International Journal of Sports and Exercise Medicine
A Non-Displaced C1 Fracture in Amateur Wrestling: A Case Report
Sergen Devran1*, Turgut Akgul2 and Omer Batın Gozubuyuk1
1Sports Medicine Department, Istanbul University, Turkey
2Orthopedics Department, Istanbul University, Turkey
*Corresponding author: Sergen Devran, Sports Medicine Department, Istanbul University, Istanbul Faculty of Medicine, Turkey, E-mail: sergen_devran@hotmail.com
Int J Sports Exerc Med, IJSEM-3-055, (Volume 3, Issue 2), Case Report; ISSN: 2469-5718
Received: January 09, 2017 | Accepted: March 18, 2017 | Published: March 20, 2017
Citation: Devran S, Akgul T, Gozubuyuk OB (2017) A Non-Displaced C1 Fracture in Amateur Wrestling: A Case Report. Int J Sports Exerc Med 3:055. 10.23937/2469-5718/1510055
Copyright: © 2017 Devran S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We present a case of a bilateral atlas posterior arc fracture that occurred during wrestling training. Atlas bone fractures are rare although may result with catastrophic consequences. A male amateur wrestler aged 25 years, who was otherwise healthy fell on his head while doing a cartwheel and could not continue training. He was admitted to the outpatient orthopedics clinic with persistent neck pain and dizziness after 7 days. X-ray and computed tomography of the patient revealed a stable fracture of C1 vertebra. He was then treated with a hard collar for 6 weeks. After removal of the collar, cervical strengthening exercises were started, which gradually increased in the rehabilitation program. The patient was allowed to perform contact sports 12 weeks after the incident.
Keywords
Wrestling injuries, Axial compression, Atlas fracture, Posterior arc
Introduction
Cervical neck injuries comprise of 0.8-14.9% of sports injuries and are commonly seen in wrestling [1]. Although they can be seen in many other sports, American football, rugby, surfing and ice hockey have a greater incidence [2]. Atlas (C1) fracture, seen in 2-13% of all spinal trauma cases and 2% of all spinal fractures, occur commonly with axial loading [3,4]. Forces with sudden head or neck rotational moments may also cause fracture of atlas. Shallow-water diving, falling or vehicle accidents are other common mechanisms of injury. Due to its close proximity to the brainstem, C1 fractures may cause catastrophic results such as chronic disability or death [5]. Wrestling, American football, gymnastics and ice hockey are type of sports known with such results [6].
The rate of catastrophic injuries is 0.01% in high school and collegiate athletes, which most commonly occurs during games when athletes are defending takedown movements [7]. The injury occurs when an athlete is grabbed and then thrown to the ground on their head by their opponent [7]. Here, we represent a case of atlas fracture in an amateur wrestler, the diagnosis, treatment, and return to sports process.
Case Report
A male amateur wrestler aged 25-year had a pain due to cervical neck injury during warm-up and could not continue training. He was performing a backwards cartwheel movement and fell on his head on the mat before completing the movement. He described a spring feeling on his spine followed by a sudden pain and loss of voluntary bodily control, which led him to fell on the ground. Dizziness and cervical neck pain occurred immediately afterwards; however, alleviation of these symptoms made him delay admittance to a clinic. He continued aerobic training for a week (i.e. running, stationary bicycle) but the dizziness did not resolve.
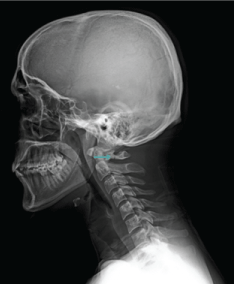
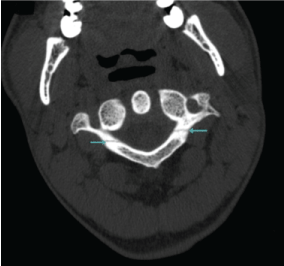
The athlete then presented to the orthopedics department with symptoms of persistent dizziness and neck pain. Upon physical examination, he had tenderness on the cervical spine and pain on both active and passive neck extensions. There were no sensory or motor deficits on neurologic examination. A lateral radiograph was performed and probable C1 stable fracture (Figure 1) was confirmed with computed tomography (CT), which revealed the final diagnosis of "bilateral posterior arc fracture of the atlas" (Figure 2). The patient was advised to use a hard-collar for 6 weeks. Six weeks after the injury, he had no symptoms and physical examination was normal. A second CT was performed in which callus formation was seen (Figure 3). He was then free to leave the collar and was referred to the sports medicine outpatient clinic for further recommendations and exercise prescription. There was no palpable tenderness and range of movement deficit in axis, resisted cervical flexion, extension, lateral flexion, and rotations in both directions, were painless upon physical examination in the sports medicine clinic. Neurologic re-examination was completely normal, and no signs for Horner or Wallenberg's syndrome were present. Spurling test was also negative.
