Journal of Rheumatic Diseases and Treatment
Scleroderma Renal Crisis
Gioacchino Li Cavoli*, Luisa Bono, Calogera Tortorici, Carlo Giammarresi, Tancredi Vincenzo Li Cavoli and Ugo Rotolo
Nephrology-Dialysis, Civico-Benfratelli and Di Cristina Hospital, Italy
*Corresponding author: Dr. Gioacchino Li Cavoli, Nephrology-Dialysis, Civico-Benfratelli and Di Cristina Hospital, 43 via Francesco Cilea, 90144 Palermo, Italy, Tel: 393-3323-18100, Fax: 3909-166-63454, E-mail: gioacchinolicavoli@libero.it
J Rheum Dis Treat, JRDT-3-046, (Volume 3, Issue 1), Case Report; ISSN: 2469-5726
Received: November 22, 2016 | Accepted: February 11, 2017 | Published: February 14, 2017
Citation: Cavoli GL, Bono L, Tortorici C, Giammarresi C, Cavoli TVL, et al. (2017) Scleroderma Renal Crisis. J Rheum Dis Treat 3:046. 10.23937/2469-5726/1510046
Copyright: © 2017 Cavoli GL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Scleroderma or Systemic sclerosis is a vascular and fibrotic disease with organ-based complications and high mortality and morbidity. Renal involvement can be quite varied and scleroderma renal crisis is the most severe manifestation. We report our experience. In February 2016 a 52-year-old male was admitted to hospital with pulmonary oedema and severe arterial hypertension (240/120 mmHg). From 2015 he was suffering from Scleroderma and renal failure due to biopsy proven thrombotic microangiopaty. We treated the scleroderma renal crisis with haemodialysis, plasma exchange, nitroglycerin I.V., ramipril, irbesartan and amlodipine p.o. with significant improvement. Then the patient started Extracorporeal Photopheresis, scheduled as 2 treatments every month for 6 months. After 2 months he was able to stop haemodialysis (creatinine 5 mg/dl, Glomerular filtration rate 16 ml/min). The patient completed the scheduled Extracorporeal Photopheresis cycle. After 10 months the creatinine was 4.6 mg/dl and cardiovascular and respiratory functions were stable. Scleroderma renal crisis is a life-threatening complication of Systemic Sclerosis. With the advent of ACE- inhibitors, mortality associated with SRC decreased from 76% to < 10% but up to now there is no cure for SSc. In our experience, after pharmacological therapy and haemodialysis, we performed a cycle of ECP. Further studies are needed to confirm this treatment option.
Keywords
AKI, Hypertension, Thrombotic microangiopaty, Haemodialysis, Chronic renal failure
Introduction
Scleroderma or Systemic Sclerosis (SSc) is a vascular and fibrotic disease with worldwide distribution and a female/male ratio 3-4:1. Its etiology is unknown and the pathogenesis is characterized by uncontrolled over production of connective tissue and vascular thickening and narrowing. Scleroderma is a systemic disease and leads to organ-based complications with high mortality and morbidity. Early diagnosis is important as early treatment could potentially lead to better outcomes. Scleroderma renal crisis (SRC) is the most severe complication of SSc Prior the advent of ACE-inibithors, short-term survival in SRC was < 10%. Studies have shown that CD4+ T cell activation is a key factor in the pathogenesis. Extracorporeal photopheresis (ECP), is a well-established leukapheresis-based therapy for the treatment of cutaneous T-cell lymphoma. ECP is one of the promising therapeutic strategies in other severe and difficult-to-treat conditions, (graft-versus-host disease after allogeneic stem cell transplantation, prevention and treatment of rejection in solid organ transplantation, Crohn’s disease, SSc). We report our experience on SRC treated with medical therapy and ECP [1].
