Journal of Otolaryngology and Rhinology
Radio-clinical Aspects of Laryngocele: About Three Cases
Abou-elfadl M*, Elbousaadani A, Abada RL, Rouadi S, Roubal M and Mahtar M
Otorhinolaryngology and Neck Surgery department, 20 August Hospital, Casablanca, Morocco
*Corresponding author:
Dr. Abou-elfadl Maryame, Otorhinolaryngology and Neck Surgery department, 20 August Hospital, PO Box 9619 Moulay Rchid, Casablanca, Morocco, Tel: +212667932692, E-mail: maryameabouelfadl@gmail.com
J Otolaryngol Rhinol, JOR-2-012, (Volume 2, Issue 1), Case Series
Received: December 08, 2015: Accepted: January 28, 2016: Published: January 30, 2016
Citation: Abou-elfadl M, Elbousaadani A, Abada RL, Rouadi S, Roubal M, et al. (2016) Radio-clinical Aspects of Laryngocele: About Three Cases. J Otolaryngol Rhinol 2:012
Copyright: © 2016 Abou-elfadl M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use,
distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The laryngocele is a dilation of the laryngeal saccule filled with air which communicates with the lumen of the larynx. It is pathology, rare but can be serious. Symptoms are varied and diagnosis is based on direct laryngoscopy and scanner. The treatment is purely surgical. We discussed, through three different cases, the clinical, radiological and therapeutic modalities of laryngocele.
Keywords
Laryngocele, Swelling, Dysphonia, Dyspnea, Laryngoscopy, Scanner, Surgery
Introduction
Laryngocele is a benign dilatation of the laryngeal saccule that may extend internally into the airway or externally through the thyrohyoid membrane. It can be asymptomatic. Laryngoscopy and CT scan are necessary for diagnosis. Surgery is the treatment of choice.
We presented three different cases of about laryngocele and discussed the clinical, radiological and therapeutic modalities of laryngocele.
Materials and Methods
We reported cases of three patients treated for laryngocele in our service during 2 years (2013-2014).
Results and observations
Here we discuss each case individually.
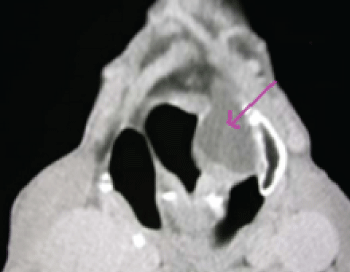
Observation n°1- Pyolaryngocele: A 65 year old male presented to the emergency room, in acute respiratory distress, with a three-mouth history of dysphonia. He was a heavy smoker. After tracheotomy to secure a free airway, physical examination revealed a mobile larynx without neck swelling. He had fever (38.3°C) and analytically had white cell count of 25300 U/mm3 with 83% neutrophil leukocytes and C - reactive protein (CRP) of 27 mg/dl. Computed tomography of neck revealed a mixed laryngocele with collection and air-fluid level at internal cyst causing total airway obstruction (Figure 1). Direct laryngoscopy objectived a bulging of the right ventricular band obstructing laryngeal lumen with a normal aspect of mucosa in favor of a laryngocee. A diagnosis of laryngopyocele was confirmed.
The laryngopyocele was drained and a large amount of purulent material was removed and cultures were collected. The patient was treated with intravenous antibiotics, including, Amoxicillin-Clavulanic acid, Metronidazole, Gentamycin and corticotherapy (methylprednisolone). Culture revealed the presence of Pseudomonas aeruginosa. Resection of the laryngocele was performed by the external lateral cervical approach. Post-operative recovery was uneventful with decannulation and closing the tracheostoma. Histology was in favor of laryngocele and no evidence of malignancy.
.
Figure 1: Computed tomography of neck revealing a mixed laryngocele with collection and air-fluid level at internal cyst causing total airway obstruction.
