Journal of Otolaryngology and Rhinology
Ramsay Hunt Syndrome Type 2: A Review of an Uncommon and Unwelcome Neurodermatologic Disease
Reid A. Waldman1*, Corey W. Waldman2 and Steven D. Waldman1
1University of Missouri-Kansas City School of Medicine, USA
2Krieger Eye Institute, USA
*Corresponding author:
Reid A. Waldman, University of Missouri-Kansas City School of Medicine, Kansas City, Missouri, USA, Tel: 913-327-5999, E-mail: rawthf@mail.umkc.edu
J Otolaryngol Rhinol,
JOR-1-003, (Volume 1, Issue 1),
Review Article
Received: July 30, 2015: Accepted: August 26, 2015: Published: August 28, 2015
Citation: Waldman RA, Waldman CW, Waldman SD (2015) Ramsay Hunt Syndrome Type 2: A Review of an Uncommon and Unwelcome Neurodermatologic Disease. J
Otolaryngol Rhinol 1:003
Copyright: © 2015 Waldman RA. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Ramsay Hunt Syndrome Type II is the eponym given to a constellation of symptoms including a vesicular rash of the external ear and the ipsilateral two thirds of the tongue with associated paralysis of the seventh cranial nerve.* The syndrome, which is also known as herpes zoster oticus, as well as, shingles of the geniculate ganglion, is caused by re-activation of the varicella-zoster virus (VZV) within the geniculate ganglion and associated sensory nerves. Frequently, other cranial nerves including the VIII, IX, X, and XI nerves are affected suggesting that Ramsay Hunt syndrome may be more properly thought of clinically as a polycranial neuronitis rather than an infection limited to the geniculate ganglion of the seventh cranial nerve. Rapid diagnosis and treatment of this rare neurodermatologic condition is crucial to avoid permanent complications.
Introduction
First described in 1907 by James Ramsay Hunt, an American neurologist, Ramsay Hunt syndrome is the eponym given to a constellation of symptoms including a vesicular rash of the external ear and the ipsilateral two thirds of the tongue with associated paralysis of the seventh cranial nerve [1]. The syndrome, which is also known as herpes zoster oticus and Hunt's syndrome, is believed to be caused by reactivation of dormant varicella-zoster virus (VZV) within the geniculate ganglion and associated sensory nerves. This reactivation of dormant virus results in a painful erythematous vesicular rash involving the involving the ear as well as the anterior two/thirds of the ipsilateral tongue and anterior palate. Frequently, other cranial nerves are affected [2]. This article will review the clinical presentation of this uncommon painful neurodermatologic condition and present treatment options to help palliate the acute symptoms associated with this disease and to hopefully prevent the development of postherpetic neuralgia.
Clinical Syndrome
Ramsay Hunt Syndrome Type II is the eponym given to a constellation of symptoms including a vesicular rash of the external ear and the ipsilateral two thirds of the tongue with associated paralysis of the seventh cranial nerve.* The syndrome, which is also known as herpes zoster oticus, as well as, shingles of the geniculate ganglion, is caused by re-activation of the varicella-zoster virus (VZV) within the geniculate ganglion and associated sensory nerves. Frequently, other cranial nerves including the VIII, IX, X, and XI nerves are affected suggesting that Ramsay Hunt syndrome may be more properly thought of clinically as a polycranial neuronitis rather than an infection limited to the geniculate ganglion of the seventh cranial nerve [3]. Rapid diagnosis and treatment of this rare neurodermatologic condition is crucial to avoid permanent complications.
