets.
• Provide coaching and mentorship for junior staff.
Organizational effectiveness competency
• Be innovative in revising work process to improve efficiency and effectiveness.
• Integrate organization core values and objectives into daily work.
Analysis of self-perceived competency using a 5-year in present rank as a cutoff
When stratified by five-year in present rank of participants, the functional (t = 8.18, df = 2, < 0.0001), personal (t = 5.91, df = 2, < 0.0001), people & team (t = 9.39, df = 2, < 0.0001) and organizational effectiveness competency (t = 6.14, df = 2, < 0.0001) were found to have a significant difference in self-perceived competency (Table 2). Participants were found to have a significant improvement in all self-perceived sub-competencies with the increase in years of present unit, present rank and years in UCH using ANOVA test (Table 3). It was revealed that nurses with less self-perceived competency had a higher training needs on care management (r = - 0.9, p = 0.008).
![]()
Table 2: Comparing self-perceived competency and self-perceived training needs with the number of year in present rank.
View Table 2
![]()
Table 3: A significant improvement of senior registered nurses under years of present unit, present rank and years in UCH for all self-perceived sub-competencies.
View Table 3
Self-perceived training needs
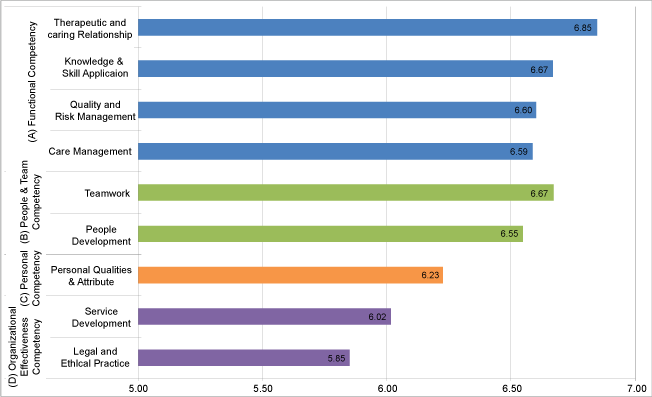
The overall mean of self-perceived training needs was 6.48 (SD = 1.54). The mean of training needs under functional, people & team, personal and organizational effectiveness competency were 6.65 (SD = 1.56), 6.62 (SD = 1.77), 6.23 (SD = 1.75) and 5.95 (SD = 1.93) respectively (Figure 2). Junior registered nurses reflected that they needed more training on care management [F(3,872) = 11.04, P < 0.0001], and knowledge & skills management [F(3,871) = 3.32, P = 0.019]. Conversely, senior registered nurses required more training on people development [F(3,870) = 3.15, P = 0.024], and service development [F(3,868) = 11.04, P = 0.005].
.
Figure 2: Mean of self-perceived training needs on functional, personal, people & team, and organizational effectiveness competency.
View Figure 2
Analysis of training needs using a mean of self-perceived training needs as a cutoff
When using a mean of self-perceived training needs as a cutoff under functional competency, a total of 17 trainings are important to the nursing development including chronic disease management, workplace violence, communication skills, motivational interview skills, risk management, basic & advanced life and death education, emergency preparedness and contingency plan, transportation of critically ill patient, pharmacology for nurses, complaint management, wound management, resuscitation skills, post-registration certificate course in specialty nursing, and managing difficult clients.
When using a mean of self-perceived training needs as a cutoff under people & team competency, a total of 3 trainings are important to the nursing development including clinical mentorship, anger and conflict management, and crisis management.
When using a mean of self-perceived training needs as a cutoff under personal competency, a total of 7 trainings are important to nursing development including effective meeting skills, clinical supervision & ward management skills enhancement, effective presentation skills, managing EQ at work, advanced writing, clinical leadership & management skills enhancement, and decision making and analytical skills.
When using a mean of self-perceived training needs as a cutoff under organizational effectiveness competency, a total of 4 trainings are important to the nursing development including lean management, project management, Hospital Authority Bylaws and security management, and change management.
