Journal of Otolaryngology and Rhinology
Ortner's Syndrome Caused by Idiopathic Pulmonary Artery Aneurysm
Aleix Rovira1*, Marta Fulla Campi2, Julio Nogués Orpí3 and Manel Maños Pujol4
14th Year resident, Department of Otorhinolaryngology, Hospital Universitari de Bellvitge, University of Barcelona, Spain
23rd Year resident, Department of Otorhinolaryngology, Hospital Universitari de Bellvitge, University of Barcelona, Spain
3Chief of head and neck surgery division, Department of Otorhinolaryngology, Hospital Universitari de Bellvitge, University of Barcelona, Spain
4Professor and Chairman, Department of Otorhinolaryngology, Hospital Universitari de Bellvitge, University of Barcelona, Spain
*Corresponding author:
Aleix Rovira, Department of Otorhinolaryngology, Hospital Universitari de Bellvitge, C/ Feixallarga s/n. Hospitalet de Llobregat. 08908, University of Barcelona L'Hospitalet de Llobregat, Barcelona, Spain, Tel: +34678960441, E-mail: roviracasasaleix@gmail.com
J Otolaryngol Rhinol, JOR-2-015, (Volume 2, Issue 1), Case Report
Received: January 12, 2016: Accepted: February 23, 2016: Published: February 26, 2016
Citation: Rovira A, Campi MF, Orpí JN, Pujol MM (2016) Ortner's Syndrome Caused by Idiopathic Pulmonary Artery Aneurysm. J Otolaryngol Rhinol 2:015
Copyright: © 2016 Rovira A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The Ortners syndrome or cardiovocal syndrome is an uncommon entity characterized by hoarseness due to left recurrent laryngeal nerve paralysis caused by identifiable cardiovascular disease. The most common conditions which may lead to Ortner's syndrome include mitral stenosis, aortic aneurysm, mitral valve prolapsed, cardiovascular surgery, aortic dissection etc. Herewith, we report the case of an atypical etiology of cardiovocal syndrome in a patient with a Pulmonary Artery Aneurysm (PAA).
Keywords
Dysphonic, Vocal cord palsy, Ortner, Pulmonary aneurism
Introduction
Hoarseness is a common condition underlying many different causes. The left recurrent laryngeal nerve paralysis caused by identifiable cardiovascular disease is known as Ortner's syndrome or cardiovocal syndrome. Ortner's syndrome was first described by Norbert Ortner in 1897, in a patient with mitral stenosis with dilated left atrium [1]. Many other etiologies have been identified as the cause of this entity. We present here the first Ortner's syndrome due to idiopathic pulmonary aneurysm without primary pulmonary hypertension.
Case Report
A healthy 42-year-old woman was referred to the ear, nose and throat (ENT) department complaining about three-month history of hoarseness, with no other associated pathology. She was a non-smoker patient without any relevant past medical history.
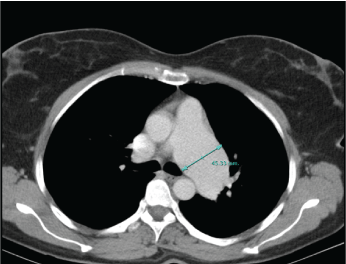
The clinical examination with indirect laryngoscopy revealed a paralyzed left vocal cord in paramedian position while the rest of the otolaryngologic exam was normal. Tuberculosis, Lyme disease and syphilis infections were ruled out as well as collagen vascular disorders and sarcoidosis. No prior history of blunt or penetrating trauma neither surgery was identified. Contrast-enhanced computed tomography (CT) of the neck and chest was performed to rule out any cervico-thoracic process causing the symptoms. The CT examination showed a PAA that involves the trunk and the main left pulmonary artery, with a maximum diameter of 45 mm. The echocardiogram study showed neither structural cardiopathy nor pulmonary hypertension, so it lead to the diagnosis of idiopathic PAA. A specialist for cardio-thoracic surgery was consulted but surgical intervention was dismissed due to the low risk of artery dissection according to the size of the aneurysm and the symptoms of the patient. Currently, the patient is followed by the speech therapist, the cardiothoracic surgeon and the ENT surgeon with improvement of the voice quality.