In the nonimmune host, primary infection with VZV presents as the childhood exanthem chickenpox. During a primary infection, the varicella virus can invade the geniculate ganglia becoming dormant there as the host mounts an immune response. The virus maintains itself there, producing no clinically evident disease, until conditions are suitable for the virus to re-active. Evidence suggests that such conditions are characterized by a subsequent decrease in cell-mediated immunity which allows the dormant VZV residing within the geniculate ganglion to multiply and spread to the corresponding nerves producing the pain, vesicular skin lesions, and motor deficit of the seventh cranial nerve that is characteristic of Ramsay Hunt syndrome [2]. This is primarily seen in immunosuppressed patients such as those who are HIV position, those with malignancy (particularly lymphoma, those receiving immunosuppressive therapy (chemotherapy, steroids, radiation), those over the age of 60, and those afflicted by chronic, debilitating illness [4,5].
Most commonly, acute herpes zoster is seen in thoracic dermatomes after re-activation of dormant virus within the thoracic sympathetic ganglia. The second most common site of reactivation is first division of the trigeminal nerve [6]. In less than 0.8% of the general population, dormant VZV may reactivate within the geniculate ganglion and its associated nerves resulting in facial pain, hearing loss, vertigo, vesicles in the ear, and pain [7].
Signs and Symptoms
When reactivation of VZV occurs, the patient may experience a prodrome of flu-like symptoms accompanied by a dull, deep, aching sensation in the ear which often progresses to sharper, dysesthetic, neuritic-type pain in the distribution of the geniculate ganglion. This pain will usually precede the eruption of the characteristic vesicular rash by 3 to 7 days, often causing those who seek treatment in the prodromal period to be misdiagnosed with otitis media, costochondritis of the concha, and other disorders of the ear [7].
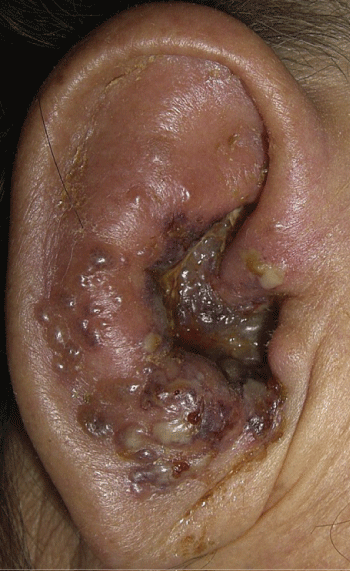
The clinical diagnosis of shingles becomes apparent when the characteristic vesicular rash appears. Like its antecedent infection, chickenpox, the dermatologic manifestations of Ramsay Hunt Syndrome Type II appear in crops of macular lesions, which rapidly progress to papules, and then to vesicles involving the ear as well as the anterior two/thirds of the ipsilateral tongue and anterior palate. (Figure 1,2) As the disease progresses, the vesicles begin to coalesce and rupture ultimately leading to crusting of the open lesions. The skin and mucosa affected by the lesions can be extremely painful with worsening the pain secondary to movement or contact. As healing of the lesions occurs the crusts and scabs fall away, leaving pink scars in the distribution of the rash that gradually become hypopigmented and atrophic. Overtime, complete or near complete resolution of the cutaneous manifestations of the disease occurs. Finally, the acute presentation of Ramsay Hunt can also be characterized by a lower motor neuron homolateral facial paralysis that is clinically analogous to Bell's palsy. Additionally, if other adjacent cranial nerves are involved, the patient may develop vertigo, tinnitus, and hearing loss.
.
Figure 1: Characteristic vesicular eruptions secondary to varicella zoster virus in a patient with Ramsay Hunt syndrome.
View Figure 1
.
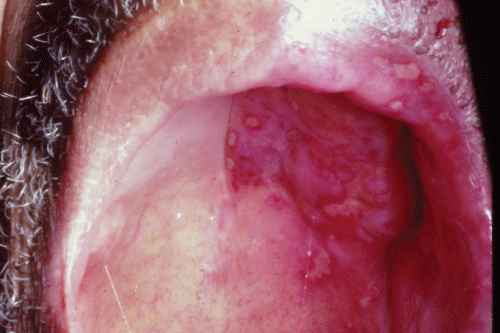
Figure 2: Healing vesicular lesions of the lip and palate in a patient with Ramsay Hunt syndrome.