Training needs perceived by DOM/NC/SNO on RN
Under a functional competency, nine out of 29 training needs perceived from RN of more than 5 years of experience were found to have a significant difference from that from DOM/NC/SNO including nurse-patient relationship (X2 = 5.76, df = 1, p = 0.016), clinical communication skills (X2 = 10.87, df = 1, p = 0.001), patient safety (X2 = 4.07, df = 1, p = 0.044), resuscitation skills (X2 = 11.84, df = 1, p = 0.001), transportation of critically ill patient (X2 = 6.1, df = 1, p = 0.013), wound management (X2 = 7.48, df = 1, p = 0.006), workplace violence (X2 = 11.42, df = 1, p = 0.001), introduction of continence care (X2 = 5.39, df = 1, p = 0.02), and pharmacology for nurses (X2 = 3.88, df = 1, p < 0.05). Conversely, two out of 15 training needs perceived from RN of more than 5 years of experience were found as high as that from DOM/NC/SNO including mindfulness-based wellness resilience (66.6% vs. 94.1%, X2 = 5.67, df = 1, p = 0.017), and decision making and analytical skills (76.2% vs. 100%, X2 = 4.96, df = 1, p = 0.026) under a personal competency. Under an organizational effectiveness competency, one out of 7 training needs perceived from RN with more than 5 years of experience were found as high as that from DOM/NC/SNO including lean management (66.6% vs. 91.3%, X2 = 6.13, df = 1, p = 0.013).
On the other hand, two out of 9 training needs perceived from RN with less than 5 years of experience were found to have a significant difference from DOM/NC/SNO including advanced supervisory skills (X2 = 4.84, df = 1, p = 0.028), and advanced writing (X2 = 8.69, df = 1, p = 0.003) under a people & team competency. Two out of 15 training needs perceived from RN with less than 5 years of experience were found to have a significant difference from DOM/NC/SNO including effective meeting skills (X2 = 10.09, df = 1, p = 0.001), and advanced writing (X2 = 8.69, df = 1, p = 0.003) under a personal competency. Conversely, ten out of 29 training needs perceived from RN with less than 5 years of experience were found as high as that from DOM/NC/SNO including nurse-patient relationship (69.4% vs. 88%), patient health assessment on admission (67.5% vs. 92%), patient discharge planning (73.7% vs. 95.8%), patient safety (66.6% vs. 92%), patient documentation (65.3% vs. 88%), primary nursing (66.2% vs. 88%), evidence-based practice (73.5% vs. 94.4%), use of nursing informatics system (70% vs. 100%), occupational safety and health (66.3% vs. 90.9%), and basic concept on continuous quality improvement (64.8% vs. 95.5%) under a functional competency. One out of 9 training needs perceived from RN with less than 5 years of experience was found as high as that from DOM/NC/SNO including workplace staff relationships (65.9% vs. 96%) under a people & team competency. Two out of 15 training needs perceived from RN with less than 5 years of experience were found as high as that from DOM/NC/SNO including self-care and resilience on nursing (64.6% vs. 92.9%), and managing EQ at work (69.8% vs. 100%) under a personal competency.
Training needs perceived by WM on RN
Under a functional competency, one out of 29 training needs perceived from RN with more than 5 years of experience were found to have a significant difference from WM including wound management (X2 = 7.48, df = 1, p = 0.006). Conversely, one out of 9 training needs perceived from RN with more than 5 years of experience was found as high as that from WM including crisis management (81.9% vs. 96.6%). Two out of 15 training needs perceived from RN with more than 5 years of experience was found as high as that from WM including mindfulness-based wellness resilience (66.6% vs. 90.9%), and decision making and analytical skills (76.2% vs. 95.5%) under a personal competency. One out of 7 training needs perceived from RN with more than 5 years of experience was found as high as that from WM including lean management (66.6% vs. 88.2%) under an organizational effectiveness competency.
Interestingly, some training needs perceived from RN with less than 5 years of experience were not as high as that from WM including effective meeting skills (67.4% vs. 33.3%), advanced writing (69% vs. 20%), clinical leadership & management skills enhancement (72.4% vs. 20%), and clinical supervision & ward management skills enhancement (69.1% vs. 21.4%) under a personal competency.
Fifteen out of 29 training needs perceived from RN with less than 5 years of experience was found as high as that from WM including nurse-patient relationship (69.4% vs. 97.3%), clinical communication skills (76.5% vs. 97.3%), patient health assessment on admission (67.5% vs. 94.6%), patient discharge planning (73.7% vs. 94.6%), patient safety (66.6% vs. 100%), patient documentation (65.3% vs. 97.3%), primary nursing (66.2% vs. 94.6%), resuscitation skills (85.6% vs. 97.3%), life and death education (82% vs. 96.9%), workplace violence (70.4% vs. 97.2%), introduction of continence care (74% vs. 91.7%), evidence-based practice (73.5% vs. 96.4%), use of nursing informatics system (70% vs. 100%), occupational safety and health (66.3% vs. 96.4%), and basic concept on continuous quality improvement (64.8% vs. 96.6%) under a functional competency. Three out of 9 training needs perceived from RN with less than 5 years of experience was found as high as that from WM including workplace staff relationship (65.9% vs. 94.3%), basic supervisory skills (70.9% vs. 92.3%), clinical mentorship training (71% vs. 94.4%) under a people & team competency. Three out of 15 training needs perceived from RN with less than 5 years of experience was found as high as that from WM including self-care and resilience in nursing (64.6% vs. 84%), mindfulness-based wellness resilience (62.4% vs. 88.2%), and managing EQ at work (69.8% vs. 92.6%) under a personal competency.
