International Journal of Surgery Research and Practice
Approach to Interdigital Pilonidal Sinus: Our Clinical Experience and Literature Review
Vahit Onur Gul1*, Sebahattin Destek2, Ergin Etkin3, Serkan Ahioglu4, Zeynep Tatar5, Serhat Ozer6 and Yesim Erbil7
1Department of General Surgery, Edremit Military Hospital, Balikesir, Turkey
2Department of General Surgery, Tuzla Hospital, Istanbul, Turkey
3Department of Orthopedic Surgery, Edremit Military Hospital, Balikesir, Turkey
4Laboratory, Edremit Military Hospital, Balikesir, Turkey
5Patomer Laboratories, Istanbul, Turkey
6Department of General Surgery, Konya Military Hospital, Konya, Turkey
7Department of General Surgery, Istanbul University, Istanbul, Turkey
*Corresponding author: Vahit Onur Gul, Edremit Military Hospital, General Surgery Department, 10300 Edremit/Balikesir, Turkey, Tel: +905323669227, E-mail: vonurgul@hotmail.com
Int J Surg Res Pract, IJSRP-3-042, (Volume 3, Issue 1), Review Article; ISSN: 2378-3397
Received: March 05, 2015 | Accepted: June 09, 2016 | Published: June 11, 2016
Citation: Gul VO, Destek S, Etkin E, Ahioglu S, Tatar Z, et al. (2016) Approach to Interdigital Pilonidal Sinus: Our Clinical Experience and Literature Review. Int J Surg Res Pract 3:042. 10.23937/2378-3397/1410042
Copyright: © 2016 Gul VO, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Interdigital pilonidal sinus disease, also called "barber's disease," is an acquired occupational disease. Although sacrococcygeal pilonidal sinus disease is a common surgical issue, interdigital pilonidal sinus disease is rare and more likely localized between the fingers and toes. Approximately 50 cases of this disease have been published. However, there are insufficient publications on the incidence of this disease. This disease is caused by the penetration of newly cut, short, and sharp hair through interdigital skin. Although it is known as barber's disease, it can be observed in patients in other professions related to hair and feature cut. Surgical excision is the accepted approach for treating this disease. Because of the complex structure of the hand anatomy and the high overall recurrence rate of pilonidal disease, preoperative determination of the best excision boundaries is important. It is thought that personal hygiene and use of protective measures are essential for preventing interdigital pilonidal sinus disease, which is acquired occupationally. In this study, we explain the importance and methods for prevention, protective surgical approach, and treatment of interdigital pilonidal sinus disease.
Keywords
Barber's disease, Pilonidal sinus, Interdigital pilonidal sinus
Introduction
Sinuses containing hair were observed for the first time by Herbert Mayo in 1830 [1]. The term pilonidal sinus was first defined by Hodge in 1880 using a combination of the words "pilus" for hair in Latin and "nidus" for nest. In addition, Hodge conducted initial investigations on the pathomechanisms that cause the disease. Hodge thought that the disease was caused by vestigial structures resulting from abnormal development of the coccygeal median raphe [2].
The etiology of pilonidal sinus was initially thought to be congenital; however, acquired theories have recently come to the fore. Although the etiology has not been fully clarified, the disease is thought to be mostly caused by the formation of an acute and chronic infection focus under the skin by hair shed from the skin [3]. The theory on the congenital origin of disease was considered until 1946 but was disproved by Patey and Scarff because of the infrequency of pilonidal disease in children [1,2].
The histological structure of interdigital pilonidal sinus disease (IPSD) observed in barbers was defined as a foreign body granuloma for the first time in 1942 by Templeton. The discovery of pilonidal sinus has subsequently been an important step in terms of adoption, and the absence of hair follicles in the skin between fingers has been shown [4]. IPSD is more likely to occur in barbers; however, it can be observed in people from other professions such as dog groomers, upholsterers, milkmen, and wool shearers. These cases are also known as "sheep shearer's disease" or "milkman granuloma" and are caused by dog and goat hair exhibiting the same mechanism [5-9]. Although approximately 50 case reports have been published, no comprehensive study has been conducted on barber's disease, which is described as IPSD [10-15]. In this study, we review barber's disease by compiling our clinical experience together with other published studies.
