Journal of Otolaryngology and Rhinology
Extracapsular Dissection-Endocapsular Decompression: An Easy Method to Avoid Facial Nerve Injury in Surgery for Extended Parapharyngeal Adenomas of the Parotid Gland
D'Ascanio Luca*, Palmeri Annamaria Iole, Pappacena Marco and Piazza Fabio
Department of Otolaryngology - Head & Neck Surgery, "Carlo Poma" Civil Hospital, Italy
*Corresponding author:
Luca D'Ascanio, Department of Otolaryngology - Head & Neck Surgery, "Carlo Poma" Civil Hospital, Mantova, Italy, Tel: 39-3283186967, Fax: 39-(0)376201624, E-mail: l.dascanio@gmail.com
J Otolaryngol Rhinol,
JOR-1-005, (Volume 1, Issue 1),
Case Report
Received: August 6, 2015: Accepted: September 7, 2015: Published: September 9, 2015
Citation: Luca DA, Iole PA, Marco P, Fabio P (2015) Extracapsular Dissection-Endocapsular Decompression: An Easy Method to Avoid Facial Nerve Injury in Surgery for Extended Parapharyngeal Adenomas of the Parotid Gland. J Otolaryngol Rhinol 1:005
Copyright: © 2015 Luca DA. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The optimal surgical approach for extended parapharyngeal pleomorphic adenomas of the parotid gland is still controversial, also in relation to the possible complications of this type of surgery. We report our experience on 5 patients treated in the last 4 years with the "extracapsular dissection-endocapsular decompression" surgical approach for parotid deep lobe extended adenomas. The surgical details are described. No complication in terms of temporary/permanent facial paralysis, sialocele or Frey's syndrome was noticed. No adenoma recurrence was recorded. Further trials with long-term follow-up should be performed to confirm these findings and definitely demonstrate the efficacy of this method to prevent recurrences.
Keywords
Endocapsular decompression, Parotid gland, Pleomorphic adenoma, Facial nerve, Medicolegal complications
Introduction
Over the past three decades, the approach to parotid gland benign tumors has changed from superficial or total parotidectomies to partial/selective parotidectomies or extracapsular dissection [1]. Despite the controversies in the international literature, a general agreement on the value of the partial parotidectomy approach is currently well established [1-3]. The principles of partial/selective parotidectomies have recently been extended by some authors to the management of parotid deep lobe benign tumors, shifting surgical treatment of these neoplasms from total or near total parotidectomies to selective deep lobe resections (SDLRs) [3]. Despite the advantages of SDLRs in terms of reduced complications with respect to more extensive procedures, the frequency of permanent/temporary facial nerve functional impairment in case of SDLR for pleomorphic adenoma of the parotid deep lobe is still considerable [3-5]. Extended parapharyngeal adenomas mostly arise from parotid deep lobe and grow medially into the parapharyngeal space [6]. Surgery of extended parapharyngeal adenomas is one of the most common causes of litigation in head and neck practice, because of the anatomical structures (i.e. facial nerve) potentially damaged during parapharyngeal adenoma excision [7].
In order to avoid such risk, in the last 4 years we have treated 5 cases of extended pleomorphic adenomas of the parotid deep lobe with an "extracapsular dissection-endocapsular decompression" approach. The results and basic principles of our technique are discussed.
Case series
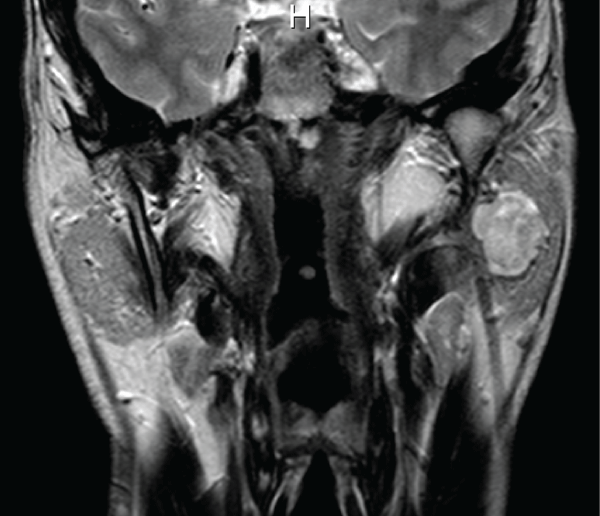
Between 2012 and 2015 we operated 5 (4M, 1F; age range: 34-67 years) patients affected by extended pleomorphic adenoma of the parotid gland deep lobe (Table 1). Among those patients, 1 male presented also a synchronous adenoma of the parotid inferior tail (Figure 1 and Figure 2). Preoperative ultrasound-guided fine-needle aspiration cytology and contrast-MRI were performed in all our patients. All subjects signed a preoperative written informed consent. Institutional review board was obtained from our Hospital's committee.
