Obstetrics and Gynaecology Cases - Reviews
Long Term Triptorelin Therapy in a Large Endometriosis Nodule Arising in an Episiotomy Scar
Basma Darwish1, Gregoire Leleup2, Cécile Martin2 and Horace Roman1,3*
1Department of Obstetrics and Gynecology, Rouen University Hospital, France
2Department of Radiology, Rouen University Hospital, France
3Research Group 4308 ‹‹ Spermatogenesis and Gamete Quality ››, IHU Rouen Normandy, IFRMP23, Reproductive Biology Laboratory, Rouen University Hospital, France
*Corresponding author: Horace Roman, Department of Obstetrics and Gynecology, Rouen University Hospital-Charles Nicolle, 1 rue de Germont, 76031 Rouen, France, Tel: (33) 232 888 754, Fax: (33) 235 981 149, Email: horace.roman@gmail.com
Obstet Gynecol Cases Rev, OGCR-2-039, (Volume 2, Issue 3), Case Report; ISSN: 2377-9004
Received: May 04, 2015 | Accepted: May 23 2015 | Published: May 26, 2015
Citation: Darwish B, Leleup G, Martin C, Roman H (2015) Long Term Triptorelin Therapy in a Large Endometriosis Nodule Arising in an Episiotomy Scar. Obstet Gynecol Cases Rev 2:039. 10.23937/2377-9004/1410039
Copyright: © 2015 Darwish B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Endometriosis is the extra-uterine presence of endometrial glands and stroma, most often in the pelvis. It is very occasionally found in extra-abdominal sites. Perineal endometriosis is the presence of endometrial tissue in the perineal sites. Endometriosis of the perineum and vulva is extremely rare, with the most common site being episiotomy scars.
Case presentation: We present the management of a 41-year old patient presenting with a 60 mm-diameter endometriosis nodule in an episiotomy scar. Due to the large nodule size, exclusive medical treatment was proposed instead of radical surgery. The patient received continuous therapy by triptorelin associated with add-back therapy for 36 months, leading to a decrease in nodule volume by 67% and the disappearance of all painful complaints. The treatment was then followed by a progestin upon absence of symptoms. No bone mineral density changes were revealed or other adverse events recorded. The patient is willing to continue medical therapy until menopause.
Conclusion: Medical therapy can successfully be used in the treatment of endometriosis nodule in an episiotomy scar when aesthetic and functional results cannot be assured by surgical treatment. Triptorelin can be used on a long - term basis when associated with an add-back therapy with no adverse effects.
Keywords
Deep endometriosis, Triptorelin, Add-back therapy, Medical therapy, Episiotomy scar
Abbreviations
BMD: Bone Mineral Density, GnRHa: Gonadotrophin Releasing Hormone Agonist, MRI: Magnetic Resonance Imaging, AMM: Autorisation de Mise sur le Marche (French Drug Administration Agency)
Background
Endometriosis is defined as the presence of functioning endometrial tissue outside of the uterine cavity, and affects 6 to 10% of all women of childbearing age [1]. Endometriosis most commonly involves pelvic organs such as ovaries, uterosacral ligaments, the Douglas pouch or bowel, and only rarely spreads beyond the pelvic region. The prevalence of endometriosis implants in the perineum is rare, and usually follow vaginal deliveries. Endometriosis nodules arising in an episiotomy scar have been but rarely reported in literature and hence there are no definitive treatment recommendations. Several authors after extrapolation of data concerning the management of pelvis endometriosis have however suggested wide surgical excision of those nodules as the most suitable option [2-6]. To bring new data to this topic, we report a case of a large episiotomy scar endometriosis nodule, for which esthetic considerations rendered wide excision inappropriate. Treatment was thus exclusively medical and resulted in excellent outcomes, which will be followed until the menopause. Menopause is a natural biological process defined as occurring 12 months after the last menstrual period and marks the end of menstrual cycle. While on treatment as used in our case, menopause can be determined by the appearance of menopause-associated symptoms which may include hot flushes and night sweats.
