Journal of Otolaryngology and Rhinology
Unusual Manifestation of Herpes Zoster Infection Involving the Greater, Lesser Occipital and Transverse Cervical Nerve: A Case Report
Emilio Mevio*
Department of Otorhinolaryngology, Fornaroli Hospital, Italy
*Corresponding author:
Emilio Mevio, Department of Otorhinolaryngology, Fornaroli Hospital, via Donatore del sangue 50, 20013 Magenta, Italy, Tel: 39-382302525, E-mail: emevio@libero.it
J Otolaryngol Rhinol,
JOR-1-004, (Volume 1, Issue 1),
Case Report
Received: July 27, 2015: Accepted: September 1, 2015: Published: September 3, 2015
Citation: Mevio E (2015) Unusual Manifestation of Herpes Zoster Infection Involving the Greater, Lesser Occipital and Transverse Cervical Nerve: A Case Report. J Otolaryngol Rhinol 1:004
Copyright: © 2015 Mevio E. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We here present a case of Varicella Zoster Virus (VZV) infection with involvement of C2 and C3 right cranial nerve. The initial symptoms (right occipital neuralgia, pharyngodynia, and otalgia) were complicated by vesicular skin lesions spread along the course of the right transverse cervical and of greater occipital nerve. The diagnosis was confirmed by serological tests. Therapeutical approach is then commented.
Keywords
Herpes zoster, Cervical plexus
Introduction
The most common presentation of Herpes Zoster infection in the head and neck region is Ramsay Hunt syndrome (RHS). RHS represents a complication of the Varicella Zoster Virus (VZV) infection, tipically presenting with the triad of ipsilateral peripheral type facial nerve paralysis, ipsilateral ear pain and erythematous vesicles in the external auditory canal. Herpes Zoster results from the reactivation of VZV in the dorsal root ganglia and RHS can be associated with trigeminal, abducent, glossopharyngeal, and vagus nerve, but rarely with hypoglossal nerve [1-3]. However, some unusual variants may occur [4]. We describe an atypical case of VZV syndrome with involvement of greater occipital nerve (branch of second cervical nerve), the auriculotemporal branch of the lesser occipital nerve (branch of second cervical nerve) and transverse cervical nerve (branches of second and third cervical nerve).
Case
A 60-year-old female had presented with headache which was localized in the right occipital region, right otalgia and pharyngodinia for the last 4 days. She described sharp, electric shock-like pain attacks with a sudden onset, ending in a few seconds. Palpation of the right greater occipital nerve triggered the pain. Vesicular skin lesions were detected along the course of the transverse cervical nerve (Figure 1) and of the greater occipital nerve. There was no evidence of oral or pharyngeal mucosal lesions. Her past medical history revealed a varicella infection in childhood, but she had no history of head or neck neuralgia. Based on the morphologic characteristics and distribution of skin lesions and increased VZV-specific IgM antibody titer in blood (2.42 Vs < 1.0: negative index), patient was diagnosed as having Herpes Zoster. Viral infection was treated with famciclovir 500 mg, 8 hourly, for 15 days; pain was treated with dexibuprofen (400 mg, 8 hourly, for the first week and as needed thereafter). The patient refused the steroid therapy that we usually associated to antiviral treatment.
.
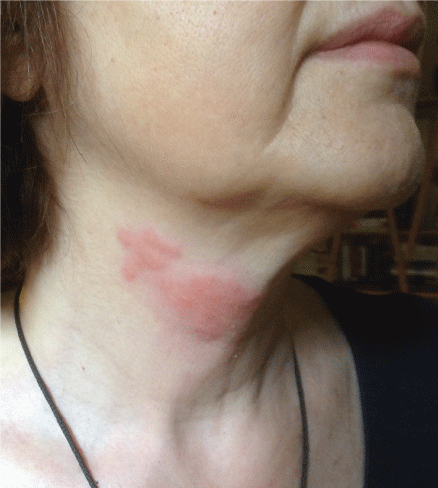
Figure 1: Vesicular skin lesions along the course of the right transverse cervical nerve
View Figure 1
Ten days after the treatment start, skin lesions and pain improved: the patient recovered completely 4 weeks after.
Discussion
Distinct neurologic syndromes associated with Herpes Zoster infection include acute or chronic encephalitis, ophthalmic Zoster with contralateral hemiparesis, myelitis, polyradiculitis, motor neuropathies, and a variety of cranial and peripheral nerve palsies, including Bell's palsy and RHS [4]. The most common presentation of herpes zoster in the head and neck region is RHS. The syndrome is caused by reactivation of VZV infection in the geniculate ganglion of the facial nerve. Its clinical hallmarks are facial palsy, otalgia, and herpetic vesicles around the auricle and external auditory canal. In rare cases symptoms also involve other cranial nerves. Shim et al. [5] reported a case of a patient with RHS who developed dysphagia due to multiple cranial nerve involvement including the glossopharyngeal nerve and vagus nerve.
