International Journal of Virology and AIDS
Modification of Antiretroviral Therapy in a Cohort Study of HIV-Infected Patients Attending an Urban Teaching Hospital in Kenya
AO Owuor1,2*, GN Lule2, CF Otieno2, EO Omonge2, MC Maritim2 and P Memiah3
1Kenyatta National Hospital, Kenya
2Department of Clinical Medicine and Therapeutics, University of Nairobi, Kenya
3University of Maryland School of Medicine, USA
*Corresponding author: AO Owuor, Senior House Officer, Kenyatta National Hospital, Department of Clinical Medicine and Therapeutics, University of Nairobi, Nairobi, Kenya, Tel: 254722897527; E-mail: andrewowuor@gmail.com
Int J Virol AIDS, IJVA-1-003, (Volume 1, Issue 1), Research Article; ISSN: 2469-567X
Received: October 07, 2014 | Accepted: November 24, 2014 | Published: November 28, 2014
Citation: Owuor AO, Lule GN, Otieno CF, Omonge EO, Maritim MC et al. (2014) Modification of Antiretroviral Therapy in a Cohort Study of HIV-Infected Patients Attending an Urban Teaching Hospital in Kenya. Int J Virol AIDS 1:003. 10.23937/2469-567X/1510003
Copyright: © 2014 Owuor AO, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: To determine the prevalence and factors associated with ART modification among HIV patients on 1st line therapy attending a large Teaching Hospital in Kenya.
Methods: A retrospective cross-sectional clinical record review. All patients who commenced ART from January 2005 to June 2011 and had at least 1 follow-up visit were evaluated. Baseline data, including socio demographic and clinical variables was collected using a standard chart abstraction tool.
Results: Out of 1,022 patients 658 (64.4%) were female and the mean age of study participants was 37.8years. The median CD4+ count at initiating ART was 149cells/ml (IQR 55-248). The most common first-line regimens were stavudine (d4T) and zidovudine (AZT) based at 63% and 13.3% respectively. 1775 patients modified their initial ART at a rate of 36.8% (95% confidence interval [CI] 35.4-38.2%). The commonest reasons for modifying ART were toxicity accounting for 66.5%, treatment failure 12.9%, and co-morbid conditions 9.4%. The most frequent toxic effects were lipodystrophy (41.3%), peripheral neuropathy (10.6%) and anemia (5.9%). The median time to modifying therapy was 28 months (IQR 15-41). Immunological outcome of modification pre and post-modification was 335 cells/ml (IQR 8-497) to 399 cells/ml (IQR 257-611) with p=0.001. In the multivariate analysis WHO clinical stage III (odds ratio [OR], 2.9 [95%CI 1.7-2.8]; p=0.001), and IV (5.5 [2.8-11.0]; p=0.001), CD4+ count =200cells/ml (2.4 [1.5-4.0]; p=0.001) were associated with likelihood of modifying ART.
Conclusion: There was a high rate of ART modification in this study. Drug toxicity was the most frequent reason for treatment modification; however it did not affect treatment success. The median duration to modification of first-line ART was 28 months. Low CD4+ count, increasing WHO stage and longer duration of ART was associated with likelihood of ART modification.
Introduction
The introduction of antiretroviral therapy (ART) has led to significant reductions in Acquired Immune-Deficiency Syndrome (AIDS) related morbidity and mortality [1]. In 2007, the World Health Organization (WHO) estimated that 1 100 000 adults and children were living with Human Immune-deficiency Virus (HIV) in Kenya. Of these HIV-infected individuals, 470 000 persons were estimated to be in need of antiretroviral therapy (ART), of whom only 177 000 (38%) were actually receiving ART [2,3]. As the number of patients starting ART in Kenya continues to rise, numerous medical and logistical challenges have arisen, at both the individual and national levels as only limited antiretroviral drugs are routinely available. These limited options make the modification (switching or substitution) of regimens because of treatment failure, drug toxicities or contraindications a particularly major issue in the scale up of national HIV treatment programs.
Quantifying the frequency of modification of specific regimens while remaining continuously on ART is important as it provides a rough estimate of the rate at which ART regimens are failing or not tolerated. This use of modification remains an important marker of unsuccessful therapies whether due to their inability to control the virus or because of their intolerable adverse effects in a patient's life.