Case Presentation
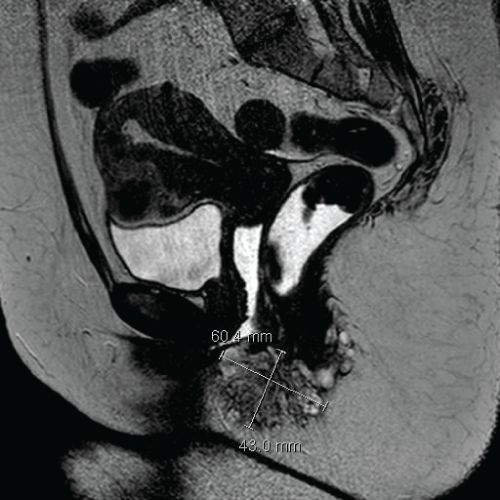
A 41-year old woman was referred to our department in April 2011 for advice concerning a large endometriosis nodule which had grown over time into an episiotomy scar. She had delivered twice 18 and 13 years before, with a right medio-lateral episiotomy performed each time. A year after the second delivery, the patient felt a small swelling at the episiotomy site and ten years later, when she completely abandoned contraceptive pill intake, she observed rapid growth of the swelling, which became larger and more painful during menses. Clinical gynecological examination revealed a solid tender mass 5 to 6cm in diameter, on the episiotomy site and close to the internal anal sphincter. Biopsy of the lesion revealed multiple endometriosis foci surrounded by fibrous tissue. Magnetic resonance imaging (MRI) showed a large endometriosis nodule of diameter attaining 60mm, with an estimated volume of 37.94cm3 (Figure 1). As wide excision would have led to an uncertain esthetic results, first line medical treatment by triptorelin was proposed (Decapeptyl� 11.25mg every 3 months, IPSEN Pharma, Boulogne Billancourt, France) associated with add back therapy by percutaneous estradiol (Estreva� 0.1%, 0.5 mg/day, TEVA Sante, Paris-La Defense, France) to induce prolonged therapeutic amenorrhea. Three months later, the patient was completely pain free, and the treatment thus prolonged for a year. The patient was reviewed yearly thereafter with a follow up MRI before every visit for clinical evaluation and an assessment of bone mineral density (BMD).
.
Figure 1: Sagittal magnetic resonance imaging section revealing the endometriosis nodule before treatment
View Figure 1
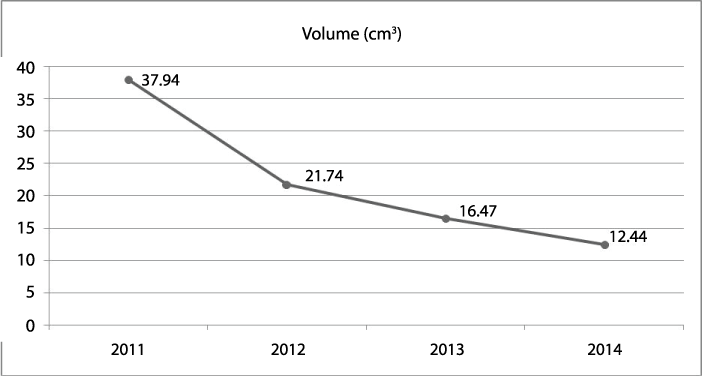
MRI examinations showed progressive significant reduction in the nodule size with volume measurements of 21.74cm3, 16.47cm3 and 12.44cm3, at 1, 2 and 3 years respectively, representing an overall volume reduction of 67.2% (Figure 2, Supplementary Figures 1-3).
.
Figure 2: Progressive decrease of the volume of the endometriosis nodule during therapy using triptorelin.
View Figure 2
.
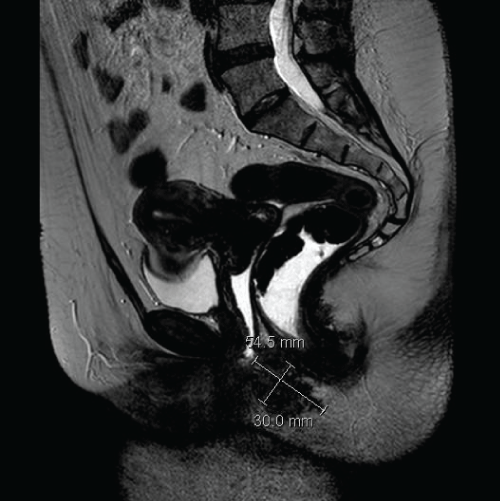
Supplementary Figure 1: Sagittal magnetic resonance imaging section showing the endometriosis nodule performed after 1-year therapy using triptorelin
View Supplementary Figure 1
Volume was calculated using the ellipsoid volume formula (volume=4/3*π*r1*r2*r3 where r is the radius in each of the 3 axes). Bone mineral density was assessed yearly showing unchanged normal results. Three years later, the patient is asymptomatic and has not experienced any adverse effects.
.
