Journal of Otolaryngology and Rhinology
Synchronous Laryngeal Tuberculosis and Cancer, a First in Literature
Thilaga Rajendran*, Velayutham Kamaru Ambu and Azila Alias
Department of Otorhinolaryngology, Hospital TuankuJa'afar Seremban, Malaysia
*Corresponding author:
Thilaga Rajendran, Department of Otorhinolaryngology, Hospital TuankuJa'afar Seremban, Negeri Sembilan, Malaysia, E-mail: thilaga1510@yahoo.com
J Otolaryngol Rhinol, JOR-3-030, (Volume 3, Issue 1), Case Report; ISSN: 2572-4193
Received: June 13, 2016 | Accepted: March 28, 2017 | Published: March 30, 2017
Citation: Rajendran T, Ambu VK, Alias A (2017) Synchronous Laryngeal Tuberculosis and Cancer, a First in Literature. J Otolaryngol Rhinol 3:030.
Copyright: © 2017 Rajendran T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Summary
Laryngeal cancer is rising in incidence among elderly men with history of smoking. Laryngeal tuberculosis is a rare clinical entity and the incidence is significantly less than 1% of all tuberculosis. This case report highlights the co-existence of laryngeal cancer and TB in a 75-year-old man who presented to us with a 4-year history of hoarseness. Flexible laryngoscopy revealed a mass at right false cord extending to left false cord. First biopsy showed severe dysplasia and was suggested for deeper biopsy. A second biopsy taken after a delay confirmed moderately-differentiated squamous cell carcinoma with evidence of laryngeal tuberculosis. The tumour was already more extensive from initial staging of T2N1M0 to a T4N1M0 transglottic tumour. Patient was given options of initiation of anti-tubercular drugs and radiotherapy, or a plan for total laryngectomy after stabilizing on anti-tubercular drugs. However, patient was undecided, which has led to the tumour being more extensive. Patient was started on anti-tubercular drugs for approximately 6 months and subsequently deteriorated. Patient was not fit for any chemo or radiotherapy. Based on this case report, it is shown that TB and malignancy can occur synchronously at the same anatomical location and the importance of early diagnosis and treatment need to be highlighted.
Background
To highlight the incidence of synchronous pathologies that mimic each other, this appears to be the first in literature. Laryngeal tuberculosis (TB) is a rare clinical entity and incidence of the illness is significantly less than 1% of all tuberculosis cases. Worldwide, 9.6 million people are estimated to have fallen ill with TB in 2014, comprising of 5.4 million men, 3.2 million women and 1.0 million children. Of the 9.6 million new TB cases, 58% were in the South-East Asia and Western Pacific regions [1]. In Malaysia, incidence of tuberculosis per 100,000 people is steadily increasing from 87 in 2011 to 103 in 2014, which includes all forms of TB [2]. It is fast rising as a non-communicable disease in the country. The influx of foreigners has been attributed to the rise. Moreover, many foreigners hail from higher TB burden countries like Indonesia, Myanmar, Cambodia, Vietnam and the Philippines. There is also a higher risk of getting TB among those with co-morbid or immunodeficiency conditions, like diabetes mellitus, chronic obstructive lung disease, HIV (human immunodeficiency virus) and the elderly and smokers [3]. The Malaysian Health Ministry recorded 16,918 TB cases with 1,504 deaths in 2007. In 2012, the total number of TB cases increased to 22,710 with 1,520 deaths. There has been a steady increase of TB cases from 2007 to 2012 with the notification rate of 72 cases per 100,000 people in 2012. The mortality rate due to this disease is between 5.3 to 5.8 deaths for every 100,000 people [4]. The clinical manifestations of tuberculosis nowadays are very general with more multiorgan involvement as this case study has proven to be. However, the incidence of synchronous laryngeal cancer with TB is rare one as a result of improvement in public health care and development of effective antitubercular chemotherapy.