Studies conducted in sub-Saharan Africa have shown that viral suppression and improvement in immune status can be achieved among patients with near-perfect adherence to antiretroviral therapy [4]. It has been observed, however, that prolonged exposure to ART may result in untoward adverse drug reactions, poor adherence, and the emergence of drug-resistant mutants with attendant treatment failure [5,6].
Studies on patients taking proprietary ART from the developed world indicate that 36-44% of patients may modify (switch or substitute) their ART regimen at 1 year of therapy [7]. In these studies, younger female patients, those with a lower CD4 cell count and higher viral load at the start of therapy, those who had previously been treated, and those who were on 4-drug regimens were more likely to modify their ART regimens [5,8,9].
In a study by Messou et al. in 2012 HIV infected adults in Ivory Coast assessing the rate and causes of first ART they found 483 (24%) patients changed treatment in a 2 year follow-up period [10]. A review of AIDS Relief data by Amoroso et al. of 6520 patients, a total of 36% of patients modified ART over a 2year period [11]. A long-term cohort study in Europe found that at 6 years over 80% of patients on treatment had started at least one new drug (substitution) and nearly half had started a new class of drugs (switch) [12].
As durable success is most likely with the first regimen, with sequential regimens leading to progressively less durable and less effective viral suppression, the avoidance of modification of therapy is imperative. Several studies have established the median time to ART modification to occur at approximately one year [8,9]. Kumarasamy in a South India study found a median time to modification of ART of 13 months whereas O'Brien in the USA found a median time of 8 months [8,13] Pallela et al. in a multicenter study in the USA found a median time to initial modification of ART of 11.8 months [14]. Sequential ART regimens were of progressively shorter duration, demonstrated less viral suppression and CD4 cell count benefit, yet low morbidity and mortality rates were sustained [14]. Durable response to ART was associated with being pre-ART therapy naive, prompt response to ART, and protease inhibitor-based initial ART (indinavir or nelfinavir) in this study [14].
The aim of this study was determine the reasons, immunological outcome and predictors of initial modification of HAART among HIV patients at Kenyatta National Hospital (KNH) HIV/AIDS Outpatient Clinic.
Methods
This was a retrospective observational descriptive cross-sectional clinical record review, conducted among HIV positive patients on ART aged 18 years and above, between February and May 2012.. The Kenyatta National Hospital (KNH) provides Comprehensive Care Centre (CCC), which is a HIV/AIDS Outpatient Clinic offering holistic healthcare and the setting for initiation and/or follow-up for patients on ART. A list of all patients on ART from January 2005 to June 2011 was generated from CCC computerized database. Patients with a history of ART modification were then selected and their files and medical records were retrieved from the KNH Central Registry for inclusion into the study. Hence, a total of 4820 patients were enrolled to describe ART modification in an unselected large cohort of cases in the selected hospital. The following data was extracted: Demographic data, ART regimen at initiation and after modification, reasons for modification, patients' CD4+ count, WHO stage at initiation and time to modification of initial ART.
Operational Definition
In this study, any alteration of 1 or more components of a participant's regimen was defined as modification. A change of one or two drugs within a single drug regimen due to drug-related toxicity as well as changes due to drug interactions or contraindications was termed as substitution. Changes of one or two drugs within a single drug regimen or change from an approved first-line ART regimen to an approved second line ART regimen due to treatment failure was defined as a switch.
Immunological responses was defined as the increase in the CD4+ cell count from baseline and the absolute increase in the CD4+ cell count at three to six months post-modification.
Data Management and Analysis
Statistical analysis was done using SPSS version 17.0 (Chicago, IL). Patient demographics were summarized using means, medians and interquartile ranges (IQRs) for continuous variables and counts and percentages for categorical data. Time from ART initiation to modification (substituting or switching any antiretroviral) was presented as a median and interquartile range. Chi-square test was applied for associations between modification, gender and baseline WHO clinical stage. Student-T test and Mann-Whitney U-test were used to compare the mean age and median initial CD4 count respectively between patients whose regimen was modified and those with no modification of therapy. Statistical test with p< 0.05 was considered significant.
The study obtained approval from the Department of Clinical Medicine and Therapeutics (University Of Nairobi) and Kenyatta National Hospital (KNH) Research and Ethics Committee.