View Figure 2
In the majority patients, the neuropathic pain associated with Ramsay Hunt Syndrome resolves as the skin lesions heal; however, in a small minority of patients, pain may persist beyond lesion healing. This persistent pain is known as postherpetic neuralgia. Notably, this affliction effects elderly patient at a much higher rate than their younger counterparts [7]. The pain of postherpetic neuralgia can range from a mild, self-limited annoyance to severe, unremitting, debilitating pain that is exacerbated by light touch, movement, anxiety, or temperature change. To avoid the disastrous sequela of postherpetic neuralgia, prompt, accurate diagnosis and treatment are imperative.
Testing
Although in most patients the diagnosis of Ramsay Hunt syndrome can be made on clinical grounds, in some patients, especially those with other dermatologic conditions that confuse the clinical picture (e.g. Kaposi's sarcoma), laboratory testing may be beneficial. In such patients, the diagnosis of acute herpes zoster may be confirmed by obtaining a Tzanck smear from the base of a fresh vesicle. When VZV is the causative agent this reveals multinucleated giant cells and eosinophilic inclusions [8]. To differentiate acute herpes zoster from localized herpes simplex infection, polymerase chain reaction testing of the patient's tears, saliva, and/or blood may be beneficial [9].
Differential Diagnosis
When encountering a case of probable Ramsay Hunt syndrome, a careful search for underlying occult malignancy or other systemic disease that may be responsible for the patient's underlying immunocompromised state is always indicated. A careful history and physical examination will aid the clinician in identifying changes in clinical status that may precede the development of complications, including myelitis or dissemination of the virus. Other diseases that may mimic the pain associated with Ramsay Hunt syndrome include diseases of the ear and sinuses, glaucoma, retro-orbital tumors, inflammatory diseases such as Tolusa-Hunt syndrome, and intracranial pathology, including tumors and infections [7].
Treatment
There are two primary goals when treating a patient suffering from Ramsay Hunt syndrome: (1) to provide immediate relief of acute pain and symptoms, (2) to prevent complications including exposure keratopathy of the ipsilateral cornea due to the patient's inability to properly close the eye, and (3) to prevent the late complication of postherpetic neuralgia. Clinical experience suggests that earlier treatment is associated with less development of postherpetic neuralgia [10]. Because older patients and severely immunocompromised patients are at highest risk for developing postherpetic neuralgia, early aggressive treatment of these patients is mandatory.
Antiviral Agents
Famciclovir, valacyclovir, and acyclovir have been shown to shorten the duration of viral shedding as well as shorten the course of the acute cutaneous manifestations of the VZV infection [11]. There is increasing evidence that the early use of these antiviral agents may also help prevent the development of postherpetic neuralgia [12]. These drugs are also thought to help attenuate the severity and duration of the disease in severely immunocompromised patients [13]. These antiviral agents can be used in conjunction with the treatment modalities discussed below.
Sympathetic Nerve Blocks
Stellate ganglion blocks utilizing local anesthetics and steroids can be used in combination with antivirals to help relieve the symptoms associated with Ramsay Hunt syndrome as well as to help decrease the incidence of postherpetic neuralgia [14]. Stellate ganglion block of the sympathetic ganglia on the affected side is thought to accomplish these salutary effects by blocking the neural ischemia that occurs secondary to decreased blood flow of the intraneural capillary bed that is the result of the profound sympathetic stimulation caused by the acute viral inflammation of the nerve and geniculate ganglion. If untreated, this ischemia can cause endoneural edema which results in increasing endoneural pressure which causes a further reduction of endoneural blood flow. If the decreased endoneural blood flow allowed to persist, irreversible nerve damage and associated persistent neuropathic pain and paralysis will result.