Case Presentation
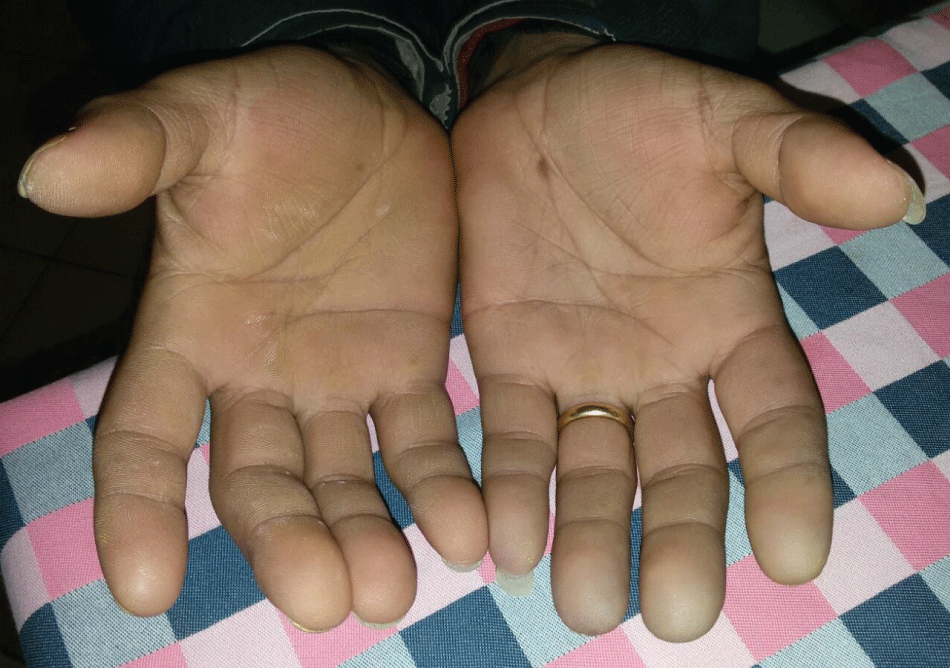
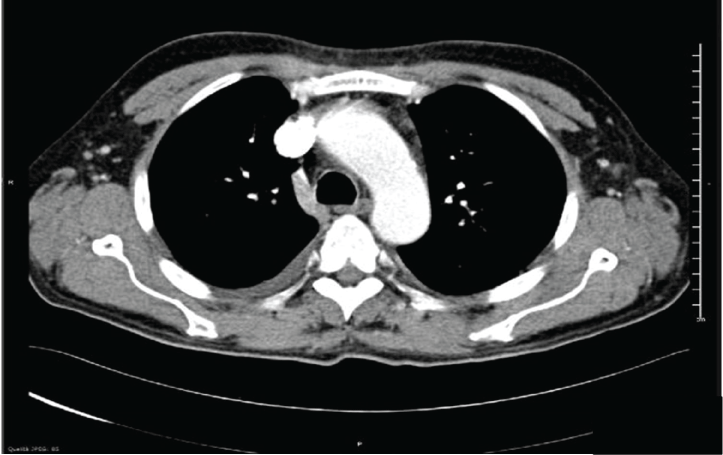
In January 2015 a 52-year-old male was admitted to hospital with dispnoea ed arterial hypertension. Clinical examination highlighted: diffuse cutaneous sclerosis, Raynaud phenomenon (Figure 1) and esophageal dysmotility. Laboratory investigations showed: Creatinine 3.5 mg/dl, Urea 110 mg/dl, Hb: 10.5 gr/dl. A renal biopsy was performed. At light microscopy, among 18 glomeruli, ten showed ischemic collapse with mesangiolysis, glomerular basement membrane reduplication, thickening of interlobular arteries and luminal narrowing due to thrombotic material; slight tubular atrophy and interstitial fibrosis. At immunofluorescence microscopy, focal staining for fibrinogen was seen in arteriolar walls. These findings were attractive for thrombotic microangiopaty. The patient started therapy with hypotensive and steroid drugs. In February 2016 the patient was admitted to hospital with pulmonary oedema and severe arterial hypertension (240/120 mmHg). Due to reduced renal function, the therapy with ACE-Inibitorors was interrupted . At the admission, laboratory investigations demonstrated severe renal failure (Creatinine 8.9 mg/dl ) and schistoytes in the peripheral blood film. ANA title resulted 1:320; tests for anti-Scl70, anti-RNA-polymerase III and other immunological autoantibodies were negative. Lung CT scan showed pleuro-pericardic effusion and ground-glass opacifications with reticular pattern (Figure 2). Because of echocardiography demostrated a thoracic aortic dilation, the patient underwent to CT Angiography with evidence of aortic arch dilation (diameter 43 mm) without signs of aortic dissection. (Figure 3) Pulmonary assessement showed a slight restrictive ventilatory defect. We performed a prompt aggressive intervention with haemodialysis, plasma exchange and therapy with nitroglycerin I.V. and ramipril, irbesartan and amlodipine p.o. with significant improvement and early good blood pressure control. Later the patient started Extracorporeal Photopheresis (ECP) therapy, scheduled as 2 treatments every month for 6 months. Because of persistent renal function deterioration, the patient continued haemodialysis but after 2 months he was able to stop haemodialysis (creatinine 5mg/dl, Glomerular filtration rate 16 ml/min). The Patient completed the scheduled Extracorporeal Photopheresis cycle. After 11 months the Creatinine was 4.6 mg/dl and cardiovascular and respiratory functions were stable.