Discussion
Etiopathogenesis
IPSD was first described by Allington and Templeton in 1942 [4,16]. It is characterized by the formation of foreign body granulation through both the dermis and epidermis layers of the skin. The microscopic absence of a cyst wall and the true epithelium in excised tissue is the most important evidence that the disease does not develop from congenital tissue residues. Karydakis suggested that the disease develops by free hair invading vulnerable skin areas. IPSD is now generally accepted as an acquired disease independent of body location [16-19].
In addition, IPSD is known as an occupational disease among barbers because the sinuses develop a foreign body reaction against customers' hair. The disease is generally located in the interdigital spaces; however, it may occur in other parts of the body, including the finger pulp, palms, and periungual or subungual regions. Furthermore, it has been rarely detected in other areas such as the penis, scalp, axilla, abdomen, neck, and groin areas [20-25]. Interdigital pilonidal sinus is rarely observed on the foot but can be caused by wearing open sandals during a haircut; only two cases have been reported in the literature [26,27]. This disease can also be observed in different regions in the same patient. Jochims and Brandt presented a case of pilonidal sinus found on all interdigital areas of both hands [28].
Although the number of female hairdressers working with men's hair worldwide has increased recently, male hairdressers traditionally constitute the main patient population [29]. Patel et al. retrospectively examined 24 cases reported in the literature and noted that all patients who developed pilonidal sinus were male [25]. Moreover, the disease has been diagnosed in three females who were working as professional dog groomers [5,6,8].
Histopathology
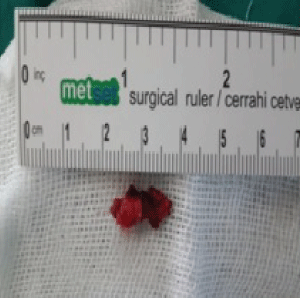
Samples collected from cases reported in the literature revealed different colors and thicknesses, suggesting that the interdigital pilonidal sinus does not contain a patient's own hair, unlike the case when the disease develops in the sacrococcyx, umbilicus, chest, anal canal, ear, and scalp [22,29-31]. This disease is initiated by short, thick, and sharp hair penetrating the skin of the interdigital sulcus. The disease progresses with the formation of a sinus and eventually a cyst. The collection of short hairs in the sinus results in inflammation and the formation of classical pilonidal sinus disease.
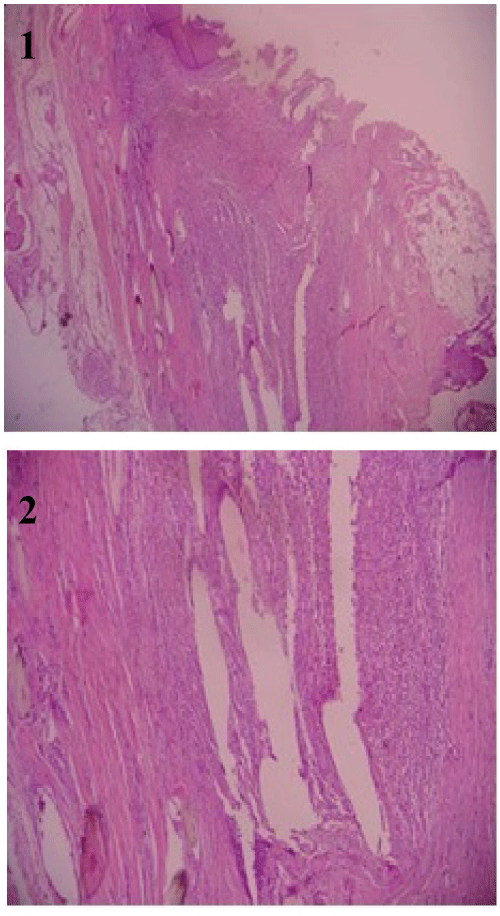
IPSD is mostly observed in male hairdressers serving male customers. Only male hair is hard, thick, and dense enough to pierce the epidermis. Men's hair is shorter, thicker, harder, and sharper than women's hair, and these features consequently facilitate its penetration. In contrast, female hair is commonly long, thin, and soft; therefore, it cannot penetrate the interdigital space [7,29,32]. Although healthy skin generally protects against physical damage and environmental factors, there are a few conditions when hair may penetrate the subcutaneous layer. First, hair undergoes structural changes during a haircut; therefore, it may become sharp as needles. Second, hair that is cut in a barber shop becomes stickier because of increased moisture and electrostatic features of the hair. Third, the development of the hair cuticle in the form of a tile gives a hook feature to hair. The epidermis is very thin, and moisturizers and shampoos routinely used by hairdressers can easily create discomfort in this area. In contrast, hair is generally collected in the crotch region [33]. Histological studies on samples of pilonidal sinus disease reveal that hair fragments that penetrate the skin are first surrounded by nonspecific inflammatory infiltrate and granulomas and then develop a foreign body granulomatous reaction. Therefore, sinuses or pseudo hair follicles that consist of keratin-like material are formed or wounds in the skin are tapered with the epithelium. Subsequently, a cyst-like mass forms in the dermis and may or may not be connected to the skin surface. All reaction phases can be determined by a histological examination of the affected skin area because of the nature of the chronic inflammatory process [33-36] (Figures 1 and Figure 2).
