Journal of Hypertension and Management
Prevalence of Hypertensive Emergency in Emergency Room of Rajavithi Hospital
Sumitra Piyanuttapull* and Jaruboot Angsanakul
Emergency medicine department, Rajavithi Hospital, College of Medicine, Rangsit University, Bangkok, Thailand
*Corresponding author:
Sumitra Piyanuttapull, MD, Cardiologist, Department of Emergency medicine, Rajavithi Hospital, College of Medicine, Rangsit University, 2 Phayathai Road, Rachathewi, Bangkok 10400, Thailand, Tel: +66-0-23548087, Fax: +66-0-23545477, E-mail: sumitra.piya@gmail.com
J Hypertens Manag, JHM-2-010, (Volume 2, Issue 1), Research Article; ISSN: 2474-3690
Received: March 08, 2016 | Accepted: April 06, 2016 | Published: April 09, 2016
Citation: Piyanuttapull S, Angsanakul J (2016) Prevalence of Hypertensive Emergency in Emergency Room of Rajavithi Hospital. J Hypertens Manag 2:010. 10.23937/2474-3690/1510010
Copyright: © 2016 Piyanuttapull S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Hypertensive crisis is common among patients visiting emergency room (ER). Majority of these patients can be treated on an outpatient basis (hypertensive urgency). Other patients have acute end-organ damage and higher morbidity and mortality (hypertensive emergency). However, no study on the prevalence of hypertensive emergency in ER in Thailand was found. We aim to evaluate the prevalence and also potential predictors of hypertensive emergency.
Methods: Medical records of patients who have systolic blood pressure > 180 mmHg and/or diastolic blood pressure > 120 mmHg were reviewed. The exclusion criteria include age < 18 years old, near death, a history of recent traumatic event, and a diagnosis of an acute ischemic stroke fast track. The patients were classified into two groups: hypertensive emergency and hypertensive urgency. The prevalence of hypertensive emergency and potential predictors of hypertensive emergency was analyzed.
Results: From June 1, 2013 to August 18, 2014, we found 307 patients with hypertensive crisis and 60 patients (19.5%) were hypertensive emergency. Among several potential predictors of hypertensive emergency, these 3 predictors: dyspnea, dizziness and being transferred from outpatient department (OPD) to ER due to hypertensive crisis were significant.
Conclusion: Hypertensive emergency is common among patients with hypertensive crisis in ER. Dyspnea is a positive predictor of hypertensive emergency. Negative predictors include dizziness and being transferred from OPD to ER.
Keywords
Hypertensive crisis, Hypertensive emergency, Hypertensive urgency, Acute end-organ damage
Background
Hypertensive crisis is common among patient visiting emergency room (ER). Majority of the patients with this condition have few symptoms and no end-organ injury (hypertensive urgency). Other patients with acute end-organ injury are classified as hypertensive emergency [1].
Patients with Hypertensive emergency are usually treated by rapidly decreasing blood pressure approximately 25 percent within two hours in order to prevent further target organ injury resulting in the decline of morbidity and mortality. The most common strategies are intravenous antihypertensive agents while patients with hypertensive urgency can be treated with oral antihypertensive agents on an outpatient basis with close follow up [1].
Hypertensive emergency and hypertensive urgency are differentiated by history, physical examination and appropriate investigation. These may include some special blood tests and also CT scan of the brain. The resources needed to identify hypertensive emergency result in difficulty to the health care providers at the low resource center such as in the primary care centers. Many hospitals in Thailand cannot have many blood test, urine test and X-ray after the office hour. If all patients with hypertensive crisis were treated as hypertensive emergency and referral to tertiary care center was made, it would consume a huge resource and burden to the patient’s family and the public.
In Thailand, the prevalence hypertensive emergency in emergency room is unknown. If we know the prevalence and the proportion of hypertensive emergency to hypertensive crisis, it will make easier to estimate the risk of patients with hypertensive crisis.
Thus, we studied the prevalence of hypertensive emergency of patients in emergency rooms of Rajavithi hospital and we also reviewed and analyzed the potential predictors of hypertensive emergency in patients with hypertensive crisis.
Materials and Methods
Patients
This study was done at the emergency room of Rajavithi hospital, a tertiary care center in Bangkok, Thailand. The hypertensive crisis in this study is defined as systolic blood pressure(SBP) > 180 mmHg or diastolic blood pressure (DBP) > 120 mmHg according to the most recently updated definition of the European Society of Hypertension and European Society of Cardiology (ESH/ESC) [1]. From June 1, 2013 to August 18, 2014, any medical records of the patients visiting emergency department with SBP ≥ 180 mmHg or DBP ≥ 120 mmHg were reviewed. The data of any patients who fulfill eligibility criteria were collected and analyzed. The eligible criteria are shown as table 1.
![]()
Table 1: Eligibility criteria.
