International Journal of Surgery Research and Practice
A Rare Case of Subtotal Parotidectomy of Bilateral Oncocytomas with Facial Nerve Preservation
Constantinos Aristotelous1, Sofia Georgiou Korsavva2* and Georgios Pantelas3
1Preston Hospital, Lancashire Teaching Hospitals NHS Foundation Trust, England, United Kingdom
2Hairmyres Hospital, Lanarkshire, Glasgow, United Kingdom
3OMFS Clinic, Nicosia General Hospital, Nicosia, Cyprus
*Corresponding author: Sofia Georgiou Korsavva, St George's Medical School London, Cranmer Terrace, London SW17 0RE, Hairmyres Hospital, Lanarkshire, Glasgow, United Kingdom, Tel: 44-0-20-8672-9944, E-mail: sophiadr@live.com
Int J Surg Res Pract, IJSRP-3-045, (Volume 3, Issue 2), Case Report; ISSN: 2378-3397
Received: June 07, 2015 | Accepted: August 31, 2016 | Published: September 02, 2016
Citation: Aristotelous C, Korsavva SG, Pantelas G (2016) A Rare Case of Subtotal Parotidectomy of Bilateral Oncocytomas with Facial Nerve Preservation. Int J Surg Res Pract 3:045. 10.23937/2378-3397/1410045
Copyright: © 2016 Aristotelous C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Oncocytomas are a group of rare tumours of the parotid glands which have benign epithelial origin with incidence about 1% of parotid neoplasms but can exist in many organs. Bilateral non-malignant parotid oncocytomas are very rare. We report the case of a 63-year-old female patient who presented to the outpatients' clinic of Oral and Maxillofacial Surgery (OMFS) service with bilateral facial swelling of one year duration. Clinical examination determined bilateral parotid oncocytoma. Imaging studies revealed hypodense expansive masses on both parotid glands. A biopsy of the nodular lesions confirmed the presence of oncocytoma. The patient was initially treated with right subtotal parotidectomy and preservation of the facial nerve. The tumor of the left parotid was under follow-up due to its slow progression and it has been successfully removed two years after the right parotid oncocytoma. The patient to-date remains in good health and disease free, two years following the left subtotal parotidectomy.
Introduction
Oncocytes are found in many different organs but more often in normal salivary glands. They have intense eosinophilic and granular cytoplasm of epithelial cells and centrally located nuclei with profound chromatin pattern [1]. They appear as the major part in pathological conditions of the salivary glands, including diffuse oncocytosis, multifocal nodular oncocytic hyperplasia (MNOH), oncocytic metaplasia, oncocytomas and oncocytic carcinoma [1].
World Health Organisation (WHO) classifies oncocytomas according to histological approach in three discrete categories; oncocytosis, oncocytoma and oncocytic carcinoma [1,2]. They most frequently occur between 60-80 years of life with a slightly higher prevalence on females and are commonly unilateral [3,4]. They often present as multilobulated or painless, mobile masses of firm consistency. The diagnostic imaging modalities of choice are Computed tomography (CT) or magnetic resonance imaging (MRI) [4,5].
The prevalence of bilateral oncocytomas of the parotid glands is far rarer than the unilateral prevalence [3,4]. However, the clinical and pathological behavior of the tumors is indistinguishable regardless of their incidence whether unilateral or bilateral [6-8]. Only 0.7% of oncocytic neoplasms or other masses present as bilateral oncocytomas and they account for 1% of all parotid tumours [9]. A literature review from the last 30 years revealed less than 20 cases [9,10].
In this case report we discuss the case of a patient with bilateral parotid oncocytomas that were successfully removed in two stages. The patient was followed-up for two years, every 2 months and so far there has been no recurrence of the parotid oncocytomas.
Case Report
A 63-year-old woman presented to our outpatients' clinic of Oral and Maxillofacial Surgery (OMFS) with bilateral parotid swelling. She reported no pain or other abnormality, just the swelling on her parotids. Her past medical history included difficult to control hypertension, cardiac arrhythmias, obesity and hyperthyroidism. Her surgical history include dresection of multiple lipomas from different areas on her trunk and shoulders, total thyroidectomy, and a partial mastectomy due to breast cancer. Her medications included warfarin, antiarrythmics, and thyroxine.