.
Figure 1: Hematoxylin-Eosin.
Figure 2: Hematoxylin-Eosin, × 40.
Histological examination.
Fibrosis and multinucleated giant cells located within the dermal tissue support around the free hair bodies. Participation of an active chronic inflammatory reaction characterized by an intense pilonidal sinus tract.
View Figure 1 and 2
Clinical and preoperative approach
The main disease symptoms include spontaneous drainage of hair pieces from inflamed cysts, pain, swelling, erythema, and a purulent exudates [29,30,34,37]. Pilonidal sinuses are usually asymptomatic. Most cases of non occupational pilonidal sinus disease are not recognized by the patient. Because of the asymptomatic disease progression and failure to treat patients, the true incidence of the disease remains unclear. Another reason why the disease incidence has remained unclear is the low level of doctors' awareness of the disease [29,33,38]. Currie et al. [34] suggested that the diseases rate is approximately 13% among male hairdressers. Similarly, the disease prevalence rate was proposed to be 13% in male barbers in another study [34]. Both these studies were conducted in the 1950s, and no current data are available.
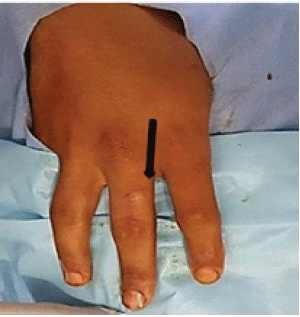
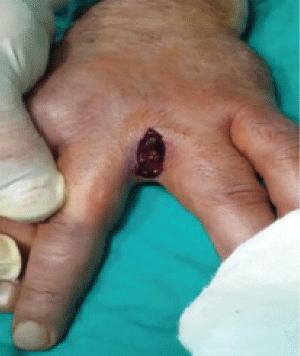
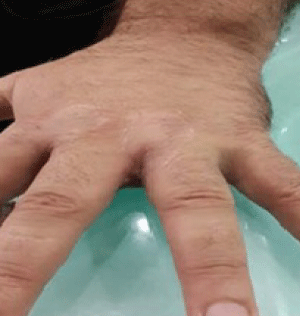
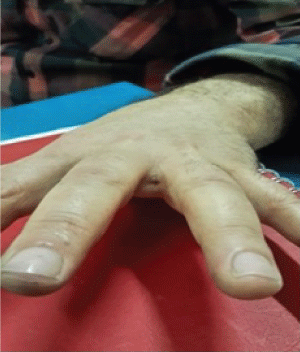
We experienced two patients with pilonidal sinus developed in a rare location. One of the patients had been working as a hairdresser for 7 years, and a pilonidal cyst was identified on the proximal dorsal part of the third finger of his right hand (Figure 3). The other patient had been working as a hairdresser for 25 years and had the same complaints he had from his first operation on the first interdigital space of the right hand in 2003. A second operation was performed on the second interdigital web of the left hand in 2007, and he underwent a third operation on the second interdigital space of the right hand in 2011. In addition to the previous three operations, the patient underwent a fourth operation in our clinic with a diagnosis of IPSD in the third and fourth interdigital spaces of the left hand (Figure 4).
.
Figure 4: Interdigital pilonidal sinus disease in the third interdigital space of the left hand.
