Journal of Otolaryngology and Rhinology
Metastatic Colorectal Carcinoma to Thyroid Gland on Background of Long Standing Multinodular Goiter
May Lim1*, Annabelle C Leong1 and Vijayadwaja Desai2
1Department of Otolaryngology, Khoo Teck Puat Hospital, Singapore
2Department of Anatomical Pathology, Khoo Teck Puat Hospital, Singapore
*Corresponding author:
May Lim, MBBS (Singapore), MRCS (Edin), Department of Otolaryngology, Khoo Teck Puat Hospital, 90 Yishun Central, Singapore 768828, Tel: +65 6602 2197, Email: may.lim@mohh.com.sg
J Otolaryngol Rhinol, JOR-2-014, (Volume 2, Issue 1), Case Report
Received: January 01, 2016: Accepted: February 22, 2016: Published: February 25, 2016
Citation: Lim M, Leong AC, Desai V (2016) Metastatic Colorectal Carcinoma to Thyroid Gland on Background of Long Standing Multinodular Goiter. J Otolaryngol Rhinol 2:014
Copyright: © 2016 Lim M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction:Tumor metastases from colorectal carcinoma to the thyroid gland are extremely rare. We present a case of metastatic colonic adenocarcinoma to the thyroid occurring in a longstanding multinodular goiter together with a review of existing literature.
Case report:A 60 year old lady presented acutely with stridor in 2014 on a background of colorectal carcinoma diagnosed 2003 and multinodular goiter diagnosed in 2006. Imaging showed multinodular goiter with suspicious foci of malignancy causing tracheal invasion and compression. She underwent tracheostomy and biopsy of thyroid isthmic tumor, which confirmed metastatic colonic carcinoma.
Conclusions:Patients with pre-existing thyroid disease have increased risk of developing metastatic thyroid nodules. Surgical treatment may reduce compressive symptoms or avoid further dissemination of primary carcinoma. However long-term prognosis is dependent on stage of primary tumor.
Our case represents the longest known interval of 11 years from primary diagnosis of colorectal carcinoma to detection of clinically significant thyroid metastases.
Keywords
Neoplasm metastasis, Thyroid nodule, Colorectal carcinoma, Airway obstruction
Introduction
Tumor metastases to the thyroid gland are uncommon in clinical practice, with the overall clinical incidence at 1.4-3% [1,2]. In particular, thyroid metastases from a primary colorectal carcinoma are extremely rare. Fewer than 50 such cases have been reported in the world literature [3], with only two cases reported thus far in our local population [4]. We present a case of metastatic colonic adenocarcinoma to the thyroid, occurring in a longstanding multinodular goiter eleven years after initial diagnosis of the primary tumor, together with a review of current literature. To our knowledge, our present case represents the longest interval between initial diagnosis of a colonic primary and subsequent development of metastases to the thyroid.
Case Report
In 2003, a 49 year old Chinese lady presented with a 3 month history of per rectal bleeding. A colonoscopy demonstrated a recto-sigmoid tumor whose biopsy showed moderately differentiated adenocarcinoma. Carcinoembryonic Antigen (CEA) levels were elevated at 525.5 ug/L. She underwent low anterior resection with salpingo-oophorectomy and total hysterectomy for colorectal carcinoma with uterine and ovarian invasion. One year later, she further underwent Hartmann's procedure with resection of anastomotic segment for carcinoma recurrence, followed by postoperative chemoradiotherapy.
Four years after the diagnosis of the primary tumor, she was discovered to have secondary lung metastases and underwent left lateral thoracotomy and upper lobe wedge resection. She suffered recurrence of the lung metastases one year later and was there after treated for the subsequent six years till October 2014 with multiple lines of palliative chemotherapy.
In December 2014, the patient, by then 60 years of age, was admitted and referred to our department for sudden onset dyspnea and inspiratory stridor. At time of admission, it was noted that she had a history of a multinodular goiter noted on follow up serial Computed Tomography (CT) imaging since 2006. It had been reported to be causing tracheal deviation and mild tracheal compression but at that point there were no suspicious features reported on imaging to suggest carcinoma or metastases. The patient had thereafter declined further investigations for the goiter.She did not undergo fine needle aspiration cytology for the thyroid nodules. The goiter was noted to be stable on subsequent follow up serial CT imaging done annually from 2007 to 2013 to monitor her lung metastases - there were no features to suggest malignant change or metastatic deposits.
