Journal of Otolaryngology and Rhinology
Reduction of Bilateral Anterior Table Frontal Sinus Fractures Using Balloon Sinus Dilation Catheters: A Case Report
Andrew Petersen1, Fariha Farid2, Richard Klapchar1, Sumit Bapna3 and Boris Karanfilov3*
1Ohiohealth ENT, Columbus, Ohio, USA
2Providence Health, Everett, Washington, USA
3Ohio Sinus Institute, Ohio, USA
*Corresponding author:
Boris Karanfilov, Ohio Sinus Institute, 5378 Avery Rd, Dublin, Ohio 43016, USA, Tel: 614-771-9871, E-mail: bk@ohiosinus.com
J Otolaryngol Rhinol, JOR-2-027, (Volume 2, Issue 4), Case Report
Received: August 29, 2016 | Accepted: November 30, 2016 | Published: December 03, 2016
Citation: Petersen A, Farid F, Klapchar R, Bapna S, Karanflov B (2016) Reduction of Bilateral Anterior Table Frontal Sinus Fractures Using Balloon Sinus Dilation Catheters: A Case Report. J Otolaryngol Rhinol 2:027.
Copyright: © 2016 Petersen A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Frontal sinus fractures contribute to 5-15% of all facial fractures and are most often associated with motor vehicle accidents (52%) and assault (26%) [1]. Although less common than other facial fractures, their management deserves special attention due to the risk of short and long-term complications [2]. The management algorithm for frontal sinus fractures is one that has been debated in the literature for many years with no clear consensus. More recently, there has been a trend towards sinus preservation with a focus on restoring normal anatomy instead of the traditional management of frontal sinus obliteration or cranialization [2,3]. The evaluation, classification, and management of such injuries continue to be studied.
We report the use of multiple balloon sinus dilation (BSD) catheters in the reduction of bilateral anterior table frontal sinus fractures in a 13-year-old male following sports injury. This case is unique in that it displays a less-invasive surgical correction of anterior table frontal sinus fractures using a new surgical tool and follows the literature-supported trend towards sinus preservation. More extensive frontal sinus fractures with severe comminution or displaced posterior table fractures may still deserve open approaches with mini-plating and possible sinus obliteration to assure fracture reduction, fixation, and prevent the risk of intracranial infection [4]. However, in isolated anterior table frontal sinus fractures, endoscopic minimally invasive techniques save the patient from the morbidity of larger procedures while maintaining a functioning frontal sinus.
Prior reports using balloon catheters as tools for fracture reduction have been cited and will later be discussed in more detail. Our case is unique in that we used multiple BSD catheters to simultaneously reduce bilateral anterior table frontal sinus fractures.
Keywords
Sinus dilation catheter, Balloon sinus dilation, Frontal sinus fracture, Sinusitis, Frontal sinusitis
Case Report
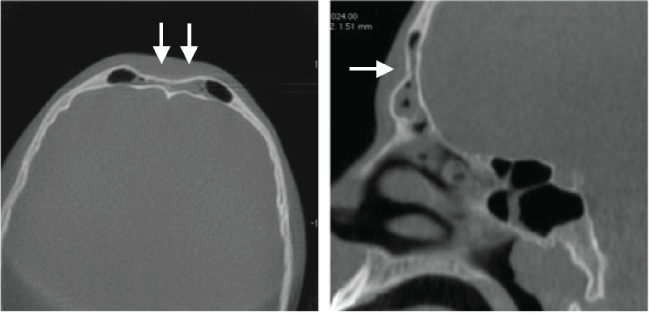
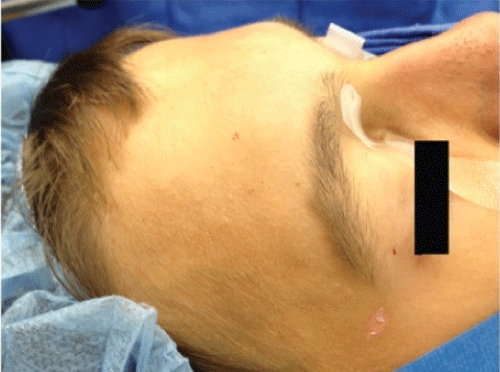
A 13-year-old male who sustained an anterior table frontal sinus fracture while playing basketball presented to the emergency department for evaluation. A head computed tomography (CT) scan and full workup was preformed and he was found to have no other injuries or neurologic symptoms. The patient denied epistaxis, clear rhinorrhea, diplopia or blurry vision. On exam, there was evidence of depression of the anterior table of the frontal sinus with cosmetic deformity. The nasal bones were intact. Same day referral to our clinic was made where nasal endoscopy was performed and there was no evidence of CSF rhinorrhea or septal hematoma. In office, high-resolution cone beam CT scan was preformed for greater assessment of the frontal sinus anatomic structures and preoperative surgical planning compatible with computer image guidance systems. Imaging revealed bilateral isolated anterior table frontal sinus fractures without posterior table involvement (Figure 1and Figure 2).
