International Journal of Surgery Research and Practice
Anti-Rotational Plates with Intramedullary Nailing Stabilize Femoral Shaft Fracture Nonunion: A Biomechanical Study
Xianzhi Ma1, Manyi Wang1, Bosong Zhang2*, Zhendong Wang2, Yunbang Lang2 and Xiaofeng Gong2
1Medical Center Tsinghua University, Beijing, China.
2Orthopaedic Trauma Center of Jishuitan Hospital, The Teaching Hospital of Tsinghua University, Beijing, China.
*Corresponding author: Bosong Zhang, MD, Department of Orthopedics Trauma, Beijing Jishuitan Hospital of China, Xinjiekou Street No. 31, Xicheng District, Beijing, 100035, China, Tel: 136-21219567, Fax: 010-58516158, Email: zhangbosong@sina.com
Int J Surg Res Pract, IJSRP-2-034, (Volume 2, Issue 2), Research Article; ISSN: 2378-3397
Received: August 05, 2015 | Accepted: December 24, 2015 | Published: December 28, 2015
Citation: Ma X, Wang M, Zhang B, Wang Z, Lang Y, et al. (2015) Anti-Rotational Plates with Intramedullary Nailing Stabilize Femoral Shaft Fracture Nonunion: A Biomechanical Study. Int J Surg Res Pract 2:034. 10.23937/2378-3397/1410034
Copyright: © 2015 Ma X, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objectives: The purpose of this study was to determine the biomechanical effects of treating femoral shaft fracture nonunion with an anti-rotation plate (AP) in addition to intramedullary nailing (IM) to provide a theoretical basis for their clinical application.
Methods: Twenty-five synthetic bones were divided into the experimental (IM + AP, n = 20) and control (IM, n = 5) groups. The experimental group included four subgroups based on the number of screws and fixation method: IM + AP with two (C2 group) or three (C3 group) bicortical common screws and IM + AP with two (L2) or three (L3) unicortical locking screws. The experimental model was constructed in which their ends were embedded in the embedding apparatus. At last, the specimens were affixed to the mechanical testing system. Torsion testing was performed until each specimen's failure, while their torsional angle and torque values were recorded. All the data obtained have been analyzed by SPSS 10.0.
Results: 1. The mean value of the anti-torsional strength in the IM + AP group was greater than that in the IM group (0.01 < P < 0.05), which was statistically significant.
2. Based on the comparisons between the subgroups of IM+AP, the mean values of anti-torsional strength didn't show much difference. However, when the torsion angle turned to 25°, the mean value in the C3 group was greater than the C2 group (0.01 < P < 0.05) which was statistically significant. When the torsion angle turned to 5°, 10°, 25°, the mean value in the L3 group was greater than the L2 group (0.01 < P < 0.05) which was statistically significant. When the torsion angle turned to 20°, 25°, the mean value in the L3 group was greater than the C2 group (0.01 < P < 0.05) which was statistically significant.
Conclusions: 1. The anti-torsional strength in the IM + AP group was stronger than that in the IM group.
2. The anti-torsional strength of 3-screw groups (L3,P3) was stronger than the 2-screw groups (L2,P2). When the number of the screws was the same, there was no significant difference between unicortical locking screws groups and bicortical common screws groups.
3. Reserved IM + AP with three unicortical locking and bicortical conventional screws gave the strongest fixation, suggesting it should be used in the clinic for treating femoral shaft fracture nonunion.
Keywords
Biomechanics, Anti-rotational plate, Femoral shaft fracture nonunion
Introduction
Intramedullary nailing (IM) is the primary method for treating nonunion of femoral shaft fractures [1]. However, with the advancement of IM technique and the increasing clinical indications, the incidence rate of femoral shaft fracture nonunion, according to the literature review, was 0.8-2% [2]. Regarding its treatment, exchanging intramedullary nailing is considered as the golden standard treatment for femoral shaft fracture nonunion, with a cure rate of up to 70-100% [1,3]. However, several reports have suggested that this method may increase the risk of future femoral shaft fracture nonunion [4,5]. Ueng et al. [6] firstly reported that reversed IM and additional plate fixation, with copious autologous bone grafting from the iliac crest, and is an effective and highly successful treatment with a union rate of up to 100%. Thus, this method has been extensively used by orthopedists and in clinical medicine generally. However, the biomechanical effects of the number and fixation methods of the screws used to secure the additional plate have not yet been described. Zhang et al. [7] stated that the main mechanical function of the additional plate is to provide rotational stability for the fracture site, which is called 'Anti-rotational plate' (AP).
