Journal of Rheumatic Diseases and Treatment
Chronic Large Joint Synovitis in Systemic Lupus Erythematosus: Finding What You Look For
B Hodkinson1*, I Okpechi2 and SA Botha-Scheepers1
1Department of Medicine, Division of Rheumatology, University of Cape Town and Groote Schuur Hospital, Cape Town, South Africa
2Division of Nephrology and Hypertension, University of Cape Town, South Africa
*Corresponding author: Dr. Bridget Hodkinson, Department of Medicine, Division of Rheumatology, University of Cape Town and Groote Schuur Hospital, J47 Old Main Building, Groote Schuur Hospital, Observatory 7925, Cape Town, South Africa, Tel: +27 (0)21 404 2131, Fax: +27 (0)21 448 3253, E-mail: drbridget@gmail.com
J Rheum Dis Treat, JRDT-2-037, (Volume 2, Issue 3), Case Report; ISSN: 2469-5726
Received: May 10, 2016 | Accepted: June 01, 2016 | Published: July 03, 2016
Citation: Hodkinson B, Okpechi I, Botha-Scheepers SA (2016) Chronic Large Joint Synovitis in Systemic Lupus Erythematosus: Finding What You Look For. J Rheum Dis Treat 2:037. 10.23937/2469-5726/1510037
Copyright: © 2016 Hodkinson B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Systemic lupus erythematosus, Synovitis, Musculoskeletal TB, Osteonecrosis
Case Report
Systemic Lupus Erythematosus (SLE) patients commonly have musculoskeletal complaints. We describe two SLE patients with persistent knee pain and swelling that were initially mistaken for inflammatory arthritis.
Case 1
A 30-year-Black African female was diagnosed with SLE when she presented with a Coombs positive haemolytic anaemia, lymphopenia, polyarthritis, oral ulcers and a malar rash. Her antinuclear antigen (ANA) was positive, she had hypocomplementaemia and she was HIV negative. She was commenced on oral corticosteroids (initially high dose 60 mg/day and later weaned to 15 mg daily), chloroquine sulphate and azathioprine. Her blood counts and SLE symptoms improved. Four months after diagnosis, she developed a right knee monoarthritis. Despite intra-articular steroid injections, nonsteroidal anti-inflammatories, her knee symptoms persisted. Plain X-rays of the knees and chest were unremarkable, but she had an elevated C-reactive protein (14 mg/l) and very high ESR (88 mm/h). Over the next four months, three joint aspirations were Gram and Ziehl-Neelsen stain and culture negative. A synovial biopsy submitted for histology revealed necrotising granulomatous inflammation. The positive Ziehl-Neelson stain for acid-fast bacilli confirmed the diagnosis of osteoarticular Mycobacterium tuberculosis infection (Figure 1). She had no history of previous tuberculosis (TB), and there was no evidence of extra-pulmonary disease elsewhere. Her knee swelling and symptoms resolved within 3 months of commencing anti-TB treatment, and this therapy was continued for 18 months.
.
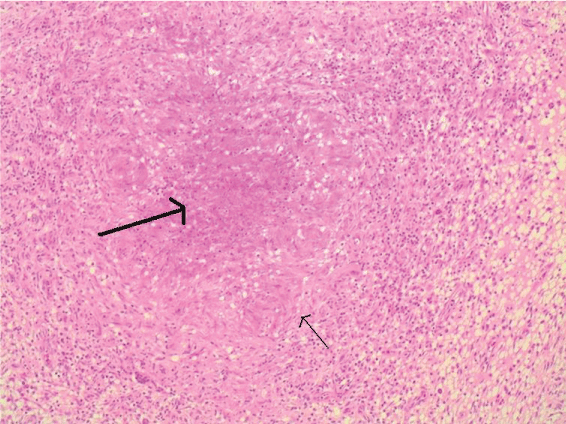
Figure 1: Haematoxylin and Eosin stain of Case 1 synovial biopsy showing a caseating granuloma with central necrosis (large arrow) surrounded by palisading epithelioid macrophages (small arrow). Ziehl Neelsen stain revealed acid-fast bacilli.