On the other hand, laryngeal cancer is rising in incidence especially amongst elderly men who have strong history of smoking. A clear association has been made between smoking, excess alcohol ingestion, and the development of squamous cell cancers of the upper aerodigestive tract. For smokers, the risk of the development of laryngeal cancer decreases after the cessation of smoking but remains elevated even years later when compared to that of non-smokers. Globally, the incidence of laryngeal carcinoma is relatively low in comparison to that of carcinomas of all organs. Laryngeal cancer comprises 2% to 5% of all malignant diseases diagnosed annually worldwide [5]. According to Malaysian National Cancer Registry, a total number of 103,507 new cancer cases were diagnosed in Malaysia during the period of 2007 till 2011. Laryngeal cancer recorded a number of 938 cases, which comprises about 0.9% [6].
Case Presentation
A 75-year-old patient, who was first seen in our ORL clinic in August 2015, presented with 4-year history of hoarseness, associated with worsening dysphagia, noisy breathing and constitutional symptoms. Patient admitted smoking 1 to 2 packs of cigarettes daily for more than 30 years. There was no prior history of tubercular infection in the patient and there were no close TB contacts. On examination, there was an audible stridor and a small palpable lymph node measuring approximately 1.5 cm at level IV on the left side.
Investigations
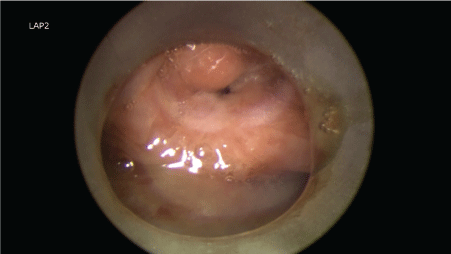
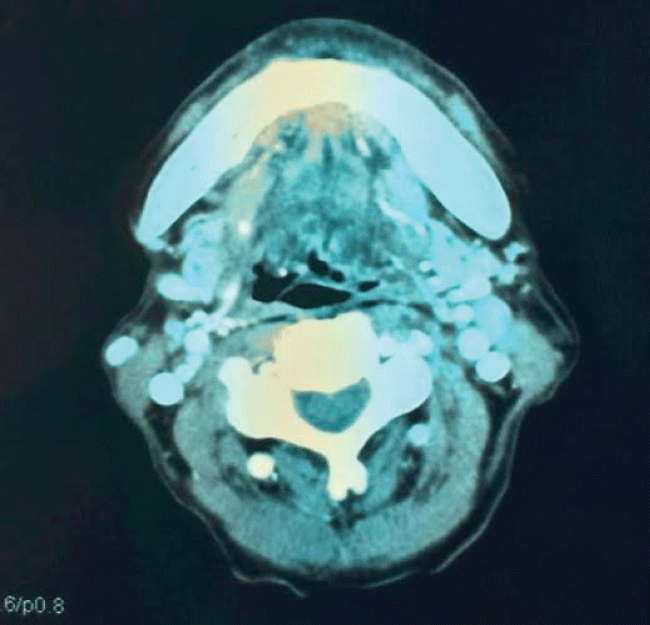
Flexible laryngoscopy revealed a mass at right false cord extending to left false cord. Both vocal cords were not clearly visualized. Initially tumour was staged as T2N1MO, with suspicion of reactive lymph node. Airway was only about 25%, almost closing on inspiration; hence, tracheostomy was performed and preceded with direct laryngoscopy. A friable mass was seen over left false cord, extending into anterior commissure and right vocal cord at its anterior one third. The mass also seen extending anteriorly into the subglottic area 1.5 cm below the vocal cords (Figure 1). Esophagocopy was normal. First biopsy taken in August 2015 showed severe dysplasia with area suspicious of invasion. It was suggested by the pathologist for deeper biopsy. Subsequently, CT imaging showed findings of a laryngeal tumour, involving both false and true cords, with transglottic extension, and invasion into pre-epiglottic and both paraglottic spaces. But no distant metastasis has been reported (Figure 2). Based on the CT findings, the tumour was staged as T4N1M0. A second biopsy done in October 2015 showed more extensive mass involving both true cords and false cords. The mass also involved both the anterior and posterior commisures. The delay in second biopsy was because patient went to a different hospital for second opinion. The second biopsy confirmed moderately-differentiated squamous cell carcinoma. The tumour was already more extensive from initial staging of T2N1M0 to a T4N1M0 transglottic tumour. Meanwhile tissue sent for AFB culture and smear also confirmed laryngeal tuberculosis.
.
Figure 2: CT neck-laryngeal tumour (involving both false and true cords) with transglottic extension.
