International Journal of Sports and Exercise Medicine
A New View of Responses to First-Time Barefoot Running
Michael Wilkinson1*, Nick Caplan1, Richard Akenhead2 and Philip R Hayes1
1Faculty of Health and Life Sciences, Northumbria University, UK
2ASPETAR, Sports Medicine Institute, Qatar
*Corresponding author: Dr. Michael Wilkinson, Department of Sport, Exercise and Rehabilitation, Northumbria University, Northumberland Building, Newcastle-upon-Tyne, NE1 8ST, UK, Tel: 44(0)191-243-7097, E-mail : mic.wilkinson@northumbria.ac.uk
Int J Sports Exerc Med, IJSEM-1-010, (Volume 1, Issue 2), Original Investigation; ISSN: 2469-5718
Received: April 30, 2015 | Accepted: May 25, 2015 | Published: May 28, 2015
Citation: Wilkinson M, Caplan N, Akenhead R, Hayes PR (2015) A New View of Responses to First-Time Barefoot Running. Int J Sports Exerc Med 1:010. 10.23937/2469-5718/1510010
Copyright: © 2015 Wilkinson M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We examined acute alterations in gait and oxygen cost from shod-to-barefoot running in habitually-shod well-trained runners with no prior experience of running barefoot. Thirteen runners completed six-minute treadmill runs shod and barefoot on separate days at a mean speed of 12.5km.h-1. Steady-state oxygen cost in the final minute was recorded. Kinematic data were captured from 30-consecutive strides. Mean differences between conditions were estimated with 90% confidence intervals. When barefoot, stride length and ground-contact time decreased while stride rate increased. Leg-and vertical stiffness and ankle-mid-stance dorsi-flexion angle increased when barefoot while horizontal distance between point of contact and the hip decreased. Mean oxygen cost decreased in barefoot compared to shod running (90% CI -11% to -3%) and was related to change in ankle angle and point-of-contact distance, though individual variability was high (-19% to +8%). The results suggest that removal of shoes produces an alteration in running gait and a potentially-practically-beneficial reduction in mean oxygen cost of running in trained-habitually-shod runners new to running barefoot. However, high variability suggests an element of skill in adapting to the novel task and that caution be exercised in assuming the mean response applies to all runners.
Keywords
Running, Barefoot, Economy, Gait
Introduction
The popularity of barefoot and minimalist-shoe running has been steadily increasing in recent years with articles in the popular media and several web sites [1]. Scientific interest has also increased over the same period with attention focussing on mechanical and energetic differences between shod and barefoot/minimalist-shoe conditions and populations.
From a series of studies, Robbins and colleagues [2-5] proposed a plantar-sensory mediated protective behaviour hypothesis that could be applied to barefoot locomotion. The hypothesis suggested a sensory-feedback loop where the sensation of vertical and horizontal loading triggers impact-avoidance reflexes in the legs. Impact avoidance behaviour is initiated to reduce unpleasant plantar sensations and pain [4]. Applied to barefoot running, the plantar-sensory feedback hypothesis would predict alterations in gait to minimise discomfort. The changes anticipated would be those that would reduce the rate of vertical and horizontal impact loading. Lieberman et al. [6] found habitually-barefoot runners had a three-fold lower peak-impact force and approximately a two-fold lower loading rate compared to habitually-shod runners asked to run barefoot. A difference in typical foot-strike pattern was also observed between the two groups, with all habitually-shod runners adopting a heel strike and 88% of habitually-barefoot runners using a mid/forefoot strike. Theoretically, vertical-and horizontal loading could also be reduced by decreasing the distance between the point of ground contact and the general centre of mass. Reducing this distance could reduce the braking impulse and the magnitude of the associated ground-reaction forces. A decrease in lever arm length by landing closer to the centre of mass could also reduce joint torque and therefore the muscle force required to counteract those torques. Shorter stride length, faster stride rate and reduced ground contact time would also be expected, all of which are characteristic of habitual-barefoot runners compared to shod [6-9]. The differences in gait between habitually-barefoot and habitually-shod runners are consistent with gait alterations that would be expected from the plantar-sensory feedback hypothesis.
It has been suggested that running barefoot might also reduce oxygen cost at any given running speed [10,11] and therefore could theoretically improve performance [12]. Studies comparing running economy in barefoot and minimal shoe versus shod have reported equivocal findings [9-11,13-18]. Five out of eight studies have reported significant reductions in the oxygen cost of running barefoot versus shod [10,11,13,15-17] though the studies had varying degrees of rigor and control.
