Journal of Nutritional Medicine and Diet Care
Dietitian Experience with Exclusive Enteral Nutrition for the Treatment of Crohn Disease
Catherine Wall1, Andrew Day1* and Richard Gearry2
1Department of Paediatrics, University of Otago Christchurch 8140, New Zealand
2Department of Medicine, University of Otago Christchurch 8140, New Zealand
*Corresponding author:
Andrew Day, MD, PhD, Professor of Paediatrics, Head of Department of Paediatrics, University of Otago, Christchurch, 2 Riccarton Ave, PO Box 4345, Christchurch 8140, New Zealand, Tel: 64-3-364-0747, Fax: 64-3-378-6355, E-mail: andrew.day@otago.ac.nz
J Nutri Med Diet Care, JNMDC-2-015, (Volume 2, Issue 2), Original Research
Received: March 05, 2016: Accepted: May 24, 2016: Published: May 27, 2016
Citation: Wall C, Day A Gearry R (2016) Dietitian Experience with Exclusive Enteral Nutrition for the Treatment of Crohn Disease. J Nutri Med Diet Care 2:015.
Copyright: © 2016 Wall C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Aim:To understand the role(s) of New Zealand dietitians in the management of Crohn disease and dietitian experience using exclusive enteral nutrition.
Methods:An electronic survey of Dietitians New Zealand members was undertaken. A link to the survey was disseminated through their weekly electronic newsletter. Survey responses were analyzed using descriptive statistics and responses from pediatric and adult dietitians were compared using Fisher's exact test and Chi-squared test. Open ended questions were summarized using thematic analysis. The responses of New Zealand dietitians were compared to dietitian practice internationally and current inflammatory bowel disease standards of care.
Results:Seventy-seven dietitians saw patients with gastrointestinal complaints, 58 of whom were referred patients with Crohn disease. Fifty dietitians assessed a case of Crohn disease monthly or a few times a year. Pediatric and adult dietitians predominately received Crohn disease patient referrals for different reasons. Thirty-five dietitians, including 10 pediatric dietitians, had previously used exclusive enteral nutrition to treat active Crohn disease in a median of three patients. Barriers to prescribing exclusive enteral nutrition included limited Crohn disease patient load and limited referrals from gastroenterologists or surgeons. Supplementary enteral nutrition was mostly used to treat nutritional concerns. Dietitians would find useful further professional development on how to use exclusive enteral nutrition, more patient resources, professional support and also more scientific evidence to support its use with adult patients.
Conclusions:New Zealand dietitians have limited experience using exclusive enteral nutrition and are possibly underutilized in the multidisciplinary care of Crohn disease patients in New Zealand.
Keywords
Crohn's disease, Dietitian, Enteral nutrition, Exclusive enteral nutrition
Introduction
Crohn disease (CD) is an inflammatory bowel disease (IBD) characterized by recurring and remitting inflammation which leads to chronic symptoms such as diarrhoea, abdominal pain and rectal bleeding [1]. CD, unlike ulcerative colitis (UC), can affect the lining of the gastrointestinal tract anywhere from the mouth to the anus but most commonly disease is isolated to the terminal ileum, the colon, or the ileum and the colon [1]. CD presents as transmural inflammation, which means that it may affect the whole depth of the intestinal lining, not just the mucosa, as seen in UC. In addition, CD may be present in multiple locations in the bowel with healthy sections of bowel separating them which is referred to as skip lesions. There is currently no known cure for CD and therefore current treatments are focused on minimizing inflammation and extending periods of disease remission.
A decade ago, Canterbury, New Zealand (NZ) had one of the highest incidence rates of CD in the world at 16.5/100,000/year [2]. The incidence and prevalence of IBD is increasing world-wide [3] and NZ is unlikely to be immune from this trend. CD treatment usually involves the use of immuno-modulators (e.g. Azathioprine and Methotrexate), anti-inflammatories (e.g. Mesalazine), biological agents (e.g. Adalimumab and Infliximab) and/or surgery. Exclusive enteral nutrition (EEN) is also used in many paediatric centers to induce disease remission and avoid the side effects of anti-inflammatory medications [4]. However, there is no international agreement about the use of EEN in the treatment of adults [5].