View Figure 1
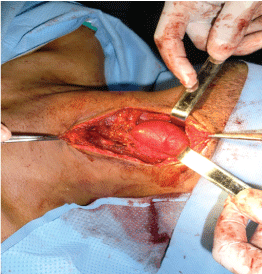
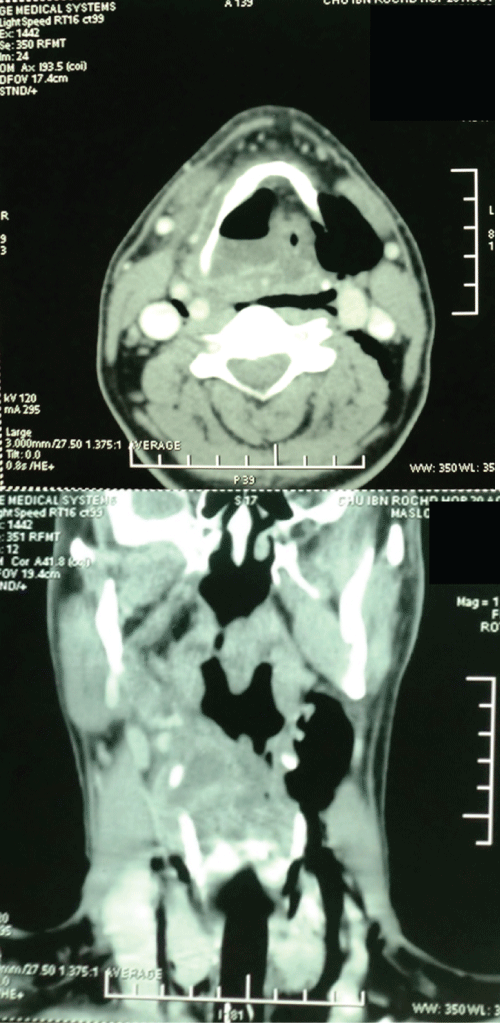
Observation n°2- Mixed laryngocele: A 23-year-old male with 5 years of hoarseness, complicated by dyspnea on exertion one month ago. He do not had any disease. Clinical examination revealed a painless soft mass at the left side of the neck, about 5 cm in size, conducting vibration during speech, manually reducible and covered with normal skin. Fibrolaryngoscopy showed a supraglottic mass covered with normal mucosa, extending into airways from the left wall of hypopharynx. A computed tomography (CT) scan showed a large mixed internal and external laryngocele without regional lymphadenopathy (Figure 2). Resection of the laryngocele was performed by the external lateral cervical approach (Figure 3). Post-operative recovery was uneventful. The final histological diagnosis of the specimen was laryngocele.
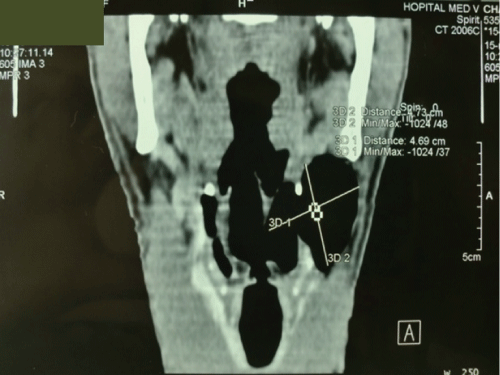
.
Figure 2: A computed tomography (CT) scan showed a large mixed internal and external laryngocele.
View Figure 2
Observation n°3- Internal pyolaryngocele: A 10-year-old male presented to our hospital with a short duration of hoarseness, odynophagia, and dyspnea for two weeks. He had no past medical history. Physical examination revealed a mobile larynx without neck swelling and no fever. Indirect laryngoscopy showed a sub-mucosal mass in the region of the left false cords and aryepigottic folds. CT scan of the neck showed an abscess of the left ventricular band (Figure 4). The patient received a medical treatment and resection of the laryngocele after few days by a lateral thyrotomy. Histological exam confirmed the laryngocele.
Discussion
A laryngocele is an abnormal saccular dilatation of the appendix of the laryngeal ventricle of Morgagni, which maintains its communication with the laryngeal lumen [1]. The incidence of laryngocele is estimated to be one per 2.5 million of the population per year [2-4]. It have been reported to be five times more frequent in men, with a peak incidence in the sixth decade of life [2,4]. Children can also be affected by this benign pathology as our reported cases.