Two competing hypotheses to explain the reduction in oxygen cost have emerged. The first proposes that reductions in oxygen cost are attributable to removal of the mass of the shoe, which would decrease the energy required to swing the legs [19]. The magnitude of decrease in the oxygen cost of running is suggested by Frederick et al. [19] to be 1% per 100g of mass removed from each foot. The alternative hypothesis proposes that reductions in oxygen cost are attributable to an increased use of stored elastic energy [17]. This increase in stored elastic energy being primarily from the longitudinal arch in the foot and the Achilles tendon [20,21]. In addition to controlling for shoe mass, Perl et al. [17] also controlled stride frequency and foot-strike type reporting that runners were 2.4% more economical in minimal footwear (Vibram Five Fingers) than in standard-cushioned running shoes. The economy advantage of the minimal shoe condition was attributed to increased storage and return of elastic energy in the lower extremities, primarily the longitudinal arch of the foot. A recent study provided further evidence of oxygen-cost reductions in barefoot-versus-shod running that exceeded magnitudes predicted by shoe mass removal [22].
While both the shoe-mass-and elastic-energy-storage hypotheses can be supported by data from different studies, the influence of gait alterations consistent with barefoot running and expected from the plantar-sensory feedback hypothesis have not been examined. Specifically, altered distance from point of contact to centre of mass has received little attention. Furthermore, the control of factors confounding comparisons between barefoot and shod running (shoe mass, stride length, foot-strike pattern and barefoot-running experience), while increasing internal validity, detract from ecological validity. Investigation of acute alterations resulting from simply removing ones shoes and running freely barefoot in runners new to barefoot running is required. There is also a need to express any change in oxygen cost between shod and barefoot running in the context of a pre-determined practically beneficial magnitude of change. This context is vital to understanding whether there might actually be any performance benefit. Such context has not been provided in previous studies on this topic.
The purpose of this study was to examine acute alterations in gait and oxygen cost of running in well-trained runners new to barefoot running and to examine the latter in the context of a change associated with improved running performance. We hypothesised that, as a result of greater sense of impact: 1. there would be adjustments in the gait of habitually-shod runners with no prior experience of running barefoot; Specifically, stride length and contact time would be reduced and stride rate increased, reducing the distance between initial foot contact and the hip joint when barefoot and; 2. the steady-state oxygen cost of running barefoot at a fixed running speed would be reduced compared to shod. In light of current equivocal findings, we also examined whether removal of shoe mass and / or gait adjustments could best account for any change in steady-state oxygen cost from shod-to-barefoot running.
Method
Subjects
With institutional ethics approval, thirteen well-trained distance runners (8 male, 5 female) participated. The calibre of runners ranged from good club to regional representation. All subjects trained at least 5 times per week and none had previous experience of structured/regular running barefoot. Mean ± standard deviation age, mass, stature and VO2max were 29 ± 2 years, 58.5 ± 9.3kg, 1.69 ± 0.1m and 60.9 ± 3.6ml.kg-1.min-1 for the females, and 24 ± 6 years, 71.8 ± 5.1kg, 1.82 ± 0.1m and 64.6 ± 8.3ml.kg-1.min-1 for the males. Verified mean 10k race times were sub 40 min and sub 39 min for females and males respectively. Testing was carried out in April at the end of the general preparation stage of annual training for the subjects. Subjects were informed of the procedures and subsequently provided written-informed consent.
Experimental design
Subjects attended three treadmill-running sessions on separate days separated by at least 24 but never more than 72 hours for determination of VO2max and lactate threshold from an incremental test (visit 1) and steady-state oxygen uptake (VO2) and gait characteristics during six-minute shod and barefoot runs at individualised speeds below lactate threshold (visits 2 and 3). The order of barefoot and shod visits was counterbalanced. During visit 1 and the shod six-minute run, subjects wore their own cushioned-heel running shoes (mean shoe mass per pair 0.66 ± 0.10kg). All visits were completed at the same time of day and in similar environmental conditions (mean temperature 20.6 ± 1.5�C; barometric pressure 992 ± 22.3mb; relative humidity 31.0 ± 4.6 %). Subjects were instructed to attend test sessions well rested, well hydrated, having not eaten in the two hours prior to testing, and to have refrained from caffeine and alcohol consumption and heavy exercise for the previous twelve hours.