Professional development and training framework on competency for registered nurse
A professional development and training framework on competency for registered nurse was developed according to the mean of self-perceived training needs using a cutoff by five-year in present rank (Table 4).
![]()
Table 4: A professional development and training framework on competency for registered nurses below or equal to 5 years, and more than 5 years of present rank.
View Table 4
Discussion
According to a competence literature review undertaken by [28], competency and competence are not necessarily synonymous. Competency refers to one's actual performance in a situation whereas competence points to a potential ability and/or a capability to function in a given situation. Thus, competence is required before a nurse can expect to achieve competency. Although Meretoja with her research group has studied and published a lot of results concerning nurses' competence level [29-31]. We aimed to determine nurse's competency by comparing current work functioning with established competency frameworks developed in the Hospital Authority according to a registered nurse's role in this study.
A high response rate (82.4%) of this study revealed that registered nurses were appreciated to reflect their self-perceived competencies and training needs. The main reason was that there was no similar study conducted in the past to explore the true training needs for RN. They had demonstrated an open-minded attitude to support the study and agreed with the direction and value of the study. It was because the study would have an influence on their career pathway and progression development. In addition, it might be partly because of the efforts made by DOM and WM, who gave nurses the opportunity and time to complete the questionnaire and briefed them of the significance of this study in future planning of nursing training. Thus, it reflected that RN hoped to acquire more skills and knowledge to improve quality and safety to perform nursing care and to cope with service needs.
Any perceived training that meant nurses could not carry out their jobs competently was addressed immediately as evident made by that nurses with less self-perceived competency required a higher training need. In this study, nurses perceived they were weak at competencies related to quality improvement, patient wellness, disease-related management, self-resilience, and method for clinical workflow improvement. Interestingly, in spite of a low rating of people and team competency, and organizational effectiveness competency, training needs perceived by RN on these competencies were not as high as expected. It was because the existing training structure in the Hospital Authority emphasizes on skill and knowledge of nursing care at the beginning phase. Secondly, delegation, supervision and some matters required to integrate organization core value and direction into practice were not a major role of junior nurses so that it was not surprising that they perceived to have a low competency in those areas. For the same reason, this could explain why these training needs were not ranked at a high priority. Notwithstanding the low training needs perceived from junior nurses, delegation and supervision are of utmost importance to ensure patient safety and patient outcomes from the viewpoint of senior level managers and ward managers. This finding was comparable to other studies that suggested junior nurses need to improve their delegation skills [32,33]. In clinical settings, there are other healthcare workers like healthcare assistance and nursing students who should be supervised and delegated safely. Otherwise, inefficient workload distribution, insufficient supervision of delegated tasks and key aspects of care being missed, duplicated and incorrectly performed may happen [34,35]. In future, it is essential to re-educate them the importance of a variety of degree of delegation and supervision in clinical settings even though they are the junior nurses.
This study used a 5-year as a cutoff point to define junior from senior nurse. In fact, it is particularly difficult to have a clear definition of the term "junior nurse". In a study of [36], a junior nurse does not have much experience to respond creatively to somewhat complex care situations. According to the career progression framework for nursing in Hospital Authority, nurses who obtained at least 5 years of working experience would generally be considered for studying specialty training programme. As a result, the data were analysed by a stratification of 5-year to explore the difference of competencies and training needs.
One of the strengths in this study was to analyse self-perceived competency and training needs towards 3 major domains like personal growth, professional development, and service development. When stratified by 5 years of present rank to compare the difference of training needs, it was discovered that junior RN emphasized professional development training whereas senior RN focused on personal growth training. Lots of practicing nurses, indeed, complained of junior nurse's insufficient competence [37]. The finding supported that professional development trainings were not sufficient for junior RN.
In the study, the difference between senior level managers and RNs on training needs was compared. Obviously, senior level managers did not completely understand training needs from what RNs expected in some domains. Traditionally, DOMs and WMs usually nominate senior and junior RNs subject to their performance, competencies and other factors based on their perception. They might think that respective trainings should be matched with the seniority of RN regardless of their true competencies. The fact is that no matter how experience nurses work in clinical setting, they still need the relevant trainings as what junior nurses perceive. Nursing Services Division, therefore, requires keeping on conducting a team alignment and culture transformation across different levels of nurses to ensure everyone understand the direction and strategy of planning in nursing. It is an effective programme to promote team spirit, reinforce commitment and professional vocation in the career pathway, and the 3-year nursing strategic plan of UCH.
