Journal of Otolaryngology and Rhinology
Nasal Glomangiopericytoma: Case Report and Clinicohistopathologic Overview
Sheldon P. Hersh, MD1* and William H. Rodgers, MD, PhD2
1Department of Otolaryngology, Lenox Hill Hospital, New York, USA
2Department of Pathology, New York Hospital Queens, New York, USA
*Corresponding author:
Sheldon P. Hersh, MD, 110-11 72nd Ave. Suite 1B, Forest Hills, New York, 11375, USA, Tel: 718 2619000, Fax: 718 2680504, E-mail: sphersh@aol.com
J Otolaryngol Rhinol,
JOR-1-007, (Volume 1, Issue 1),
Case report
Received: August 11, 2015: Accepted: September 23, 2015: Published: September 25, 2015
Citation: Hersh SP, Rodgers WH (2015) Nasal Glomangiopericytoma: Case Report and Clinicohistopathologic Overview. J Otolaryngol Rhinol 1:007
Copyright: © 2015 Hersh SP. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Glomangiopericytoma, also known as sinonasal hemangiopericytoma, is a rare sinonasal neoplasm that commonly occurs during the sixth or seventh decade of life, often presenting with complaints of nasal congestion and epistaxis. Identified in less than 0.5% of all sinonasal tumors, this typically indolent lesion is a different tumor from the far more common and aggressive so-called soft tissue hemangiopericytoma that arises in varying sites throughout the body. Sinonasal hemangiopericytoma often presents as a polypoid mass with highly distinctive histopathologic features. Treatment, in most instances, requires that local excision with adequate margins be performed in concert with monitored follow-up examinations to guard against the distinct possibility of recurrence.
Introduction
Originating from perivascular modified smooth muscle cells; sinonasal glomangiopericytoma is a rare vascular neoplasm that may take on the macroscopic appearance of common inflammatory polyps. Distinctive histopathologic and immunohistochemical features serve to differentiate nasal glomangiopericytomas from soft tissue hemangiopericytomas arising at unrelated sites as well as other nasal tumors that may possess overlapping histologic components. A case report follows describing the endoscopic excision of an isolated polypoid nasal mass in a patient who presented with a three year history of unilateral nasal congestion and intermittent epistaxis.
Case Report
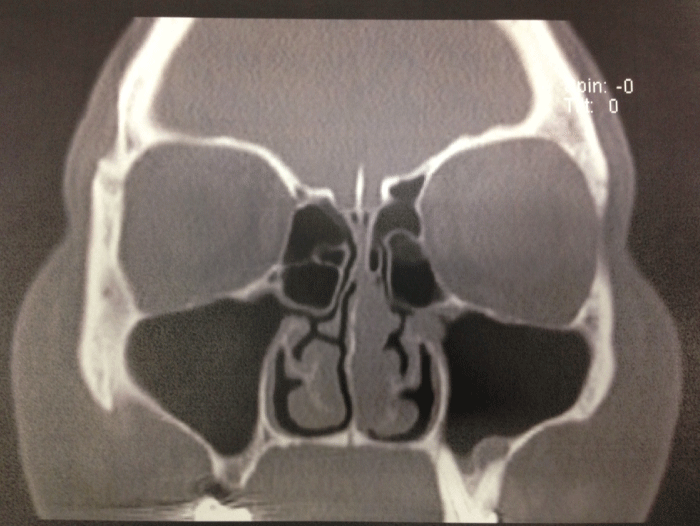
A 41 year old female presented with a three year history of left nasal congestion interspersed with occasional episodes of self-limiting left epistaxis. Her medical history was notable for hypertension and perennial allergies (dust mites and mold). She denied any prior history of smoking, nasal trauma or previous sinonasal surgery. Routine and endoscopic examination of the nose revealed an erythematous polypoid lesion within the left nasal cavity that originated from the superior most aspect of the nasal septum. No other nasal pathology was appreciated. CT imaging of the paranasal sinuses (Figure 1) revealed a 2.3 × 2.2 soft tissue mass along the left side of the nasal septum without evidence of related destructive change. Uneventful endoscopic excision of the lesion soon followed.
.
Figure 1: Coronal CT image demonstrating a polypoid soft tissue mass which seems to arise from medial wall of the left nasal cavity and partially obstructing the superior and mid nasal cavity.