View Figure 2
Differential Diagnosis
Laryngeal cancer; Laryngeal tuberculosis.
Treatment
Patient was offered two treatment options. The first option being initiation of anti-TB drugs and radiotherapy, followed by review in 6 months' time to see the progress of illness. Another option was for total laryngectomy after stabilizing on anti-tubercular drugs. However, patient was undecided, which has led to the tumour being more extensive. Patient was referred to chest clinic and was started on anti-tubercular drugs for approximately 6 months since October 2015. Patient was referred to oncology team at National Cancer Institute for opinion. Having been reviewed in the oncology centre, patient was deemed unfit for chemo or radiotherapy as patient's general conditions were worsening.
Outcome and Follow-up
Patient passed away due to the adverse effects of his illness in early 2016. Patient was on anti-tubercular drugs for almost 6 months as he defaulted management of his laryngeal tumour. Patient was under our follow-up for less than a year before passing away.
Discussion
This case report presents the likelihood of both malignancy and chronic granulomatous lesions like TB co-existing together. These synchronous pathologies appear to be first case reported in literature. While extra pulmonary TB in the head and neck region most frequently occurs in the cervical lymph nodes (> 90%), involvement of larynx is only about 2% to 6%. Involvement of the temporal bone, sinonasal cavity, eye, pharynx, thyroid and skull base are even less frequently observed [7,8] Laryngeal TB is due to Mycobacterium tuberculosis. It represents the most frequent laryngeal granulomatous disease, but primary laryngeal location is exceptional. In TB, the larynx becomes infected either by a direct spread from the lungs, or by a haematogenous spread from sites other than the lungs. Since pathognomonic characteristics indicative of laryngeal TB do not exist, the infection is easily mistaken for the more frequently occurring laryngeal carcinoma [9,10].
The characteristics of laryngeal TB have changed over the years and it has become a challenge for medical experts to distinguish this disease from other illnesses. Besides, on laryngoscopy, tuberculosis infection may present as either a mass or ulcer which can mimic malignancy [11,12]. In the past, laryngeal TB typically affected young people in the second or third decade of life. Today, laryngeal TB mainly involves people in their 50s or 60s presenting first and foremost with hoarseness (80% to 100%). This was initial complaint of our patient. Other symptoms are odynophagia (50% to 67%) and to a lesser extent, dysphagia, dyspnoea, stridor, cough and haemoptysis [13].
According to a review about tuberculosis in Malaysia in 2014, 10% to 11% of TB cases at a tertiary level chest clinic were classified as extra pulmonary tuberculosis. And about 14% of pulmonary TB patients also had extra pulmonary involvement however there is no data available regarding number of laryngeal involvement of extra pulmonary tuberculosis [14]. On the other hand, laryngeal carcinoma is the main differential diagnosis in our patient's case. Laryngeal cancer is one of the increasing malignancies in otorhinolaryngology after nasopharyngeal carcinoma. But the incidence of it is actually low compared to other malignancies. In men, it comprises 1% of all carcinomas and in women it is much less. The importance of early diagnosis of cancer, in general, cannot be better illustrated than in the larynx [15]. According to National Cancer Institute of United States, in 2012, there were estimated 88,852 people living with larynx cancer in the country with a good 5-year survival rate of about 60.6% [16]. On the other hand, late detection can lead to losing the larynx or slow death from a fungating mass in the neck.
Retrospective study of 137 cases with carcinoma of the larynx seen in the Universiti Kebangsaan Malaysia (UKM) and General Hospital Kuala Lumpur between 1981 to 1988 revealed the peak incidence was in the seventh decade and the male to female ratio was 7.6:1 [17]. The most common symptom at presentation was hoarseness (90%). The most common histological type was squamous cell carcinoma (87%) whilst by site, transglottic involvement was the commonest (55%). The patient discussed in this case report does have the similar clinical findings as shown by the study. Laryngectomy has been a mainstay for treatment of advanced laryngeal squamous cell carcinoma for over 50 years. While total laryngectomy offers significant therapeutic benefit, it is fraught with some complications. The development of pharyngocutaneous fistula after total laryngectomy is one of the most common complication [18]. Though the preferred option in such cases will be laryngectomy, however, there is a high risk of pharyngocutaneous fistula secondary to anastomotic breakdown especially in patients being treated simultaneously for TB. According to an online article published in 2007 from Clinical Otolaryngology & Allied Sciences, postoperative pharyngocutaneous fistula is a troublesome complication in head and neck surgery and occurred in 8 out of 53 patients following total laryngectomy (15%) [19]. Pre-operative radiotherapy, residual cancer post radiotherapy and surgical technique of closure are other factors that seem to increase risk of fistula formation. Literature review did not show any reports to suggest increasing incidence of pharyngocutaneous fistula formation in tuberculosis patients.