EEN treatment for CD involves the exclusive ingestion of an elemental or polymeric liquid formula for a period of usually six to eight weeks. EEN has been shown to be as efficacious as corticosteroids in treating active disease in children [6]. While EEN is also efficacious in adults with CD, a meta-analysis [7] and a Cochrane review [8] have shown corticosteroids to be superior to EEN on an intention-to-treat basis in adult populations. Reasons for these differences are not clear, but may include the palatability of nutritional formula utilized in early clinical trials with adults, and the inclusion of treatment-naïve patients compared to patients with long standing disease [9].
Poor nutritional status is common in people with CD, particularly during periods of active disease, but also when the disease is in remission [10]. Optimal management of CD requires a multidisciplinary approach involving the gastroenterologist and/or surgeon, specialist gastroenterology nurses, dietitians, psychologists and other specialties [11]. UK and Australian IBD standards of care consider the inclusion of a dietitian in the gastroenterology multidisciplinary team to be essential [11,12] in order to optimize the nutritional status of this nutritionally high risk patient group. Overall, the dietitians' role is to optimize nutritional status through the management of poor oral intake, weight loss, micronutrient deficiencies and control of symptoms, including functional symptoms. In addition, the pediatric dietitian's role is likely to include management of EEN [10]. In NZ patients are often diagnosed and managed by a specialist gastroenterologist in a tertiary center. Dietary outpatient care, however, may be provided by dietitians in tertiary centers, private practice or those working in smaller provincial centers. This research aimed to understand the current role(s) of NZ dietitians in the management of CD patients and to outline their experience with the use of EEN for patients with active CD.
Methods
Participants
All NZ dietitians who were members of the national professional association, Dietitians NZ were contacted by e-mail and invited to complete an electronic survey anonymously. This member group was composed of 488 dietitians working in clinical, public health, research, foods service and pharmaceutical industry settings. A web-based survey link was disseminated via Dietitians NZ's weekly electronic newsletter during August and September 2013. Dietitians were asked to follow an electronic link to the online survey and were reminded to complete the survey three weeks after the initial newsletter advertisement.
Survey design
The survey questions were adapted from a survey used with North American physicians to understand their attitudes and use of enteral nutrition to treat pediatric CD [13]. The survey platform was Question Pro Online Survey Software Application (www.questionpro.com), which contained single choice, multiple choice and open-ended questions. Question branching was included so that dietitians answered only questions relevant to their experience with CD patients and enteral nutrition. The survey was pre-tested with an Australian dietitian who frequently uses EEN to treat CD and a colleague who has experience with online survey design. Their feedback was incorporated into the final version of the survey.
This survey did not require ethical approval; however, the data collected from survey respondents were managed ethically, and anonymity of survey respondents was maintained.
Data analysis
Descriptive statistics including means, standard deviations, ranges and percentage of responses were calculated using Microsoft Excel 2010. Responses from pediatric and adult dietitians were compared using Fisher's exact test and Chi-squared test in Prism 6 version 6.05 (GraphPad Software Inc). Open ended questions were summarized using thematic analysis.
Results
The survey was started by 102 of the 488 active Dietitians NZ members which is a response rate of 21%. Of the 102 dietitians who started the survey, six did not complete it and 25 (25%) did not see patients for gastrointestinal (GI) complaints. The remaining 77 dietitians (16% of the total membership) saw a patient with GI related complaint at least a few times a year and 58 dietitians saw a patient with CD at least a few times a year (Figure 1).