View Figure 1
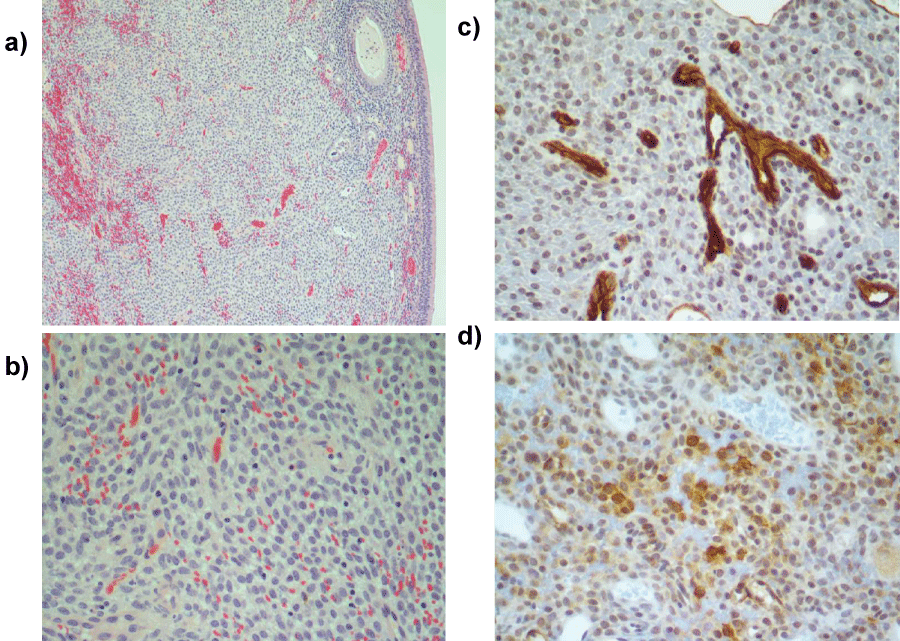
Histopathology of the resected tumor (Figure 2) reveals a submucosal nodular proliferation of slightly eosinophyllic spindle shaped cells with ovoid nuclei and with minimal cytologic atypia. Rare normal mitotic figures are present. Tumor cells are arranged in fascicles with an associated vascular component consisting of irregular capillary channels including "stag-horn" configured blood vessels. The immunohistochemical profile (muscle actin HHF35 positivity, figure 2) supported myoid differentiation typical of pericytes.
.
Figure 2(a-d): Representative photomicrographs demonstrate the submucosal proliferation of "Myoid appearing" ovoid to spindle shaped cells arranged in fascicles (2a, 100×; 2b, 400× H and E) with irregular vascular channels including "stag-horn" blood vessels (2c, 400× CD-34 immunohistochemistry). The ovoid spindle-shaped cells are focally reactive for muscle actin (2d, 400× HHF35 immunohistochemistry). Ovoid spindle cells are non-reactive for smooth muscle actin, CD31, CD-117, and are reactive for vimentin (not shown). Vascular spaces are also immunoreactive for CD-31 (not shown).
View Figure 2(a-d)
Discussion
Sinonasal glomangiopericytoma (SNGPC), also known as sinonasal hemangiopericytoma (SNHPC), is a rare neoplasm now recognized as originating from perivascular modified smooth muscle cells (pericytes) [1]. This tumor should be distinguished from those soft tissue tumors with histologic features originally defined by Stout and Murray as hemangiopericytoma (HPC) [2,3]. Tumors typically classified as hemangiopericytoma lack the immunohistochemical and electron microscopic features of myoid differentiation typical of pericytes. Marked differences in clinicopathologic findings [4-6] between so called soft tissue hemangiopericytomas and those in the sinonasal tract resulted in use of the term sinonasal-type hemangiopericytoma whenever these lesions happen to present in the nasal cavity or paranasal sinuses.
Granter et al. [7] refer to an assemblage of neoplasms that display perivascular myoid differentiation and other distinctive overlapping features as a spectrum or continuum of related tumors. The constituent entities comprising this spectrum of tumors are not only interconnected but at times may prove to be indistinguishable from one another. Amongst the tumors studied, a distinctive group with features that fall in between that of a glomus tumor and classic HPC was given the name glomangiopericytoma. Glomus bodies are comprised of arteriovenous anastomoses surrounded by glomus cells that serve as specialized thermoregulatory. In 2005, the World Health Organization identified GPC as a unique sinonasal low malignancy tumor that demonstrates a perivascular myoid phenotype [8].
Most cases of SNGPC occur within the nasal cavity with notably fewer reported cases presenting in the paranasal sinuses and nasopharynx [9]. While nasal congestion and epistaxis are, by and large, the most common symptoms, other complaints including pain, headache, visual disturbance, serous otitis media, proptosis, and infraorbital anesthesia have been described [9,10]. A number of other sinonasal vascular lesions with overlapping histologic features that may be mistaken for a glomangiopericytoma include lobular capillary hemangioma, solitary fibrous tumor, leiomyoma and angiofibroma [11]. Hypertension, trauma, extended steroid use and pregnancy have all been identified as potential precipitating conditions [11,12].
