Journal of Otolaryngology and Rhinology
Endoscopic Transcanal Cartilage Myringoplasty for Repair of Subtotal Tympanic Membrane Perforation: A Method to Avoid Postauricular Incision
Khaled M Mokbel*, Waleed Moneir, Hossam Elsisi and Ahmed Alsobky
Department of ORL, Head and Neck surgery, Mansoura University, Mansoura, Egypt
*Corresponding author:
Khaled M Mokbel, MD, Professor ORL, Department of ORL, Head and Neck surgery, Mansoura University, Mansoura, Egypt, E-mail: ootology@yahoo.com, khmokbel@gmail.com
J Otolaryngol Rhinol,
JOR-1-010, (Volume 1, Issue 2),
Original Article
Received: November 20, 2015: Accepted: December 24, 2015: Published: December 28, 2015
Citation: Mokbel KM, Moneir W, Elsisi H, Alsobky A (2015) Endoscopic Transcanal Cartilage Myringoplasty for Repair of Subtotal Tympanic Membrane Perforation: A Method to Avoid Postauricular Incision. J Otolaryngol Rhinol 1:010
Copyright: © 2015 Mokbel KM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Our aim is to evaluate transcanal endoscopic approach in repair of subtotal tympanic membrane perforation in a trial to prevent conventional postaural approach. Our study was done in 80 patients with unilateral dry subtotal tympanic perforations. They were 44 males and 36 females. Their ages ranged from 18-50 years with mean of 33 years. Autograft thin (0.2 mm) auricular cartilage shield was used to repair tympanic membrane perforation. Patients were divided into two groups according to the approach. Group "A" was approached by endoscopic transcanal myringoplasty while in group "B" by microscopic postauricular myringoplasty. The least follow up period was 6 months with range from 6 to 24 months. The take rate was significantly high in group A (100% in A and 90% in B). Postoperative air bone gap was significantly improved in both groups especially in group "A". There was significant difference (P value < 0.0001) between the postoperative air bone gap averages of both groups (8.50 ± 1.25 in A and 9.25 ± 0.75 in B). We concluded that subtotal perforation of the tympanic membrane is better to be repaired by transcanal endoscopic myringoplasty to avoid the postaural method and to gain more precised result with better hearing.
Keywords
Subtotal perforation, Endoscopic myringoplasty, Cartilage graft, Postauricular approach
Introduction
Tympanoplasty is one of the commonest operations performed on the middle ear. Traditionally over many years, tympanoplasty has been done using the operating microscope with its optical limitations which have remained the same over the last three decades despite the continuous technical advancements [1]. Till the last decade endoscopes had been mainly used for diagnosis and photography. Recently some authors encouraged to use the endoscope in different middle ear surgeries either alone or in assistance of the microscope [2]. Few papers have been published describing the use of the endoscope in repair of small tympanic membrane perforation by different graft materials but we did not find papers describing the use of the endoscope in repair of total and subtotal perforations. Traditionally microscopic repair of such types of perforation has been done through a postauricular incision in order to obtain wide exposure [3]. Cartilage graft is widely used and strongly established to be beneficial in obtaining good take rate in myringoplasty. Cartilage graft is rigid with more durability and resistance so it is preferred in repair of large tympanic membrane perforations [4].
Materials and Methods
After getting approval of the institutional ethical committee and written consent from all enrolled patients, this study was conducted on 80 patients with unilateral dry subtotal tympanic membrane perforation repaired by an ultrathin auricular cartilage shield graft covered by temporalis fascia where it is the preferred graft of the senior first author [4]. They included 36 females and 44 males. Their ages range from 18-50 years with mean of 33 years. Patients in our study were selected from the Otologic Outpatient Department of Mansoura University Hospital from January 2011- February 2014. Complete Oto-endoscopic examination was performed for all patients. Preoperative audiological investigations were completed for all patients in the form of pure tone audiometry (air conduction and bone conduction thresholds at frequencies from 500-4000 Hz and air bone gap (ABG). Patients were divided blindly into 2 groups. The patient and the surgeon were unaware of which group, endoscopic or microscopic, the patient was in. The patients were numbered from 1 to 80. Patient no. 1 was assigned for group A and patient no. 2 assigned for group B and so on.
All patients were fulfilled all the inclusion criteria which included; dry perforation for 3 months or more, no evidence of ossicular disease with air bone gap (ABG) of ≤ 35 dB, no previous ear surgery, no sinonasal problems and medical fitness with no diabetes mellitus. Group A included 40 patients operated by the endoscopic transcanal approach and group B included another 40 patients repaired by microscopic postauricular approach. In both groups we used the underlay/overlay technique placing the graft under the annulus and remnants of tympanic membrane but over the malleus handle. Follow up was ranged from 6 to 24 months. Data were evaluated using online GraphPad software where mean and standard deviation were calculated and unpaired t test was used to compare between two mean to calculate P value.