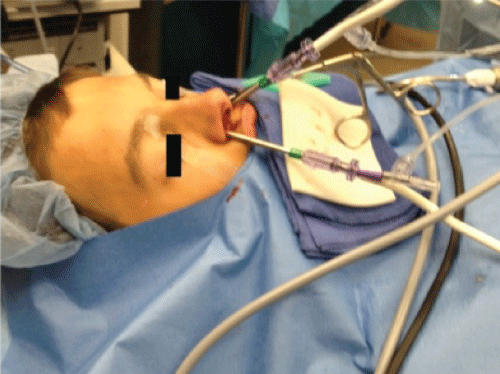
The patient subsequently underwent functional endoscopic sinus surgery under general anesthesia. Endoscopic dissection of the frontal recess was performed with a 70-degree endoscope and a 5 mm mid-forehead incision was made to allow direct visualization of the fractures. A balloon sinus dilation catheter (Acclarent, Inc. Menlo Park, CA) was then advanced into both the right and left frontal sinus under endoscopic guidance. Two separate 7 × 16 mm balloons were inserted through the dissected frontal recess and positioned at the most depressed portion of the anterior table fractures. The balloons were then individually inflated to 12 atmospheres with direct visualization of fracture reduction (Figure 3).
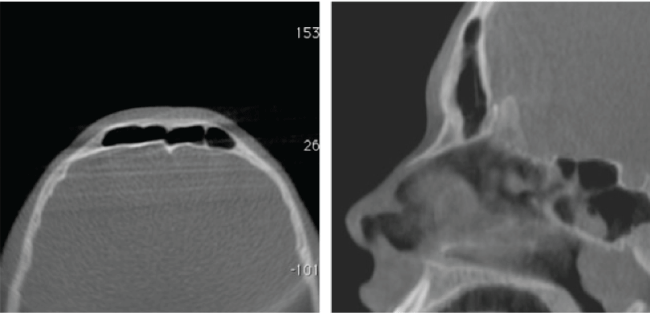
Cortisporinotic suspension soaked gel foam pieces were placed into the frontal sinus to serve as a scaffold during healing. Bilateral Merocel finger-cot meatal spacers were placed and the procedure was complete. The patient was discharged to home with pain medications, oral antibiotics, and activity restrictions. On postoperative day 7 the nasal packing was removed which revealed healing nasal mucosa with no signs of stenosis or ostial obstruction. CT was performed at 2 months, which showed successful reduction of the anterior table fractures (Figure 4). The frontal sinus outflow tract was open and functional at 12 months.
Discussion
In the past, management of frontal sinus fractures followed well described algorithms, however, with the advent of modern endoscopic techniques, recommendations are shifting towards frontal sinus physiologic preservation. Short and long-term complications of frontal sinus fractures include poor cosmesis, delayed mucocele formation, ostial obstruction, and development of chronic rhinosinusitis [2,5,6]. Additional complications may occur when the posterior frontal sinus table is involved, which includes the risk of meningitis and intracranial infection. An area of particular focus and controversy is when fractures involve the frontal sinus outflow tract (FSOT).
The traditional management of fractures involving the FSOT includes a bicoronal incision and sinus obliteration or cranialization. The approach includes a large incision with wide exposure of the frontal bone and fracture, which risks supratrochlear and supraorbital nerve injury, further fracture comminution, bony devascularization, and poor cosmesis [2]. Cosmetic concerns include bicoronal incision scar, hair loss, and irregular frontal contour due to bony loss or the use of an osteoplastic flap and mini-plate application [3,5]. Additionally, the frontal sinus mucosa is removed and the sinus cavity is obliterated, usually with fat, and then separated from the nose with packing or live tissue, in the form of a pericranial flap, and synthetic tissue sealants [2-4]. Long-term complications include development of chronic frontal sinusitis and delayed mucocele formation, which can be difficult to adequately image in the setting of obiterative techniques, as fat and other packing materials may mask an acute infectious or suppurative process [7].
In patients with isolated anterior table frontal sinus fractures, current rhinologic consensus recommends a more conservative surgical approach aimed at sinus mucosa preservation and restoration of normal anatomy [5,8]. Instead of sinus obliteration, newer protocols involve open reduction internal fixation of fracture sites, 4 weeks of oral antibiotics, follow up CT scans, and then endoscopic sinus surgery, if warranted [2].The use of endoscopic balloon reduction of anterior frontal sinus fractures follows this trend towards sinus preservation, as described by previous authors. The impact of sinus preservation is significant, as it allows continued sinus aeration and reduces the risk of frontal chronic rhinosinusitis and delayed mucocele formation [2,4]. Endoscopic fracture reduction also allows for reliable follow up imaging, shorter operative times, and avoids the previously mentioned risks associated with sinus obliteration procedures.