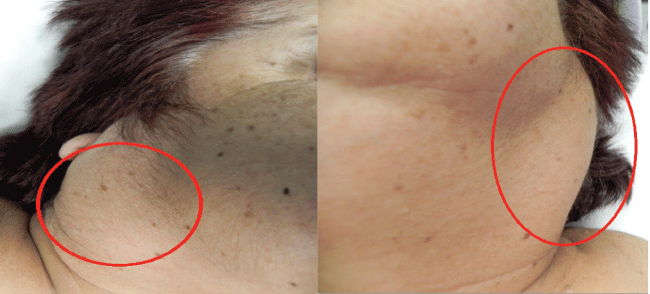
Clinical examination revealed soft tissue swelling with multiple, small and well circumcised small lumps of soft-elastic consistency on both parotids right and left. The drain of saliva from the parotid ducts was normal. The clinical diagnosis was bilateral oncocytoma, however additional diagnostic tests were ordered to confirm this, as this is a very rare type of tumor (Figure 1).
.
Figure 1: Preoperative view of the patient showing the mass over the right and left parotids.
View Figure 1
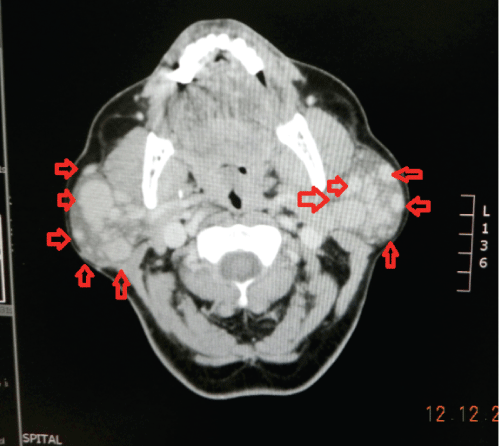
CT revealed multiple hypodense areas on both sides with bilateral multifocal and homogenously enhancing parotid solid masses with well-defined margins involving both the superficial and deep lobes of the parotid glands. Multiple lumps surrounded the outer parenchyma of parotids giving the impression of lymph nodes enlargement. From the imaging results lymphoma was also considered in the differential diagnosis [4,5] (Figure 2).
.
Figure 2: Computed tomography scan (no contrast). Significant bilateral parotid enlargements with increased glandular density (red triangles).
View Figure 2
A fine needle aspiration biopsy (FNAB) was negative for malignancy but it was unclear if it was pleomorphic adenoma. Due to the inadequacy of the FNAB to provide a definitive diagnosis, a core biopsy followed, with a non-definitive result. A nodules lesion biopsy of the right parotid was done and a block of multiple nodules lesions were excised from the gland. The histology showed nodules corresponding to oncocytic neoplasia. The oncocytes had lots of eosinophilic protoplasm and semicircular "homeomorphic" nuclei. The diagnosis was confirmed asoncocytoma of the right parotid. Due to the patient's frailty and her fear of the biopsy procedures, the left parotid gland was biopsied at a subsequent admission, and it also confirmed our initial clinical diagnosis as bilateral parotid oncocytoma.
Because of the benign character of the oncocytoma a follow-up approach on a yearly basis was decided. Subsequently, a year later a second CT showed a stable non progressive character and no further progression of the oncocytoma's solid masses.
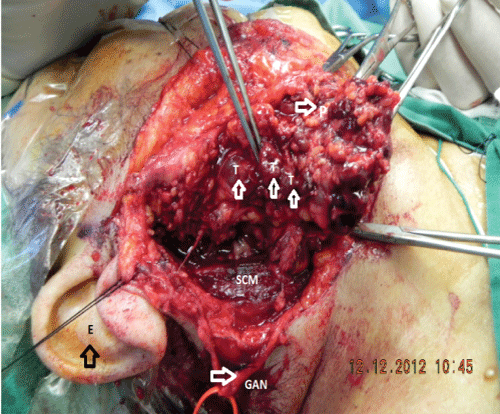
Two years after the initial diagnosis of oncocytoma the patient consented for the removal of her parotid masses due to chronic discomfort by a significant enlarged gland. This was an invasive procedure under general anesthesia. The patient's heart condition and the anticoagulation treatment were managed pre-operatively by the consultant cardiologist. A right subtotal parotidectomy was performed, with a facial nerve branches preservation technique, as the right side was the biggest one and the patient was keen to have this done first. Two years later a left subtotal parotidectomy was performed with a facial nerve branches preservation technique again successfully (Figure 3 and Figure 4).