The precise aetiology of laryngocele is unknown [2]. Many authors have hypothesized that congenital or acquired factors may be responsible. It is believed that laryngoceles occur in subjects with congenitally dilated saccule [2,3]. A less important role is played by the narrowness of the periventricular connective tissue and the weakening of the thyroaryepiglottic muscles a congenital weakness or defect predisposes to the formation of laryngoceles under the influence of acquired factors that increase intra-glottic pressure such as professional trumpet playing, glass blowing, singing, straining at passing of stools, weight lifting and carcinoma of the larynx are considered to promote the development of laryngoceles [2,3,5,6].
Laryngoceles can be internal, external, or mixed [2]. A review of the English literature showed that the most common type is the mixed laryngocele (44%), 30% were internal and 26% were external [2]. Bilateral laryngoceles were found in 23% [6]. An association of laryngoceles with squamous cell carcinoma of the larynx has been well established, necessitating a high index of suspicion for malignancy when present. Celin et al. reported an incidence of laryngoceles concurrent with squamous cell carcinoma of the larynx of 4.9-28.8% [7].
When the connection between the laryngocele and the laryngeal lumen becomes occluded, as a result of inflammation, infection, and tumors, mucus can accumulate, and a mucocele can develop. A secondarily infected mucocele is called a laryngopyocele [3].
A total of 39 cases of laryngopyocele have been reported in the world literature, only in 4 of these cases had a laryngopyocele causing acute airway obstruction and only one case of internal laryngopyocele causing acute airway obstruction has been reported until now [2,8,9].
Symptoms of laryngoceles depend on the subtype [3]. They are usually asymptomatic [2]. The most frequent presenting symptom is hoarseness. Variable degrees of dyspnoea, dysphagia, cough and stridor may be present, depending on the dimension of the laryngocele. Laryngopyocele may present with signs of rapidly progressive respiratory obstruction and/or an infected painful neck mass which may rapidly increase in size. They must be included in the differential diagnosis of hoarseness and odynoaphagia with a lateral neck mass [9,10].
The endoscopic examination and direct laryngoscopy reveal a false vocal fold and arytenoid swelling overlied with normal laryngeal mucosa. It should be noted that all the patients with symptoms of airway problems should at least go through an upper airway endoscopic evaluation to rule out upper airway obstruction.
On CT scanning, a laryngocele appears as a well-defined lesion arising beneath the false vocal cords and communicating with the laryngeal airway. The thyrohyoid membrane will limit internal laryngoceles, while the combined and external laryngoceles will lie superficial to the thyrohyoid membrane at the point of insertion of the superior laryngeal nerve and vessels. Air filled laryngoceles are easily identified on CT due to low CT density. Alternately, a fluid-filled external laryngocele may mimic the appearance of a branchial cleft cyst, or pharyngocele, only to be differentiated based on location and absence of digestive signs (food blockage, dysphagia).
Laryngopyocele demonstrate a thick enhancing wall, surrounding the laryngocele on contrast-enhanced CT. Magnetic resonance imaging is recommended for distinguishing laryngoceles from an underlying laryngeal neoplasm when fluid or debris are present within the dilated cavity [8,9].
Histologic findings may show a cyst lined by a variety cell types. Respiratory type epithelium is the most common although areas of oncocytic epithelium as well as squamous epithelium may be present as a result of metaplastic change [8]. A fibrous connective tissue wall containing mucous or seromucous glands are also typically observed. Squamous epithelium may become the predominant epithelial lining in the presence of infection, with an associated chronic inflammatory cell infiltrate scattered within the fibrous connective tissue, and in the case of a laryngopyocele, abundant neutrophils located within the connective tissue and adhering to the cystic epithelium [8] The most common bacteria isolated from laryngopyocele are Escherichia coli, Haemolytic streptococcus B, Staphylococcus aureus and Pseudomonas aeruginosa [2].