Surgical Steps in the Endoscopic Group A
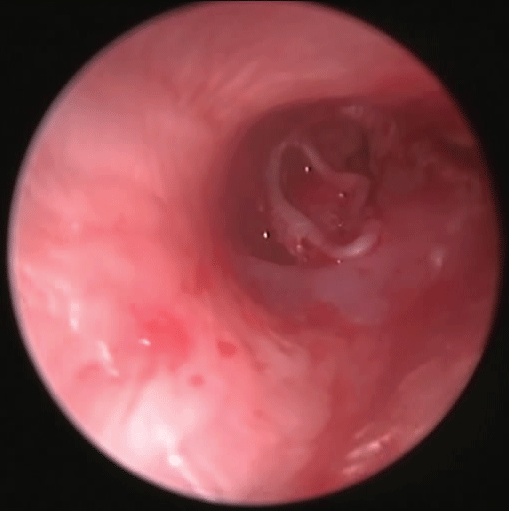
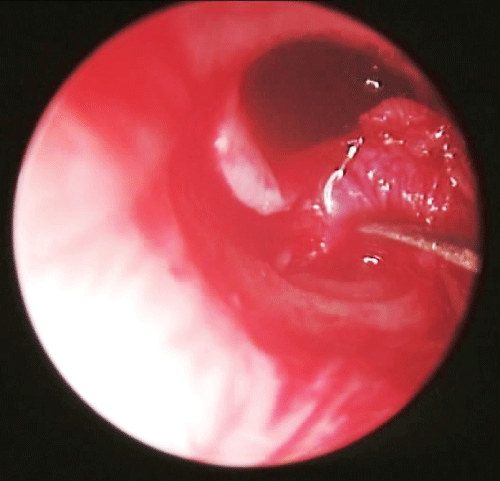
All cases were operated under local anesthesia with xylocaine 2% in 1/50000 epinephrine. Injections were done in 4 points at the external canal meatus and 4 points inside the canal at the cartilage- bony junction. A wide angle Storz Otoendoscope "0" degree (2.7 mm diameter) connected to storz camera and a led light source of 150 W were used. The camera was connected to a TV screen with a video recording system. The patient was draped with towels with a bowl containing an antifogging solution to clean the tip of the endoscope. The external canal was cleaned with saline after local anesthesia injection. The endoscope was introduced through the canal to examine the perforation and insinuated in the middle ear to visualize its cavity as well as ossicles. In all steps the instruments were introduced just before the entry of the endoscope to allow visualization of the instrument. The endoscope was removed then a sickle knife was just introduced before the endoscope to cut the edges of the perforation. The edge of the perforation was everted and visualized by the endoscope for any epithelial remnants to ensure complete removal of epithelium. The disc knife was used to make a circumferential incision just medial to the cartilage/bony junction.
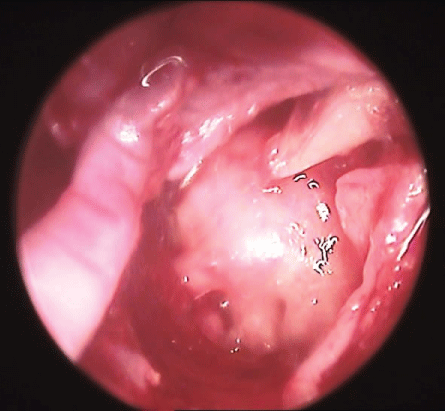
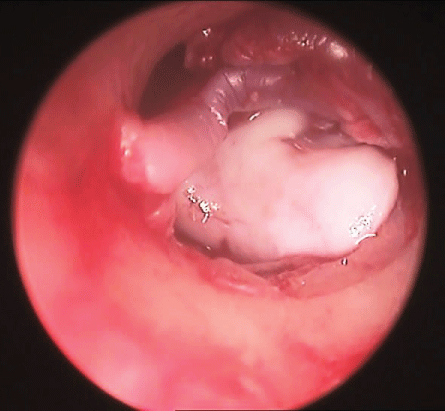
The incision was taken from 1-6 o'clock (right ear) and from 11-6 o'clock (left ear), to obtain a wide skin flap. By using a dissector the flap was elevated till reaching the annulus. By scissors the flap was cut superiorly and inferiorly to facilitate its anterior reflection. The handle of malleus should be cleaned of any attached tissues, make clear that also the mucosa by crocodile forceps and a needle. The cartilage graft was taken by a separate incision in the medial aspect of the auricular scapha after its infiltration with the local anesthesia. An oval piece of cartilage without perichondrium on either side was excised. The cartilage was thinned to 0.2 mm [4] by a special instrument called Conchotome (Kurz Co. Germany). A wedge was excised from the cartilage to adapt the handle of malleus. Gel foam pieces were placed in the middle ear and the graft was placed. A piece of dried temporalis fascia was prepared from the ipsilateral temporalis muscle by a separate incision. The fascia was placed on the cartilage shield and laid on the posterior bonny wall of the external canal. The endoscope was used to precisely and carefully place the graft under the edge of the perforation circumferentially. The posterior skin flap, annulus and remnants of the tympanic membrane were returned back on the posterior wall, Gel foam pieces were place in the external canal and gauze pack with antibiotic ointment. The temporal incision was closed in 2 layers with interrupted sutures by Vicryl 4/0 for the inner layer and Silk 4/0 for skin. The auricular incision was closed in one layer of interrupted sutures by Vicryl 4/0.