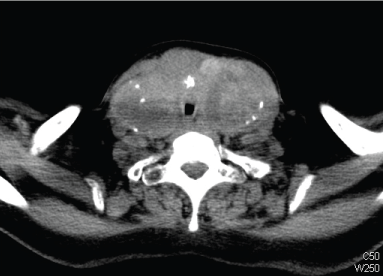
Urgent CT imaging performed during the emergency admission in 2014 confirmed the presence of a multinodular goiter with gradual progressive enlargement over the years. This time however, interval development of lobulated soft tissue suggestive of focus of thyroid malignancy was noted arising from an isthmus nodule, with projection into the lumen of the trachea causing further tracheal narrowing. At the point of maximal narrowing, the trachea was only 7 × 6 mm in axial diameter at the level of C7 (Figure 1).
.
Figure 1: Axial cross section of CT Neck image showing maximal point of trachea compression and invasion caused by diffuse goitre.
View Figure 1
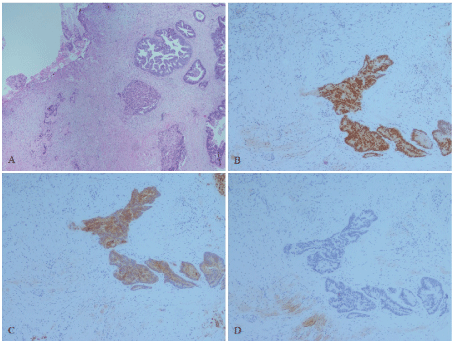
In view of the threat to the patient's airway, she underwent a tracheostomy and biopsy of thyroid isthmic tumor. Intraoperatively, a hard irregular thyroid lesion invading thyroid and cricoid cartilages was noted, with invasion into the subglottis. Histology of the specimen showed infiltration by a moderately differentiated adenocarcinoma, confirmed to be of colorectal origin via haematoxylin & eosin (H & E) staining (Figure 2, slide A). Further relevant immunohistochemistry stainswere also carried out to confirm adenocarcinoma of intestinal origin as detailed in figure 2 - the tissue stained positive for Caudal Type Homeobox 2 (CDX2) and cytokeratin 20 (CK 20), and negative for Thyroid transcription factor - 1 (TTF-1).
.
Figure 2: Histopathological slides (A) to (D) confirming diagnosis of metastatic colonic adenocarcinoma to the thyroid; (A) H & E stain demonstrating connective tissue infiltrated by adenocarcinoma with colonic pattern of malignant glands with necrosis; (B) & (C) CDX2 and CK 20 staining respectively demonstrating positive staining malignant glands confirming adenocarcinoma of intestinal origin and (D) TTF-1 staining demonstrating negative staining glands, excluding a thyroid primary (A to D: X 20).
View Figure 2
She continued follow up with the medical oncologists for further management of her metastatic disease and was enrolled in a chemotherapy drug trial. Three months later, as her thyroid metastatic disease continued to progress, she was taken off this drug and underwent palliative radiotherapy to control the disease. She responded well and has since been enrolled in another clinical drug trial. To date, she continues to remain asymptomatic.
Discussion
Tumor metastases to the thyroid represent a rare entity. Studies have shown that less than 5% of all such metastases become clinically apparent [5]. The Mayo Clinic reviewed nearly ten thousand fine needle aspiration (FNA) biopsies over a 10-year period and reported the incidence of secondary malignancy to the thyroid gland to be approximately 0.5% [6]. Similarly, a large Swiss study that analyzed FNAs over a 12-year period found the prevalence of secondary neoplasms of the thyroid gland to be 0.16% [7].