Excision of the laryngocele can be performed by endoscopic, external or combined approach. The choice of the approach depends on the type and size of the laryngocele. Treatment of the mixed laryngocele is still controversial. Several authors prefer an external approach. Most of the patients with combined laryngoceles (86.2%) were treated using an external approach. The reported advantages of external approaches are good exposure of the laryngocele, a more precise procedure and a low recurrence rate. Disadvantages are skin scarring, higher morbidity, longer duration of surgery, longer hospitalization period, and higher costs [4]. Three types of external procedures have been used during the past 20 years; the transthyrohyoid membrane approach, thyrotomy with resection of the upper 1/3 of the thyroid cartilage, and V-shaped thyrotomy. The transthyrohyoid membrane approach was the one most often used, in 68% of the cases treated using external techniques. The advantage of this procedure when compared with the other two is that no resection of the thyroid cartilage is done. The disadvantage is limited exposure of the paraglottic space. Thyrotomy with resection of the upper 1/3 of the thyroid cartilage and V-shaped thyrotomy were used in a minority of patients. The first endolaryngeal resection of a combined laryngocele using robotic surgery was reported in 2013 [4]. According to the authors, this technique seems to have several advantages when compared with microlaryngoscopy. For instance, optics are placed in the oral cavity, thus allowing closer, angulated vision of the surgical field. In addition, rather than using traditional laryngoscopes, instruments are introduced through mouth gags, which offer a wider view and range of motion.
Resection small internal laryngoceles can be performed utilizing a CO2 laser following protection of the false vocal fold ipsilateral to the laryngocele. Following an incision to the superior surface of the false vocal fold, the limits of the laryngocele are identified and the laser is used to dissect the lesion from the surrounding paraglottic tissue [5,8]. On the other hand, the endolaryngeal management of laryngoceles has the disadvantages of providing limited surgical exposure, causing endolaryngeal scarring and requiring experience with special instruments. Furthermore, the probability of incomplete resection of large laryngoceles limits the use of the endoscopic approach. However, the last seems not to be of clinical significance, since no recurrence has been reported to date following the use of endolaryngeal techniques [4].
In the case of pyolaryngocele, aggressive antibiotic therapy, analgesia, and aspiration of the purulent content can avert the need for an emergency tracheostomy [10,11].
Conclusion
Laryngopyocele can sometimes be revealed by an episode of acute respiratory distress requiring tracheotomy. If there is no respiratory distress and if the infection is cured, endoscopic treatment with or without laser can be performed for internal laryngocele. The cervical approach is recommended for external or combined laryngocele.
Conflict of Interests
The authors declare that there is no actual or potential conflict of interest in relation to this paper. No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this paper.
References
-
Prasad N, Singh M, Nagori R, Singh S (2015) Laryngopyocele: Presenting with pressure symptom. Int J Appl Basic Med Res 5: 228-230.
-
Vasileiadis I, Kapetanakis S, Petousis A, Stavrianaki A, Fiska A, et al. (2012) Internal laryngopyocele as a cause of acute airway obstruction: an extremely rare case and review of the literature. Acta Otorhinolaryngol Ital 32: 58-62.
-
Andreou Z, Randhawa PS, O'Flynn P, Vaz FM (2011) Endoscopic Management of an Internal Laryngopyocele Presenting with Acute Airway Obstruction. Case Reports in Surgery.
-
Zelenik K, Stanikova L, Smatanova K, Cerny M, Kominek P (2014) Treatment of Laryngoceles: what is the progress over the last two decades? Biomed Res Int 2014: 819453.
-
Lancella A, Abbate G, Dosdegani R (2007) Mixed laryngocele: a case report and review of the literature. Acta Otorhinolaryngol Ital 27: 255-257.
-
Prasad KC, Vijayalakshmi S, Prasad SC (2008) Laryngoceles - presentations and management. Indian J Otolaryngol Head Neck Surg 60: 303-308.
-
Celin SE, Johnson J, Curtin H, Barnes L (1991) The association of laryngoceles with squamous cell carcinoma of the larynx. Laryngoscope 101: 529-536.
-
Werner RL, Schroeder JW, Castle JT (2014) Bilateral laryngoceles. Head Neck Pathol 8: 110-113.
-
Aksoy EA, Elsurer C, Serin GM, Unal OF (2013) Bilateral internal laryngoceles mimicking asthma. J Res Med Sci 18: 453-456.
-
Gafton AR, Cohen SM, Eastwood JD, Dang MK, Hoang JK (2013) Recurrent laryngopyocele: CT-guided hookwire localization for re-excision surgery. AJNR Am J Neuroradiol 34: E39-42.
-
Felix JA, Felix F, Mello LF (2008) Laryngocele: a cause of upper airway obstruction. Braz J Otorhinolaryngol 74: 143-146.