International Journal of Sports and Exercise Medicine
Validity of a Kinect-based Tracking System for Clinical Assessment of Knee Kinematics
Edward Nyman, Jr.*
Motion Capture Laboratory, Department of Kinesiology, The University of Toledo, USA
*Corresponding author: Edward Nyman, Jr., Ph.D, Assistant Professor, Department of Health and Human Performance, College of Health Professions, The University of Findlay, 1000 N. Main Street, Findlay, OH, USA, Tel: 419-434-5969, E-mail: nyman@findlay.edu
Int J Sports Exerc Med, IJSEM-2-032, (Volume 2, Issue 1), Original Research; ISSN: 2469-5718
Received: August 15, 2015 | Accepted: January 01, 2016 | Published: January 04, 2016
Citation: Nyman E (2016) Validity of a Kinect-based Tracking System for Clinical Assessment of Knee Kinematics. Int J Sports Exerc Med 2:032. 10.23937/2469-5718/1510032
Copyright: © 2016 Nyman E. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The primary objective of this study was validation of a three-dimensional single-camera system (Kinect) for use as a clinical screening tool for evaluating knee kinematics during drop jump landings. Lower extremity kinematics for each of eight adolescent female participants were simultaneously tracked by a traditional motion capture system and the prototype Kinect-based tracking system during performance of a drop jump landing task. Peak sagittal plane knee flexion angle and minimum knee separation distance (utilized as a surrogate for frontal plane knee valgus) were calculated from data collected independently from both systems over five successive trials. Data were smoothed and output as mean averages for each participant for each system then time matched and evaluated statistically with Pearson product correlations to determine system validity. Correlations between the two systems for peak knee flexion angle (r = 0.963, P < 0.001) and minimum knee separation distance (r = 0.916, P < 0.001) indicated similarity. As traditional motion capture has long been considered to be a standard method for assessing knee kinematics, these results indicate that this Kinect-based system provides valid kinematic values for drop jump landing assessment. Further application of this system to clinical efforts, such as ACL injury prevention, should be explored.
Keywords
Kinect, kinematics, Screening, knee
Introduction
Recent advances in three-dimensional (3D) motion analysis (MOCAP) and enhanced two-dimensional video-based systems have rapidly advanced knee kinematics research. A number of impactful studies have examined 3D kinematics during landing, cutting, and deceleration, particularly with respect to elevated predisposition to ACL injury [1-14]. In many of these studies, dynamic knee valgus moment and reduced knee flexion angle have been implicated as major contributing factors to non-contact ACL injury [5,12]. Such studies have often been combined with longitudinal epidemiological data to give a more astute picture of the correlation between neuromuscular control strategies and acute knee injury, particularly to the ACL. Additionally, a number of recent studies have examined the efficacy of feedback training aimed at altering control strategies in ways that may decrease the likelihood of injury [15]. The ability to provide real-time qualitative and quantitative data, via motion capture approaches, may enhance such efforts.
With abundant research now linking aberrant neuromuscular control with ACL injury risk, the need for accurate quantitative measurement systems for assessing lower extremity kinematics has become paramount. However, there are practical limitations to laboratory-based 3D MOCAP systems, including the high cost of the equipment, requisite time for the clinician to be trained in its use, and logistical challenges with the transport of such a system for field-based applications. Logically, the need for a system that provides accuracy comparable to contemporary laboratory biomechanics instrumentation, without the significant limitations aforementioned, would be ideal for field and clinical use, thus bringing the benefits to many more individuals at risk.
Recently, advances in open-source natural interaction interfaces for human gesture recognition and resultant human skeletal tracking have changed the dynamics of traditional motion analysis [16-21]. With the advent of new hardware and software, Prime Sense (Tel Aviv, Israel) provided Microsoft (Redmond, WA, USA) with a platform (Kinect, Microsoft Corporation, Redmond, WA, USA) capable of real-time capture and recording of human kinematics outside of a traditional motion analysis laboratory [16,22]. Kinect uses calibrated structured infrared light emission and detection to track limb segments within a defined physical capture volume. The calibrated volume enables marker less joint center tracking for dynamic environments. If such a system can be utilized as a surrogate for laboratory-based MOCAP systems, it may provide clinicians with a powerful tool to assist in the quantitative evaluation of aberrant functional biomechanics such as those linked to higher risk of ACL injury.