BSD is a minimally invasive surgical tool for the treatment of chronic rhinosinusitis that was introduced in 2005 and then approved for use in the office setting, under local anesthesia, in 2011. BSD catheters were designed to be less traumatic tools to open the paranasal sinuses and reduce the need for formal dissection and removal of bony septa and mucosa. BSD catheters are flexible with narrow diameters, which allow for ease of positioning in the narrow and variable FSOT [9-11]. These properties appeal to surgeons for the endoscopic reduction of frontal sinus fractures that would be difficult to reach via traditional endoscopic instruments.
Our report describes the use of multiple BSD catheters to endoscopically reduce bilateral anterior table frontal sinus fractures in the acute, post-injury setting. There are previous reports of using sinus dilation balloon catheters and custom balloons made from Foley catheters for frontal sinus fracture reduction [12,13]. While limited in numbers, there has been initial success in the use of balloons to reduce anterior table frontal sinus fractures. Our report adds to the evidence of the success of this technique and describes a new application for the use of multiple balloons in instances of bilateral fractures involving the frontal sinus outflow tract. Degree of fracture displacement, comminution, or posterior table involvement may however still dictate open procedures with sinus obliteration [4].
Disadvantages to fracture reduction with BSD catheters include the limited view of fracture lines via endoscopic approaches. We found that using a 5 mm mid forehead incision allowed us to sufficiently visualize fracture lines while adding little morbidity or cosmetic sacrifice. Additionally, there is limited ability to stabilize fractures with endoscopic-guided balloons, compared to open reduction internal fixation techniques. We were able to adequately support our reduced fracture with gel foam packing within the frontal sinus. While successful at reducing simple anterior table frontal sinus fractures, severely comminuted fractures still pose a challenge. It is unlikely that multiple bony fragments or severely displaced fracture lines would be able to achieve adequate reduction with the use of balloons and endoscopic techniques alone, thus proper patient selection is vital. There are also potential complications with the use of BSD catheters themselves including CSF leak and orbit penetration [10,11]. Ultimately, the minimally invasive benefits outweigh the risks when careful use of BSD catheters is applied to reduce frontal sinus fractures in carefully selected patients.
Conclusion
BSD catheters may be considered as fracture reduction tools in the management of isolated anterior table frontal sinus fractures. They have shown the ability to reduce bilateral frontal sinus fractures involving the frontal sinus outflow tract with effective long-term results. With proper patient selection, balloon catheters are effective tools in the management of anterior table frontal sinus fractures with the aim of sinus preservation.
References
-
Johnson J, Rosen C, Bailey B (2013) Bailey's Head And Neck Surgery-Otolaryngology. (5th edn), Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins, 1255-1271.
-
Smith T, Han J, Loehrl T, Rhee J (2002) Endoscopic Management of the Frontal Recess in Frontal Sinus Fractures: A Shift in the Paradigm? Laryngoscope 112: 784-790.
-
Emara T, Elnashar I, Omara T, Basha W, Anany A (2015) Frontal sinus fractures with suspected outflow tract obstruction: A new approach for sinus preservation. J Craniomaxillofac Surg 43: 1-6.
-
Carter K, Poetker D, Rhee J (2010) Sinus Preservation Management for Frontal Sinus Fractures in the Endoscopic Sinus Surgery Era: A Systematic Review. Craniomaxillofac Trauma Reconstr 3: 141-149.
-
Stanley R (1988) Management of Frontal Sinus Fractures. Facial Plastic Surg 5: 231-235.
-
Gonty A, Marciani R, Adornato D (1999) Management of frontal sinus fractures: A review of 33 cases. J Oral Maxillofac Surg 57: 372-379.
-
Weber R, Draf W, Keerl R, Kahle G, Kind M, et al. (2002) Magnetic resonance imaging following fat obliteration of the frontal sinus. Neuroradiology 44: 52-58.
-
Bell R, Dierks E, Brar P, Potter J, Potter B (2007) A Protocol for the Management of Frontal Sinus Fractures Emphasizing Sinus Preservation. J Oral Maxillofacial Surg 65: 825-839.
-
Levy J, Marino M, McCoul E (2016) Paranasal Sinus Balloon Catheter Dilation for Treatment of Chronic Rhinosinusitis: A Systematic Review and Meta-analysis. Otolaryngol Head Neck Surg 154: 33-40.
-
Bolger W, Vaughan W (2006) Catheter-based dilation of the sinus ostia: Initial safety and feasibility analysis in a cadaver model. Am J Rhinol 20: 290-294.
-
Brown C, Bolger W (2006) Safety and Feasibility of Balloon Catheter Dilation of Paranasal Sinus Ostia: A Preliminary Investigation. Ann Otol Rhinol Laryngol 115: 293-299.
-
Hueman K, Eller R (2008) Reduction of anterior frontal sinus fracture involving the frontal outflow tract using balloon sinuplasty. Otolaryngol Head Neck Surg 139: 170-171.
-
Yoo M, Kim J, Song H, Lee B, Jang Y (2008) Endoscopic Transnasal Reduction of an Anterior Table Frontal Sinus Fracture: Technical note. Int J Oral Maxillofac Surg 37: 573-575.