Procedures
Visit 1 - Incremental-treadmill test: Subjects completed an incremental running test comprising two parts. In part one, subjects ran at increasing speeds for 6-10 four-minute stages on a motorised treadmill (Model 3p 4.0, H/P Cosmos Quasar Medical treadmill, Nussdorf-Traunstein, Germany) starting between 9 and 12km�h-1 (depending on 10k PB time) with 0.5km�h-1 increases at the end of each stage. Treadmill gradient was set at 1% to reflect the additional energy cost of outdoor running [23]. Oxygen uptake was calculated continuously from expired air samples using an online breath-by-breath system (Cortex metalyzer 3B, GmbH, Germany). The analyser was calibrated before each test using room air and a span gas of known concentrations of O2 and CO2. Volume was calibrated using a 3-L syringe according to manufacturer's guidelines. During 60-second recoveries between stages, subjects stood astride the moving treadmill belt while a finger-prick capillary blood sample was taken for immediate determination of blood lactate concentration by an automated analyser (Biosen C-line, EKF Diagnostics). The test was terminated when subjects' blood lactate turn point was exceeded. Blood lactate turn point is defined as a second and sustained rise in blood lactate concentration usually occurring between 3-5mmol�L-1 [24]. The first increase in blood lactate above baseline values signified the lactate threshold and was determined after test termination [24]. The speed at which the threshold occurred was then recorded (sLT). The lactate analyser was calibrated before each test according to manufacturer's guidelines using a 5mmol�L-1 standard. Stability of the calibration was checked after each test using the same standard. Intra-sample coefficient of variation for the analyser was 0.47%. Subjects were allowed a minimum of 15 minutes recovery before commencing part two of the treadmill test.
Part two was used to assess maximal oxygen uptake (VO2max). The treadmill speed began at 4km�h-1 below the final running speed from part one. Subjects ran continuously with speed being increased by 0.5km�h-1 every 30 s until volitional fatigue. Five minutes after completion a finger prick blood sample was collected for analysis of blood lactate concentration. Oxygen uptake and heart rate were recorded continuously. A stationary-retrograde-time average of the breath-by-breath VO2 was calculated with the highest 30-s mean taken as the VO2max. The lowest speed that elicited the VO2max was recorded as the speed at VO2max (s VO2max).
Visits 2 and 3 - Steady-state physiological and gait testing: Twenty percent of the difference between VO2 at lactate threshold and VO2max was calculated for each subject. This difference was subtracted from VO2 at the lactate threshold and subjects ran on the treadmill continuously for six minutes at the speed shown to elicit this VO2 (12.5 ± 2.1km�h-1) to ensure oxygen uptake steady state [25]. No instructions were given on how to run during either the shod or barefoot trials. Expired gas was continuously collected and analysed by an online breath-by-breath system as described above. A mean of VO2 in the final 60 seconds of each run was taken as the absolute oxygen cost of running in each condition. Test-retest (typical) error for steady-state oxygen uptake in our lab has been reported as 1.2ml.kg-1.km-1 (1.1%) [26].
Two 1-m infra-red timing strips were attached to the sides of the treadmill, level with the running surface, to record stride length, stride rate, contact and flight times at 1Khz (Opt jump-next, Micro gate, Bolzano, Italy). Before the run started, 25-mm reflective markers were positioned on the right acromion process, greater trochanter, femoral-lateral epicondyle, and lateral malleolus and on the posterior aspect of the calcaneus and distal end of the 1st metatarsal when barefoot, or directly over these landmarks when shod. A floodlight was used to illuminate the markers. Each run was filmed perpendicular to the plane of motion at 100 frames per second using a high-speed camera (A602fc-2, Basler, Ahrensburg, Germany) and transferred via fire wire to specialist motion analysis software (Motus 9.0, Vicon Motion Systems, Oxford, UK). Peak ankle-dorsi flexion and knee-flexion angle at mid stance were calculated and leg and vertical stiffness estimated [27] from 10-consecutive strides in the final minute of running. Mean stride rate and length, contact and flight times were determined from 30-consecutive strides in the final minute of exercise. The horizontal distance between initial point of ground contact and the hip marker was also calculated. Foot-striking technique was classified by ankle angle at contact. A dorsiflexion angle at initial impact (a positive angle relative to horizontal) was classified as a rear-foot strike and a plantar-flexion angle (negative relative to horizontal) was classified as a forefoot strike [28].