While recent work has indeed successfully validated the Kinect for use in postural control evaluation [17], the validity of the Kinect for dynamic activities, such as in drop jump landings, has yet to be evaluated. The purpose of this study was to assess the validity of a clinically-oriented Kinect-based knee kinematics tracking system as a tool for evaluating lower extremity biomechanics, particularly those consistent with risk of non-contact ACL injury, during drop jump landings (DJL) in young female athletes. We hypothesized that this novel system would produce valid lower extremity peak kinematics relative to those produced via traditional laboratory-based MOCAP.
Materials and Methods
Participants
Eight adolescent female participants were randomly chosen from area competitive gymnastics programs. This population was selected, as the incidence of ACL injury in women's gymnastics, as in soccer and basketball, is relatively high in comparison to participants of other sports [23]. All participants and a parent or legal guardian provided written informed consent and assent after having the experimental procedures and possible risks associated with participation detailed. All experimental protocols and the informed consent/assent documents were approved by the university's institutional review board. Enrolled participants were required to be free from lower extremity and spine musculoskeletal injury, have no history of orthopedic surgery, no recent concussions, and intact bilateral ACLs. Mean age of all participants was 15.0 (1.6) years, mean height was 1.60 (0.07) meters, mean mass was 53.0 (7.1) kilograms, and mean competitive gymnastics ability was Level 7 (1) out of a possible range of Level 1 (lowest) through Level 10 (highest) per the sport's national governing body (USA Gymnastics, Indianapolis, IN, USA) (Table 1).
![]()
Table 1: Participant anthropomorphic data and peak kinematics.
View Table 1
Kinect-based tracking system design
A clinically-oriented lower extremity kinematic tracking system consisting of a commercially available depth-camera (Kinect, Microsoft Corporation, Redmond, WA, USA), open source driver package (NiTE, PrimeSense, Tel Aviv, Israel), open source programming (OpenNI.org), and graphical user interface software (Processing.org, MIT, MA, USA) for laptop PC was developed for this study. A portable Kinect-based evaluation station (Figure 1), designed to optimize collection and real-time display of kinematic data, was fabricated utilizing the aforementioned program, rolling cart, laptop PC (Lenovo, Beijing, China), and a top-mounted 24-inch flat screen monitor (Samsung, Seoul, South Korea), facilitating real-time three-dimensional coordinate data capture (Figure 1).
When the Kinect system was activated, participants were automatically recognized and calibrated based on an initial kinematic pose, after which the system tracks the participant's movements in real time. Such tracking capability was afforded by the Kinect's random forest algorithm approach to identifying limb segments and applying best-fit human musculoskeletal joint centers. All kinematic data captured by the Kinect camera are initially processed by an imbedded proprietary randomized decision forest software algorithm wherein 'skeleton' segments are derived from a fusion of two-dimensional (x and y coordinate) pixel tracking along with the third dimensional point value provided by the depth image value [16]. These segments were tracked and plotted in real-time, resulting in frontal and sagittal plane angular rotations and displacements, with minimal latency at a rate of 30 Hz [16,24].
The custom software utilized for the clinical knee kinematic tracking system calculates two metrics representative of those commonly utilized in ACL injury prevention biofeedback studies; peak knee flexion angle and minimum normalized knee center separation distance - defined as height normalized distance between the calculated centers of the left and right knee joint [13]. This alternative value was chosen as a surrogate for traditional frontal plane bilateral knee valgus angles due to the advantage of providing a single representative value that could be readily utilized as part of future biofeedback programs. The knee center separation distance vector is recorded in units of millimeters while the knee flexion angle was recorded in degrees. The system logs a tab-delineated file of time coded knee flexion angles and center knee separation distance for each participant's individual data capture sessions.
Procedures for lab-based validation
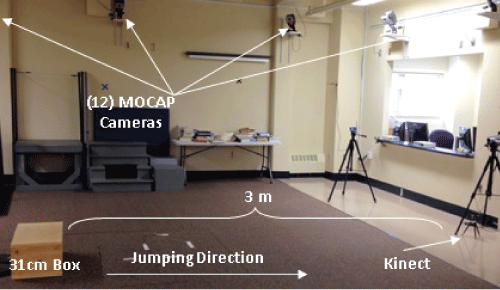
All validation testing was conducted in the Motion Analysis Laboratory at the University of Toledo, with a multiple system camera set-up as depicted in Figure 2.
