Journal of Otolaryngology and Rhinology
Use of Vestibular Evoked Myogenic Potentials in Ear Selection for Surgical Treatment of Bilateral Benign Paroxysmal Positional Vertigo
Sandhu JS1,2*, Rea PA3 and Ray J1
1Department of Ear, Nose & Throat Surgery, Royal Hallamshire Hospital, UK
2University of Leicester Medical School, Maurice Shock Building, Leicester University, UK
3Department of Ear, Nose & Throat Surgery, Leicester Royal Infirmary, UK
*Corresponding author:
Dr. JS Sandhu, Department of Ear, Nose & Throat Surgery Royal Hallamshire Hospital, Glossop Road, 36 Totley Brook Road, Dore, Sheffield, S17 3QS, UK, Tel: +44 (0) 7921189307, E-mail: jassandhu@nhs.net
J Otolaryngol Rhinol, JOR-2-017, (Volume 2, Issue 2), Case Report
Received: January 05, 2016: Accepted: March 31, 2016: Published: April 02, 2016
Citation: Sandhu JS, Rea PA, Ray J (2016) Use of Vestibular Evoked Myogenic Potentials in Ear Selection for Surgical Treatment of Bilateral Benign Paroxysmal Positional Vertigo.
J Otolaryngol Rhinol 2:017
Copyright: © 2016 Sandhu JS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In cases of intractable benign paroxysmal positional vertigo (BPPV) where conservative management has failed, surgical plugging of the semi-circular canal can provide an effective solution. Where bilateral disease is present, selecting the ear on which to operate can provide a challenge as there is often a pre-existing vestibulopathy and therefore surgery carries a considerable risk of chronic imbalance. It is therefore essential to gather maximal information regarding vestibular function as possible. We propose using the vestibular evoked myogenic potential test as a powerful adjunct to this process and discuss a complex case in which this has been successfully implemented.
Keywords
Benign paroxysmal positional vertigo, BPPV, Vestibular evoked myogenic potential, VEMP, Intractable vertigo, Posterior semicircular canal plugging
Introduction
Benign paroxysmal positional vertigo (BPPV) is a common cause of dizziness accounting for 17%-40% of clinical presentations [1]. In a significant proportion of BPPV cases (6%-14%) the disease is found to be present bilaterally, with it occurring more commonly following head trauma [2]. Usually an effective treatment is provided by particle repositioning manoeuvres [3]. Where bilateral disease is present a sequential approach is often taken. However in a small number of cases conservative treatment is unsuccessful and surgical intervention is required. This is usually carried out using the posterior semicircular canal occlusion (PSCO) technique [4]. The procedure involves occluding the canal lumen such that endolymphatic movement is compromised thus rendering the canal dysfunctional.
Usually the surgery is carried out on the side which is most affected by the BPPV and has the lowest overall vestibular function, thereby providing the maximum opportunity for post-surgical central compensation to take place. In order to assess vestibular function the most commonly used technique is the bi-thermal caloric test [5]. Although well established and readily available the test is limited to providing information relating to function of the lateral semicircular canal in the low frequency range. In order to add further information relating to otolith function the vestibular evoked myogenic potential [6] (VEMP) test can be utilised. In this paper we discuss a case of intractable bilateral BPPV where the choice of treatment ear was not clear. VEMP testing was therefore used to aid in the decision process and a comparison of pre and post surgical testing shows a marked improvement in overall balance as well relief from the BPPV.
Case
A 49 year-old woman was first referred to our tertiary Ear Nose and Throat (ENT) balance service three years ago. At the time she gave a two-year history of short lasting intermittent bouts of true rotatory vertigo coupled with continuous disequilibrium and imbalance. There were no reported complaints of hearing loss, tinnitus, aural fullness or any other otological symptoms. There was no history of any headaches and magnetic resonance imaging showed no abnormalities. Physical examination including otological, neurological and oculomotor components did not show any deficits.