View Table 1
Hypertensive emergency is defined as hypertensive crisis with acute end-organ damage, such as acute decompensate heart failure, acute myocardial infarction, aortic dissection, cerebral infarction, intra-cerebral hemorrhage, hypertensive encephalopathy, acute renal failure, hypertensive retinopathy, and eclampsia.
Statistical Analysis
The sample size calculated from equation for estimating infinite population proportion. Based on the proportion of hypertensive emergency in hypertensive crisis in the previous study [3] which found 24%, sample size calculation was 307 cases at alpha error = 0.05 and error 20% of proportion = 0.048.
Data were presented as mean ± standard deviation (SD) or median (range) for continuous variables, and number (%) for categorical variables. The difference in frequencies between patients with hypertensive emergency and hypertensive urgency was analyzed using Chi-square or Fisher’s exact test. Student t-test or Mann-Whitney U test was used to compare continuous variables between two groups. Binary Logistic regression was performed to find factors associated with hypertensive emergency. A p-value less than 0.05 was considered significant.
Ethical issue
This study was reviewed and approved by the ethics committees of Rajavithi hospital and was funded by Rajavithi hospital.
Results
There were 76,079 patients visited emergency room of Rajavithi hospital in the study period. Seven hundred ninety-one patients had SBP ≥ 180 mmHg or DBP ≥ 120 mmHg at the screening blood pressure measurement. The prevalence of patients with hypertensive crisis was 307 patients. Hypertensive emergency was found in 60 of 307 (19.5%). The prevalence rate of hypertensive emergency is 78.87 per 100,000 patients.
Descriptive characteristics of the study population are shown in table 2. The four most common organs injured are acute decompensate heart failure, cerebral infarction, intracranial hemorrhage and acute renal failure, respectively.
![]()
Table 2: Descriptive characteristics of the study population, mean ± SD or number (%).
View Table 2
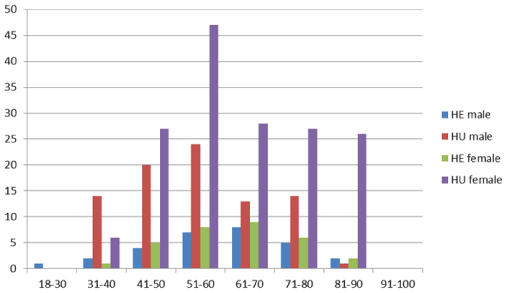
The number of patients with Hypertensive emergency and Hypertensive urgency defined by sex as shown in figure 1.
.
Figure 1: The bar chart shows the number of patients with Hypertensive emergency and Hypertensive urgency, the number of patients (vertical axis) and age (years) (horizontal axis).
View Figure 1
Comparing the hemodynamic parameters between hypertensive emergency (HE) group and hypertensive urgency (HU) group, none of these was significantly different. Symptoms including chest pain, dyspnea and dizziness were also significantly different between the two groups. The characteristics of patients who were transferred from outpatient department (OPD) to ER were also significantly different. Details of the comparison are shown in table 3.
![]()
Table 3: Comparison of the characteristics between groups and hypertensive emergency (HE) hypertensive urgency (HU), mean ± SD or number (%).
View Table 3
When analyzing each factor by Univariate binary logistic regression, 3 predictors were significantly different between hypertensive emergency and hypertensive urgency. Details are shown in table 4.
![]()
Table 4: Predictors of hypertensive emergency and Odds ratios analyzed by binary logistic regression.
View Table 4
Discussion
We found 60 patients with hypertensive emergency in the study period which representing 19.5% of hypertensive crisis. Hypertensive emergency prevalence rate was 78.87 per 100 000 patients. There was no published data on the hypertensive emergency in Thailand to compare with our study. Compared with study from other countries, they found hypertensive emergency accounts for 11.0 - 63.8% of hypertensive crisis [3-9]. In a study of Kat JN et al., hypertensive emergency proportions were low. It probably related to the criteria of hypertensive crisis used (SBP ≥ 180 mmHg or DBP ≥ 110 mmHg) [6]. Vilela-Martin JF et al. found quiet high hypertensive emergency proportion because DBP ≥ 120 mmHg was used to define hypertensive crisis [9]. Merlo C et al. study the hypertensive crisis in the primary care unit and the proportion of hypertensive emergency they found was only 9% [10]. This may be explained by the fact that patients who were seriously ill sometime go directly to the hospital.