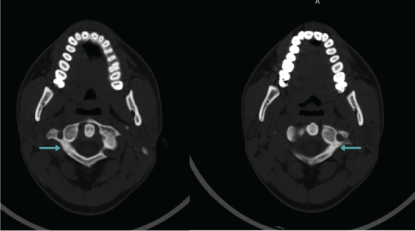
.
Figure 3: Axial CT scan after 6 weeks of injury demonstrates healing with callus formation.
View Figure 3
No exercises were given in the first visit and the patient was permitted to accommodate daily life without a collar. The patient was asked to attend follow-up visits every two weeks. Two weeks later, daily isometric exercises (self-resisted flexion, extension, and rotation while sitting upright), and a basic cervical stabilization exercise (prone cobra) with emphasis on extensors was given to be performed 10 seconds hold x 10 repetitions. Aerobic fitness exercises such as running on a cushioned platform or stationary bicycle were promoted in order to regain his pre-injury fitness capacity. At his 3rd visit to the sports medicine department, isometric strength exercises were increased in duration (i.e. 20 seconds hold x 20 repetitions) and additionally, core and cervico-thoracic stabilization program was given. The program included: modified bridging (10 reps), push-ups with trunk stabilization (10 reps), side plank (5 reps 30 seconds hold), and plank (5 reps 30 seconds hold). At his 4th visit, isometric exercises were exchanged with light-to-moderate Theraband concentric strengthening exercises (10 reps each axis) and the core stabilization program was increased in duration (doubled hold-times). At the 5th visit neck concentric strengthening was advanced to moderate-to-hard Theraband with 15 reps each movement; rolling plank, straight leg raise, supine bilateral leg lifts and heeltap (20 reps each) were added for more core stabilization. At his last and 6th visit, core exercises were doubled in repetition and his strength program was organized to include cervico-thoracic exercises and core stabilization exercises every other day. On his last visit, his neck strength was significantly increased upon manual muscle testing and the patient had no fear of re-injury. He was able to perform all functional movement tests and felt psychologically ready to train, at which time he was cleared to participate in contact sports by the sports physician.
Discussion
Neck injury prevalence is reported as 0.8-14.9% among all injuries in wrestling. Although the neck is a common site of injury, cervical spine fractures are rare; some have catastrophic results [1].
In wrestling, most catastrophic injuries such as fractures or luxations of the cervical spine occur due to axial and/or rotational loading on the head and cervical region. Mueller and Cantu [8] reported in their study from the National Center for Catastrophic Sports Injury Center (NCCSIR) that between 1982 and 2001 there were 2 fatal and, 46 catastrophic injuries in high school, and 1 injury in collegiate athletes, with a rate of 0.97 and 0.72 per 100,000 wrestlers in the high school and collegiate population, respectively. Laudermilk [9] collected data from the NCCSIR between 1982-1987 and of the 24 catastrophic injuries recorded, half were related with cervical spine, spinal cord or head, whereas the other half was with cardiopulmonary etiology. Surprisingly, 42% of the spine-related injuries occurred with the "takedown" movement as in our case. Additionally, 71% of these injuries occurred during matches, as expected, but contrary to our case. Boden, et al. [7] reviewed the NCCSIR data between 1981-1999 and found that 34 out of 35 catastrophic injuries were seen in high school, and the remaining one in a collegiate athlete, in line with other reports. The authors reported a catastrophic injury rate of 0.01%, which most commonly occurred when athletes were defending a takedown movement, during a game.
Cervical spine fractures commonly occur during flexion-rotation mechanism while the spine is axially loaded. The stress is concentrated on vertebrae and facet joints, which causes the fracture. Acute onset of pain, and numbness radiating into arms and legs should raise suspicion of spinal fracture or dislocation. Several injury mechanisms and types of injuries have been summarized [10]: however, due to the complexity and high speed of movements in wrestling, mechanisms of injury cannot be easily differentiated [11]. Pasque and Hewett [11] described injuries that most commonly occurred during the "takedown" movement, specifically to the defending or the disadvantaged athlete being hit on the mat, and the faster and stronger the movement, the more severe the injury.
Different types of fractures are seen in the atlas, which were further classified by Gehweiler into 5 types (Table 1) [12]. Although not common, cervical fractures may result with brainstem or spinal cord pressure when there is atlanto-occipital or atlanto-axial instability and lead to death [13].
![]()
Table 1: Fracture types of Atlas.
View Table 1
Several difficulties exist when diagnosing an atlas fracture. Classically, patients with atlas fracture have a history of an impact on the head, report upper neck pain [14] without accompanying neurologic deficit, and they are harder to detect on an X-rays; whereas, lower cervical fractures usually present with neurologic symptoms and are easier to diagnose radiologically. A definitive diagnosis of an atlas fracture is made with CT and ligamentous injuries are further exposed with magnetic resonance imaging (MRI) [15].