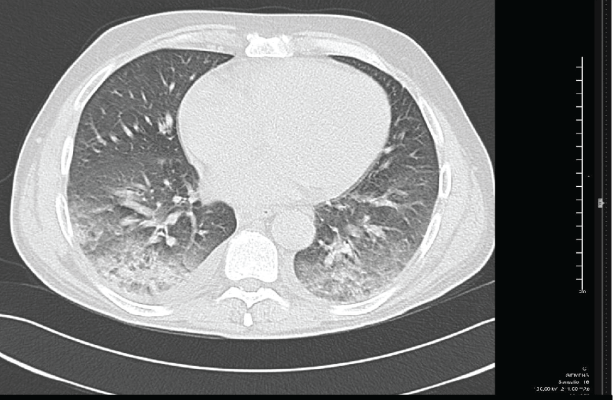
.
Figure 2: CT scan of the lungs: pleural and pericardic effusion and ground-glass opacifications with reticular pattern.
View Figure 2
Discussion
Scleroderma is a rare multisystem immune disease affecting 1-2 patients per 100000 in the United States with striking female predominance and unknown pathogenesis involving both genetic and environmental factors. The course is chronic and often progressive. The pathophysiology is based on 3 cardinal features: small vessel vasculopathy, production of autoantibodies, and fibroblast dysfunction leading to progressive visceral and vascular fibrosis in multiple organs [2]. The heterogeneous clinical manifestations (inflammation and fibrosis of the skin, vascular abnormalities, organ damage and autoantibody production) vary from increased connective tissue in localized areas of skin (morphea) to diffuse and generalized disease (SSc) [3]. A characteristic pattern of blood vessel abnormalities is seen in the nail beds and nailfold videocapillaroscopy can easily identify SSc microvascular hallmarks as giant capillaries and avascular areas, but also less specific and frequent changes as ectasia, microhemorrhages, bushy capillaries, and reduced capillary density [4]. On the basis of the extent of skin involvement there are 2 subsets: limited cutaneous SSc and diffuse cutaneous SSc. Howewer, several distinct phenotypes exists within each subset as well as the overlap between SSc and other autoimmune diseases such as polymyositis, Sjogren syndrome, polyarthritis, autoimmune liver disease and SLE. Virtually every organs can be affected in SSc. The severity of visceral organs involvement, including the gastrointestinal tract, lungs, heart, and kidneys.determines survival as it affects critical organs. Limited forms of the disease (CREST syndrome: calcinosis, Raynaud’s phenomenon, esophageal dysmotility, sclerodactily,teleangectasia) also occur but are seldom associated with renal disease. Rarely, the visceral abnormality may occur in the abscence of cutaneous lesions (scleroderma sine scleroderma). Antinuclear antibodies, mainly against topoisomerase 1 (Scl 70) are present in more than 95% of patients [5]. Renal involvement can be quite varied, from a low-grade proteinuria and slight impairment of glomerular filtration rate to a more marked reduction in renal blood flow and acute kidney injury. SRC is a life-threatening complication of SSc, characterized by iuxtaglomerular hyperplasia; progressive reduction in renal blood flow, aggravated by vasospasm, leads to severe hyperreninemic hypertension that culminates in malignant hypertension. High mortality is reported with a 5-year survival rate of 65%. The reported frequency of SRC in SSc is 10-20% [6,7]. SRC is more common in patients receiving corticosteroids, the risk increasing with increasing dose. The disease is sometimes triggered by use of nephrotoxic drugs and/or intravascular volume depletion. Other risk factors for SRC include African American race, male gender, diffuse cutaneous SSc. Thrombotic microangiopathy is detected in 43% of cases, and anti-RNA-polymerase III antibodies are present in one-third of patients [8]. The histopathologic hallmar k of SRC is a proliferative obliterative vasculopathy with concentric “onion skin” narrowing of arterioles and glomerular ischemia. Transplantation may be a reasonable treatment option, but progression of disease in other visceral organs may limit life expectancy. With the advent of ACE inhibitors, mortality associated with SRC decreased from 76% to < 10% but up to now there is no cure for SSc. No medications appear to be truly