View Figure 4
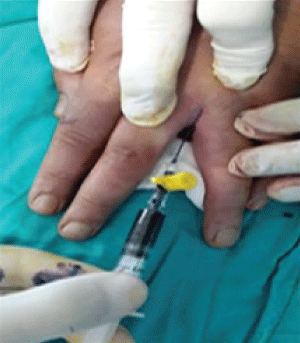
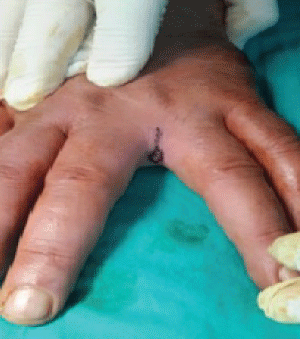
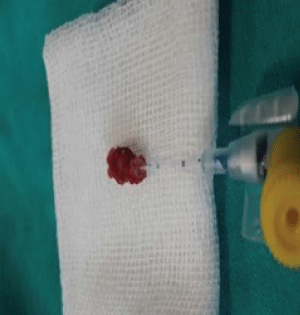
Damaged tissue should be completely excised to avoid the recurrence of pilonidal sinus disease. Therefore, preoperative or intraoperative determination of surgical margins is extremely important to reduce loss of function in patients. Two main approaches are used to determine excision boundaries: preoperative depth measurement of the lesion with a stile and injection of methylene blue to intraoperatively determine the resection site [29,32] (Figures 5 and Figure 6). In addition, fistulography may be useful to determine the surgical boundaries in complicated cases of a fistula or when the margins cannot be detected by traditional approaches [29].
Imanish et al. suggested that ultrasonography, patient history, and physical examination improve the diagnostic certainty of IPSD and help determine areas requiring surgery to completely eliminate the disease [39].
Good hemostasis is required to better visualize the complicated anatomic structure of the hand during the surgical procedure. In particular, surgery with local anesthesia does not provide adequate hemostasis in the interdigital space and may cause tissue edema that will likely prevent surgical exposure. Anesthetic techniques controlled with a tourniquet, such as regional intravenous anesthesia, may be preferred to provide adequate hemostasis and a comfortable and safe surgical intervention in these patients [40-42].
Compared with other pilonidal sinus diseases, IPSD most frequently appears in the hand. Therefore, the surgeon should be knowledgeable of the hand anatomy. Deep and superficial transverse metacarpal ligaments, blood vessels, nerves, and the digital extensor mechanism are at risk during IPSD surgery. Knowledge of the local anatomy, determination of the boundaries during surgery, and a sensitive approach to tissues in the exposed area will reduce the incidence of unwanted complications. Unrequired tissue resection may cause damage to anatomical structures. Notably, intermetacarpal and metacarpophalangeal joint instability can be caused by transverse metacarpal ligament damage and digital vasculo-neural injury may result in circulatory complications, including local and superficial necrosis and gangrene, or neurologic deficits, including hypoesthesia and total axonal degeneration [43-45].
Treatment and prevention
There is no consensus on disease treatment. In 1955, Powell stated that conventional protection is insufficient [46]. Traditional treatment approaches include ineffective methods such as removing hair from sinuses, draining exudate, and administering antibiotics. Total excision of the sinus tissue is considered the most effective treatment method for the disease [5,29,36,47,48]. However, Schroder et al. proposed that IPSD can be completely treated by removing embedded hair [49].
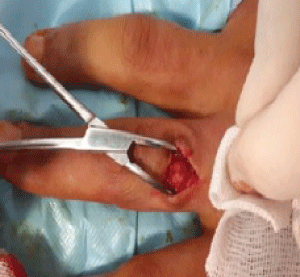
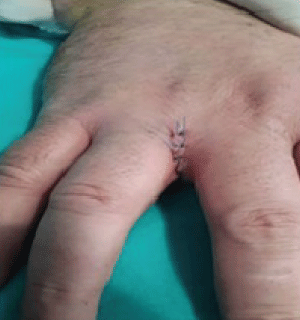
A common treatment approach is to remove the cyst, followed by primary closure (Figures 7, Figure 8, Figure 9 and Figure 10). Although a lower recurrence rate is reported with secondary healing after excising the cyst, there are a number of disadvantages, including the formation of scar tissue and prolonged recovery time [5,25,29,30,32,48,50]. In addition, Efthimiadis et al. suggested that surgical excision, curettage, and primary closure are safe treatment methods [51]. At present, closure of a defect that develops after surgical excision with a flap is quite a popular approach, particularly in patients with sacrococcygeal pilonidal disease. Furthermore, positive results have been proposed by some clinicians after applying a rotation flap to repair skin defects caused by excision. However, other studies have suggested that flaps should only be used to repair cases with a fistula, recurrence, or wide excision [29,36,52-54].