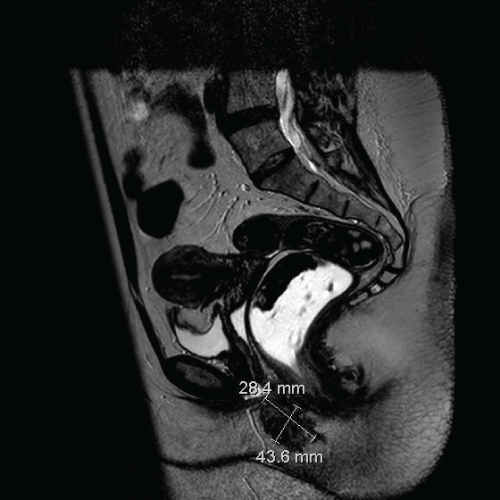
Supplementary Figure 2: Sagittal magnetic resonance imaging section showing the endometriosis nodule performed after 2-year therapy using triptorelin
View Supplementary Figure 2
.
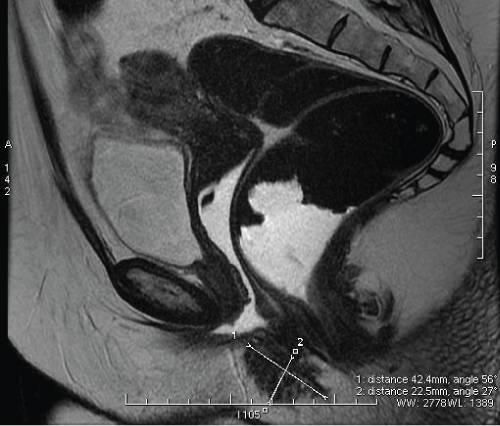
Supplementary Figure 3: Sagittal magnetic resonance imaging section showing the endometriosis nodule performed after 3-year therapy using triptorelin
View Supplementary Figure 3
Clinical examination shows a significant reduction in tumor size with a lack of tenderness on palpation (Supplementary Figures 4,5). Due to the patient's entire satisfaction and the positive results obtained from medical treatment, it was decided to carry on the therapy up to menopause. Due to the high expenses related to the use of triptorelin, the success of medical treatment and the ability to thus obtain similar results, decision was made to continue treatment with progestins instead, using chlormadinone acetate thereafter.
.
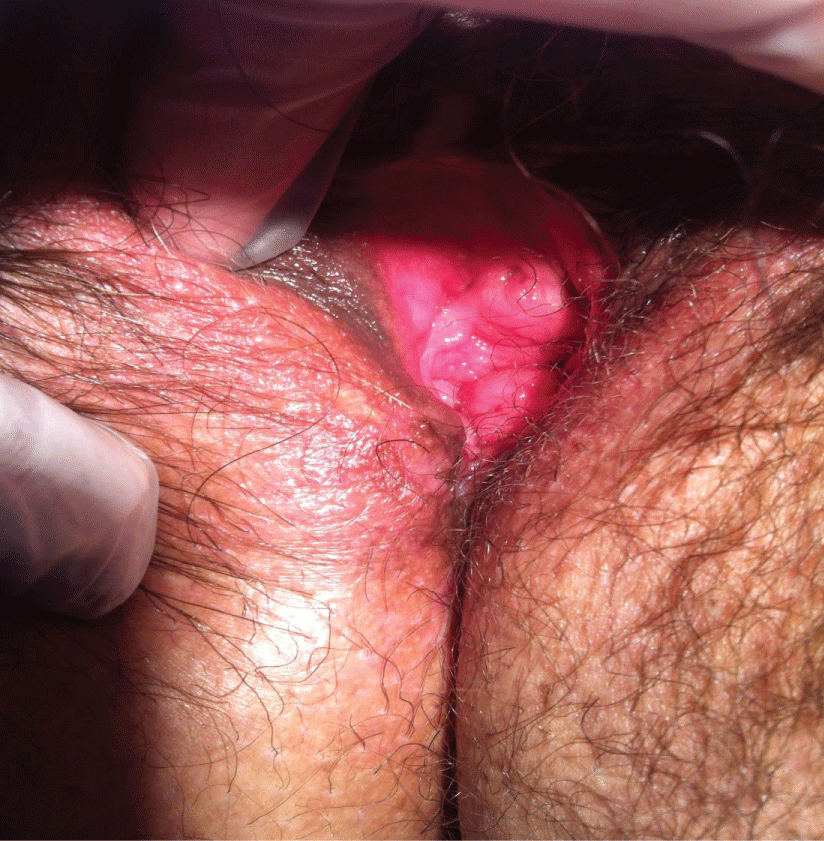
Supplementary Figure 4: Endometriosis nodule after 3-year therapy using triptorelin
View Supplementary Figure 4
.