Results
Baseline characteristics of the respondents
A list of 1775 patients who had modification of therapy was retrieved from the CCC computerized database of 4820 patients on ART and actively on follow-up. About 1352 patient files were retrieved from the KNH Central Registry of which 107 patients had modified therapy less than six months/follow-up appointment. A further 223 patients' data were missing and incomplete, thus 1022 patients satisfied the inclusion criteria.
As illustrated in Table 1, Male to female ratio in this study was 1:1.8 with the mean age of the patients being 37.8 (IQR 18-77) years. Majority of the patients (61.2%) were at WHO clinical stage II and III of HIV/AIDS. The baseline median CD4+ cell count of the patients' was 149 cells/ml (IQR 55-248) with majority of the patients (63.6%) having a CD4+ less than 200 cells/ml. Demographic characteristics of the excluded patients were similar to the study cohort hence no bias was introduced to the study (Table 1).
![]()
Table 1: Baseline characteristics.
View Table 1
Regimen variability
Of the 1022 patients evaluated, 986 (96.5%) initiated ART with two NRTIs and one NNRTI. Overall, 644 (63%) patients initiated ART with a D4T-containing regimen, of these, 430 (42.1%) were given a fixed-dose combination of stavudine(D4T)/lamivudine(3TC)/nevirapine(NVP) (Figure 1). After modification, majority of the patients 758 (74.2%) were on a Tenofovir (TDF) based regimen. Of these, 460 (45%) were on a fixed-dose combination of TDF/lamivudine(3TC)/efavirenz(EFV), 102 (10%) were on a combination of TDF/3TC/ritonavir boosted lopinavir (LPV/r) as the most common second-line treatment (Figure 2).
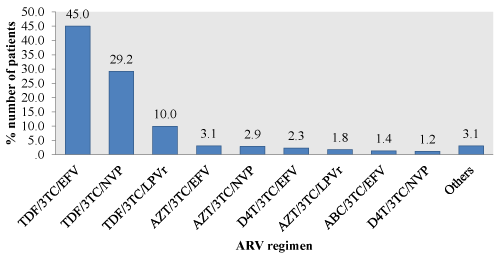
Figure 1: Initial ARV regimen.
View Figure 1
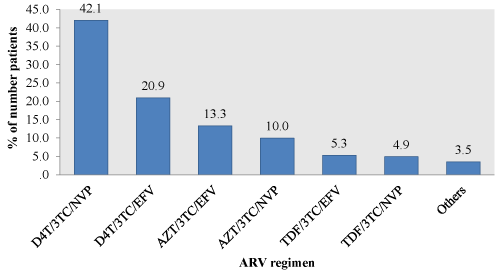
Figure 2: Subsequent ARV regimen.
View Figure 2
Treatment modifications
Overall, 1775 patients had treatment modification, at a rate of 36.8% (95% CI 35.4-38.2) for the initial modification as illustrated in Table 2. Drug substitutions accounted for majority 890 (87.1%) of the modifications with switches accounting for the remaining 132 (12.9%). From this, toxicity related substitutions accounted for 680 (66.5%) of initial treatment modification among patients on ART, 132 (12.9%) with treatment failure 132 (12.9%), 96 (9.4%) co-morbid conditions, 96 (9.4%) and other reasons accounting for 114 (11.2%) of the treatment modifications in the overall population (Table 3).
![]()
Table 2: Prevalence of therapy modification
View Table 2
![]()
Table 3: Modification of regimen.
View Table 3
Specific reasons for modification
The commonest causes of toxicity were lipodystrophy 422 (41.3%), peripheral neuropathy 108 (10.6%) and anemia 60 (5.9%) being the commonest causes of toxicity related therapy modification. Substitution from NVP to EFV related to the initiation of anti-tuberculosis treatment 52 (5.1%) pregnancy-related substitution of EFV to NVP 42 (4.1%) Drug substitutions due to hepatitis B co-infection 2 (0.2%), new guidelines accounted for 82 (8%) whereas lack of stock accounted for 26 (2.7%) of other reasons for therapy modification in the overall study population with modification of therapy (Table 4).
![]()
Table 4: Specific reasons for modification.