The thyroid gland has been postulated as an uncommon site for metastases due to several factors [3,8], such as its relatively fast bloodflow, making adhesion and implantation of tumor cells more difficult. Moreover, the high oxygen saturation and high iodine content of thyroid tissue results in an inhibitory effect on tumor cell growth. In colorectal carcinoma, secondary metastases usually occur due to hematogeneous spread via the portal system, making the liver the most common site, followed by the lungs, the bones and the brain [5]. Metastatic spread from a colonic primary to the thyroid gland has thus been hypothesized to occur via a hematogenous route. Indeed, most of the reported cases of colorectal carcinoma metastases to the thyroid had concomitant or pre-existing liver or lung metastases [3].
It has also been suggested that certain patients with pre-existing thyroid disease, in particular follicular neoplasms or multinodular goiter, may have an increased risk of developing metastatic nodules within the thyroid gland [7,8]. This was certainly true for our case, whereby the thyroid metastases was preceded by metastases to the lungs, and occurred in a longstanding goiter.
The time of diagnosis of secondary metastases to the thyroid gland compared to initial diagnosis of the colorectal malignancy has been reported to be highly variable in the literature, ranging from concomitant diagnosis of both a colorectal primary and a thyroid secondary [5], to diagnosis of the secondary metastases up to seven years after initial diagnosis of colorectal carcinoma [3]. An extensive literature search showed that our present case represents the longest interval of eleven years between initial diagnosis of a colon primary and subsequent development of thyroid metastases. Metastases to the thyroid may present as a single nodule, or as multiple foci within the thyroid gland. Many patients commonly present with a solitary thyroid nodule (75%) or with symptoms of airway compression [1,9]. Most patients are euthyroid, although cases of hypothyroidism (secondary to infiltration of thyroid gland by tumor tissue) and hyperthyroidism/thyrotoxicosis (secondary to gland destruction and leakage of stored hormones into the blood stream) have both been reported [9].
Investigation of any suspected secondary thyroid malignancy should include a directed history, clinical examination, thyroid function tests, FNA biopsy and appropriate imaging. It is important to avoid misdiagnosis, as characteristic clinical presentation associated with metastatic tumours is similar to that of primary thyroid cancer.
On ultrasound, thyroid metastases typically appear hypoechoic with ill-defined margins and internal vascularity. Of note, calcifications usually observed in primary thyroid malignancies are not a typical feature of thyroid metastases [1,9,10].
With regard to FNA biopsies, the lack of thyroglobulin, Thyroid Transcription Factor -1 (TTF-1) and calcitonin staining may also suggest a non-thyroid primary, although anaplastic thyroid carcinomas may also exhibit similar behavior. Thus, further stains relevant to the known primary may be required to confirm secondary thyroid metastases on fine needle aspiration [1,9]. Recent studies have also proposed the use of subtypes of anti cytokeratin antibodies CK 20 (which stain specifically for adenocarcinomas of the colon) and CK 7 (which stain for adenocarcinomas of the breast, lung and other glandular tissue) that may be useful in differentiating a primary thyroid carcinoma from a metastatic thyroid carcinoma [10-13]. In our case, the histopathological slides stained positive for CK 20, as well as CDX2, both markers of adenocarcinomas of intestinal origin.
The role of surgery in patients with secondary thyroid metastases has both palliative and curative intent. The former aims to reduce airway and esophageal compression for symptomatic relief, whilst the latter is undertaken avoid further dissemination of the primary carcinoma in selected patients with isolated metastases [9,13]. The decision for surgery should be made bearing in mind the patient's general fitness, stage of disease and presence of compressive symptoms.
The impact of thyroid metastases on eventual prognosis is controversial. Papi et al. compared patients with and without secondary thyroid metastases and found that detection of metastases to thyroid gland does not significantly impact the survival rate, whilst older studies have surmised a poorer prognosis [6,9,14]. A multicentric study by Calzolari et al. also concluded that resection of secondary thyroid metastases does not significantly prolong survival [15]. Long term prognosis seems to be more dependent on the stage of the primary tumor, rather than the presence of secondary thyroid metastases [1,8,16].
In our case, a tracheostomy was performed to relieve the symptoms of airway compression, to allow the patient to consider other therapeutic options for the longstanding lung metastases, which were well controlled thus far after chemotherapy. To date, palliative radiotherapy for disease control of the airway also appears to have good response thus far.