effective in patients with aggressive disease and long-term prognosis remains disappointing [9]. According 2013 American Society for Apheresis guidelines pathophysiology of SSc lends little support to the use of Therapeutic Plasma Exchange [10]. In the experience of Cozzi (2012) Plasma exchange in addition to ACE-inhibitors could be a therapeutic option in patients with SRC who develop microangiopathy or are intolerant to high doses of ACE inhibitors [11]. Recommendations from European League Against Rheumatism (EULAR) confirm ACE inhibitors as first-line therapy for SRC but the prevention of SRC lacks consensus [12]. Recent advances in the understanding of scleroderma's pathogenesis leads to interest in the role of activated T cells, resulting in inflammation, microvascular damage and fibrosis. Extracorporeal Photopheresis (ECP) is an extracorporeal form of immunotherapy, FDA approved for the treatment of cutaneous T-cell lymphoma [13]. Some reports indicate that photopheresis is a promising treatment in the therapy of solid organ transplant rejection [14], graft versus host disease [15], scleroderma and other autoimmune diseases resistant to conventional therapy [16]. In 2000 Muellegger RR and coll. reported an overall improvement and/or stabilization of skin changes and physical performance in 5 of 11 patients (45%) suffering from systemic sclerosis treated with extended Extracorporeal Photochemotherapy [17]. In 2012 among 16 patients with diffuse cutaneous SSc, Papp G and coll. reported reduction of dermal thickness and improvement of joints mobility after ECP [18]. In 2016 the immunomodulatory effects of ECP treatments were confirmed by the same Authors in nine patients with diffuse cutaneous SSc treated with 24 ECP treatments per patient in total [18]. During photopheresis lymphocytes are collected from the patients by leukapheresis and after exposure to 8-methoxypsoralen (8-MOP) and UVA radiation, reinfused into the patient circulation. ECP can promote the apoptotic death of pathogenic T-cells and the induction of cell-mediated anticlonotypic immune response against pathogenic clones of T lymphocytes [19]. ECP downregulates the immune response and induces tolerance by regulatory T cells. The advantage of photopheresis treatment is the low frequency of side effects related to treatment. The disadvantages are the practical efforts required and the high treatment cost [20,21]. Confirmation of ECP treatment outcome in additional SSc patient will certainly increase the clinical value of our experience.
Conclusion
SSc is a chronic multisystem disorder and SRC is the most dreaded complication. Up to now, the prognosis of SRC has remarkably improved but SRC still remains an important cause of morbidity and mortality. After the introduction of ACE-inhibitors to treat SRC, no new therapeutic approaches showed efficacy. In our experience, after pharmacological therapy and haemodialysis, we performed a cycle of ECP. Further studies are needed to confirm this treatment option.
Conflict of Interest
The Authors have declared that no conflict of interest exists.
References
-
Knobler R, Berlin G, Calzavara-Pinton P, Greinix H, Jaksch P, et al. (2014) Guidelines on the use of extracorporeal photopheresis. J Eur Acad Dermatol Venereol 28: 1-37.
-
Wollheim FA (2005) Classification of systemic sclerosis. Visions and reality. Rheumatology (Oxford) 44: 1212-1216.
-
van den Hoogen F, Khanna D, Fransen J, Johnson SR, Baron M, et al. (2013) 2013 Classification criteria for systemic sclerosis: an American College of Rheumatology/European League against Rheumatism collaborative initiative. Arthritis Rheum 65: 2737-2747.