Learning Points/Take Home Messages
1. TB and malignancy can occur synchronously at the same anatomical location.
2. Extrapulmonary tuberculosis like laryngeal tuberculosis is on the rise especially in developing countries.
3. Laryngeal TB should be considered as a differential diagnosis in any laryngeal disease and in particular in the case of a laryngeal carcinoma.
4. Final diagnosis is invariably based on histopathological findings as it is difficult to distinguish malignancy and TB from laryngoscopic features of mass alone.
References
-
World Health Organization (WHO) (2014) Global Tuberculosis Report.
-
World Health Organization (WHO) (2014) Reports of Malaysia's Incidence of Tuberculosis.
-
Benedict Ng (2014) TB kills more annually than dengue, Malaymail online newspaper.
-
Ministry of Health Malaysia (2013) A Report of Tuberculosis in Malaysia
-
Mastronikolis NS, Papadas TA, Goumas PD, Triantaphyllidou IE, Theocharis DA, et al. (2009) Head, neck: Laryngeal tumors: an overview. Atlas Genet Cytogenet Oncol Haematol 13: 888-893.
-
Malaysian National Cancer Registry Report (2007-2011) Malaysia Cancer Statistics, Data and Figure.
-
Levenson MJ, Ingerman M, Grimes C, Robbett WF (1984) Laryngeal tuberculosis: Review of twenty cases. Laryngoscope 94: 1094-1097.
-
Thaller SR, Gross JR, Pilch BZ, Goodman ML (1987) Laryngeal tuberculosis as manifested in the decades 1963-1983. Laryngoscope 97: 848-850.
-
El Kettani NE, El Hassani M, Chakir N, Jiddane M (2010) Primary laryngeal tuberculosis mimicking laryngeal carcinoma: CT scan features. Indian J Radiol Imaging 20: 11-12.
-
Ansari S, Amanullah MF, Ahmad K, Dhungel K, Gupta MK, et al. (2013) A rare case of laryngeal tuberculosis simulating malignancy. Nepal Journal of Medical Sciences 2: 200-202.
-
Rout MR, Moharana PR (2012) Tuberculosis of larynx: A case report. Indian J Tuberc 59: 231-234.
-
Smulders YE, De Bondt BJ, Lacko M, Hodge JA, Kross KW (2009) Laryngeal tuberculosis presenting as a supraglottic carcinoma: a case report and review of the literature. J Med Case Rep Nov 20: 9288.
-
AM Hunter, JW Millar, AJA Wightman, NW Horne (1981) The changing pattern of laryngeal tuberculosis. The Journal of Laryngology & Otology 95: 393-398.
-
Swarna Nantha Y (2014) A Review of Tuberculosis Research in Malaysia. Med J Malaysia 69: 88-102.
-
Minckler DS, Meligro CH, Norris HT (1970) Carcinosarcoma of the Larynx: Case Report with Metastases of Epidermoid and Sarcomatous Elements. Cancer 26: 195-200.
-
Cancer of Larynx, SEER Stat Fact Sheets: National Cancer Institute, Unites States.
-
A Sani, H Said, S Lokman (1992) Carcinoma of Larynx in Malaysia. Med J Malaysia 47: 297-302.
-
Liang JW, Li ZD, Li SC, Fang FQ, Zhao YJ, et al. (2015) Pharyngocutaneous fistula after total laryngectomy: A systematic review and meta-analysis of risk factors. Auris Nasus Larynx 42: 353-359.
-
J Lundgren, J Olofsson (1979) Pharyngocutaneous fistulae following total laryngectomy. Clinical Otolaryngology &Allied Sciences 4: 13-23.