Another case of Herpes Zoster involving the ophthalmic and maxillary divisions of the trigeminal nerve with accompanying rare complications such as alveolar bone necrosis and rapid tooth exfoliation was reported by Pushpanshu et al. [6]. Dyspnea resulting from diaphragmatic paralysis caused by motor roots involvement in patients with acute Herpes Zoster infection was described by Lin and Oike in 2012 [7,8].
Most clinicians readily recognize typical clinical signs and symptoms of Varicella and Herpes Zoster. However, in certain circumstances and in special populations, VZV infection can present with unusual manifestations. The reported case represents a unusual combination of facial Herpes lesions and pain in the C2 and C3 regions [9,10].
The diagnosis was made easier by the clinical symptoms and the characteristic distribution of the typical skin vesicles along selective areas of innervation of C2 and C3. The increased VZV-specific IgM antibody in blood confirmed the suspected diagnosis.
Famciclovir was chosen as antiviral treatments taking into account its therapeutic efficacy and patient compliance. Famciclovir is actually a prodrug, which is converted into the active form (penciclovir) in the liver. Famciclovir is active against the same viruses as acyclovir but has a longer duration of action [11]. Therefore, it can be taken only three times each day.
In a literature review was demonstrated a statistically significant difference between combined antiviral-conticosteroid therapy and treatment with corticosteroids alone. The complete remission or a good recovery of nerve sensitivity and function was more frequent in patients treated with combined therapy [12]. The effectiveness of corticosteroid therapy can be explained by their pharmacological effects on inflammatory edema of neurogenic structures. In our case the patient refused the corticosteroid treatment and we choosed a nonsteroid anti-inflammatory drug in order to have a comparable effect. In any case all authors agree with the fact that there was a tendency to better remission in patients treated promptly.
References
-
Zainine R, Sellami M, Charfeddine A, Beltaief N, Sahtout S, et al. (2012) Ramsay Hunt syndrome. Eur Ann Otorhinolaryngol Head Neck Dis 129: 22-25.
-
Eun Woong Ryu, Ho Yun Lee, So Yoon Lee, Moon Suh Park, Seung Geun Yeo (2012) Clinical manifestations and prognosis of patients with Ramsay Hunt syndrome. Am J Otolaryngol 33: 313-318.
-
Lee HH, Huang LK, Hu CJ, Chen CC (2014) Atypical Ramsay Hunt syndrome. Acta Neurol Taiwan 23: 80-81.
-
Gnann JW Jr (2002) Varicella-zoster virus: atypical presentations and unusual complications. J Infect Dis 186 Suppl 1: S91-98.
-
Shim JH, Park JW, Kwon BS, Ryu KH, Lee HJ, et al. (2011) Dysphagia in Ramsay Hunt's Syndrome - A Case Report. Ann Rehabil Med 35: 738-741.
-
Pushpanshu K, Kaushik R, Srivastava S, Punyani SR (2013) An unusual complication of tooth exfoliation and osteonecrosis following herpes zoster infection of trigeminal nerve: a case report and literature review. Minerva Stomatol 62: 241-5.
-
Lin CM, Shieh WB, Chiang PC, Shieh MG, Liu YC, et al. (2012) An unusual cause of dyspnea in a patient with cervical herpes zoster. J Clin Neurosci 19: 608-609.
-
Oike M, Naito T, Tsukada M, Kikuchi Y, Sakamoto N, et al. (2012) A case of diaphragmatic paralysis complicated by herpes-zoster virus infection. Intern Med 51: 1259-1263.
-
Kihara T, Shimohama S (2006) Occipital neuralgia evoked by facial herpes zoster infection. Headache 46: 1590-1591.
-
Ipekdal HI, YiÄYitoÄYlu PH, Eker A, OzmenoÄYlu M (2013) Occipital neuralgia as an unusual manifestation of herpes zoster infection of the lesser occipital nerve: a case report. Acta Neurol Belg 113: 201-202.
-
Gopal MG, Shannoma, Kumar B C S, M R, A S N, et al. (2013) A comparative study to evaluate the efficacy and safety of acyclovir and famciclovir in the management of herpes zoster. J Clin Diagn Res 7: 2904-2907.
-
Wagner G, Klinge H, Sachse MM (2012) Ramsay Hunt syndrome. J Dtsch Dermatol Ges 10: 238-244.