A Redon or face-lift incision is performed and a skin-subcutaneous flap is elevated. The great auricular nerve and its posterior branch are identified on the surface of the sternocleidomastoid muscle, dissected and preserved. The main trunk of the facial nerve is identified using classical landmarks and carefully dissected. The nerve branches are isolated and the superficial lobe of the parotid gland is raised. The superficial lobe is usually split into two halves (superior and inferior) to achieve an easier and quicker approach to the deep lobe. In one case, a superficial parotidectomy was carried out because of a concomitant plemorphic adenoma of the superficial lobe. Once the tumor of the parotid deep lobe is identified, only those branches of the facial nerve in contact with the lateral surface of the adenoma are freed from the underlying tumor. Some glandular tissue is left attached to the facial nerve branches to guarantee the blood supply and reduce the risk of functional impairment due to ischemia/traction (Figure 3).
.
Figure 1: Coronal T2-MRI scan showing a pleomorphic adenoma (diameter: 41mm) occupying the deep lobe of the left parotid gland.
View Figure 1
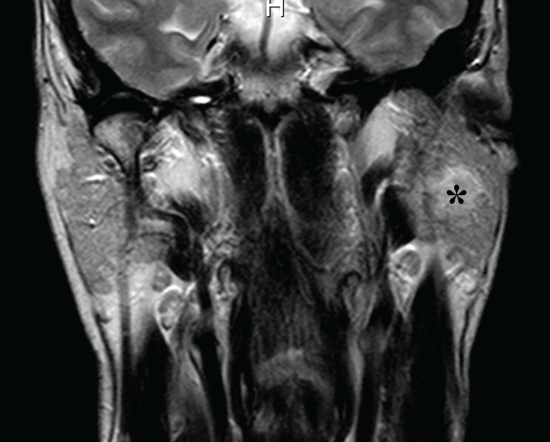
.
Figure 2: Coronal T2-MRI scan (more anterior) of the same patient, showing a smaller second pleomorphic adenoma (white arrow) occupying the inferior tail of the left parotid gland. Deep lobe adenoma(*).
View Figure 2
The adenoma is freed from the surrounding glandular tissue of the parotid deep lobe by accurately following the tumor capsule, without interrupting it, as far as possible ("extracapsular dissection") [8]. Then a small (2-3mm) incision is performed on the lateral surface of the tumor capsule and the adenoma content is removed either by suction or microdebrider (as already reported for schwannomas) [9].
![]()
Table 1: Main features of tumors and patients submitted to surgery for extended parapharyngeal adenomas with extracapsular dissection-endocapsular decompression technique.
View Table 1
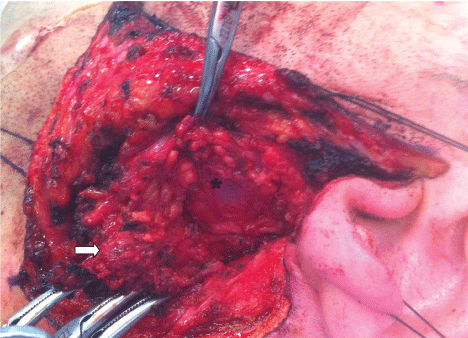
.
Figure 3: Intraoperative view after superficial parotidectomy for the removal of the parotid tail adenoma (white arrow); the superficial lobe is pulled inferiorly. The deep lobe adenoma (*) can be noticed beneath the branches of the facial nerve.