An effective functioning of the healthcare system is highly dependent on competent health services management workforce [38]. A nursing professional development specialist designs different training programmes for different levels of nurses to enhance their competencies. The nursing professional development specialist indeed requires a tool to understand the financial implications of workforce and dynamic changes of manpower. This study provides an opportunity for senior level managers and RNs to express their desires and feedbacks. It also guides the nursing professional development specialist to provide respective trainings for various levels of RNs so as to prevent mis-allocation of resources.
Training facilitates nurses to provide an opportunity and broad structure for the professional development. Besides, it helps nurses in attaining personal growth. Under a theory of personality, training needs analysis may serve as a tool for transactional analysis and a systematic psychotherapy for personal growth and personal change [39]. Based on the findings, RNs expressed their training needs to support their personal growth. In future, the TNA should be conducted periodically to create a continual review cycle of professional development and training [40]. It can promote an ongoing commitment to providing effective professional development opportunities and training.
Conclusions
This study sheds light on the strength and direction of training needs and the significantly correlated perspective from senior level managers and RNs. The findings of this study suggest that senior RNs need to have trainings on personal growth whereas junior RNs need to have trainings on professional development to strengthen their competencies. A professional development and training framework based on competency for registered nurse was developed. The TNA helped to create a positive reviewing process on professional development opportunity and training addressing nurses' learning requirements in the upcoming 3 years.
Implications for Nursing Management
The results of this study indicate that it is essential to develop a competency-based training framework to guide professional development specialists on planning of optimal trainings for registered nurses. As a senior manager, it is vital important to address on the needs of registered nurses to develop their competencies effectively and efficiently based on the requirements from an organization. In addition, a gap of respective training needs between senior management and registered nurses was noted. It is evidently to draw attention from senior nurse managers that training needs for RNs are not often the same as what they perceive.
Limitations
There are a lot of training programmes for various objectives. Thus, it is difficult to include all categories of training programme in the questionnaire. However, respondents might write down other training needs they intend to have.
On the other hand, there are different ways to collect relevant information from nursing staff [41] illustrated some examples such as practice experience, reflection, questioning, practice audits, self-assessment tests, peer interview and other sources. Considering that a structural training framework should be designed in the upcoming years, a survey is the most appropriate TNA data collection tool. Some argued that a questionnaire including lists of training needs might shape the respondents to consider the itemized training needs solely and neglect other potential trainings. This issue was brought to discuss in our study panel and came to a conclusion that such questionnaire design could stimulate and guide the respondents to perceive their training needs based on the three major domains.
RNs from different departments were given multiple identical briefing sessions. For those who did not attend the session and had queries on the study, they were encouraged to contact corresponding authors to ensure all data were valid.
Acknowledgement
The authors would like to heartfelt thanks to all nurses to support this study.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of Interest
No conflict of interest has been declared by the authors.
References
-
Devi VR, Rao MM (2012) Training needs identification of nursing staff - a case study of a health care organization. EXCEL International Journal of Multidisciplinary Management Studies 2: 147-153.
-
Pilcher J (2016) Learning Needs Assessment: Not Only for Continuing Education. J Nurses Prof Dev 32: 122-129.
-
Brown J (2002) Training needs assessment: A must for developing an effective training program. Public Personnel Management 31: 569-578.
-
Salas E, Cannon-Bowers JA (2001) The Science of Training: A Decade of Progress. Annu Rev Psychol 52: 471-499.
-
Hamilton S (2013) Assessing knowledge skills in the NHS: a training needs analysis approach. Health Info Libr J 30: 168-173.
-
Barnes C (2014) Education and training -What's the difference?
-
Gould D, Kelly D, White I, Chidgey J (2004) Training needs analysis. A literature review and reappraisal. Int J Nurs Stud 41: 471-486.
-
Dierdoff CE, Surface EA (2008) Assessing training needs: Do work experience and capability matter? Human Performance 21: 28-48.
-
(2005) Core Competency for Enrolled Nurses, Registered Nurses & Advanced Practice Nurses in Hospital Authority.
-
World Health Organization (WHO) (2009) Global standards for the initial education of professional nurses and midwives. Nursing & Midwifery Human Resources for Health.
-
Nilsson J, Johansson E, Egmar AC, Florin J, Leksell J, et al. (2014) Development and validation of a new tool measuring nurses self-reported professional competence - The nurse professional competence (NPC) Scale. Nurse Educ Today 34: 574-580.