Steroids
Clinical experience suggests that the administration of steroids, either orally or injected in combination with local anesthetic when performing stellate ganglion block may not only decrease the acute symptoms associated with Ramsay Hunt syndrome, but decrease the incidence of persistent facial paralysis by 50% [14,15]. Additionally, it has been found to decrease the incidence of postherpetic neuralgia. A dose of 80mg of prednisone administered in divided doses orally and then tapered by 5mg per day is a reasonable course of treatment so long as the patient is carefully monitored for the side effects associated with high dose oral steroid use such as gastrointestinal bleeding.
Opioid Analgesics
Opioid analgesics may be useful in palliating the severe acute somatic pain associated with Ramsay Hunt syndrome [7]. These drugs are less effective in the relief of the neuritic pain that is also often present. Careful administration of potent, long-acting narcotic analgesics (e.g., oral morphine elixir or methadone) on a time-contingent rather than as-needed basis may be used concurrently with the administration of antiviral agents, steroids, and sympathetic neural blockade. Because many patients with Ramsay Hunt syndrome are elderly or have severe, multisystem disease, careful monitoring for the potential side effects of potent narcotic analgesics (e.g., confusion or dizziness, which may cause a patient to fall) is warranted. Daily dietary fibre supplementation and milk of magnesia should be started along with opioid analgesics to prevent constipation.
Adjuvant Analgesics
The anticonvulsants gabapentin and pregablin may be beneficial in the palliation of neuritic pain of acute herpes zoster involving the geniculate ganglion and may be used concurrently with neural blockade, opioid analgesics, steroids, and other adjuvant analgesics including the antidepressant compounds [16,17]. As with the use of opioids, patients receiving gabapentin must be closely monitored for central nervous system side effects. Studies suggest that gabapentin and pregablin also may help prevent the development of postherpetic neuralgia [18]. Treatment with gabapentin and pregablin should begin early in the course of the disease.
Carbamazepine is a reasonable next step for patients with severe neuritic pain who have failed to respond to nerve blocks and gabapentin or pregablin [19]. Mandatory monitoring of hematological parameters, especially in patients receiving chemotherapy or radiation therapy, is indicated to identify potentially life threatening idiopathic aplastic anemia associated with carbamazepine [20]. Phenytoin may also be used to treat intractable neuritic pain associated with Ramsay Hunt syndrome, but this drug should be avoided in patients with lymphoma because the drug may induce a pseudolymphoma-like state that is difficult to distinguish from the actual primary lymphoma itself [21].
If significant sleep disturbance is present, then antidepressants may be useful adjuncts in the initial treatment of patients with Ramsay Hunt syndrome [22]. Antidepressants may also help decrease the neuritic component of the pain and exert a mood-elevating effect that may be desirable in many patients. As with the other adjuvant analgesics, patients must be observed closely for central nervous system side effects. These drugs may also cause urinary retention and constipation that may be mistakenly attributed to herpes zoster myelitis.
Physical Modalities
The application of ice packs to the lesions of acute herpes zoster may provide symptomatic relief in some patients, while the application of heat will often increase pain as a result of increased conduction of small fibers. Transcutaneous electrical nerve stimulation and vibration may also provide symptomatic relief. The favorable risk-to-benefit ratio of these physical modalities makes them reasonable alternatives for patients who cannot or will not undergo sympathetic neural blockade and do not tolerate the aforementioned pharmacologic interventions.
Topical application of a tepid solution of aluminum sulfate as a soak will provide symptomatic relief and promote the drying of the crusting and weeping lesions of the acute VZV infection [23]. Topical application of zinc oxide ointment as a protective agent may be especially useful if temperature sensitivity of the affected area is a problem [23]. Disposable diapers can be used as an absorbent padding to promote drying of the weeping lesions and to protect healing lesions from contact with clothing and sheets. Topical capsaicin and lidocaine may also provide symptomatic relief of persistent pain after the acute vesicular lesions have healed [24].