View Figure 3
Such maneuver allows an endoluminal collapse ("endocapsular decompression") and increases the "dissecting space" between the medial aspect of the adenoma capsule and the surrounding structures (glandular tissue, major vessels and pterygoid muscles) (Figure 4). The surgical field is accurately washed and examined to rule out the presence of any residual adenoma tissue. Finally, the superficial parotid lobe is repositioned and sutured to the pre-tragal tissues and sternocleidomastoid muscle with resorbable sutures, achieving a complete reconstruction of the parotid fascia. A suction drain is inserted and the skin flap is sutured back in place. None of our patients showed any complication in terms of temporary/permanent facial paralysis, sialocele or Frey's syndrome (Figure 5). No adenoma recurrence has been recorded so far (follow-up ranging between 4 years and 5 months).
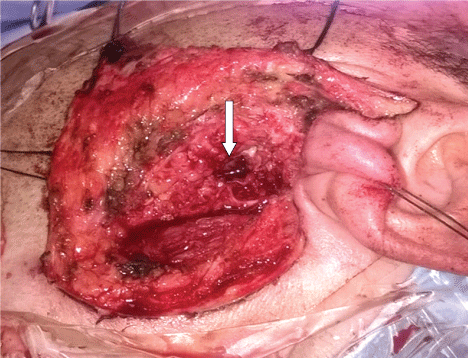
.
Figure 4: Intraoperative view after excision of the deep lobe adenoma through the "extracapsular dissection-endocapsular decompression" approach. Only those branches of the facial nerve which are in contact with the lateral surface of the adenoma are freed from the underlying tumor, which reduces the risk of functional nerve impairment. Notice the small size of the residual defect (arrow) in the deep lobe after adenoma removal, which improves facial aesthetic outcome.
View Figure 4
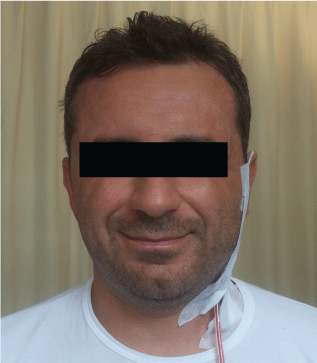
.
Figure 5: The same patient showing no facial impairment on the first postoperative day.
View Figure 5
Discussion
The improvement in surgical techniques and the effectiveness of conservative procedures for the treatment of benign tumors of the parotid gland have led to a change in the primary goals of parotid surgery. These procedures should aim at complete tumor resection, prevention of recurrences and preservation of facial nerve function with satisfactory cosmetic results and low complication rates [3,10]. The standard approach to a deep parotid lobe tumor is traditionally represented by total/near total parotidectomy, with sacrifice of the superficial lobe and dissection of all the branches of the facial nerve. This leads to several functional and esthetic disadvantages. In particular, the complete dissection of the facial nerve increases the risk of temporary or permanent facial nerve weakness, which represents the most common cause of lawsuits in salivary gland surgery [7]. Other proposed approaches (i.e. transcervical, transparotid-transcervical, transmandibular-transcervical, transparotid-intraoral) have shown similar drawbacks in terms of functional disadvantages [4,11]. In the attempt to reduce facial nerve complications, some authors proposed partial deep lobe parotidectomies [3], which are however associated with relevant risks of facial impairment, especially in case of tumor location in the upper/anterior part of the parotid deep lobe [4]. In our experience, the "extracapsular dissection-endocapsular decompression" approach has proved to be useful to treat extended pleomorphic adenomas of the parotid deep lobe with no case of temporary/permanent facial weakness. Such result is attained by limiting nerve lift to the branches proximal to the tumor [3] and by preserving a "cuff" of vascularised glandular tissue around the nerve. The "endocapsular decompression" [9] allows to overcome the drawbacks of the limited field exposure by producing an "endoluminal collapse" of the adenoma which can be easily detached from the surrounding tissues (glandular tissue, major vessels) without traction to the nerve. The "endocapsular decompression" procedure, borrowed from schwannoma surgery [9], is carried out through a "minimal" (2-3mm) interruption of adenoma capsule in order to reduce the risk of tumor dissemination. The adenoma content is easily removed by suction or microdebrider and the operating field is abundantly washed with ringer solution to remove any possible remnant of adenoma tissue.