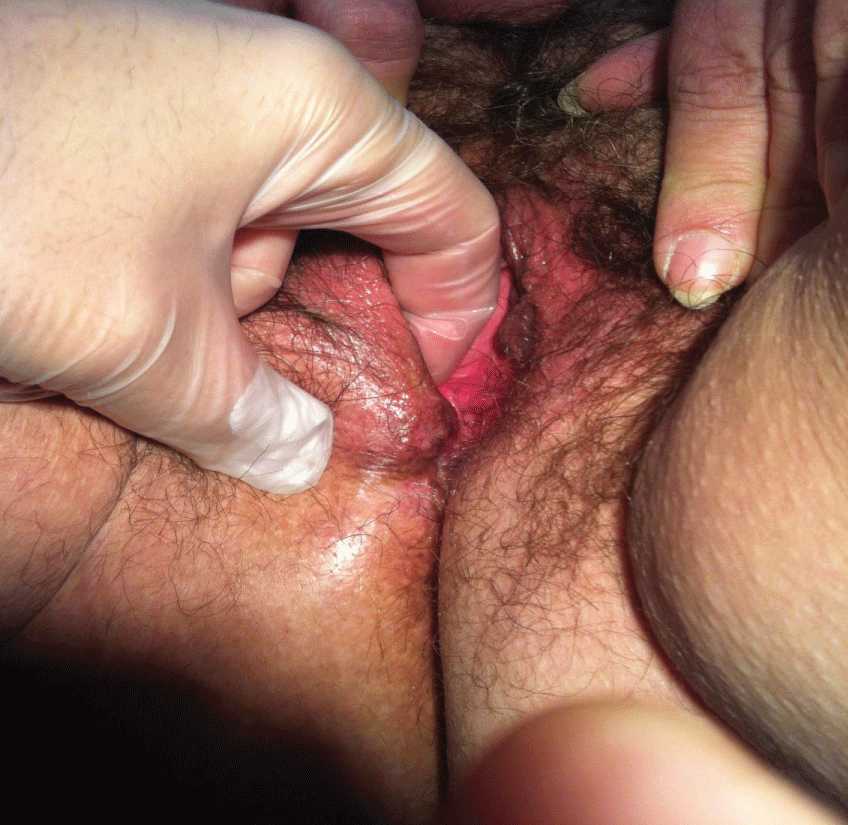
Supplementary Figure 5: Painless endometriosis nodule after 3-year therapy using triptorelin
View Supplementary Figure 5
Comment
We report a case of unusual localization of endometriosis implant, in which exclusive medical treatment led to excellent outcomes. A review of the literature shows that wide excision is the treatment advocated by the majority of authors [2-6] but that the number of reported cases of endometriosis nodule at an episiotomy site reported in the literature is too small to provide conclusions on the most appropriate treatment. It is our belief that the collection of such case reports or case-series may contribute to improved knowledge in this specific topic.
The pathogenesis of the nodule may be explained by the direct implantation of endometrial cells following vaginal delivery, somehow similar to that of nodules developing in cesarean scars. Clinical history is crucial in the diagnosis and choice of the management. Reproductive age, previous vaginal delivery with episiotomy, and the presence of palpable nodules accompanied by cyclic changes during menses should be taken into account.
Due to the proximity of anal sphincter, wide excision of such nodules may be challenging. Furthermore, when the volume to excise is large, repair of the vulva and vaginal vestibule can also be difficult and responsible for postoperative dyspareunia. These circumstances were the determining factors in our case, leading us to privilege medical treatment over surgery.
Since hormonal therapies are not curative of endometriosis but only suppressive, they should be continuously administered. Triptorelin� is a gonadotropin-releasing hormone agonist (GnRHa) which inhibits the release of luteinizing hormone and follicle stimulating hormone, and leads to ovarian suppression similar to a reversible post-menopausal state. When administered for 6 consecutive months, GnRHa can reduce the volume of deep endometriosis nodules by up to 30% [7]. However, disruption of the therapy is immediately followed by nodule growth [7]. In our case, 3-year administration of GnRHa was followed by significant regression in nodule volume to 33% of baseline value. In a recent randomized trial, Angioni et al. [8] showed that GnRHa administered in patients with incomplete resection of deep endometriosis allowed for an improvement in pain similar to that recorded in women with complete surgery. However, favorable outcomes disappeared shortly after finishing treatment, leading to the conclusion that medical therapy is a valuable tool when the main goal is reducing symptoms over and above mandatory resection of endometriosis implants, and when it is administered continuously.