The purpose of this study was to determine the biomechanical effects of treating femoral shaft fracture nonunion with an anti-rotation plate (AP) in addition to intramedullary nailing (IM) to provide a theoretical basis for their clinical application.
Materials and Methods
Materials and equipments
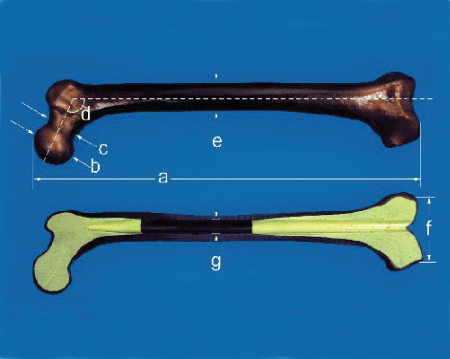
Artificial femurs (#3414, medium, left; Sawbones, USA), (Figure 1) AO intramedullary nails (Synthes Corporation, diameter: 10mm, length: 34 cm), and Anti-rotational plates (Synthes Corporation,7 hole narrow 4.5 series locking compression plate, 424.551/5 hole narrow 4.5 series locking compression plate, 424.571) were purchased. The embedding apparatus and mechanical testing system (MTS 858 MiniBionix testing machine; MTS Systems, Eden Prairie, MN, USA) were purchased.
Experimental groups
Twenty-five synthetic bones were divided into experimental group (IM + AP, n = 20) and control (IM, n = 5) groups. The experimental group was further divided into four subgroups based on the number of screws and fixation method: IM + AP with two (C2 group) or three (C3 group) bicortical common screws and IM + AP with two (L2) or three (L3) unicortical locking screws (Table 1).
![]()
Table 1: Groups of experiment
View Table 1
Preparation of specimens
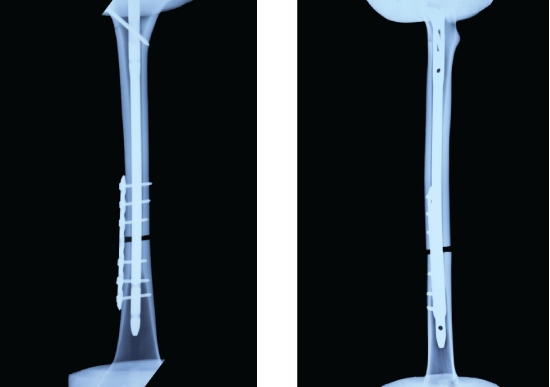
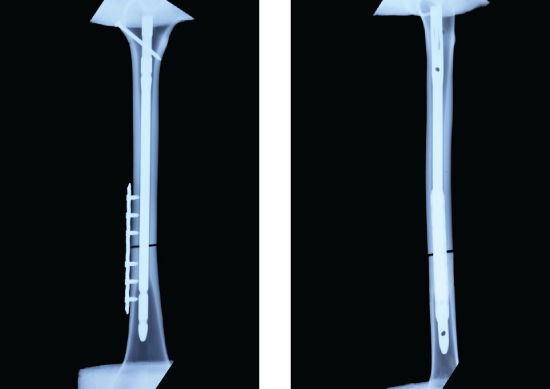
Based on the methods used in previously published studies [8], transverse osteotomies were performed on the model bones. Fractures were made 60% along the length of the femur, measured from the lesser trochanter to the adductor tubercle. After reducing the fracture, all specimens were reamed using the standard Kuntscher reamers, and up to a diameter of 11 mm. An AO intramedullary nail was inserted after reaming. One interlocking screw was fixed at the proximal portion and two screws were fixed at the distal portion. About IM+AP, firstly, according to the above method, IM was inserted and one interlocking screw was fixed at the proximal portion. But no screw in the distal portion was fixed in order to make the model of nonunion to maintain the rotational instability on the fracture site. In groups C3 and L3, an anti-rotational 7-hole plate was used to fix the fracture site, and the fracture of the proximal and distal parts were fixed with three bicortical common (C3) or three unicortical locking (L3) screws (Figure 2). In groups C2 and L2, an anti-rotational 5-hole plate was to fix the fracture site, and the fractures of the proximal and distal parts were fixed with two bicortical common (C2) or two unicortical locking (L2) screws (Figure 3).