View Figure 1
Case 2
A 30-year-old female of mixed racial ancestry was diagnosed with SLE, with class IV nephritis with crescents, arthritis and discoid skin lesions. She was ANA and dsDNA positive, HIV negative, and had no antiphospholipid antibodies. She was treated with intravenous solumedrol 500 mg daily for 3 days followed by oral corticosteroids at 60 mg daily which were tapered to 15 mg daily over 4 months, chloroquine sulphate and mycophenolate mofetil. Within 4 months, her SLE was inactive but she complained of a painful right knee. On examination, she had bilateral knee effusions, but no synovitis of any other joint. The knee was aspirated on two occasions, and the serous fluid was shown to be a Type 2 inflammatory fluid (slightly turbid with a white cell count 2000-10000, 20-70% neutrophils), with negative bacterial and fungal cultures. Intra-articular steroids were unhelpful, and symptoms and swelling continued for the next four months. Plain radiographs showed a fragmented medial epicondyle of the right knee (Figure 1) and MRI of the right knee demonstrated a joint effusion, large bony infarcts with surrounding oedema in the medial and lateral femoral condyles, proximal tibia and patella in keeping with osteonecrosis (Figure 2). The left knee had a small infarct of the proximal tibia.
.
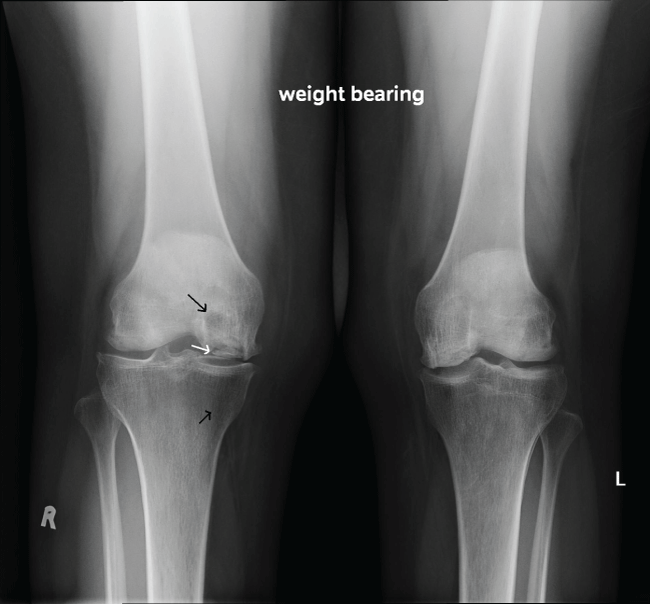
Figure 2: Weight bearing radiograph of both knees (Case 2) with fragmented right medial epicondyle (white arrow) and radiolucencies in the distal tibia and proximal femur (black arrows).
View Figure 2
.
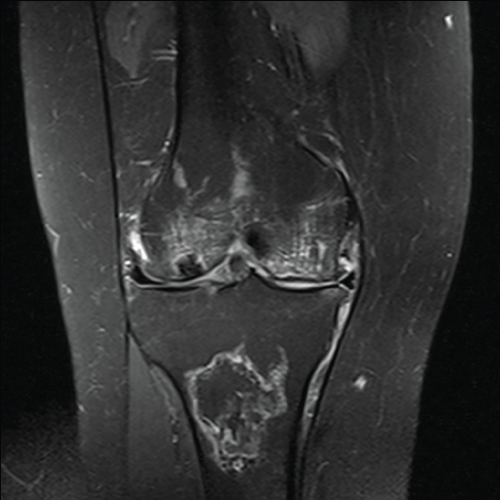
Figure 3: Noncontrast magnetic resonance image (MRI) of the right knee featuring an effusion, and large bony infarcts in the medial and lateral femoral condyles as well as the tibial metaphysis with surrounding oedema. The left knee MRI showed smaller femoral condyle infarcts.