In order to establish baseline measurements a series of audiovestibular tests were conducted. Audiometry and tympanometry were both within the normative range. Caloric testing showed zero response on the right side to warm, cool and ice water irrigations. The left side yielded responses of 2.5°/s and 2.0°/s to warm and cool irrigations respectively. Computerised dynamic postuography was used to assess sensory organization. This showed poor overall balance and strikingly minimal input from the vestibular system (Figure 1). Her case notes confirmed that her initial Dix-Hallpike testing had been negative, however during subsequent consultations showed bilateral posterior canal BPPV with the left side dominating over the right. The distribution of side and severity of the BPPV with respect to time is summarised in table 1. Given these findings and the clinical history, a diagnosis of bilateral BPPV with underlying vestibulopathy was made and a management plan based on a combination of particle repositioning manoeuvres and vestibular rehabilitation was formulated.
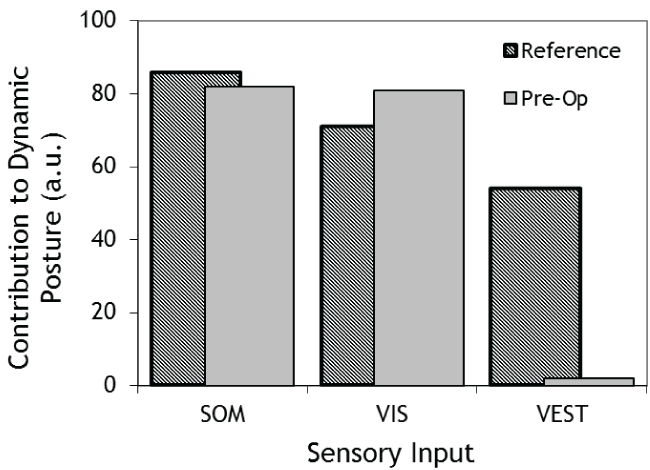
.
Figure 1: Computerised Dynamic Postuography showing the contributions of somatosensory (SOM), visual (VIS) and vestibular (VEST) inputs pre-surgery compared to age-normalised values.
View Figure 1
![]()
Table 1: History of BPPV symptoms with side and severity of response to Dix-Hall-Pike Testing.
View Table 1
Unfortunately the conservative treatment regime did not prove successful. Although the particle repositioning manoeuvres resolved the BPPV for short periods of time it continued to return with attacks becoming more frequent over time. This in turn impacted the vestibular rehabilitation therapy, which was beneficial during the quiescent periods of BPPV but decompensation occurred following the intermittent attacks of BPPV. As a result it was decided that surgical canal occlusion was necessary. Whilst it was clear that the left ear was most affected by the BPPV the dilemma was that this was the side that according to caloric testing retained the most vestibular function. Therefore operating on this side carried a significant risk of worsening her overall balance. Therefore it was necessary to further investigate the functionality of the vestibular system to ascertain if the assumption that the left side was stronger than the right was actually correct. This was achieved by utilising the VEMP test. There are many forms of the VEMP test [7]. The set-up that was used in this case involved an air-conduction stimulus and recording at the contracted ipsilaterral sternocleidomastoid (SCM) muscle. This is also referred to as the C-VEMP in the literature. The contraction is needed as the response is inhibitory and thus requires background muscle tonicity to be present. In this configuration the end organ being tested is the ipsilateral saccule. Results from VEMP testing showed there to be responses bilaterally with a small clinically insignificant difference between the two sides (Figure 2).
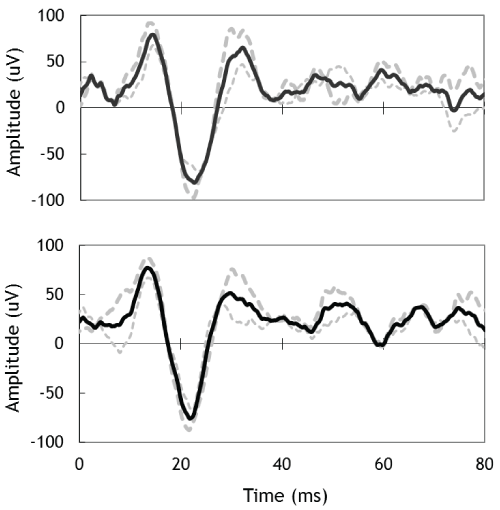
.
Figure 2: Cervical VEMPs for left-ear (top) and right-ear (bottom) obtained using 100 dB 500 Hz air-conduction tone-bursts. Dashed grey lines are individual runs and the solid black lines are averaged responses.