Embedding the model femurs
Firstly, the specimens were placed in the embedding apparatus (Figure 4), ensuring that there was overlap between the longitudinal axis and the central red line of the scale. Then, polymethylmethacrylate (PMMA) was infused into the embedding apparatus. After embedding, the specimens were placed in the mechanical testing system (Figure 5).
Mechanical testing
Biomechanical testing was performed on an MTS 858 (Figure 6). The proximal portion of the specimen was fixed the fasten axis, while the distal portion was fixed the free-rotational axis on MTS 858. About the torsion direction of the specimen, its distal portion, relative to its proximal portion, was external rotation. During the torsion test, each specimen was externally rotated through angles of 0-25° with no axial loading at a rate of 0.5°/s, and the torsion-angle curves and torque values were recorded. (The most torsion angle which has been recorded was 25° in the experiment, because at current angle, mechanical failure of L2 group has been occurred.)
Statistical analysis
Data collected from the synthetic femurs were analyzed using analysis of variance (ANOVA) followed by Tukey-Kramer post-hoc pairwise comparisons in SPSS 10.0 (IBM, Armonk, NY, USA). P-values less than 0.05 were considered as statistically-significant differences.
Results
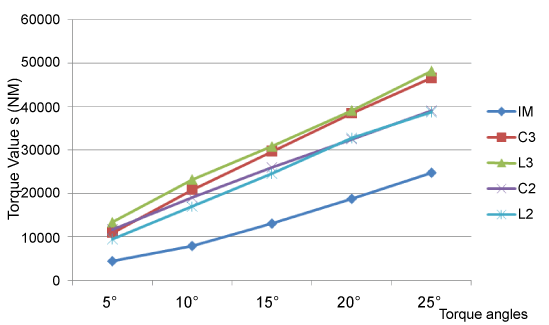
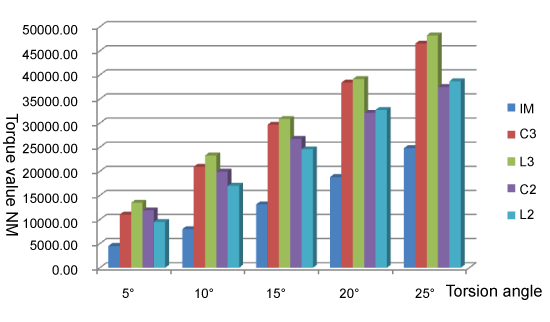
The mean and standard deviation of the torque angles (°) and torque values (Nm) for each group are shown in figure 7 and figure 8.
.
Figure 7: The comparison of the mean and standard deviation of torque values (Nm) in torsion angles (°) and for each group
View Figure 7
.
Figure 8: The comparison of the mean and standard deviation of torque values (Nm) in torsion angles (°) and for each group
View Figure 8
1. The mean value of the anti-torsional strength in the IM + AP group was greater than that in the IM group (0.01 < P < 0.05), which was statistically significant.
2. Based on the comparisons between the subgroups of IM + AP, the mean value of anti-torsional strength didn't show much difference. However, when the torsion angle turned to 25°, the mean value in the C3 group was greater than the C2 group (0.01 < P < 0.05) which was statistically significant. When the torsion angle turned to 5°, 10°, 25°, the mean values in the L3 group was greater than the L2 group (0.01 < P < 0.05), which was statistically significant. When the torsion angle turned to 20°, 25°, the mean value in the L3 group was greater than the C2 group (0.01 < P < 0.05), which was statistically significant (Table 2).
![]()
Table 2: The pair wise comparisons between the subgroups of IM + AP
View Table 2
Discussion
The method of exchanging IM is considered as the golden standard treatment for femoral shaft fracture nonunion, with a cure rate of 72%-100% according to the literature [2,3]. However, Banaszkiewicz and Weresh et al. [4,5] reported high failure rates (73% and 58%) after treatment with this method. Park et al. [8,9] confirmed that the method of exchanging IM had higher failure rate for nonisthmal femoral nonunion, whose main reasons is its mechanical instability. In Ueng's study, it was discovered that IM was not able to provide enough rotational stability in nonisthmal femoral nonunion, rotational instability in fracture area is also observable during the operation.