In this study, we found 1 positive predictor and 2 negative predictors of hypertensive emergency. Dyspnea is a positive predictor and may be explained by the fact that most common target organ injury is acute decompensate heart failure. Zampaglione B et al., Martin JF et al., and AlBannay R et al. also found that dyspnea is a positive predictor of hypertensive emergency [3,5,7]. Negative predictors include being transferred from OPD to ER and dizziness. The reason why patients who were transferred from OPD to ER have lower risk of hypertensive emergency may because patients who can go to OPD must have better physical capability and less severe symptoms. It also indirectly tells us that some patients know when they are severely ill. Low proportion of hypertensive emergency to hypertensive crisis in the study of Merlo C et al. further confirm our finding because their study was done at primary care unit which comparable to outpatient department [10]. Dizziness was associated with lower risk of hypertensive emergency for unexplainable reason. However, there are many previous studies had the same finding [7-9].
Older Age was associated with increasing risk of hypertensive emergency in some studies [3,7,9]. History of hypertension is significantly different between hypertensive emergency group and hypertensive urgency group in study of Zampaglione B et al. [3]. Few studies found that diabetes was associated with hypertensive emergency [5,7]. Chest pain may indicate ischemic heart disease and some studies have found a positive relationship with Hypertensive Emergency [3,8]. Higher SBP, DBP, mean arterial blood pressure and heart rate were not consistently associated with higher risk of hypertensive emergency [3,4,7,10]. However, we did not find any association of these factors to the type of hypertensive crisis.
In a previous studies and our study, the four most common target-organs injury were acute decompensate heart failure, cerebral infarction, intracranial hemorrhage and acute renal failure, representing more than 70% [3,6-9].
Limitation
First, this study is a retrospective study and some medical records were inaccessible. However, we reviewed medical record of every patient in the study period that fulfills the eligible criteria and we had enough subjects according to the sample size calculation. Thus, the problems described above are unlikely to affect the reliability of the outcome and our analysis.
Second, we excluded the patients who were classified as emergency severity index (ESI) level 1. It may lessen the number of patients with hypertensive emergency because they may severely ill enough to be classified as ESI level 1.
Third, we found quiet small number of patients with hypertensive emergency. This may diminish the validity of the results.
Fourth, the majority of patients in our study are female as shown in Figure 1. This may reflect the truth that women were the predominant patients visiting our emergency room.
In the analysis of potential predictors of hypertensive emergency, the predictors we found still need further evaluation in a prospective cohort study to define accuracy of each predictor because our study is a retrospective study and the predictors may not be recorded in every patient.
The prevalence of hypertensive emergency and proportion of hypertensive emergency from this study can help Thai health care providers in assessing the risk of patients with hypertensive crisis in ER. With the predictors of hypertensive emergency, Thai health care providers will be able to effectively estimate the risk of patients with hypertensive crisis and may result in better outcome.
Conclusion
Hypertensive emergency is common among patients with hypertensive crisis in ER. Dyspnea is a positive predictor of hypertensive emergency. Negative predictors include dizziness and being transferred from OPD to ER.
References
-
(2013) 2013 ESH/ESC Guidelines for the management of arterial hypertension: the Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Journal of Hypertension 31: 1925-1938.
-
Gilboy N, Tanabe T, Travers D, Rosenau AM. (2011) Emergency Severity Index (ESI): A Triage Tool for Emergency Department Care, Version 4. Implementation Handbook 2012 Edition. AHRQ Publication No. 12-0014. Rockville, MD. Agency for Healthcare Research and Quality.
-
Zampaglione B, Pascale C, Marchisio M, Cavallo-Perin P (1996) Hypertensive urgencies and emergencies. Prevalence and clinical presentation. Hypertension 27: 144-147.
-
Al Bannay R, Bohm M, Husain A (2013) Heart rate differentiates urgency and emergency in hypertensive crisis. Clin Res Cardiol 102: 593-598.
-
Al Bannay R, Husain A (2012) Hypertensive crisis: comparison between diabetics and non-diabetics. Int J Cardiol 154: 198-200.
-
Katz JN, Gore JM, Amin A, Anderson FA, Dasta JF, et al. (2009) Practice patterns, outcomes, and end-organ dysfunction for patients with acute severe hypertension: the Studying the Treatment of Acute hyperTension (STAT) registry. Am Heart J 158: 599-606.
-
Martin JF, Higashiama E, Garcia E, Luizon MR, Cipullo JP (2004) Hypertensive crisis profile. Prevalence and clinical presentation. Arq Bras Cardiol 83: 131-136.
-
Pinna G, Pascale C, Fornengo P, Arras S, Piras C, et al. (2014) Hospital admissions for hypertensive crisis in the emergency departments: a large multicenter Italian study. PloS one 9: e93542.
-
Vilela-Martin JF, Vaz-de-Melo RO, Kuniyoshi CH, Abdo AN, Yugar-Toledo JC (2011) Hypertensive crisis: clinical-epidemiological profile. Hypertens Res 34: 367-371.
-
Merlo C, Bally K, Tschudi P, Martina B, Zeller A (2012) Management and outcome of severely elevated blood pressure in primary care: a prospective observational study. Swiss Med Wkly 142: w13507.