Participants were instrumented for traditional MOCAP with thirty-six 20mm spherical retro-reflective lower extremity markers (Figure 3) and marker trajectories were tracked at 200 Hz with a 12-camera array (Eagle cameras and Cortex software, Motion Analysis Corporation, Santa Rosa, CA, USA).
Two independent 50 cm × 50 cm force plates (OR-6-5-1, AMTI, Watertown, MA, USA), sampling at 2000 Hz, facilitated demarcation of initial ground contact during landings. Each of the participant's separate trials was recorded simultaneously by both the MOCAP and Kinect-based systems.
All participants were introduced to a well-established 31cm drop jump landing task [2,25,26] via initial verbal explanation and secondary visual demonstration by a trained member of the research team, after which participants were permitted up to three practice trials. In such trials, the subject was requested to jump off of the box with both feet and land on the ground in front of the box, immediately 'absorbing' the landing as if preparing for further athletic activity. Once the participant was comfortable performing the task, five successful trials were performed during which the DJL kinematics were collected simultaneously by the Kinect-based system and the MOCAP system. The Kinect system was positioned directly in front of the participant at a distance of 3 meters and a height of 0.3 meters relative to the jump landing area (Figure 2).
Peak knee flexion angle and minimum knee center separation distance for the first 30 ms after initial ground contact were recorded simultaneously by the Kinect-based system as well as the full 12-camera MOCAP system. The frame of initial ground contact was established for the 3D MOCAP video from the force platform data and matched to the synced Kinect system, visually. Thirty milliseconds (30 ms) was used as the kinematic temporal variable as numerous studies have demonstrated that ACL insult likely occurs within that timeframe [26].
Data processing and statistical analysis
Kinematic artifact (noise), resident in the tracking of joint kinematics via the Kinect system is due largely to variations in participant morphology, and is influenced by participant clothing. This was partially mitigated by the requirement for form-fitting clothing worn by the participants. All Kinect-derived joint kinematics data was smoothed via a standard RMS approach. For the traditional MOCAP system, movement artifact resulting from the inherent inertial properties of the retro-reflective markers was minimized by using small low mass markers and insuring a secure attachment of all markers directly to the skin. Following data collection, all MOCAP marker trajectories were filtered with a 12 Hz fourth order Butterworth filter and the same RMS smoothing treatment was applied to the derived kinematics.
MOCAP kinematic data was exported from Cortex (Motion Analysis Corporation, Santa Rosa, CA, USA) to Visual 3D (C-Motion, Germantown, MD, USA) where construction of a lower-body 3D model in accordance with standard Newton-Euler conventions was completed. Peak knee flexion angle and minimum knee center separation distance were calculated in Visual 3D via a standard inverse kinematics approach, averaged over the five trials, and recorded for comparison to the Kinect data.
All statistical analyses were performed in SPSS v17.0 (IBM, Armonk, NY, USA). Pearson product moment correlations were calculated for each dependent variable between the two systems. The dependent variables were minimum knee flexion angle and participant height-normalized minimum knee center separation distance within the first 30ms after initial ground contact. Alpha-level was set a priori at p ≤ 0.05 for all statistical comparisons.
Results
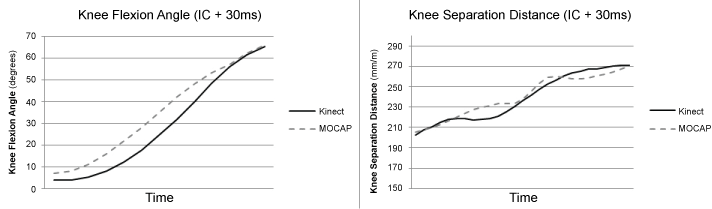
The Kinect-based system and MOCAP system yielded highly correlated results with a Pearson's r of 0.963 (P < 0.001) for peak knee flexion angle and Pearson's r of 0.916 (P < 0.001) for normalized minimum knee separation distance. As illustrated in Figure 4 (data from one representative participant), peak knee flexion angle and normalized knee separation distance kinematics as measured by the Kinect-based and MOCAP system were similar.