From an aesthetic point of view, our technique achieves satisfactory cosmetic results. Preservation of the superficial lobe reduces the surgical defect and allows for complete reconstruction of the parotid bed, thus preventing depression in the preauricular area and deformation of the facial contour. Furthermore, our conservative approach preserves the function of the parotid gland and seems to reduce the occurrence of Frey's syndrome [3].
The more controversial point of our procedure is its oncological safety. Previous reports on "extracapsular dissection" for pleomorphic adenomas clearly demonstrate its safety for the treatment of benign tumors of the superficial lobe [8]. However, the lack of randomized trials for deep lobe tumors, due to the rarity of this localization, does not allow drawing definite conclusions on this topic. In our experience, we did not notice any recurrence, however further studies with a longer follow-up will be useful to for a definite clarification of this issue. The main contraindications are obviously represented by the treatment for recurrences and malignancies, for which a "standard" total parotidectomy is the treatment of choice.
In conclusion, the "extracapsular dissection-endocapsular decompression" is a technically easy approach for the treatment of benign tumors of the deep parotid gland which allows avoiding facial nerve impairment and offers some interesting advantages in terms of aesthetics and Frey's syndrome prevention. Despite its encouraging oncological results, further trials with long-term follow-up periods should be performed to confirm these findings and definitely demonstrate the ability of this method to prevent recurrences.
References
-
Papadogeorgakis N (2011) Partial superficial parotidectomy as the method of choice for treating pleomorphic adenomas of the parotid gland. Br J Oral Maxillofac Surg 49: 447-450.
-
O'Brien CJ (2003) Current management of benign parotid tumors--the role of limited superficial parotidectomy. Head Neck 25: 946-952.
-
Sesenna E, Bianchi B, Ferrari S, Copelli C, Ferri T, et al. (2013) Selective deep lobe parotidectomy for pleomorphic adenomas. Int J Oral Maxillofac Surg 42: 1129-1133.
-
Ikoma R, Ishitoya J, Sakuma Y, Hirama M, Shiono O, et al. (2014) Temporary facial nerve dysfunction after parotidectomy correlates with tumor location. Auris Nasus Larynx 41: 479-484.
-
Musani MA, Zafar A, Suhail Z, Malik S, Mirza D (2014) Facial nerve morbidity following surgery for benign parotid tumours. J Coll Physicians Surg Pak 24: 569-572.
-
Sergi B, Limongelli A, Scarano E, Fetoni AR, Paludetti G (2008) Giant deep lobe parotid gland pleomorphic adenoma involving the parapharyngeal space. Report of three cases and review of the diagnostic and therapeutic approaches. Acta Otorhinolaryngol Ital 28: 261-265.
-
Hong SS, Yheulon CG, Sniezek JC (2013) Salivary gland surgery and medical malpractice. Otolaryngol Head Neck Surg 148: 589-594.
-
Mantsopoulos K, Koch M, Klintworth N, Zenk J, Iro H (2015) Evolution and changing trends in surgery for benign parotid tumors. Laryngoscope 125: 122-127.
-
Chennupati SK, Schipor I, Mirza N (2006) Microdebrider decompression of schwannoma: a novel method of excising a neck mass. Laryngoscope 116: 2086-2088.
-
Bianchi B, Ferri A, Ferrari S, Copelli C, Sesenna E (2011) Improving esthetic results in benign parotid surgery: statistical evaluation of facelift approach, sternocleidomastoid flap, and superficial musculoaponeurotic system flap application. J Oral Maxillofac Surg 69: 1235-1241.
-
Horowitz G, Ben-Ari O, Wasserzug O, Weizman N, Yehuda M, et al. (2014) The transcervical approach for parapharyngeal space pleomorphic adenomas: indications and technique. PLoS One 9: e90210.