No standards or guidelines for treatment and rehabilitation of C1 fractures alone or in combination with other cervical spine injuries have been developed. Instead, treatment recommendations for isolated C1 fractures and are typically based on a group of case series. Most isolated C1 fractures are managed with use of a rigid collar, a halo-thoracic brace, or sterno-occipitomandibular immobilization [5]. In cases with more significant fracture displacement, more rigid immobilization with the halo vest or Minerva jacket may be required [16]. But these orthosis have some significant complications like slippage, loosening, infection, and irritation and discomfort are common. Fracture of the atlas can be treated effectively also with a rigid cervical collar alone with good neurologic recovery and segmental stability [17]. Treatment should be individualized: however, immobilization is needed and should extend up to 6-8 weeks in stable fractures [10]. In order to exclude late instability, flexion and extension X-rays should be performed [5]. Occasionally, orthotic stabilization may result in nonunion or continued instability, in which case surgical intervention is necessary [13]. Although, operative intervention for C1 fractures is rarely needed more complex cases, such as AOD (atlanto-occipital dislocation) or when neurologic compromise is present [14,18].
We have reported a case of a stable cervical fracture in an amateur wrestler who presented to our clinic and detailed information was given about his physical examination, diagnosis, treatment, and rehabilitation. Although neck injuries are common, vertebrae fractures are not commonly seen, but may result with catastrophic outcomes. For this reason, suspicion of a fracture should be present in patients with cervical trauma having an axial load. Athletes may return to sports safely with prompt diagnosis and a correct rehabilitation program.
References
-
Hewett TE, Pasque C, Heyl R, Wroble R (2005) Wrestling injuries. Med Sport Sci 48: 152-178.
-
Bailes JE, Petschauer M, Guskiewicz KM, Marano G (2007) Management of cervical spine injuries in athletes. J Athl Train 42: 126-134.
-
Marcon RM, Cristante AF, Teixeira WJ, Narasaki DK, Oliveira RP, et al. (2013) Fractures of the cervical spine. Clinics (Sao Paulo) 68: 1455-1461.
-
Matthiessen C, Robinson Y (2015) Epidemiology of atlas fractures--a national registry-based cohort study of 1,537 cases. Spine J 15: 2332-2337.
-
Kakarla UK, Chang SW, Theodore N, Sonntag VK (2010) Atlas fractures. Neurosurgery 66: 60-67.
-
Boden BP, Tacchetti RL, Cantu RC, Knowles SB, Mueller FO (2006) Catastrophic cervical spine injuries in high school and college football players. The American Journal of Sports Medicine 34: 1223-1232.
-
Boden BP, Lin W, Young M, Mueller FO (2002) Catastrophic injuries in wrestlers. Am J Sports Med 30: 791-795.
-
Mueller FD, Cantu RC (2002) Nineteenth Annual Report of the National Center for Catastrophic Sports Injury Research: Fall 1982-Spring 2001. Chapel Hill, NC: National Center for Catastrophic Sports Injury Research.
-
Laudermilk JI (1988) Catastrophic injuries in junior high school and high school wrestling: a five-season study. Chapel Hill, University of North Carolina.
-
Dvorak J (2016) FIFA Diploma in Football Medicine.
-
Pasque CB, Hewett TE (2000) A prospective study of high school wrestling injuries. Am J Sports Med 28: 509-515.
-
Fracture of Atlas (C1) - Gehweiler Classification (2016).
-
Mead LB, Millhouse PW, Krystal J, Vaccaro AR (2016) C1 fractures: a review of diagnoses, management options, and outcomes. Curr Rev Musculoskelet Med 9: 255-262.
-
Garrett M, Consiglieri G, Kakarla UK, Chang SW, Dickman CA (2010) Occipitoatlantal Dislocation. Neurosurgery 66: 48-55.
-
Radcliff KE, Sonagli MA, Rodrigues LM, Sidhu GS, Albert TJ, et al. (2013) Does C1 Fracture Displacement Correlate with Transverse Ligament Integrity?. Orthopaedic Surgery 5: 94-99.
-
Lauweryns P (2010) Role of conservative treatment of cervical spine injuries. Eur Spine J 19: 23-26.
-
Lee TT, Green BA, Petrin DR (1998) Treatment of stable burst fracture of the atlas (Jefferson fracture) with rigid cervical collar. Spine (Phila Pa 1976) 23: 1963-1967.
-
Lee C, Woodring JH (1991) Unstable Jefferson variant atlas fractures: an unrecognized cervical injury. AJNR Am J Neuroradiol 12: 1105-1110.