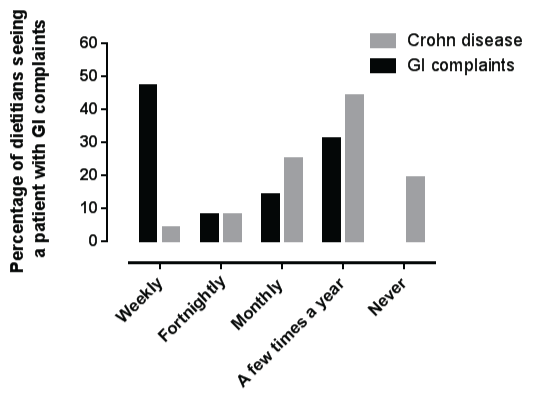
.
Figure 1: Difference in frequency of presentation of patients with Crohn disease and general gastrointestinal complaints (n = 77 dietitians).
View Figure 1
Dietitians who saw patients with CD predominately worked in a public or private hospital (83%) or in a private or publically funded community setting (26%). Ten (17%) dietitians worked in more than one clinical setting. Dietitians had a range of clinical experience; 16% had less than two years of experience, 48% had between two and ten years of experience and 36% had more than ten of experience. At least one dietitian from each region in NZ, except Gisborne, saw patients with CD at least a few times a year. Forty-eight of the dietitians predominately cared for adult patients with CD and 10 dietitians predominately cared for pediatric patients aged less than 16 - 17 years old. The survey did not ask dietitians to specify if they saw both pediatric and adult patients.
The majority of dietitians saw a patient with CD a few times a year (31) and eight dietitians (three pediatric and five adult dietitians) saw at least one patient with CD every fortnight (Figure 1). The dietitians who saw patients with CD more frequently worked in public hospitals in larger centers which have a tertiary hospital. A sub-group analysis found that the frequency of presentation of patients with CD did not differ between pediatric and adult dietitians (χ2 (2, N = 58) = 2.72, p = 0.25). All dietitians commonly received patient referrals for weight loss: 90% of pediatric dietitians and 71% of adult dietitians. However, pediatric dietitians received significantly more referrals for EEN (p < 0.0001) and micronutrient deficiencies (p < 0.004) compared with adult dietitians (Figure 2).
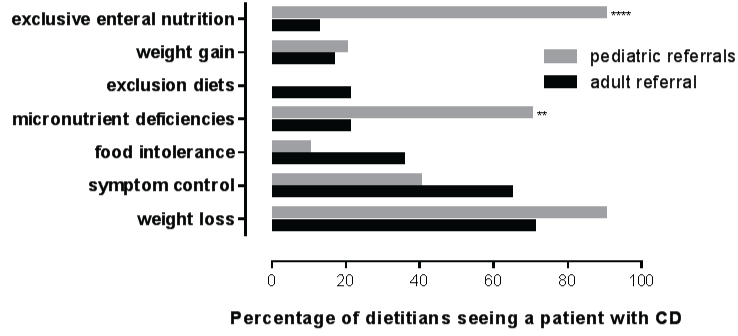
.
Figure 2: Common reasons patients with CD are referred to adult (n = 48) and pediatric dietitians (n = 10)
(**p < 0.01, ****p < 0.0001).
View Figure 2
Most dietitians, 10 (100%) pediatric and 38 (79%) adult dietitians, who saw patients with CD were aware of EEN as a treatment option for active CD. Dietitians were asked whether they believed EEN was an appropriate treatment for their patient group and if there were any disadvantages to the treatment. Five pediatric dietitians and 25 adult dietitians answered these questions. All of the five pediatric dietitians thought that EEN should be offered as a treatment option to selected patients, but that a disadvantage of the treatment is the need for adherence to the regimen. Of the 25 adult dietitians, 20 believed that EEN may be beneficial for selected patients, two thought there was currently insufficient evidence to support its use with adults, and two dietitians were unsure if EEN would be of benefit for their patient group. Thirty (43%) dietitians felt they had adequate knowledge and/or skills to manage a patient referred for EEN. Half of the dietitians would find further professional development on the role of EEN in CD useful. They would also like more EEN patient resources, and more scientific evidence to support the use of EEN with adults, together with professional supervision.