Steps in Microscopic Group B
All cases were operated with the same anaethesia as group A. The microscope was used as a sole optical tool for all cases. The vascular strip was created through postauricular approach following the basic steps of tympanoplasty creating a laterally based flap. The perforation was repaired by a thin cartilage graft (0.2 mm) harvested as previously described in group A. A piece of temporalis fascia was harvested from ipsilateral temporalis muscle through the same postauricular incision. Canaloplasty was accomplished for cases with bony humps which have been found to obscure the microscopic view. The postauricular incision was closed by interrupted sutures using Vicryl 4/0 for subcutaneous layer and Silk 2/0 for the skin.
Follow Up in Both Groups
A systemic antibiotic was used for one week after surgery. The pack was removed after one week and the gel foam after 10 days. An antibiotic/steroid drops was prescribed for 2 weeks. All patients were followed once/2 weeks in the first 3 months then once/monthly in the first and second years. The first pure tone audiometry was done after 3 months for all cases. All cases were examined in each follow up session by the endoscope for graft take.
Results
Our study included 80 patients (36 females and 44 males) with mean of 33 years (Table 1). All cases had unilateral dry subtotal tympanic membrane perforation. Patients in group A were repaired by transcanal endoscopic cartilage myringoplasty and in group B by microscopic postauricular myringoplasty. Both groups were repaired with autologous thin (0.2 mm) cartilage shield covered with temporalis fascia. The minimum follow up period was 6 months.
![]()
Table 1: Shows number, sex and age of cases.
View Table 1
![]()
Table 2: Shows numbers of bony humps in both groups.
View Table 2
In group A, external canal bony humps were found in 7 cases (Table 2) for whom we did not perform canaloplasty because the endoscope could be passed beyond these humps without obscuring the view. The average time of surgery was 40 ± 5.50 minutes (Table 3). The graft was taken completely in all cases without any residual perforations (Table 3). The hearing was improved in all cases of this group. The mean of preoperative ABG average was 32.50 ± 1.50 and became 8.50 ± 1.25 postoperatively. Most cases in this group showed significant improvement of ABG as 85% had ABG ≤ 10 dB (Table 4).
![]()
Table 3: Time of surgery and take rate.
View Table 3
![]()
Table 4: Air bone gap (ABG) average and groups
View Table 4
In group B, there were 6 cases with bony humps obscuring the microscopic view that necessitating drilling to open the field (Table 2). The average time of surgery in this group was 55 ± 10.50 minutes. The graft was taken in 90% of cases where 10% (4 cases) failed (Table 3).
Unpaired t test was used to calculate P value. Statistical significant difference (P < 0.0001) was noticed between the preoperative and postoperative average means ABG of the two groups. The mean of preoperative ABG average was 30.75 ± 1.25 and became 9.25 ± 0.75 postoperatively. Most of cases of group A showed closure of ABG in the category ≤ 10 dB with high significant difference in comparison to that of the group B. There was none significant difference between the postoperative ABG averages of both groups (Table 4).
In the term of take rate there was significantly higher in group A, where it was 100% in A and 90% in B.