View Table 4
Duration of initial regimen
The median time to initial modification of ART was 28 months (IQR, 15-41) and varied according to the reasons for modification. Modification because of toxicity occurred at a median time of 30 months (IQR, 17-41) earlier than modifications due to treatment failure 34 months (IQR, 18.5-45.5). Modifications because of co-morbid conditions median time 20 months (IQR, 4.8-33.5) with Tuberculosis (TB) as a reason for modification with a median time of 5 months (IQR, 1.0-14.5) and pregnancy 20 months (IQR, 12-26) (Table 5).
![]()
Table 5: Duration of initial regimen (n=1022).
View Table 5
Immunological outcome of modification
The overall median CD4+ count at modification of ART was 335cells/ml (IQR, 8-497) with a median rise to 399cells/ml (257-611) post-modification with a p value < 0.001 which was statistically significant (Table 6).
![]()
Table 6: Immunological outcome of modification.
View Table 6
Factors associated with ART modification
In the evaluation of factors that were associated with modification of ART, patients in WHO clinical stage III had 3 times [OR=2.9,(95% CI: 1.7-4.8; p< 0.001] and stage IV had 5 times [OR=5.5, 95% CI: 2.8-11.0; p< 0.001] likelihood to modify their therapy compared to patients at WHO clinical stage I. Similar findings were found in patients with CD4+ counts between 100-200 cells/ml (OR=2.4, 95% CI: 1.5-4.0; p< 0.001) and patients with CD4+ counts < 100cells/ml (OR=4.5, 95% CI: 2.8-7.1; p< 0.001) compared to patients with CD4+ counts >200cells/ml at the time of initiation of ART. Age and gender were not significantly associated with modification of therapy (Table 7).
![]()
Table 7: Factors associated with ART modification.
View Table 7
Discussion
Our study had a young population with a median age of 38.1 years, this compares well with other studies [10,11]. In our study, women comprised the majority (64%) with a male to female ratio of 1:1.8 in keeping with the gender demographic distribution of HIV/AIDS in Kenya.
In this study, 36.8% of the study participants had ever modified one or more components of their initial ART regimen(s). Messou et al. and Amoroso et al. reported 24% and 36% respectively [10,11]. Among antiretroviral drugs, D4T/3TC/NVP or EFV, and AZT/3TC/EFV or NVP therapies were the most frequently prescribed initial ART (86%) and constituted majority of the modifications of ART. These regimens were the first-line therapy as per the National ART Guidelines of 2005 [6]. However, due to their associated cumulative toxicity profile, these regimens have since been changed to newer less toxic regimens, that is, TDF/3TC/EFV or NVP or LPV/r and Abacavir (ABC) based combinations as the recommended first and second-line regimens respectively as suitable for long-term use [7]. On the other hand, the broad availability of new drugs with the possibility of once-daily regimens may have also triggered treatment modification as suggested by the high proportion of patients on TDF/3TC/EFV based regimen post-modification of ART in our study.
In this study, drug side effects or toxicity accounted for more than 65% of the instances of regimen modification, reflecting the known side effects of the drugs. This is consistent with other studies where toxicity accounted for most of the modifications [9-11,13]. The most common reasons of modification in our study were lipodystrophy (41.3%) and peripheral neuropathy (10.3%) mainly due to regimens containing stavudine (D4T). This reflects an improved recognition and identification of the importance of these complications. The availability of newer and better tolerated drugs with limited evidence of long-term adverse effects as alternatives also contributed to the modifications [15].
The strategy of changing individual components of ART in the face of toxicity has been shown to be successful in several studies. Recent data have demonstrated fat recovery in patients with thymidine analogs related lipoatrophy and reduction in D4T and AZT-related dyslipidaemia on switching away from these agents [16]. In this study, modification for lipodystrophy and dyslipidemia (42% of modifications) was more common in patients changing from an initial d4T-containing or AZT-containing ART regimen, which is evidence of the close association between these drugs and lipodystrophy. Clinicians increasingly modified ART early to prevent these toxicities becoming established as evidenced by the 11.2% of patients being modified due to new guidelines.
Regimen modifications due to treatment failure accounted for 12.9% of treatment modifications. In accordance with the current guidelines [7], the majority of patients on a failing NNRTI regimen switched to a PI-based combination. However, failure to obtain a resistance test may lead to inappropriate modification of the ART regimen thus further limiting ART options.