Thirty-five dietitians, 10 pediatric and 25 adult dietitians, reported that they had managed a patient with active CD with EEN. These dietitians were geographically spread across NZ and most (26 dietitians) worked in a public hospital. Seventeen dietitians who worked with adult patients had not managed a patient with CD on EEN, and the main reasons for this included that gastroenterologists and surgeons do not refer patients for EEN treatment (13 dietitians), a limited CD patient case load (9 dietitians) and limited experience using EEN (6 dietitians).
Dietitians' clinical experience of using EEN to treat active CD varied from one to fifty patients with a median of three patients. Ten dietitians (four pediatric, six adult) had used EEN with five or more patients. One of these ten dietitians commented that their experience was gained while working in the United Kingdom, and one was not currently practicing dietetics. The other eight dietitians practiced in main centers. All four pediatric dietitians who had managed at least five patients on EEN found EEN to be a successful treatment to improve disease symptoms. In contrast, five of the six adult dietitians who had managed at least five patients on EEN reported that EEN was only sometimes successful in improving disease related symptoms.
Dietitians who had used EEN with their patients were asked to comment, in an open-ended question, which patients had responded well to EEN. In their experience EEN was most successful for patients who adhered to the treatment, were motivated, did not have complicated disease, had newly diagnosed disease and/or were young adults. However, dietitians indicated that there are barriers to EEN treatment which included the need for treatment adherence (43%), the need for a multidisciplinary approach (14%), the patient needing adequate social support (15%), the cost of enteral formula (11%) and the management of the treatment being more time intensive for the dietitian (8%).
The use of SEN by dietitians' to maintain disease remission was variable: 19% always prescribed it, 40% sometimes prescribed it, 18% rarely or never prescribed it, and 23% said the question was not applicable or did not answer. The prescription of SEN was usually used to treat nutritional concerns rather than as a means of maintaining remission of CD. There was no standard regimen and dietitians tended to use an individualized approach depending on weight, history of weight loss and current oral dietary intake.
Discussion
One of the aims of this research was to understand the role of NZ dietitians in the management of CD patients. This electronic survey suggests that patients with GI complaints frequently present to the NZ dietitians surveyed but patients with CD present much less frequently despite being at risk of poor nutritional status. It is estimated that 1 in 500 to 700 New Zealanders, or approximately 7,000 people, live with CD [14]. Based on the patient caseload of the dietitians which responded to this survey, NZ dietitians manage a small portion of the CD population. A more detailed survey of NZ dietitians would be required to ascertain if IBD service involvement and routine hospital nutritional screening is related to the observed low dietitian CD patient caseload. Regardless, the low exposure of NZ dietitians to patients with CD is concerning given the prevalence of under nutrition and may lead to poorer outcomes for patients.
Another aim of this research was to quantify NZ dietitians' experience of using EEN for active CD. Thirty-five (60%) of the 58 dietitians who see a patient with CD at least a few times a year had used EEN to treat active CD disease. EEN is recommended as a first line therapy to treat active pediatric CD [6], and nine of the ten pediatric dietitians reported commonly receiving referrals for EEN. However, most dietitians, including half of the pediatric dietitians, had managed less than five patients on EEN. Further investigation is required to ascertain if this is the true experience of pediatric dietitians or whether experienced dietitians did not complete or have access to the online survey because they are not members of the national dietetic association.