View Figure 3
In an attempt to avoid arthroplasty, intravenous zolendronic acid was administered, with dramatic clinical improvement. Within one month the swelling and pain had resolved. Unfortunately, follow-up MRI eight months later showed minimal improvement, and symptoms recurred, necessitating a right total knee arthroplasty.
Discussion
Arthritis is a common symptom in SLE, and carries a differential diagnosis (Table 1). Inflammatory polyarthritis as part of SLE affects 70-95% of patients, is frequently present at the time of diagnosis, and is a common component of lupus flares [1]. All joints can be affected, with the hand and knees being the most common. Advances in imaging have shown that clinical examination underestimates joint inflammation in SLE patients, perhaps explaining the high frequency of arthralgia and pain amongst these patients. A recent ultrasound study of SLE patients demonstrated knee synovitis in 40%, effusion in 23 and synovial proliferation in 23% [2]. MRI studies of SLE patients with polyarthralgia show synovitis, tenosynovitis and bony oedema with erosions, similar to changes seen in rheumatoid arthritis patients [3].
![]()
Table 1: Differential diagnosis of arthritis in SLE patient.
View Table 1
Septic arthritis should be a consideration in any SLE patient with an acute or subacute large joint swelling, particularly if associated with high inflammatory markers. A retrospective study of 29 SLE patients with septic arthritis showed the hip (59%) was the most commonly affected joint, followed by the knee (34%) and ankle (21%) [4]. The majority of infections were due to Salmonella (59%) or other gram negative bacteria (11%), Staphylococcus aureus (24%), or by Streptococcus pneumonia (4%). Oligoarthritis occurred in almost half the patients. Major risk factors for septic arthritis are corticosteroid use, immunosuppressive therapy, severe active SLE, and osteonecrosis.
The differential diagnosis of a chronic monoarthritis includes osteo-articular TB infection, particularly in TB endemic countries. Large weight bearing joints such as the hip and knee and the spine are the commonest sites [5]. Patients with SLE may be at particular risk of this form of extra-pulmonary disease [6]. Diagnosis can be challenging and depends on synovial fluid culture or GeneXpert PCR test, or synovial biopsy [7]. Risk factors for extra-pulmonary TB amongst SLE patients include high dose corticosteroids, other immunosuppressive therapies, lymphopenia, nephritis and inflammatory arthritis [8,9].
Osteonecrosis (ON) is a common complication of SLE, affecting 2-30% of patients [10]. Although the hip is the most common site, knee ON is well described. In a series of knee ON patients, Navaez describes gradual or sudden onset of pain, with tenderness and the presence of an effusion in 81% of patients [11]. Multiple sites of ON are frequently seen. In a series of 136 patients with knee ON, 74% had ON of at least one other large joint, commonly the other knee (82%) or hip (67%) [12]. The aetiology of ON in SLE patients is multifactorial, and predisposing factors include glucocorticoid therapy, vasculitis, Raynaud's phenomenon, antiphospholipid antibodies and high disease activity [13,14]. Early disease may respond to core decompression surgery or to bisphosphonate therapy although large randomised control studies are lacking [15,16]. Advanced cases, such as our patient, where the knee joint is destroyed require arthroplasty.
In both the cases described, there was considerable diagnostic delay despite follow-up at a specialist centre. The expense and invasiveness of synovial biopsy and histology or MRI studies to make either diagnosis frequently underlie this delay. However, awareness of the differential diagnosis and appropriate investigation of a persistent large joint swelling is critical to make a timeous diagnosis in order to prevent joint destruction. In addition, these two cases also highlight the devastating side effects of prolonged high-dose corticosteroids. This risk of corticosteroid-induced damage is increasingly recognized in SLE patients and best practice is to use moderate doses for the shortest possible time [17].