Discussion
The left vagus nerve supplies the innervation of the larynx with their two terminal branches, the laryngeal recurrent nerve and the superior laryngeal nerve. The vagus nerve emerges through the jugular foramen and runs within the carotid sheath together with the carotid artery and the internal jugular vein. The left recurrent laryngeal nerve is a branch of the left vagus nerve at the level of the aortic arch. This nerve curves below the aorta and ascends to the tracheoesophageal groove. The laryngeal recurrent nerve supplies all the muscles acting on the vocal cords, except the cricothyroid muscle, which is innervated by the superior laryngeal nerve. Due to this large trajectory, this nerve may be injured in many different locations. In unilateral vocal cord paralysis due to thoracic disease, left vocal cord paralysis was 1.75 times more frequent than the right side [2].
Neck and chest CT scan utility to identify the etiology of a vocal cord paralysis has been widely reported [2]. Sun and colleagues published a retrospective study to evaluate the profitability of this test to rule out the etiology of vocal paralysis, concluding that CT is a helpful tool for the early detection of malignant and non-malignant causes of vocal cord paralysis [2].
Many different causes have been attributed to Ortner's syndrome. It was associated with mitral stenosis or regurgitation, atrial mixoma, primary pulmonary hypertension, aortic aneurysm or dissection, pulmonary embolism, defibrillation, atrial fibrillation, cardiothoracic surgery, and heart-lung transplantation [3,4]. Although initially, enlarged left atrium was proposed as the main cause of laryngeal recurrent nerve compression, the current opinion seems to support the theory that pulmonary artery plays the main role on this pathology. In our patient, the most probable cause of the left vocal cord paralysis seems to be the compression of the left recurrent nerve at the level of the aortopulmonary window, instead of a left atrium enlargement as have been previously described by other authors.
We performed an exhaustive revision of the previous studies published about cardiovocal syndrome, identifying among 65 previous cases of these syndrome, and we did not find any patient with pulmonary idiopathic aneurysm as origin of left vocal cord paralysis.
Pulmonary artery aneurysm is a rare entity with an estimated prevalence of 1 in 14000 individuals [5]. PAA is described by a pulmonary trunk diameter exceeding 4cm diameter [4]. This entity may be classified according with the pulmonary artery pressure as high and low pressure. Among low pressure PAA infectious disorders, Behçet disease, connective tissue diseases and pregnancy have been identified as risk factor for developing this disorder [6,7]. Idiopathic PAA is also classified as in the low pressure group with a very low incidence. Deb et al. described a single institution experience on PA surgery during the period 1977-2002 [6]. In this report, 51 PA aneurysm corrections were described, of which five cases were idiopathic PAA. Treatment can be either conservative or surgical, recommending surgical repair when they are symptomatic or larger than 6 cm.
This non previous published case should illustrates to the ENT surgeon the countless different causes which may lead to a vocal cord paralysis, revealing the importance role of CT scan to identify their etiology.
References
-
Ortner N (1897) Recurrent laryngeal nerve paralysis due to mitral valve stenosis. Wien Klin Wochenschr 10: 753-755.
-
Song SW, Jun BC, Cho KJ, Lee S, Kim YJ, et al. (2011) CT evaluation of vocal cord paralysis due to thoracic diseases: a 10-year retrospective study. Yonsei Med J 52: 831-837.
-
Monwarul Islam AK, Zaman S, Doza F (2012) Ortner syndrome due to concomitant mitral stenosis and bronchiectasis. Korean Circ J 42: 507-510.
-
Lee SI, Pyun SB, Jang DH (2006) Dysphagia and hoarseness associated with painless aortic dissection: a rare case of cardiovocal syndrome. Dysphagia 21: 129-132.
-
Deterling RA Jr, Clagett OT (1947) Aneurysm of the pulmonary artery; review of the literature and report of a case. Am Heart J 34: 471-499.
-
Deb SJ, Zehr KJ, Shields RC (2005) Idiopathic pulmonary artery aneurysm. Ann Thorac Surg 80: 1500-1502.
-
Theodoropoulos P, Ziganshin BA, Tranquilli M, Elefteriades JA (2013) Pulmonary Artery Aneurysms: Four Case Reports and Literature Review. Int J Angiol 22: 143-148.