Six of the 48 adult dietitians (12.5%) commonly received referrals for EEN. One study suggests that adult patients are interested in using EEN as an alternative to corticosteroids [15] and the recent British Dietetic Association dietary guidelines for the management of CD suggest that EEN could be considered as alternative to corticosteroids [16]. Although, American adult CD treatment guidelines make no mention of nutrition [17] and the European guidelines recommend EEN for use with adults if other treatments have failed or are contraindicated or as adjunctive therapy in adults who are nutritionally compromised [18,19]. In NZ, referrals to adult dietitians were lower than was observed in a survey of UK adult acute care dietetic departments where 76/129 (59%) had received a referral for EEN in the last three months [20]. The adult dietitians who commonly received EEN referrals were located in a small number of locations in NZ, whereas the pediatric dietitians which commonly received EEN referrals were spread more evenly across NZ. This observation suggests that referrals to dietitians for EEN may vary between hospitals and/or gastroenterologists which is in keeping with the findings of a survey of North American pediatric physicians. North American physicians were more likely to recommend EEN to their patients if they had worked/trained in a center that commonly used the EEN [13]. The development, or adoption, of national treatment guidelines and EEN protocols may improve discrepancies in the geographical use of EEN in active CD.
This survey explored not only dietitian use of EEN but also their experience managing patients on EEN and their perception of EEN as a treatment for active disease. Dietitians were optimistic about the effectiveness of EEN to induce disease remission. Forty-five percent perceived that EEN was an effective treatment, and 52% felt that it was sometimes successful and was best used with specific groups of patients. Pediatric and adult dietitians' perception of the effectiveness of EEN to induce disease remission did not significantly differ (p = 0.488). Literature suggests that the level of health professional support for patients using EEN is a major contributing factor to the success of the treatment [21], therefore, dietitians' perception of the effectiveness of EEN is important, especially as patients need intensive dietetic support to optimize nutritional intake and minimize intolerance of the nutrition formula. It is likely that the involvement of optimistic and proactive health professionals may affect adherence to the treatment and therefore improve treatment outcomes.
The success of EEN, particularly in adults, is often limited by poor adherence to the treatment [9]. Of the 35 NZ dietitians who have used EEN with their CD patients, 34 stated that the need for treatment adherence was the main disadvantage of EEN treatment. Other disadvantages of EEN included the need for adequate social support and a multidisciplinary approach. North American pediatric physicians also reported compliance as the main disadvantage of EEN treatment [13]. Further, physicians who rarely used EEN reported that the main barriers to prescribing EEN more were the need for treatment adherence followed by lack of social support and lack of experience using EEN [13]. Limited experience with EEN also featured as a barrier for NZ dietitians, followed by gastroenterologists and surgeons not referring patients for EEN treatment. Dietitians identified various strategies to overcome some of these barriers, the most common being that professional development of dietitians, especially for those with limited experience utilizing EEN, is required. Further education would increase dietitian expertise and optimize treatment outcomes for patients with active CD, but also clear treatment protocols and indications for EEN developed in conjunction with the multidisciplinary team would be beneficial.
The main limitation of this survey is whether or not the respondents are representative of pediatric and adult dietitians in clinical practice in New Zealand. Although this survey was disseminated via Dietitians NZ, the national dietetic professional organization, not all clinical dietitians are members of Dietitians NZ. Due to a lack of non-responder data there may a bias towards dietitians who are aware of EEN in the treatment of CD and the results may overestimate awareness and utilization of this treatment. Another limitation is that survey pre-testing was not completed with clinical dietitians who see patients with CD less frequently or limited experience using EEN. Further surveys or audits that target dietetic departments that care for patients with IBD are required to further understand the specific role and utilization of dietitians in tertiary centers that have a high CD patient caseload and also private practice dietitians and dietitians in rural centers who may manage this patient group less frequently.
This survey provides a broad understanding of the involvement of NZ dietitians in the multidisciplinary care of patients with CD. This survey has identified that patients with CD present frequently to a few NZ dietitians in limited centers. NZ dietitians are most likely to see a patient with CD monthly or a few times a year. Most dietitians, pediatric dietitians included, have limited experience managing patients using EEN. Considering the increasing incidence and prevalence of CD, NZ dietitians maybe involved in the multidisciplinary management of only a fraction of the NZ CD population which may lead to poor outcomes for patient's long term.