In summary, a painful, swollen joint in a SLE patient should prompt consideration of a cause other than inflammatory arthritis. In particular, persistent pain and swelling, and involvement of a large joint, are important clues to a "non-SLE arthritis" and should prompt investigations for other causes, in particular septic arthritis and osteonecrosis. Remember, "You only find what you look for, and you only look for what you know".
Ethical Statement
Written informed consent was obtained from the patients for publication of this case report and accompanying images.
References
-
Grossman JM (2009) Lupus arthritis. Best Pract Res Clin Rheumatol 23: 495-506.
-
Ossandon A, Iagnocco A, Alessandri C, Priori R, Conti F, et al. (2009) Ultrasonographic depiction of knee joint alterations in systemic lupus erythematosus. Clin Exp Rheumatol 27: 329-332.
-
Boutry N, Hachulla E, Flipo RM, Cortet B, Cotten A (2005) MR imaging findings in hands in early rheumatoid arthritis: comparison with those in systemic lupus erythematosus and primary Sjögren syndrome. Radiology 236: 593-600.
-
Huang JL, Hung JJ, Wu KC, Lee WI, Chan CK, et al. (2006) Septic arthritis in patients with systemic lupus erythematosus: salmonella and nonsalmonella infections compared. Semin Arthritis Rheum 36: 61-67.
-
Pigrau-Serrallach C, Rodríguez-Pardo D (2013) Bone and joint tuberculosis. Eur Spine J 22 Suppl 4: 556-566.
-
Hodkinson B, Musenge E, Tikly M (2009) Osteoarticular tuberculosis in patients with systemic lupus erythematosus. QJM 102: 321-328.
-
Pandey V, Chawla K, Acharya K, Rao S, Rao S (2009) The role of polymerase chain reaction in the management of osteoarticular tuberculosis. Int Orthop 33: 801-805.
-
Sayarlioglu M, Inanc M, Kamali S, Cefle A, Karaman O, et al. (2004) Tuberculosis in Turkish patients with systemic lupus erythematosus: increased frequency of extrapulmonary localization. Lupus 13: 274-278.
-
Tam LS, Li EK, Wong SM, Szeto CC (2002) Risk factors and clinical features for tuberculosis among patients with systemic lupus erythematosus in Hong Kong. Scand J Rheumatol 31: 296-300.
-
Gontero RP, Bedoya ME, Benavente E, Roverano SG, Paira SO2 (2015) Osteonecrosis in systemic lupus erythematosus. Reumatol Clin 11: 151-155.
-
Narváez J, Narváez JA, Rodriguez-Moreno J, Roig-Escofet D (2000) Osteonecrosis of the knee: differences among idiopathic and secondary types. Rheumatology (Oxford) 39: 982-989.
-
Mont MA, Baumgarten KM, Rifai A, Bluemke DA, Jones LC, et al. (2000) Atraumatic osteonecrosis of the knee. J Bone Joint Surg Am 82: 1279-1290.
-
Sayarlioglu M, Yuzbasioglu N, Inanc M, Kamali S, Cefle A, et al. (2012) Risk factors for avascular bone necrosis in patients with systemic lupus erythematosus. Rheumatol Int 32: 177-182.
-
Fialho SC, Bonfá E, Vitule LF, D'Amico E, Caparbo V, et al. (2007) Disease activity as a major risk factor for osteonecrosis in early systemic lupus erythematosus. Lupus 16: 239-244.
-
Hong YC, Luo RB, Lin T, Zhong HM, Shi JB (2014) Efficacy of alendronate for preventing collapse of femoral head in adult patients with nontraumatic osteonecrosis. Biomed Res Int 2014: 716538.
-
Kalla AA, Learmonth ID, Klemp P (1986) Early treatment of avascular necrosis in systemic lupus erythematosus. Ann Rheum Dis 45: 649-652.
-
Thamer M, Hernán MA, Zhang Y, Cotter D, Petri M (2009) Prednisone, lupus activity, and permanent organ damage. J Rheumatol 36: 560-564.