Regarding the rotational instability of fracture site, Ueng [6] firstly proposed the method of retaining the original IM and plates with the autologous bone grafting treatment, which achieved the bone union in 17 patients. Soon afterwards, Park et al. also reported the same clinical efficacy. Zhang et al. [7] stated that the plate is mainly to improve the mechanical stability, as the mechanical instability is the main cause for the femoral shaft fracture nonunion. Retaining the original IM also guaranteed the axial stability and bending stability. Moreover, AP improved the rotational stability at the fracture ends, which provided the crucial mechanical elements for the local fiber cartilage calcification, and promoting callus preliminary connection. According to the study by Park et al., the torsional strength of retaining IM and plate group is 3.3 times stronger than the IM locking group. And in terms of bending strength, the former is 2.6 times stronger than the later one [9].
Based on the results from the present study, the torsional strength provided by 3-screw constructs (L3, P3) is stronger than that of 2-screw constructs (L2, P2). From the biomechanical study of Grawe B [10], it was proved that 3-screw non locking constructs is stronger than the 2-screw locking constructs. Stoffel et al. [11,12] found that the rotational stability mainly depends on the number of screws. They recommend using three screws on either side of the fracture for femoral and tibial fractures, which are mainly loaded in compression. At the same time, three or more screws are used for each main fragment, which didn't show much difference in its anti-torsional strength.
Nevertheless, when the same amount of screws is used, which one has stronger torsional strength, locking screws or non locking screws? According to the present study, two unicortical locking screw group has stronger torsional strength than the two bicortical common screw group; the three unicortical locking screw group also has stronger torsional strength than the two bicortical common screw group. But the two doesn't show any statistic significance; neither did previous literature reach a consensus conclusion. Verse et al. [13] reported that in 12 pairs of sheep tibia fractures fixed with either three locking or non-locking screws, there were no differences in four-point bending, torsion, or axial compression testing. However, these results were controversial. Fitzpatrick et al. [14] found that, in torsion and bending, the locked plating constructs provided a significantly lower stiffness and strength than the conventional constructs. They stated that the distance between the bone and locking plate eliminate their stability. Similarly, Stoffel et al. [15] reported that the locked constructs had a 26% lower torsional rigidity than the non-locked constructs, with no significant difference between the axial stiffness of the groups. On the other hand, Gardner et al. reported a subtle mechanical advantage of bicortical locked plating compared with conventional plating under torsional loading [16,17].
When choosing between using unicortical or bicortical screws in an anti-rotational plate for the fixation of the fracture site, we recommend using bicortical screws. The results of the present study suggest that unicortical screws may loosen more easily because of their weaker holding force to the bone, especially in patients with osteoporosis. Gautier et al. [18] realized that there must be sufficient cortical thickness when using unicortical locking screws to fix bone fragments to provide mechanical stability, especially in patients with osteoporosis. Roberts et al. [19] reported that unicortical locking screws were resulted in poor torsional stiffness, but an additional bicortical locking screw can increase the torsion stiffness by 58%.
According to the present study, the locking and non locking screws showed the different failure curves during mechanical testing. The rotation angle and torque at failure of the plate secured with non locking screws were less than those secured with locking screws. The torque curve increased steadily with the torsion angle in the locking group, but this trend was reversed in the non locking group, which may be explained by uneven loading at the interface between the plate and bone. The failure mechanism in the locking-screws group was due to the torsional stress that concentrated on the interfaces of both the screws and the bone with increasing torsion angle. Fracture occurred occasionally, but the screws often were unbroken. In the non locking constructs, there was often one or several loose screws at once, screw bending, or even screw rupture, with or without the fracture line.
This result of the study is significant in two perspectives. On the one hand, it proves the Anti-rotational plates provide not only the axial stability, but also anti-rotational stability on the fracture site. On the other hand, the reliable data contributes to the theoretical basis for the rational and standardized clinic use of anti-rotational plates, which provides clinicians with promising treatment options in the future.
There are some limitations in this mechanical experiment. Because this experiment was performed in vitro using model femurs, the conclusion may not be applicable to the human body. In addition, the small number of samples per group may have led to errors in comparing the groups. Finally, because of the lack of certain corresponding instruments and some manual manufacturing variability, the model specimens in each groups had some differences. For example, the bicortical common screw was fixed by hands, which may cause the imbalance in either direction or strength.
Conclusions
1. The anti-torsional strength in the IM + AP group was stronger than that in the IM group.
2. The anti-torsional strength of 3-screw groups (L3, P3) was stronger than the 2-screw groups (L2, P2). When the number of the screws was the same, there was no significant difference between unicortical locking screws groups and bicortical common screws groups.