We also found that 9.4% of regimen modifications were related not to toxicity or treatment failure, but rather to co-morbid conditions (pregnancies, tuberculosis and hepatitis B co-infection). In settings with a substantial prevalence of tuberculosis and proportion of HIV-infected women of child-bearing age as ours, both NVP and EFV have a high likelihood of being substituted for each other, for reasons other than toxicity but as a result of drug-drug interactions and potential teratogenicity. Prescribing contraceptives in women taking EFV is part of the solution, though as various studies have shown the rate of pregnancy in women taking contraceptives remains significant [17]. In addition, pregnancy rates in women taking ART will likely increase in the future, as ART helps CD4 cell counts rise with reconstitution of immunity [18].
The median time to modification was approximately 28 months. This study finding may be attributed to limited alternative/second-line ART. Some adverse events may be difficult for patients to understand and report thus infrequent diagnoses and documentation of side effects. This may curtail modification of therapy thus the relatively longer duration of treatment to modification. This is in contrast to reports from the developed world, where most patients modified their therapy at or less than one year mainly due to subtle intolerance such as gastrointestinal intolerance [9,14].
However, within the limitations stated above, the rates of toxicity and times to regimen modification reported here are consistent with those previously reported in sub-Saharan African countries [19]. As expected, D4T based regimen were associated with the highest rate of and longest time to ART modification due to long-term cumulative toxicity. Further findings of this study describe treatment failure dependent time for ART modification being 34 months, pregnancy 20 months and shortest for Tuberculosis at 5 months, which warrant intensive case finding as a stop-gap measure to reduce ART modification. A substantial number of patients, up to 36.8% did have modification of ART at least once in the first 3 years. However, approximately 65% of patients remained on the initial ART regimen over the study period. Boulle in a South African study found 72% of patients were still on their initial regimen at 3 years [20].
Our analysis showed significant improvements in immunological response (defined as increase in the CD4+ cell count from baseline and the absolute CD4+ cell count increase at 3-6 months post-modification). Immunologic outcomes at 3 months were not impaired in individuals with treatment modification regardless of the reason for change. This suggests most patients achieve successful suppression using alternative antiretroviral regimens. There is some evidence that although modification of the initial ART regimen due to intolerance does limit further treatment options, it is not associated with an unfavorable immunologic outcome later [21]. This correlates well with the findings of our study.
In our study increasing WHO clinical stage and low CD4+ cell counts were associated with increased rates of treatment modifications. This signifies an increased likelihood that drug toxicity may have a greater impact on patients in the advanced clinical category than asymptomatic patients. This may be due to the medical condition of advanced HIV patients being poorer as a result of various HIV-related illnesses. A long duration on therapy was also associated with a higher likelihood of modifying ART. This might be interpreted as suggesting that the longer individuals are exposed to antiretroviral drugs, the more likely they are to experience long-term toxicity, treatment failure and co-morbidities.
This study should be interpreted in line with some limitation. Because of the retrospective cross-sectional nature of the study it might be difficult to establish causality and therefore recommend further longitudinal studies and periodic audits of ART utilization. There were no laboratory biomarker results for some of the drug related toxicity. As for the secondary data, review of medical charts revealed some of the variables were incomplete.
Conclusion
ART modification occurred frequently in clinical practice in this centre. The most commonly reported reason for modification of initial ART regimen was long-term toxicity, treatment failure and co-morbid conditions. This study also found that modification of ART occurred late but it did not hinder immunologic outcome of treatment of HIV disease so there is a need to identify individuals at highest risk of drug toxicity, treatment failure or co-morbid conditions. Patients would also benefit greatly from more effective management of modification of ART with the known limits of future treatment options. Intensive case finding of more cases is warranted in patients at highest risk for toxicity and co-morbidities.
References
-
d'Arminio Monforte A, Sabin CA, Phillips A, Sterne J, May M, et al. (2005) The changing incidence of AIDS events in patients receiving highly active antiretroviral therapy. Arch Intern Med 165: 416-423.
-
WHO (2008) Towards Universal Access Progress Report. Scaling up priority HIV/AIDS interventions in the health sector.
-
UNAIDS, WHO (2007) AIDS epidemic update: sub-Saharan Africa regional summary.