-
De Santis M, Ceribelli A, Cavaciocchi F, Crotti C, Massarotti M, et al. (2016) Nailfold videocapillaroscopy and serum VEGF levels in scleroderma are associated with internal organ involvement. Auto Immun Highlights 7: 5.
-
Bussone G, Berezne A, Pestre V, Guillevin L, Mouthon L (2011) The scleroderma kidney: progress in risk factors, therapy, and prevention. Curr Rheumatol Rep 13: 37-43.
-
DeMarco PJ, Weisman MH, Seibold JR, Furst DE, Wong WK, et al. (2002) Predictors and outcomes of scleroderma renal crisis: the high-dose versus low-dose D-penicillamine in early diffuse systemic sclerosis trial. Arthritis Rheum 46: 2983-2989.
-
Bose N, Chiesa-Vottero A, Chatterjee S (2015) Scleroderma renal crisis. Semin Arthritis Rheum 44: 687-694.
-
Mouthon L, Bussone G, Berezné A, Noël LH, Guillevin L (2014) Scleroderma renal crisis. J Rheumatol 41: 1040-1048.
-
Guillevin L, Bérezné A, Seror R, Teixeira L, Pourrat J, et al. (2012) Scleroderma renal crisis: a retrospective multicentre study on 91 patients and 427 controls. Rheumatology 51: 460-467.
-
Schwartz J, Winters JL, Padmanabhan A, Balogun RA, Delaney M, et al. (2013) Guidelines on the use of therapeutic apheresis in clinical practice-evidence- based approach from the Writing Committee of the American Society for Apheresis: the sixth special issue. J Clin Apher 28: 145-284.
-
Cozzi F, Marson P, Cardarelli S, Favaro M, Tison T, et al. (2012) Prognosis of scleroderma renal crisis: a long-term observational study. Nephrol Dial Transplant 27: 4398-4403.
-
Shanmugam VK, Steen VD (2012) Renal disease in scleroderma: an update on evaluation, risk stratification, pathogenesis and management. Curr Opin Rheumatol 24: 669-676.
-
Shiue LH, Couturier J, Lewis DE, Wei C, Ni X, et al. (2015) The effect of extracorporeal photopheresis alone or in combination therapy on circulating CD4(+) Foxp3(+) CD25(-) T cells in patients with leukemic cutaneous T-cell lymphoma. Photodermatol Photoimmunol Photomed 31: 184-194.
-
Jaksch P, Knobler R (2014) ECP and solid organ transplantation. Transfus Apher Sci 50: 358-362.
-
Lorenz K, Rommel K, Mani J, Jin N, Hilgendorf I, et al. (2015) Modulation of lymphocyte subpopulations by extracorporeal photopheresis in patients with acute graft-versus-host disease or graft rejection. Leuk Lymphoma 56: 671-675.
-
Adamski J, Kinard T, Ipe T, Cooling L (2015) Extracorporeal photopheresis for the treatment of autoimmune diseases. Transfus Apher Sci 52: 171-182.
-
Muellegger RR, Hofer A, Salmhofer W, Soyer HP, Kerl H, et al. (2000) Extended extracorporeal photochemotherapy with extracorporeal administration of 8-methoxypsoralen in systemic sclerosis. An Austrian single-center study. Photodermatol Photoimmunol Photomed 16: 216-223.
-
Papp G, Horvath IF, Barath S, Gyimesi E, Vegh J, et al. (2012) Immunomodulatory effects of extracorporeal photochemotherapy in systemic sclerosis. Clin Immunol 142: 150-159.
-
Papp G, Horvath IF, Gyimesi E, Barath S, Vegh J, et al. (2016) The assessment of immune-regulatory effects of extracorporeal photopheresis in systemic sclerosis: a long-term follow-up study. Immunol Res 64: 404-411.
-
Vagace Vaero JM, Alonso Escobar N, De Argila Fernández-Durán D, Vargas Pérez L, Melero Ruiz J, et al. (2003) Photopheresis: new immunomodulatory therapy for T-lymphocite mediated diseases. An Med Interna 20: 421-426.
-
Maeda A (2009) Extracorporeal photochemotherapy. J Dermatol Sci 54: 150-156.