3. Reversed IM+AP with three unicortical locking and bicortical conventional screws gave the strongest fixation, suggesting it should be used in the clinic for treating femoral shaft fracture nonunion.
References
-
Sean E. Nork. Fractures of the shaft of the femur. In: Bucholz, Robert W, etc, editors. Rockwood & Green's fracture in Adults, 6th Edition.
-
Winquist RA, Hansen ST Jr, Clawson DK (1984) Closed intramedullary nailing of femoral fractures. A report of five hundred and twenty cases. J Bone Joint Surg Am 66: 529-539.
-
Brinker MR, O'Connor DP (2007) Exchange nailing of ununited fractures. J Bone Joint Surg Am 89: 177-188.
-
Banaszkiewicz PA, Sabboubeh A, McLeod I, Maffulli N (2003) Femoral exchange nailing for aseptic non-union: not the end to all problems. Injury 34: 349-356.
-
Weresh MJ, Hakanson R, Stover MD, Sims SH, Kellam JF, et al. (2000) Failure of exchange reamed intramedullary nails for ununited femoral shaft fractures. J Orthop Trauma, 14: 335-338.
-
Ueng SWN, Chao EK, Lee SS, Shih CH (1997) Augmentative plate fixation for the management of femoral nonunion after intramedullary nailing. J Trauma 43:640-644.
-
Gang, zhao, Bosong, zhang, Lin, et al. (2009) The diagnosis and treatment of femoral shaft fracture nonunion was caused by the rotational instability after the treatment of locked intramedullary nail. Chinese journal of surgery 16:1232-1235.
-
Park J, Kim SG, Yoon HK, Yang KH (2010) The treatment of nonisthmal femoral shaft nonunions with im nail exchange versus augmentation plating. J Orthop Trauma 24: 89-94.
-
Yang KH, Kim JR, Park J (2012) Nonisthmal femoral shaft nonunion as a risk factor for exchange nailing failure. J Trauma Acute Care Surg 72: E60-64.
-
Grawe B, Le T, Williamson S, Archdeacon A, Zardiackas L (2012) Fracture fixation with two locking screws versus three non-locking screws: A biomechanical comparison in a normal and an osteoporotic bone model. Archdeacon A Bone Joint Res Jun 1: 118-124.
-
Stoffel K, Dieter U, Stachowiak G, Gächter A, Kuster MS (2003) Biomechanical testing of the LCP--how can stability in locked internal fixators be controlled? Injury 34 Suppl 2: B11-19.
-
Miclau T, Remiger A, Tepic S, Lindsey R, McIff T (1995) A mechanical comparison of the dynamic compression plate, limited contact-dynamic compression plate, and point contact fixator. J Orthop Trauma 9: 17-22.
-
Verset M, Palierne S, Mathon D, Swider P, Autefage A (2012) Comparison of the effect of locking vs standard screws on the mechanical properties of bone-plate constructs in a comminuted diaphyseal fracture model. Comput Methods Biomech Biomed Engin 15: 337-339.
-
Fitzpatrick DC, Doornink J, Madey SM, Bottlang M (2009) Relative stability of conventional and locked plating fixation in a model of the osteoporotic femoral diaphysis. Clin Biomech (Bristol, Avon) 24: 203-209.
-
Stoffel K, Lorenz KU, Kuster MS (2007) Biomechanical considerations in plate osteosynthesis: the effect of plate-to-bone compression with and without angular screw stability. J Orthop Trauma 21:362-368.
-
Gardner MJ, Brophy RH, Campbell D, Mahajan A, Wright TM, et al. (2005) The mechanical behavior of locking compression plates compared with dynamic compression plates in a cadaver radius model. J Orthop Trauma 19: 597-603.
-
Gardner MJ, Griffith MH, Demetrakopoulos D, Brophy RH, Grose A, et al. (2006) Hybrid locked plating of osteoporotic fractures of the humerus. J Bone Joint Surg Am 88: 1962-1967.
-
Gautier E, Sommer C (2003) Guidelines for the clinical application of the LCP. Injury 34 Suppl 2: B63-76.
-
Roberts JW, Grindel SI, Rebholz B, Wang M, et al. (2007) Biomechanical evaluation of locking plate radial shaft fixation: unicortical locking fixation versus mixed bicortical and unicortical fixation in a sawbone model. J Hand Surg Am 32: 971-975.