In addition to recurrence, major IPSD complications include the formation of an abscess or fistula, cellulitis, lymphangitis, and osteomyelitis [5,8,55-57]. Moreover, osteolysis of the finger pulp and osteitis of the distal phalanx of the third finger have been reported [20,22]. Although sacrococcygeal pilonidal disease has a high recurrence rate, the recurrence rate of IPSD remains unclear. Patel et al. reported only two recurrences in 24 patients [25]. Some studies suggest that limited excision of the pilonidal sinus tract is a better treatment option then a wide excision to prevent recurrence, decrease recovery time, and increase patient compliance. In a retrospective study of 257 patients with sacrococygeal pilonidal sinus, Soll et al. suggested that sinusectomy with minimally invasive excision is an important alternative to methods including a flap and secondary wound healing for a low rate of recurrence [58]. In our clinic, two patients underwent surgery for IPSD using excision and primary closure, and no recurrence was observed during follow-up. Although the patients suffered from skin tightening during the initial postoperative period, this complaint disappeared within 2 weeks (Figures 11 and Figure 12).
The best method to treat this disease and prevent recurrence is protection. A number of protective methods, including regular cleaning of interdigital spaces, removal of spilled hair, use of protective creams, use of open-ended gloves, and washing of hands after every haircut, have been suggested by researchers [27,29,32,59]. One of our patients has been a barber for 25 years. This patient developed IPSD four times at different locations in both hands. The patient stated that he began to use gloves with protective cream after the second operation in 2007, despite having difficulties in cutting hair. Nevertheless, IPSD developed in two different interdigital spaces in this patient at 3-year intervals. Therefore, the protective methods suggested in the literature need to be reconsidered and further developed. Moreover, new lesions developed in our patient on parts of the hand that were different from the excised areas. In other words, unique IPSD developed in the patient each time, and no recurrence was observed. Granulation tissue that develops in the wound during the postoperative period eventually becomes scar tissue containing inactive fibroblasts, intensive collagen fibrils, elastic tissue fragments, extracellular matrix, and a few vessels [60]. Hair and feathers cannot easily penetrate scar tissue that develops in interdigital spaces. Thus, the formation of scar tissue after surgery may explain the development of the disease in different parts of the hand.
Conclusion
IPSD is an acquired, rare, but avoidable occupational disease that prevents patients from working until complete recovery. Preventing disease recurrence and postoperative complications are important.
The preventive recommendations provided in the literature are not practical for hairdressers because they work with their hands in a wet environment. We suggest that barbers clean their interdigital spaces regularly and clean and remove hair stuck under the skin. Unfortunately, an insufficient number of studies have been conducted to determine disease prevalence. It appears that patients and physicians do not have an adequate level of awareness of this disease.
Competing Interests
The authors declare no competing interests. Permission was obtained from the patients to use their information.
References
-
Patey DH, Scarff RW (1946) Pathology of postanal pilonidal sinus; its bearing on treatment. Lancet 2: 484-486.
-
Hodges RM (1880) Pilo-nidal sinus. Boston Med Surg J 103: 485-6.
-
Bascom J (1980) Pilonidal disease: origin from follicles of hairs and results of follicle removal as treatment. Surgery 87: 567-572.
-
Templeton H (1942) Foreign body granuloma or interdigital cyst with hair formation. Arch Dermatol Syph 46: 157-158.
-
Adams CI, Petrie PW, Hooper G (2001) Interdigital pilonidal sinus in the hand. J Hand Surg Br 26: 53-55.
-
Papa CA, Ramsey ML, Tyler WB (2002) Interdigital pilonidal sinus in a dog groomer. J Am Acad Dermatol 47: S281-282.
-
Patel MR (1982) Green's Operative Hand Surgery. In: Green DP, Hotchkiss RN, Pederson WC, Churchill Livingstone, Philadelphia.
-
Ito A, Yoshida Y, Yamamoto O (2013) Case of interdigital pilonidal sinus in a dog groomer. J Dermatol 40: 1051-1052.
-
Vaiude P, Dhital M, Hancock K (2011) A true pilonidal sinus in the hand of a sheep shearer. J Surg Case Rep 2011: 6.