Discussion
By using the operative microscope, the postauricular approach is the commonly used method to repair the subtotal tympanic membrane perforation [5]. Postauricular incision leads to more blood loss, long time, disturbance of the anatomy of the postauricular region with scar or even keloid formation [6]. The microscope is relatively heavy so it is not easy to move and take longer time to be adjusted. The optics of the microscope is based on that it looks in one line so it frequently needs change of the position of either the head of the patient or the microscope to obtain a good view [2,6]. Another problem in the optics of the microscope is that it can't visualize many areas of the middle ear in one view. On the other hand the endoscope has the ability to visualize many structures of the middle ear in one frame [7,8]. Moreover the surgeon can move the endoscope up, down, front and back more easily to visualize different points and regions inside the middle ear cavity. The work by looking to the monitor is another issue of endoscopic advantage, where it gives more magnification and precision of the work. The work through the monitor gives a very important advantage of following the steps of surgery by young surgeons and students so increasing the teaching and learning processes. In group A of our study we used the otoendoscope in all steps of myringoplasty without the need of operating microscope. The surgeon (1st author) held the endoscope/camera by his left hand and the instrument by his right hand. The surgeon didn't mentioned left hand fatigue or any discomfort. A very important trick is that the instrument should little precede the endoscope to allow visualization of its working tip. Frequent cleaning of the lens of the endoscope sometimes seems to be disappointing but it could be solved by avoiding touch the tip of the endoscope to the tissue or instruments. We found that the work through the TV monitor was more convenient than the work through the eye piece of the endoscope. Moreover it gives more magnification and more precised surgery. The magnification could be changed by adjusting the distance between the tip of the endoscope and the working field; it increases when the distance decreased. Many papers restrict the use of the endoscope to repair cases of small tympanic membrane perforations but in this study we used the endoscope in repair of large perforations as subtotal with very good anatomical and functional results. Variations of the external auditory canal like tortuosity, stenosis and bony humps make the view of the tympanic membrane difficult when visualized through the microscope [8-10]. Transcanal operative endoscopy bypasses the narrow segment of the ear canal and provides a wide view even when a zero endoscope is used [3,8]. By the use of the endoscope we did not need to do canaloplasty in cases with humps because the endoscope could be passed beyond the humps but we found difficulties in passing the instruments through narrow parts but we could complete the procedure with no need for canaloplasty. In our opinion curved instruments are important in such cases with humps. Inspection of the medial aspect of the perforation edge and carful removal of the epithelial debris is an important step in technique of myringoplasty [9-11]. We observed that by the use of the endoscope it was easy to inspect and evert the edge of the tympanic membrane with careful removal of epithelial remnants. We didn't notice difficulties in using one hand to complete the procedure. Recently Mobarak and Sapna [12] reported the concept and development of innovative endoscopic holder system for endoscopic otolaryngologic surgeries. On the other hand in group B where we used the postauricular incision we noticed that it was more time consuming in skin incision, tissue elevation and haemostasis. In this group we found 6 cases with bony humps that need drilling to widen the field of vision. The take rate in microscopic group was 90% whereas in endoscopic group was 100%. Postoperative infection was another issue of disadvantage of postauricular approach which has occurred in three cases. Finally we recommend avoiding postauricular incision in repair of tympanic membrane perforations even if large; instead we strongly advise to use the endoscopic approach to avoid the disadvantages of the postauricular approach also to increase the take rate because it is more precised technique.
Conflict of Interests
The authors declare that they have no conflict of interest with no financial relationship with any organization.
References
-
Rosenberg SI, Silverstein H, Willcox TO, Gordon MA (1994) Endoscopy in otology and neurotology. Am J Otol 15: 168-172.
-
Tarabichi M (1999) Endoscopic middle ear surgery. Ann Otol Rhinol Laryngol 108: 39-46.
-
Usami S, Iijima N, Fujita S, Takumi Y (2001) Endoscopic-assisted myringoplasty. ORL J Otorhinolaryngol Relat Spec 63: 287-290.
-
Mokbel KM, Thabet EM (2013) Repair of subtotal tympanic membrane perforation by ultrathin cartilage shield: evaluation of take rate and hearing results. Eur Arch Otorhinolaryngology 270: 33-36.
-
Glasscock, Shambaugh (2003) Tympanoplasty. In: Glasscock, Shambaugh Surgery of the ear. (5th edition) 24: 463-86.
-
Karhuketo TS, IIomaki JH, Puhakka HJ (2001) Tympanoscope assisted myringoplasty. ORL 63: 353-358.
-
Mohindra S, Panda NK (2010) Ear surgery without microscope; is it possible. Indian J Otolaryngol Head Neck Surg 62: 138-141.
-
Kakehata S, Futai K, Sakaki A, Shinkawa H (2006) Endoscopic transtympanic tympanoplasty in the treatment of conductive hearing loss: early results. Otol Neurotol 27:14-19.
-
Tarabichi M (2012) Principles of endoscopic ear surgery. ENT and Audiology News 21: 42-44.
-
Kozin ED, Gulati S, Kaplan AB, Lehmann AE, Remenschneider AK, et al. (2015) Systematic review of outcomes following observational and operative endoscopic middle ear surgery. Laryngoscope 125: 1205-1214.
-
Karchier E, Morawski K, Bartoszewicz R, Niemczyk K (2012) Application of the endoscopy in the middle ear surgery. Otolaryngol Pol 66: 191-195.
-
Khan MM, Parab SR (2015) Concept, Design and Development of Innovative Endoscope Holder System for Endoscopic Otolaryngological Surgeries. Indian J Otolaryngol Head Neck Surg 67: 113-119.