.
Figure 3: Intraoperative image showing the preserved great auricular nerve (FN) with macroscopic multilobulated tumour invasion (Ts). The superficial lobe of the parotid gland retracted (P). Other structures seen: right ear (E) and sternocleidomastoid muscle (SCM).
View Figure 3
.
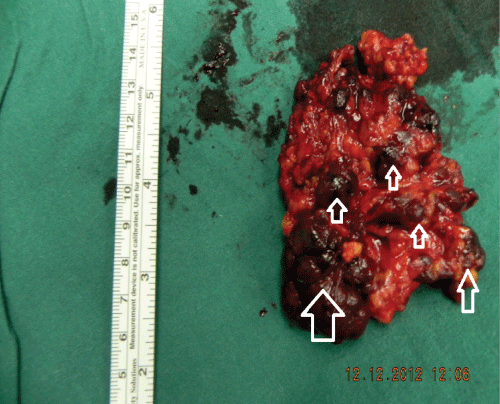
Figure 4: Gross specimen of superficial and deep lobe of the parotid gland after excision. We can notice the multiple nodules attached on the parotid parenchyma (white arrows).
View Figure 4
Post operatively there were no significant complications, with the exception of a mild paresis of the right marginal mandibular branch of the facial nerve. There were no such complications in the left subtotal parotidectomy. Two months later the paresis disappeared and the patient presented with normal movement of the right lip. A close follow-up was suggested every 2 months and the remaining right and left parotidsto-dateremain disease-free.
Discussion
Most of the parotid tumours are mixed benign tumours of 80-90% prevalence, while others are adenoid cystic, mucoepidermoid, acinic cell carcinomas and lipomas [3]. An alteration of the epithelial cells of the salivary gland ducts or acini give a formation of oncocytic cells [1,3]. Their prevalence is between the 6th and the 8th decade of life with a slightly higher affinity in females. These tumors might be seen in other organs such as the nasal thoracic cavities, ovaries, breast, kidney, thyroid, parathyroid, pituitary, larynx and pancreas [1,3].
The term "oncocyte" was first introduced by Hamperl in 1931 whilst the definition of oncocytomas was first defined by Jaffé in 1932 [3,4]. The parotid gland is the most commonly involved organ of salivary gland oncocytomas with incidence around 80% [3,4].
Oncocytomas are rare tumors that constitute less than 1% of salivary gland tumours and account for only about 2% of benign epithelial salivary gland neoplasms [3,6]. The clinical presentation of oncocytomas resembles other benign salivary tumours that present as a firm painless, mobile, multilobulated mass. Histologically a salivary neoplasm is composed of mitochondria-rich epithelial cells [7,8]. A multiphase contrast-enhanced CT could distinguish oncocytomas and offer potentially helpful but nonspecific CT features [8]. The CT features of parotid oncocytomas include a well-defined enhancing tumour of multiple lobules, with cystic component or homogenously enhanced curvilinear cleft [5,6]. These CT findings are potentially helpful in distinguishing oncocytomas from other parotid tumors in the extreme scenarios that preclude surgical resection or when biopsy results are non-diagnostic or inadequate [3,4]. However in our patient's case the CT findings were inconclusive. Due to the low prevalence of oncocytomas, only a few case reports on the CT imaging features are available as publications [8]. The common CT finding of parotid oncocytomas is a well-defined parotid swelling showing homogenous enhancement with differential diagnosis of a Warthin tumour, pleomorphic adenomas, lymphomas or basal cell adenomas [4,8]. Radiological features overlap between oncocytomas and other benign parotid tumours [4,7,8].
A cytological analysis of a parotid mass by an FNAB can be diagnostically informative. Despite the accuracy of the FNAB, some parotid neoplasms are prone to diagnostic error due to inadequate specimen sample or poor histopathological experience. In this case report after the first FNAB a differential diagnosis of pleomorphic adenoma was considered, however the tissue biopsy confirmed our initial clinical diagnosis which was bilateral parotid oncocytoma [8]. FNAB is still the most important diagnostic method for differential diagnosis of all salivary gland lesions with 94-100% specificity and 81-100% sensitivity rates [6].