-
Grobe JW (1978) Pilonidal sinus in a hairdresser. Derm Beruf Umwelt 26: 190-191.
-
King ES (1949) The intedigital pilonidal sinus. Aust N Z J Surg 19: 29-33.
-
Peter J Stern , Charles A Goldfarb (2004) interdigital pilonidal sinus. New Eng J Med 350: e10.
-
Ibáñez AT, Lara IE, Serrano AC, Padrós FJR, Marturet AJG (2011) Sinus pilonidal interdigital. Una rara enfermedad professional. Revista Española de Cirugía Osteoarticular 246.
-
Stolp A (1970) Interdigital pilonidal sinus on both hands. Dermatol Monatsschr 156: 16-22.
-
Oldfield MC (1956) A barber's interdigital pilonidal sinus. Lancet 271: 1244-1245.
-
Allington H (1942) A case for diagnosis (foreign body reaction?). AMA Arch Derm Syphilol 45: 614-665.
-
Joseph HL, Gifford H (1954) Barber's interdigital pilonidal sinus: the incidence, pathology, and pathogenesis. AMA Arch Derm Syphilol 70: 616-624.
-
Søndenaa K, Pollard ML (1995) Histology of chronic pilonidal sinus. APMIS 103: 267-272.
-
Karydakis GE (1992) Easy and successful treatment of pilonidal sinus after explanation of its causative process. Aust N Z J Surg 62: 385-389.
-
Grant I, Mahaffey PJ (2001) Pilonidal sinus of the finger pulp. J Hand Surg Br 26: 490-491.
-
Kovalcik PJ (1973) Relevancy of the barber's interdigital pilonidal sinus. JAMA 224: 1650.
-
Mohanna PN, Al-Sam SZ, Flemming AF (2001) Subungual pilonidal sinus of the hand in a dog groomer. Br J Plast Surg 54: 176-178.
-
Ngan PG, Varey AH, Mahajan AL (2011) Periungual pilonidal sinus. J Hand Surg Eur Vol 36: 155-157.
-
Sion-Vardy N, Osyntsov L, Cagnano E, Osyntsov A, Vardy D, et al. (2009) Unexpected location of pilonidal sinuses. Clin Exp Dermatol 34: e599-601.
-
Patel MR, Bassini L, Nashad R, Anselmo MT (1990) Barber's interdigital pilonidal sinus of the hand: a foreign body hair granuloma. J Hand Surg Am 15: 652-655.
-
O'Neill AC, Purcell EM, Regan PJ (2009) Interdigital pilonidal sinus of the foot. Foot (Edinb) 19: 227-228.
-
Rubio C, Feito M, Martin MA, Vidaurrazaga C, Ruiz E, et al. (2008) Interdigital pilonidal sinus in the foot. Clin Exp Dermatol 33: 656-657.
-
Jochims J, Brandt KA (1998) Interdigital pilonidal sinus ("barber's disease")--a rare occupational disease. Chirurg 69: 1280-1281.
-
Uysal AC, Orbay H, Uraloglu M, Sensoz O, Hyakusoku H (2007) Rare occupational disease of hair dressers: interdigital pilonidal sinus. J Nippon Med Sch 74: 364-366.
-
Ballas K, Psarras K, Rafailidis S, Konstantinidis H, Sakadamis A (2006) Interdigital pilonidal sinus in a hairdresser. J Hand Surg Br 31: 290-291.
-
Eryilmaz R, Sahin M, Okan I, Alimoglu O, Somay A (2005) Umbilical pilonidal sinus disease: predisposing factors and treatment. World J Surg 29: 1158-1160.
-
Eryilmaz R, Okan I, Ozkan OV, Somay A, Ensari CO, et al. (2012) Interdigital pilonidal sinus: a case report and literature review. Dermatol Surg 38: 1400-1403.
-
Rockl H, Muller E (1957) Hairs causing granuloma and fistula. Dermatol Wochenschr 136: 912-916.
-
Currie Ar, Gibson T, Goodall Al (1953) Interdigital sinuses of barber's hands. Br J Surg 41: 278-288.
-
Goodall P (1961) The aetiology and treatment of pilonidal sinus. A review of 163 patients. Br J Surg 49: 212-218.
-
Biondo V, Bastianini S, Cassarà V, Baio T, Cutuli P, et al. (2007) "Barber's hair sinus": new clinical observation. G Ital Med Lav Ergon 29: 802-803.