Discussion
The results of this study demonstrate that the Kinect-based tracking system produced peak knee flexion angles and minimum normalized knee center separation distances comparable to a traditional MOCAP system. These results are consistent with the findings of other studies that have evaluated data from Kinect-based systems, such as in the work of Clark, et al. [17], who demonstrated system validity within a comparable range (r > 0.90) to that delineated in this study. However, in contrast to studies that focused primarily on postural stability during reaching task [17-19], this study extended tracking to a more dynamic activity (DJL), therein opening the applicability to assessment of more dynamic lower extremity functional activities in a clinical environment.
The applicability of this Kinect-based approach as an alternative to traditional MOCAP systems affords clinicians the opportunity to gain valuable objective kinematic metrics in far less confined, even potentially remote, environments, at a significantly lower cost. Such portability and economy may enable those who had previously been unable to access such systems the opportunity to benefit from objective kinematic assessments. While the efforts, herein, were applied to the knee, the approach could be extended to the upper extremities, hips, torso, and head.
As in any kinematic study, some limitations are noted. Though the population targeted for this study was quite homogenous, with only female competitive gymnasts between the ages of 13 and 18 years enrolled, the benefits of this inclusion criterion outweighed disadvantages of variability in extraneous training and personal equipment or inherent sport practice surface variables that might otherwise have confounded the study. In addition, the ability to use competitive athletes who train and perform without footwear eliminated an additional potentially confounding variable of shoe-type. Additionally, the participants in this study were extremely lean. Thus, the influence of subcutaneous body fat as a factor contributing to aberrant marker movement, resulting in an additional source of kinematic signal noise, was largely mitigated. Finally, it is important to again note that this study evaluated sagittal and frontal plane kinematics, with no tracking of transverse plane rotations of the tibia with respect to the femur. As a result, internal and external tibial rotations about the femur were not considered, despite evidence of some degree of contribution from the transverse plane with respect to ACL injury.
With recent advancements in technology, it is now possible to capture quantitative kinematic data for screening and evaluation purposes outside of a traditional laboratory environment using calibrated structured infrared light in lieu of physical markers and multiple cameras. While previous research [27,28] has shown that clinical assessment of drop jump landing kinematics can identify female athletes at increased risk of non-contact ACL injury, the constraints and obstacles to automated efficient metrics have largely limited the applicability of such screening efforts to the clinic and field level with sufficient volume. The portability and ease of use of this Kinect-based system, and its ability to accurately replicate frontal and sagittal plane data for female subjects as compared with a traditional MOCAP system, may therefore make it appropriate for expanding objective screening of frontal and sagittal plane lower extremity kinematics, such as in efforts to diminish the risk of ACL injury, in settings where access to a traditional MOCAP laboratory is not practical or efficient.
References
-
Borotikar BS, Newcomer R, Koppes R, McLean SG (2008) Combined effects of fatigue and decision making on female lower limb landing postures: central and peripheral contributions to ACL injury risk. Clin Biomech (Bristol, Avon) 23: 81-92.
-
Ford KR, Myer GD, Hewett TE (2003) Valgus knee motion during landing in high school female and male basketball players. Med Sci Sports Exerc 35: 1745-1750.
-
Ford KR, Myer GD, Smith RL, Vianello RM, Seiwert SL, et al. (2006) A comparison of dynamic coronal plane excursion between matched male and female athletes when performing single leg landings. Clin Biomech (Bristol, Avon) 21: 33-40.
-
Ford KR, Myer GD, Toms HE, Hewett TE (2005) Gender differences in the kinematics of unanticipated cutting in young athletes. Med Sci Sports Exerc 37: 124-129.
-
Hewett TE, Myer GD, Ford KR, Heidt RS Jr, Colosimo AJ, et al. (2005) Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med 33: 492-501.
-
Malinzak RA, Colby SM, Kirkendall DT, Yu B, Garrett WE (2001) A comparison of knee joint motion patterns between men and women in selected athletic tasks. Clin Biomech (Bristol, Avon) 16: 438-445.
-
McLean SG, Huang X, Su A, Van Den Bogert AJ (2004) Sagittal plane biomechanics cannot injure the ACL during sidestep cutting. Clin Biomech (Bristol, Avon) 19: 828-838.
-
McLean SG, Neal RJ, Myers PT, Walters MR (1999) Knee joint kinematics during the sidestep cutting maneuver: potential for injury in women. Med Sci Sports Exerc 31: 959-968.