View Figure 2
The results from VEMP testing confirmed normal saccule function bilaterally. In comparison the small function of the lateral canal shown by the caloric results was therefore less significant. As a result it was decided that the likelihood of the surgery causing degradation in overall balance was significantly reduced and as a consequence the decision was taken to operate on the left ear.
At a six-month post surgical review the patient was found to be free of BPPV symptoms and overall balance was improving. Postuography testing was repeated at twelve months post-surgery and objectively confirmed that much better use of the vestibular inputs was being made (Figure 3).
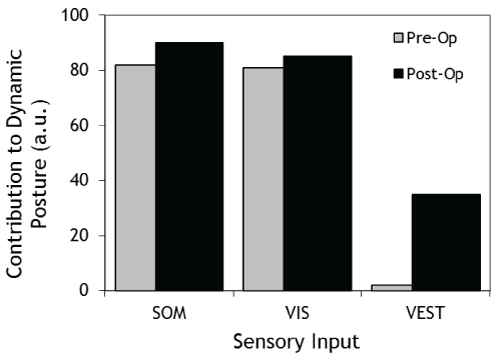
.
Figure 3: Computerised Dynamic Posturography showing the contributions of somatosensory (SOM), visual (VIS) and vestibular (VEST) inputs pre-surgery and post-surgery.
View Figure 3
Discussion
Although rare for a small number of patients with intractable posterior canal BPPV the only definite treatment option is the surgical occlusion of the posterior semicircular canal. Although this treatment is very effective at resolving BPPV it does by design remove function of the canal in question. Furthermore as with any otological procedure it carries a risk of unintentional damage to both the cochlea as well as the vestibular organ. Therefore when considering which ear to operate on both current symptoms, associated with the BPPV, and future problems that may result from the surgery such as chronic imbalance must be considered. The impact of the latter point is very dependent upon the relative vestibular function of the two sides and therefore information relating to the function of inner ear should be maximised prior to surgery. To date most ENT surgeons rely on the caloric test to provide information concerning the lateral canal. We strongly suggest that the cervical VEMP test be now routinely used to assess saccular function as it provides valuable additional information. Furthermore given that the source of the otoconia debris is known to be the utricle we also advocate that the ocular VEMP be recorded in this patient population as this test provides important additional information relating to the functional status of this end organ. Currently there is growing interest in examining whether or not information pertaining to the condition of the otolith organs may be used to shape vestibular rehabilitation management strategies. Whilst this field is in its infancy the prospects remain enticing and intriguing.
Conclusion
We have recognised the clinical application of the VEMP test as part of the pre-surgical testing of patients undergoing posterior canal plugging for intractable BPPV. Furthermore we advocate that the test be used whenever considering any procedure that may interrupt or permanently alter balance function, as it may be able to provide additional prognostic information.
Ethical Statement
1. The authors have no funding, financial relationships or conflicts of interest to disclose.
2. Permission from the patient was obtained prior to the preparation of the manuscript.
References
-
Leveque M, Labrousse M, Seidermann L, Chays A (2007) Surgical therapy in intractable benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg 136: 693-698.
-
Katsarkas A (1999) Benign paroxysmal positional vertigo (BPPV): idiopathic versus post-traumatic. Acta Otolaryngol 119: 745-749.
-
Fife TD, Iverson DJ, Lempert T, Furman JM, Baloh RW, et al. (2008) Practice parameter: therapies for benign paroxysmal positional vertigo (an evidence-based review): Report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology 70: 2067-2074.
-
Parnes LS, McClure JA (1990) Posterior semicircular canal occlusion for intractable benign paroxysmal positional vertigo. Ann Otol Rhinol Laryngol 99: 330-334.
-
(1993) Jacobson GP, Newman CW, Kartush JM, Handbook of Balance Function Testing. St Louis, MI: Mosby Year Book.
-
Colebatch JG, Halmagyi GM, Skuse NF (1994) Myogenic potentials generated by a click-evoked vestibulocollic reflex. J Neurol Neurosurg Psychiatry 57: 190-197.
-
Rosengren SM, Welgampola MS, Colebatch JG (2010) Vestibular evoked myogenic potentials: past, present and future. Clin Neurophysiol 121: 636-651.