Complications of Acute VZV Infection of the Geniculate Ganglion
Many patients suffering from Ramsey Hunt syndrome will eventually recover, but in the elderly and immunocompromised patients, serious complications may occur [3,25]. Cutaneous and visceral dissemination may range from a mild chickenpox-like rash to an overwhelming, life-threatening disseminated infection. Infection may spread from the geniculate ganglion to adjacent cranial nerves and in rare cases; the central nervous system may be affected. Myelitis may cause bowel, bladder, and extremity paresis and rarely encephalitis may occur [26]. Ocular complications secondary to the patient's inability to properly close the ipsilateral eye may result in exposure keratopathy leading to permanent corneal damage.
Conclusion
Ramsay Hunt syndrome is a rare neurodermatologic condition that is caused by reactivation of the herpes virus within the geniculate ganglion and associated nerves. Because the pain associated with acute VZV infection usually precedes the appearance of the classic vesicular skin lesions by 5 to 7 days, delay of correct diagnosis is the rule rather than the exception. Often, primary diseases of the ear such as otitis media and externa are made and occasionally, trigeminal neuralgia is diagnosed. In the setting of unexplained otalgia, the astute clinician should advise the patient to call immediately should a rash involving the ear appear as early treatment of the acute VZV infection is crucial to help avoid sequella. It is the belief of some clinicians that some patients mount a rapid immune response that greatly attenuates the clinical manifestations of acute reactivation of the VZV. As a result, reactivation within the geniculate ganglion and associated nerves does not always produce the characteristic vesicular rash of acute herpes zoster. This presence of pain in the absence of a vesicular rash is called zoster sine herpete. Some goes as far as to say that Bell's palsy may in fact be zoster sine herpete of the geniculate ganglion. It is worth noting that other causes of ear and head pain and associated facial palsy must be first ruled out before invoking a diagnosis of zoster sine herpete. Because of the potential involvement of other cranial nerves in patients with Ramsay Hunt syndrome, the patient should be advised that dizziness, hearing loss, and loss of taste may also occur. The role of the new shingles vaccine in the prevention of Ramsay Hunt syndrome has not yet been proven, but is an appealing clinical theory.
*The reader should be aware that there is some confusion surrounding the eponym Ramsay Hunt and there are three distinct diseases that bear this name: Ramsay Hunt syndrome I which is rare, degenerative, neurological disorder characterized by myoclonus epilepsy, intention tremor, progressive ataxia; Ramsay Hunt syndrome II which is described above; and Ramsay Hunt III which is an occupationally induced neuropathy of the deep branch of the ulnar nerve.
References
-
Hunt JR (1907) On herpetic inflammations of the geniculate ganglion: a new syndrome of its complications. J Nerv Ment Dis 34: 73-96.
-
Ryu EW, Lee HY, Lee SY, Park MS, Yeo SG (2012) Clinical manifestations and prognosis of patients with Ramsay Hunt syndrome. Am J Otolaryngol 33: 313-318.
-
Robillard RB, Hilsinger RL Jr, Adour KK (1986) Ramsay Hunt facial paralysis: clinical analyses of 185 patients. Otolaryngol Head Neck Surg 95: 292-297.
-
Gnann JW Jr, Whitley RJ (2002) Clinical practice. Herpes zoster. N Engl J Med 347: 340-346.
-
Whitley RJ (2009) A 70-year-old woman with shingles: review of herpes zoster. JAMA 302: 73-80.
-
Steven D. Waldman (2012) Acute Herpes Zoster of the Thoracic Dermatomes. In: Waldman SD, Saunders WB. Philadelphia. Atlas of Uncommon Pain Syndromes. Elsevier: 215-217.
-
Steven D. Waldman (2012) Ramsay Hunt Syndrome. In: Steven D Waldman, WB Saunders, Philadelphia, Atlas of Uncommon Pain Syndromes, Elsevier: 32.
-
Cohen PR (1994) Tests for detecting herpes simplex virus and varicella-zoster virus infections. Dermatol Clin 12: 51-68.