In our case the GnRHa was administered until a significant reduction in nodule volume and the disappearance of symptoms was achieved, allowing the administration of medical treatment by progestins, a decision made mainly due to the high expenses of such treatment and the possibility to maintain the same results already achieved.
The major adverse effect of GnRHa is the loss of BMD, and is therefore recommended as a second line therapy [9] with administration from 6 to 12 months [10]. To prevent side effects of GnRHa, add-back therapy should be routinely used without impairing the therapeutic result [9]. Several authors have reported long time administrations of GnRHa in combination with add-back therapy, with no adverse effects [11]. On this basis, exclusive medical therapy can be used up to menopause in older patients presenting with deep endometriosis in which wide excision can lead to unfavorable functional or esthetic outcomes. Patients should be carefully selected when initiating add-back therapy as estrogen treatment may increase the risk of morbidity in a small number of women. Serious risks are vascular and may include deep vein thrombosis or stroke. When GnRHa therapy is administered, we perform a yearly assessment of BMD to evaluate the absence of risk of osteoporosis. To date, no patient has had medical treatment disrupted due to abnormal BMD results.
In patients where add-back therapy by estradiol is contraindicated, the AMM (Drug administration agency) in France recommends the use of GnRHa for a limited duration of up to 6 months to avoid loss of BMD.
Consent
Informed consent was obtained from the patient for publication of this case report and any accompanying images.
Study Funding/Competing Interest
H.R. reports personal fees for participating in a master class organized by IPSEN Pharma (Boulogne-Billancourt, France). B.D, C.M. and G.L. declare no conflict of interest. No financial support was received for this study.
Author's Contributions
H.R. and B.D. performed acquisition and interpretation of data, and wrote the first draft of the report. H.R. attended the patient. G.L. and C.M. performed magnetic resonance imaging examinations. All authors contributed to the writing of the final manuscript.
References
-
Giudice LC, Kao LC (2004) Endometriosis. Lancet 364: 1789-1799.
-
Adamo V, Di Natale W, Meola C, Gilio M, Cavalli S, et al. (2004) Endometriosis in an episiotomy scar: a case report. Chir Ital 56: 735-738.
-
Barisic GI, Krivokapic ZV, Jovanovic DR (2006) Perineal endometriosis in episiotomy scar with anal sphincter involvement: report of two cases and review of the literature. Int Urogynecol J Pelvic Floor Dysfunct 17: 646-649.
-
Dougherty LS, Hull T (2000) Perineal endometriosis with anal sphincter involvement: report of a case. Dis Colon Rectum 43: 1157-1160.
-
Kanellos I, Kelpis T, Zaraboukas T, Betsis D (2001) Perineal endometriosis in episiotomy scar with anal sphincter involvement. Tech Coloproctol 5: 107-108.
-
Luterek K, Barcz E, Bablok L, Wierzbicki Z (2013) Giant recurrent perineal endometriosis in an episiotomy scar--a case report. Ginekol Pol 84: 726-729.
-
Fedele L, Bianchi S, Zanconato G, Tozzi L, Raffaelli R (2000) Gonadotropin-releasing hormone agonist treatment for endometriosis of the rectovaginal septum. Am J Obstet Gynecol 183: 1462-1467.
-
Angioni S, Pontis A, Dessole M, Surico D, De Cicco Nardone C, et al. (2015) Pain control and quality of life after laparoscopic en-block resection of deep infiltrating endometriosis (DIE) vs. incomplete surgical treatment with or without GnRHa administration after surgery. Arch Gynecol Obstet 291: 363-370.
-
Dunselman GA, Vermeulen N, Becker C, Calhaz-Jorge C, D'Hooghe T, et al. (2014) ESHRE guideline: management of women with endometriosis. Hum Reprod 29: 400-412.
-
Roman H (2007) Guidelines for the management of painful endometriosis. J Gynecol Obstet Biol Reprod (Paris) 36: 141-150.
-
Bedaiwy MA, Casper RF (2006) Treatment with leuprolide acetate and hormonal add-back for up to 10 years in stage IV endometriosis patients with chronic pelvic pain. Fertil Steril 86: 220-222.