-
Myer GD, Ford KR, Brent JL, Hewett TE (2007) Differential neuromuscular training effects on ACL injury risk factors in"high-risk" versus "low-risk" athletes. BMC Musculoskelet Disord 8: 39.
-
Nyland JA, Shapiro R, Caborn DN, Nitz AJ, Malone TR (1997) The effect of quadriceps femoris, hamstring, and placebo eccentric fatigue on knee and ankle dynamics during crossover cutting. J Orthop Sports Phys Ther 25: 171-184.
-
Quatman CE, Hewett TE (2009) The anterior cruciate ligament injury controversy: is "valgus collapse" a sex-specific mechanism? Br J Sports Med 43: 328-335.
-
Renstrom P, Ljungqvist A, Arendt E, Beynnon B, Fukubayashi T, et al. (2008) Non-contact ACL injuries in female athletes: an International Olympic Committee current concepts statement. Br J Sports Med 42: 394-412.
-
Sigward SM, Havens KL, Powers CM (2011) Knee separation distance and lower extremity kinematics during a drop land: implications for clinical screening. J Athl Train 46: 471-475.
-
Zazulak BT, Hewett TE, Reeves NP, Goldberg B, Cholewicki J (2007) Deficits in neuromuscular control of the trunk predict knee injury risk: a prospective biomechanical-epidemiologic study. Am J Sports Med 35: 1123-1130.
-
Benjaminse A, Otten E (2011) ACL injury prevention, more effective with a different way of motor learning? Knee Surg Sports Traumatol Arthrosc 19: 622-627.
-
Borenstein G (2012) Making Things See: 3D Vision with Kinect. Processing, Arduino, and Maker Bot: Make.
-
Clark RA, Pua YH, Fortin K, Ritchie C, Webster KE, et al. (2012) Validity of the Microsoft Kinect for assessment of postural control. Gait Posture 36: 372-377.
-
de Albuquerque A, Moura E, Vasconcelos T, Mendes LA, Nagem DAP (2012) Kinect Sensor Used As a Support Tool in Clinical Analysis. Journal of biomechanics 45: S304.
-
Dutta T (2012) Evaluation of the Kinect™ sensor for 3-D kinematic measurement in the workplace. Appl Ergon 43: 645-649.
-
Lowes LP, Alfano LN, Yetter BA, Worthen-Chaudhari L, Hinchman W, et al. (2013) Proof of concept of the ability of the kinect to quantify upper extremity function in dystrophinopathy. PLoS Curr 5.
-
Mentiplay BF, Clark RA, Mullins A, Bryant AL, Bartold S, et al. (2013) Reliability and validity of the Microsoft Kinect for evaluating static foot posture. J Foot Ankle Res 6: 14.
-
Wall SJ, Rose DM, Sutter EG, Belkoff SM, Boden BP (2012) The role of axial compressive and quadriceps forces in noncontact anterior cruciate ligament injury: a cadaveric study. Am J Sports Med 40: 568-573.
-
Sigward S, Powers CM (2006) The influence of experience on knee mechanics during side-step cutting in females. Clin Biomech (Bristol, Avon) 21: 740-747.
-
Wong W (2011) How Microsoft's PrimeSense-based Kinect Really Works.
-
Hewett TE, Myer GD, Ford KR, Slauterbeck JR (2006) Preparticipation physical examination using a box drop vertical jump test in young athletes: the effects of puberty and sex. Clin J Sport Med 16: 298-304.
-
Myer GD, Ford KR, Khoury J, Succop P, Hewett TE (2011) Biomechanics laboratory-based prediction algorithm to identify female athletes with high knee loads that increase risk of ACL injury. Br J Sports Med 45: 245-252.
-
Myer GD, Ford KR, Brent JL, Hewett TE (2012) An integrated approach to change the outcome part I: neuromuscular screening methods to identify high ACL injury risk athletes. J Strength Cond Res 26: 2265-2271.
-
Padua DA, Marshall SW, Boling MC, Thigpen CA, Garrett WE Jr, et al. (2009) The Landing Error Scoring System (LESS) Is a valid and reliable clinical assessment tool of jump-landing biomechanics: The JUMP-ACL study. Am J Sports Med 37: 1996-2002.