Conclusion
Secondary thyroid metastases from the gastrointestinal tract are extremely rare but are an important consideration for differential diagnosis in patients presenting with thyroid nodules and who have a known primary carcinoma from the colon, regardless of interval between diagnoses. Thorough investigation should be performed with this in mind. The necessary treatment should be instituted to relieve airway compromise, and to decrease tumor burden where appropriate, as the exact impact of thyroid metastases on prognosis is unknown.
Acknowledgements
We would like to acknowledge Khoo Teck Puat Hospital Otolaryngology (ENT) - Head and Neck Surgery department and National University Hospital Medical Oncology department for their support in this case report.
References
-
Goatman C, Goldsmith PJ, Antonopoulos V, Ali B (2012) Metastasis of colorectal adenocarcinoma to the thyroid: a case report and review of the literature. Case Rep Surg 2012: 179407.
-
Chung AY, Tran TB, Brumund KT, Weisman RA, Bouvet M (2012) Metastases to the thyroid: a review of the literature from the last decade. Thyroid 22: 258-268.
-
Kumamoto K, Utsumi Y, Sugano K, Hoshino M, Suzuki S, et al. (2006) Colon carcinoma metastasis to the thyroid gland: report of a case with a review of the literature. Tumori 92: 252-256.
-
Poon D, Toh HC, Sim CS (2004) Two case reports of metastases from colon carcinoma to the thyroid. Ann Acad Med Singapore 33: 100-102.
-
Hanna WC, Ponsky TA, Trachiotis GD, Knoll SM (2006) Colon cancer metastatic to the lung and the thyroid gland. Arch Surg 141: 93-96.
-
Nakhjavani MK, Gharib H, Goellner JR, van Heerden JA (1997) Metastasis to the thyroid gland. A report of 43 cases. Cancer 79: 574-578.
-
Pusztaszeri M, Wang H, Cibas ES, Powers CN, Bongiovanni M, et al. (2015) Fine-needle aspiration biopsy of secondary neoplasms of the thyroid gland: a multi-institutional study of 62 cases. Cancer Cytopathol 123: 19-29.
-
Cherk MH, Moore M, Serpell J, Swain S, Topliss DJ (2008) Metastatic colorectal cancer to a primary thyroid cancer. World J Surg Oncol 6: 122.
-
Papi G, Fadda G, Corsello SM, Corrado S, Rossi ED, et al. (2007) Metastases to the thyroid gland: prevalence, clinicopathological aspects and prognosis: a 10-year experience. Clin Endocrinol (Oxf) 66: 565-571.
-
Yoon JH, Kim EK, Kwak JY, Moon HJ, Kim GR (2014) Sonographic features and ultrasonography-guided fine-needle aspiration of metastases to the thyroid gland. Ultrasonography 33: 40-48.
-
Kim CH, Park YW, Ayala AG, Ro JY (1999) Colonic adenocarcinoma metastatic to the thyroid gland: A case report with immunohistochemical investigation. J Korean Med Sci 14(4):455-459.
-
Phillips JS, Lishman S, Jani P (2005) Colonic carcinoma metastasis to the thyroid: a case of skip metastasis. J Laryngol Otol 119: 834-836.
-
Longo R, Torino F, Sarmiento R, Gattuso D, Bernardi C, et al. (2008) Metachronous thyroid metastasis of primary rectal adenocarcinoma. Cancer Therapy 6: 409-412.
-
Lin JD, Weng HF, Ho YS (1998) Clinical and pathological characteristics of secondary thyroid cancer. Thyroid 8: 149-153.
-
Calzolari F, Sartori PV, Talarico C, Parmeggiani D, Beretta E, et al. (2008) Surgical treatment of intrathyroid metastases: preliminary results of a multicentric study. Anticancer Res 28: 2885-2888.
-
Fujita T, Ogasawara Y, Doihara H, Shimizu N (2004) Rectal adenocarcinoma metastatic to the thyroid gland. Int J Clin Oncol 9: 515-519.