Complete surgical excision of oncocytomas in the form of superficial or total parotidectomy, depending on the location of the tumour, is the treatment of choice [3,4]. Bilateral parotid tumours which are very rare, can be removed at the same time by a skillful surgeon if symptomatic or malignant. The surgical modality is based on meticulous dissection with preservation of the facial nerves [3,4]. Radiation therapy is not indicated because oncocytes are radio-resistant [4]. Local recurrence for oncocytomas following surgery is uncommon, through recurrence rates of 20-22% have been reported in the literature [6]. Malignancy in oncocytomas is even rarer and accounts for less than 1% of all salivary gland tumours [6]. Our patient remains disease-free two years after the left subtotal parotidectomy was done.
Conclusion
Oncocytomas are usually benign epithelial tumors with prevalence between the sixth and the eighth decades of life. They present with facial swelling and multiple, small and well circumcised small lumps of soft-elastic consistency on the clinical examination and are commonly unilateral. CT and MRI studies are useful to evaluate the extent of their presence and should assess oncocytomas.
Oncocytic neoplasia of the parotid gland is a rare form of salivary gland disease [6]. An FNAB contributes to the confirmation of oncocytic metaplasia and the exclusion of malignancy. In the case of an inadequate specimen from the FNAB further investigations such as a core biopsy should be performed for histological confirmation. Upon histological verification, a subtotal or total parotidectomy should be considered for the eradication of the tumour. Close follow up is suggested to proactively manage recurrence or malignancy. In our case, the CT imaging results were inconclusive for oncocytoma, and the FNAB excluded malignancy but did not reveal if the swelling was oncocytoma. The core biopsy confirmed the clinical diagnosis and the bilateral oncocytoma was successfully removed in two stages due to the patient's frailty. Our patient remains to date disease free, two years later after the left subtotal parotidectomy.
References
-
Sato S, Mitsunobu K, Ogawa Y, Nakatsuka S, Hoshida Y, et al. (2011) Multifocal nodular oncocytic hyperplasia of bilateral parotid glands: A case report with a histological variant of clear cells. Pathol Res Pract 207: 452-455.
-
Vlachaki E, Tsapas A, Dimitrakopoulos K, Kontozoglou G, Klonizakis I (2009) Parotid gland oncocytoma: a case report. Cases J 2: 6423.
-
Sepulveda I, Platin E, Spencer ML, Mucientes P, Frelinghuysen M, et al. (2014) Oncocytoma of the Parotid Gland: A Case Report and Review of the Literature. Case Rep Oncol 7: 109-116.
-
Tan TJ, Tan TY (2010) CT Features of Parotid Gland Oncocytomas: A Study of 10 Cases and Literature review. AJNR Am J Neuroradiol 31: 1413-1417.
-
Shellenberger TD, Williams MD, Glayman GL, Kumar AJ (2008) Parotid Gland Oncocytosis: CT Findings with HIstopathologic Correlation. AJNR Am J Neuroradiol 29: 734-736.
-
Uzunkulaoglu H, Yazici H, Haberal I, Dogan S, Uzunkulaoglu T (2012) Bilateral Oncocytoma in the Parotid Gland. The journal of Craniofacial Surgery 23: 246-247.
-
Mitsimponas KT, Agaimy A, Schlittenbauer T, Nkenke E, Neukam FW (2012) Case report: Oncocytic lipoadenoma of the parotid gland: a report of a new case and review of the literature. Int J Clin Exp Pathol 5: 1000-1006.
-
Patel ND, van Zante A, Eisele DW, Harnsberger HR, Glastonbury CM (2011) Oncocytoma: The Vanishing Parotid Mass. AJNR Am J Neuroradiol 32: 1703-1706.
-
Stomeo F, Meloni F, Bozzo C, Fois V, Pastore A (2006) Bilateral oncocytoma of the parotid gland: Acta Oto-Larynologica 126: 324-326.
-
Mandel L, Carrao V (2005) Bilateral Parotid Diffuse Hyperplastic Oncocytosis: Case report. J Oral Maxillofac Surg 63: 560-562.