Macroscopically, GPC lesions often closely resemble inflammatory polyps. Duval et al. [13] are of the opinion that these lesions should be biopsied preoperatively so as to avoid misdiagnosis, incomplete excision and the possibility of recurrence. Although often discovered in a predominantly middle-aged group [4], SNGPC may occur at any age [9,13]. Imaging studies, though typically non-specific, are useful in ascertaining location, tumor size and may occasionally reveal evidence of an aggressive/ invasive pattern of dissemination [14,15].
Treatment involving wide excision with clear margins is commonly curative [9]; however recurrences have been discovered in 7%-40% of cases and are likely a consequence of incomplete surgical resection [16]. Although GPC is typically categorized as a benign neoplasm, isolated cases of local invasion, regional destruction and metastatic spread have been reported [13]. Thiringer et al. [5] underscore the significance of location when assessing the biologic aggressiveness of these neoplasms. GPC involving the sinonasal tract takes on a more benign course when compared to that of other sites. Long term follow- up has been strongly advocated in light of the possibility of recurrences occurring decades following initial identification and treatment [5,13].
References
-
Thompson LD (2004) Sinonasal tract glomangiopericytoma (hemangiopericytoma). Ear Nose Throat J 83: 807.
-
Stout AP, Murray MR (1942) Hemangiopericytoma: a vascular tumor featuring zimmermann's pericytes. Ann Surg 116: 26-33.
-
Watanabe K, Saito A, Suzuki M, Yamanobe S, Suzuki T (2001) True hemangiopericytoma of the nasal cavity. Arch Pathol Lab Med 125: 686-690.
-
Compagno J (1978) Hemangiopericytoma-like tumors of the nasal cavity: a comparison with hemangiopericytoma of soft tissues. Laryngoscope 88: 460-469.
-
Thiringer JK, Costantino PD, Houston G (1995) Sinonasal hemangiopericytoma: case report and literature review. Skull Base Surg 5: 185-190.
-
Thompson LD, Miettinen M, Wenig BM (2003) Sinonasal-type hemangiopericytoma: a clinicopathologic and immunophenotypic analysis of 104 cases showing perivascular myoid differentiation. Am J Surg Pathol 27: 737-749.
-
Granter SR, Badizadegan K, Fletcher CD (1998) Myofibromatosis in adults, glomangiopericytoma, and myopericytoma: a spectrum of tumors showing perivascular myoid differentiation. Am J Surg Pathol 22: 513-525.
-
Thompson LDR, Fanburg-Smith JC, Wenig BM (2005) Borderline and low malignant potential tumours of soft tissues. In: Barnes L, Eveson JW, Reichart P, Sidransky D (eds) World Health Organization Classification of Tumours: Pathology and Genetics of Head and Neck Tumours. Lyon IARC Press 43-45.
-
Catalano PJ, Brandwein M, Shah DK, Urken ML, Lawson W, et al. (1996) Sinonasal hemangiopericytomas: a clinicopathologic and immunohistochemical study of seven cases. Head Neck 18: 42-53.
-
Gillman G, Pavlovich JB (2004) Sinonasal hemangiopericytoma. Otolaryngol Head Neck Surg 131: 1012-1013.
-
Dandekar M, McHugh JB (2010) Sinonasal glomangiopericytoma: case report with emphasis on the differential diagnosis. Arch Pathol Lab Med 134: 1444-1449.
-
Wang CC, Chu ST (2013) Glomangiopericytoma of nasal cavity: A rare sinonasal perivascular tumor. J Med Sci 33: 107-111.
-
Duval M, Hwang E, Kilty SJ (2013) Systematic review of treatment and prognosis of sinonasal hemangiopericytoma. Head Neck 35: 1205-1210.
-
Higashi K, Nakaya K, Watanabe M, Ikeda R, Suzuki T, et al. (2011) Glomangiopericytoma of the nasal cavity. Auris Nasus Larynx 38: 415-417.
-
Szewczyk-Bieda MJ, White RD, Budak MJ, Ananthakrishnan G, Brunton JN, et al. (2014) A whiff of trouble: tumours of the nasal cavity and their mimics. Clin Radiol 69: 519-528.
-
Kuo FY, Lin HC, Eng HL, Huang CC (2005) Sinonasal hemangiopericytoma-like tumor with true pericytic myoid differentiation: a clinicopathologic and immunohistochemical study of five cases. Head Neck 27: 124-129.