-
Zerboni R, Moroni P, Cannavo SP, Monti M (1990) Interdigital pilonidal sinus in barbers. Med Lav 81: 138-141.
-
Stern PJ, Goldfarb CA (2004) Images in clinical medicine. Interdigital pilonidal sinus. N Engl J Med 350: e10.
-
Imanishi H, Tsuruta D, Nomura N, Nakagawa K (2012) Clinical usefulness of ultrasonography in interdigital pilonidal sinus. J Cutan Med Surg 16: 194-196.
-
Bell MS, Reitsma BJ (2005) Solo hand surgery. Can J Plast Surg 13: 145-147.
-
Lalonde D, Martin A (2013) Epinephrine in local anesthesia in finger and hand surgery: the case for wide-awake anesthesia. J Am Acad Orthop Surg 21: 443-447.
-
Ralte P, Selvan D, Morapudi S, Kumar G, Waseem M (2010) Haemostasis in Open Carpal Tunnel Release: Tourniquet vs Local Anaesthetic and Adrenaline. Open Orthop J 4: 234-236.
-
Vargas A, Chiapas-Gasca K, Hernández-Díaz C, Canoso JJ, Saavedra MÁ, et al. (2012) Clinical anatomy of the hand. Reumatol Clin 8: 25-32.
-
Bade H, Schubert M, Koebke J (1994) Functional morphology of the deep transverse metacarpal ligament. Ann Anat 176: 443-450.
-
Al-Qattan MM, Robertson GA (1993) An anatomical study of the deep transverse metacarpal ligament. J Anat 182: 443-446.
-
Uysal AC, Alagoz MS, Unlü RE, Sensoz O (2003) Hair dresser's syndrome: a case report of an interdigital pilonidal sinus and review of the literature. Dermatol Surg 29: 288-290.
-
Powell HD (1956) Interdigital sinuses in barber's hand. Br J Surg 43: 520-521.
-
Stern PJ, Goldfarb CA (2004) Images in clinical medicine. Interdigital pilonidal sinus. N Engl J Med 350: e10.
-
Schroder CM, Merk HF, Frank J (2006) Barber's hair sinus in a female hairdresser: uncommon manifestation of an occupational dermatosis. J Eur Acad Dermatol Venereol 20: 209-211.
-
Ivance DW, Lubahn JD (1999) Interdigital pilonidal cyst. Hosp Physician 50-52
-
Efthimiadis C, Kosmidis C, Anthimidis G, Grigoriou M, Levva S, et al. (2008) Barber's hair sinus in a female hairdresser: uncommon manifestation of an occupational disease: a case report. Cases J 1: 214.
-
Aydin HU, Mengi AS (2010) Recurrent interdigital pilonidal sinus treated with dorsal metacarpal artery perforator flap. J Plast Reconstr Aesthet Surg 63.
-
Battiston B, Artiaco S, Antonini A, Camilleri V, Tos P (2009) Dorsal metacarpal artery perforator-based propeller flap for complex defect of the dorsal aspect in the index finger. J Hand Surg Eur Vol 34: 807-809.
-
Gregory H, Heitmann C, Germann G (2007) The evolution and refinements of the distally based dorsal metacarpal artery (DMCA) flaps. J Plast Reconstr Aesthet Surg 60: 731-739.
-
Metz J (1970) Osteormyelitis of the little toe as a consequence of an interdigital pilonidal sinus in an repeolsterer. Z Haut Geschlechtskr 45: 463-470.
-
Meneghini Cl, Gianotti F (1964) Granulomatosis Fistulosa Interdigitalis of Milkers' Hands. Dermatologica 128: 38-50.
-
Phillips PJ (1966) Web space sinus in a shearer. Med J Aust 2: 1152-1153.
-
Soll C, Dindo D, Steinemann D, Hauffe T, Clavien PA, et al. (2011) Sinusectomy for primary pilonidal sinus: less is more. Surgery 150: 996-1001.
-
André A, Mansat P, Gaston A (2007) The hairdresser hand: clinical aspect of pilonidal sinus. Report of 3 cases. Chir Main 26: 218-220.
-
Skalli O, Gabbiani G (1988) The biology of the myofibroblast relationship to wound contraction and fibrocontractive diseases. In: Clark R.A.F., Henson P.M., The molecular and Cellular Biology of Wound Repair. Plenum Publishing, New York.