-
Lima S, Newall F, Kinney S, Jordan HL, Hamilton B (2014) How competent are they? Graduate nurses self-assessment of competence at the start of their careers. Collegian 21: 353-358.
-
Lannon S (2007) Leadership skills beyond the bedside: Professional development classes for the staff nurse. J Contin Educ Nurs 38: 17-23.
-
Gould D, Drey N, Berridge EJ (2007) Nurses' experience of continuing professional development. Nurse Educ Today 27: 602-609.
-
Cooper E (2009) Creating a culture of professional development: a milestone pathway tool for Registered Nurses. J Contin Educ Nurs 40: 501-508.
-
Ulrich B, Buerhaus P, Donelan K, Norman L, Dittus R (2005) How RNs view the work environment: Results of a national survey of registered nurses. J Nurs Adm 35: 389-396.
-
Sinha D, Sinha S (2009) Training needs analysis Personal growth and training & development India: Word-press 139-148.
-
Weigold IK, Weigold A, Russell EJ, Drakeford NM (2014) Examination of the psychometric properties of the personal growth initiative scale-II in African American college students. Assessment 21: 754-764.
-
Robitschek C, Ashton MW, Spering CC, Geiger N, Byers D, et al. (2012) Development and psychometric evaluation of the Personal Growth Initiative Scale-II. J Couns Psychol 59: 274-287.
-
Moreno P, and Stanton A (2013) Personal growth during the experience of advanced cancer: a systemic review. Cancer J 19: 421-430.
-
Gribble N, Dender A, Lawrence E, Kirrily Manning, Falkmer T (2014) International WIL placements: Their influence on student professional development, personal growth and cultural competence. Asia-Pacific Journal of Cooperative Education 15: 107-117.
-
(2015) IBM Corp Released 2015 IBM SPSS Statistics for Windows Version 230 IBM Corp, Armonk, New York.
-
(2014) Sample size calculation. MaCorr Research.
-
Yaghmaie F (2003) Content validity and its estimation. Journal of Medical Education 3: 25-27.
-
Polit DF, Beck CT (2006) The content validity index: are you sure you know what's being reported? Critique and recommendations. Res Nurs Health 29: 489-497.
-
Nasrin P, Trisha D (2009) Developing and validating a questionnaire to measure spirituality: a psychometric process. Global Journal of Health Science 1: 2-11.
-
Streiner DL, Norman RG (2003) Health measurement scales: a practical guide to their development and use. (3rd edn), Oxford University Press.
-
Schroeter K (2008) Competence literature review. Competency & Credentialing Institute.
-
Meretoja R, Koponen L (2012) A systematic model to compare nurses' optimal and actual competencies in the clinical setting. J Adv Nurs 68: 414-422.
-
Meretoja R, Numminen O, Iso-Aho H, Leino-kilpi H (2014) Nurse competence between three generational nurse cohorts: A cross-sectional study. International Journal of Nursing Practice.
-
Meretoja R, Leino-Kilpi H, Kaira AM (2004) Comparison of nurse competence in different hospital work environments. J Nurs Manag 12: 329-336.
-
Curtis E, Nicholl H (2004) Delegation: a key function of nursing. Nurs Manag (Harrow) 11: 26-31.
-
Weydt A (2010) Developing delegation skills. The Online Journal of Issues in Nursing 15.
-
Anthony MK, Vidal K (2010) Mindful communication: a novel approach to improving delegation and increasing patient safety. The Online Journal of Issues in Nursing 15.
-
Standing TS, Anthony MK (2008) Delegation: what it means to acute care nurses. Appl Nurs Res 21: 8-14.
-
Kieft RA, de Brouwer BB, Francke AL, Delnoij DM (2014) How nurses and their work environment affect patient experiences of the quality of care: a qualitative study. BMC Health Serv Res 14: 249.
-
Duchscher JB (2008) A process of becoming: The stages of new nursing graduate professional role transition. J Contin Educ Nurs 39: 441-450.
-
Liang Z, Leggat SG, Howard PF, Koh L (2013) What makes a hospital manager competent at the middle and senior levels? Aust Health Rev 37: 566-573.
-
Lall M, Sharma S (2009) Transactional Analysis Personal growth and training & development (1st edn) Excel Books, New Delhi 134.
-
Pennington H (2011) Using a training needs analysis framework in career development. Nurs Manag (Harrow) 18: 32-36.
-
Norman GR, Shannon SI, Marrin ML (2004) The need for needs assessment in continuing medical education. BMJ 328: 999-1001.