Acknowledgements
This work was supported by grants the New Zealand Society of Gastroenterology, the New Zealand Federation of Graduate Women and Dietitians New Zealand.
References
-
Baumgart DC, Sandborn WJ (2012) Crohn's disease. Lancet 380: 1590-1605.
-
Gearry RB, Richardson A, Frampton CM, Collett JA, Burt MJ, et al. (2006) High incidence of Crohn's disease in Canterbury, New Zealand: results of an epidemiologic study. Inflamm Bowel Dis 12: 936-943.
-
Molodecky NA, Soon IS, Rabi DM, Ghali WA, Ferris M, et al. (2012) Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology 142: 46-54.
-
Whitten KE, Rogers P, Ooi CY, Day AS (2012) International survey of enteral nutrition protocols used in children with Crohn's disease. J Dig Dis 13: 107-112.
-
Brown AC, Rampertab SD, Mullin GE (2011) Existing dietary guidelines for Crohn's disease and ulcerative colitis. Expert Rev Gastroenterol Hepatol 5: 411-425.
-
Heuschkel RB (2000) Enteral nutrition in children with Crohn's disease. J Pediatr Gastroenterol Nutr 31: 575.
-
Griffiths AM, Ohlsson A, Sherman PM, Sutherland LR (1995) Meta-analysis of enteral nutrition as a primary treatment of active crohn's disease. Gastroenterology 108: 1056-1067.
-
Zachos M, Tondeur M, Griffiths AM (2007) Enteral nutritional therapy for induction of remission in Crohn's disease. Cochrane Database Syst Rev 1: CD000542.
-
Wall CL, Day AS, Gearry RB (2013) Use of exclusive enteral nutrition in adults with Crohn's disease: a review. World J Gastroenterol 19: 7652-7660.
-
O'Sullivan M, O' Morain C (2006) Nutrition in inflammatory bowel disease. Best Pract Res Clin Gastroenterol 20: 561-573.
-
The IBD Standards Group (2015) Standards for the Healthcare of People who have Inflammatory Bowel Disease 2013 Update.
-
Crohn's & Colitis Australia Quality of Care Steering Committee (2015) Interim Australian IBD Standards: Standards of healthcare for people with inflammatory bowel disease in Australia.
-
Stewart M, Day AS, Otley A (2011) Physician attitudes and practices of enteral nutrition as primary treatment of paediatric Crohn disease in North America. J Pediatr Gastroenterol Nutr 52: 38-42.
-
Health Navigator Charitable Trust. Crohn's disease.
-
Wall CL, Gearry RB, Day AS (2014) Polymeric formula is more palatable than elemental formula to adults with Crohn's disease. e-SPEN J 9: e200-e203.
-
Lee J, Allen R, Ashley S, Becker S, Cummins P, et al. (2014) British Dietetic Association evidence-based guidelines for the dietary management of Crohn's disease in adults. J Hum Nutr Diet 27: 207-218.
-
Lichtenstein GR, Hanauer SB, Sandborn WJ, Amer Coll G (2009) Management of Crohn's Disease in Adults. Am J Gastroenterol 104: 465-483.
-
Lochs H, Dejong C, Hammarqvist F, Hebuterne X, Leon-Sanz M, et al. (2006) ESPEN guidelines on enteral nutrition: Gastroenterology. Clin Nutr 25: 260-274.
-
Dignass A, Van Assche G, Leman M, Soderholm J, Colombel JF, et al. (2010) The second European evidence-based consensus on the diagnosis and management of Crohn's disease: Current Management. J Crohns colitis 4: 28-62.
-
Lomer MC, Gourgey R, Whelan K (2014) Current practice in relation to nutritional assessment and dietary management of enteral nutrition in adults with Crohn's disease. J Hum Nutr Diet 27: 28-35.
-
El-Matary W (2009) Enteral nutrition as a primary therapy of Crohn's disease: the pediatric perspective. Nutr Clin Pract 24: 91-97.