-
Coffin SE, Hodinka RL (1995) Utility of direct immunofluorescence and virus culture for detection of varicella-zoster virus in skin lesions. J Clin Microbiol 33: 2792-2795.
-
Alper BS, Lewis PR (2000) Does treatment of acute herpes zoster prevent or shorten postherpetic neuralgia? J Fam Pract 49: 255-264.
-
Uscategui T, Doree C, Chamberlain IJ, Burton MJ (2008) Antiviral therapy for Ramsay Hunt syndrome (herpes zoster oticus with facial palsy) in adults. Cochrane Database Syst Rev.
-
Tyring S, Barbarash RA, Nahlik JE, Cunningham A, Marley J, et al. (1995) Famciclovir for the treatment of acute herpes zoster: effects on acute disease and postherpetic neuralgia. A randomized, double-blind, placebo-controlled trial. Collaborative Famciclovir Herpes Zoster Study Group. Ann Intern Med 123: 89-96.
-
Bodsworth NJ, Boag F, Burdge D, Généreux M, Borleffs JC, et al. (1997) Evaluation of sorivudine (BV-araU) versus acyclovir in the treatment of acute localized herpes zoster in human immunodeficiency virus-infected adults. The Multinational Sorivudine Study Group. J Infect Dis 176: 103-111.
-
Steven D. Waldman, (2015) Stellate Ganglion Block. In: Steven D. Waldman, Comprehensive Atlas of Ultrasound Guided Pain Management Injection Techniques. Lippincott Williams & Wilkins, 156-162.
-
Murakami S, Hato N, Horiuchi J, Honda N, Gyo K, et al. (1997) Treatment of Ramsay Hunt syndrome with acyclovir-prednisone: significance of early diagnosis and treatment. Ann Neurol 41: 353-357.
-
Dworkin RH, Barbano RL, Tyring SK, Betts RF, McDermott MP, et al. (2009) A randomized, placebo-controlled trial of oxycodone and of gabapentin for acute pain in herpes zoster. Pain 142: 209-217.
-
Ostwal S, Salins N, Deodhar J, Muckaden MA (2015) Management of ramsay hunt syndrome in an acute palliative care setting. Indian J Palliat Care 21: 79-81.
-
Fashner J, Bell AL (2011) Herpes zoster and postherpetic neuralgia: prevention and management. Am Fam Physician 83: 1432-1437.
-
Steven D. Waldman, (2014) Anticonvulsants. In: Steven D. Waldman, W.B. Saunders, Philadelphia, Pain Review. Elsevier, PA.
-
Tagawa T, Sumi K, Uno R, Itagaki Y, Fujii F, et al. (1997) Pure red cell aplasia during carbamazepine monotherapy. Brain Dev 19: 300-302.
-
SOvallath S, Remya RK, Kumar C, Nayanar S (2013) Granulomatous lymphadenopathy secondary to phenytoin therapy. Seizure 22: 240-241
-
Dworkin RH, Johnson RW, Breuer J, Gnann JW, Levin MJ, et al. (2007) Recommendations for the management of herpes zoster. Clin Infect Dis 44 Suppl 1: S1-26.
-
Steven D. Waldman (2014) Acute Herpes Zoster of the Thoracic Dermatomes. In: Waldman SD, Saunders WB. Philadelphia, Pain Review. Elsevier, PA.
-
Khaliq W, Alam S, Puri N (2007) Topical lidocaine for the treatment of postherpetic neuralgia. Cochrane Database Syst Rev.
-
Aleksic SN, Budzilovich GN, Lieberman AN (1973) Herpes zoster oticus and facial paralysis (Ramsay Hunt syndrome). Clinico-pathologic study and review of literature. J Neurol Sci 20: 149-159.
-
Lionnet F, Pulik M, Genet P, Petitdidier C, Davous P, et al. (1996) Myelitis due to varicella-zoster virus in two patients with AIDS: successful treatment with acyclovir. Clin Infect Dis 22: 138-140.