-
Wools-Kaloustian K, Kimaiyo S (2006) Extending HIV care in resource-limited settings. Curr HIV/AIDS Rep 3: 182-186.
-
Carr A1, Cooper DA (2000) Adverse effects of antiretroviral therapy. Lancet 356: 1423-1430.
-
(2005) Guidelines for Antiretroviral Drug Therapy in Kenya, NASCOP, Ministry of Health (3rd edn).
-
(2011) Guidelines for Antiretroviral Therapy in Kenya, NASCOP, Ministry of Health (4th edn).
-
d'Arminio Monforte A, Lepri AC, Rezza G, Pezzotti P, Antinori A, et al. (2000) Insights into the reasons for discontinuation of the first highly active antiretroviral therapy (HAART) regimen in a cohort of antiretroviral naive patients. I.CO.N.A. Study Group. Italian Cohort of Antiretroviral-Naive Patients. AIDS 14: 499-507.
-
O'Brien ME, Clark RA, Besch CL, Myers L, Kissinger P (2003) Patterns and correlates of discontinuation of the initial HAART regimen in an urban outpatient cohort. J Acquir Immune Defic Syndr 34: 407-414.
-
Messou E, Anglaret X, Duvignac J, Konan-N'dri E, Komena E, et al. (2010) Antiretroviral treatment changes in adults from Cote d'Ivoire: the roles of tuberculosis and pregnancy. AIDS 24: 93-99.
-
Amoroso A, Sheneberger R, Edozien A, et al. (2007) Causes of Anti-Retroviral Therapy Switch: AIDS RELIEF data. 14th CROI. Los Angeles, Abstract 789.
-
Phillips AN, Dunn D, Sabin C, Pozniak A, Matthias R, et al. (2005) Long term probability of detection of HIV-1 drug resistance after starting antiretroviral therapy in routine clinical practice. AIDS 19: 487-494.
-
Kumarasamy N, Vallabhaneni S, Cecelia AJ, Yepthomi T, Balakrishnan P, et al. (2006) Reasons for modification of generic highly active antiretroviral therapeutic regimens among patients in southern India. J Acquir Immune Defic Syndr 41: 53-58.
-
Palella Jr FJ, Chmiel JS, Moorman AC, Holmberg SD; HIV Outpatient Study Investigators (2002) Durability and predictors of success of highly active antiretroviral therapy for ambulatory HIV-infected patients. AIDS 16: 1617-1626.
-
Gallant JE, Staszewski S, Pozniak AL, DeJesus E, Suleiman JM, et al. (2004) Efficacy and safety of tenofovir DF vs stavudine in combination therapy in antiretroviral-naive patients: a 3-year randomized trial. JAMA 292: 191-201.
-
Moyle GJ, Sabin CA, Cartledge J, Johnson M, Wilkins E, et al. (2006) A randomized comparative trial of tenofovir DF or abacavir as replacement for a thymidine analogue in persons with lipoatrophy. AIDS 20: 2043-2050.
-
Bussmann H, Wester CW, Wester CN, Lekoko B, Okezie O, et al. (2007) Pregnancy rates and birth outcomes among women on efavirenz-containing highly active antiretroviral therapy in Botswana. J Acquir Immune Defic Syndr 45: 269-273.
-
Loko MA, Toure S, Dakoury-Dogbo N, Gabillard D, Leroy V, et al. (2005) Decreasing incidence of pregnancy by decreasing CD4 cell count in HIV-infected women in Cote d'Ivoire: a 7-year cohort study. AIDS 19: 443-445.
-
Forna F, Liechty CA, Solberg P, Asiimwe F, Were W, et al. (2007) Clinical toxicity of highly active antiretroviral therapy in a home-based AIDS care program in rural Uganda. J Acquir Immune Defic Syndr 44: 456-462.
-
Boulle A, Orrel C, Kaplan R, Van Cutsem G, McNally M, et al. (2007) Substitutions due to antiretroviral toxicity or contraindication in the first 3 years of antiretroviral therapy in a large South African cohort. Antivir Ther 12: 753-760.
-
Vo TT, Ledergerber B, Keiser O, Hirschel B, Furrer H, et al. (2008) Durability and outcome of initial antiretroviral treatments received during 2000--2005 by patients in the Swiss HIV Cohort Study. J Infect Dis 197: 1685-1694.