Calculation of the oxygen cost of running: To ensure a valid comparison of the oxygen cost of barefoot and shod running, oxygen cost of the shod trial was expressed relative to body mass including shoe mass so that the relative oxygen cost reflected that of propelling the total mass of the subject including shoes. To account for individual differences in the running speed at which oxygen cost was assessed, the oxygen cost relative to body mass was corrected for speed and expressed as ml.kg-1.km-1 using the following calculation [24]:
ml.kg-1.km-1 = (ml.kg-1.min-1 × 60) ÷ speed
Statistical analysis
Mean and standard deviation of all response variables were calculated for the shod and barefoot runs. After confirmation of underpinning assumptions, 90% confidence intervals (90% CI) were used to estimate population mean differences between barefoot and shod conditions on all response variables expressed as change from the shod condition in absolute units and as percentage change. Differences in all variables were further examined using a magnitude-based inference approach in relation to a standardised smallest-worthwhile change of 0.2 (standard deviation units) for gait variables [29] and 4% for the oxygen cost of running. The smallest-worthwhile change for the oxygen cost of running was determined a priori and based on the mean reduction resulting from six to nine weeks of plyometric-training in well-trained male runners [30,31], a change that was accompanied by a 2.7% improvement in 3km running performance [31]. The magnitude-based inference approach provides the probability/chance that the true population mean change exceeds or is less than the smallest-worthwhile change. The chosen smallest-worthwhile change for the oxygen cost of running far exceeded the test-retest measurement error of our equipment as reported earlier. Change in oxygen cost from shod to barefoot conditions was also predicted based on removal of shoe mass [19] and compared to actual change in oxygen cost to examine the 'shoe-mass' explanation of oxygen cost reduction with barefoot running. Relationships between change in selected gait variables and change in oxygen cost (expressed as a ratio of barefoot to shod) were examined against a smallest-important correlation coefficient of ± 0.1 [29]. Change in foot strike pattern from shod to barefoot condition was simply described as frequencies in each condition. Due to a technical fault with the Opt jump equipment, contact time, flight time, stride rate and stride length data were not recorded in both conditions for some subjects. Only subjects with data from both conditions were included in analysis for the specified variables.
Results
Gait alterations
Changes in gait characteristics and confidence interval estimates of the true change are shown in table 1. In shoes, the majority of runners (9 of 13) landed on their heel. When barefoot, the majority of runners (8 of 13) landed on their forefoot. Four forefoot and four heel strikers did not alter their foot strike pattern between the conditions.
![]()
Table 1: Differences in gait characteristics in the final minute of six-minute shod and barefoot steady-state treadmill runs at the same relative intensity in well-trained habitually-shod runners
View Table 1
Oxygen cost of running
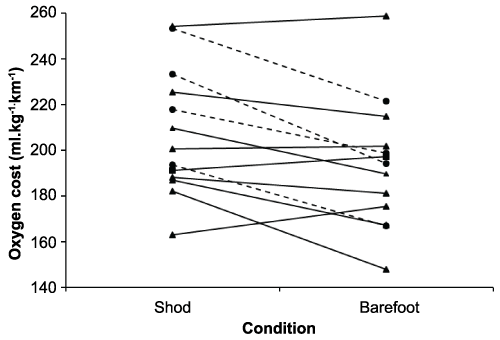
Mean relative oxygen cost of running was lower in the barefoot condition compared to shod (-14.2ml�kg-1�km-1; 90% CI -22.5 to -5.9ml�kg-1�km-1: -7%; 90% CI -11% to -3%). The likelihood of the true population mean reduction in oxygen cost when barefoot exceeding the smallest-worthwhile reduction associated with improved running performance (4%) was 90%. Variability in response was very large however, ranging from a 19% reduction to an 8% increase in oxygen cost of barefoot compared to shod running. Figure 1 illustrates individual differences in relative oxygen cost of running between the shod and barefoot conditions and the mean response.
.
Figure 1: Individual steady-state oxygen cost during the final minute of six-minutes of shod and barefoot treadmill running at a common relative-submaximal intensity in well-trained runners (n=13). Circle markers (dashed lines) indicate runners that changed from heel striking when shod to forefoot striking when barefoot. Triangle markers (solid lines) indicate runners that maintained their shod foot strike type when barefoot.
View Figure 1
Relationship between gait change and oxygen cost change
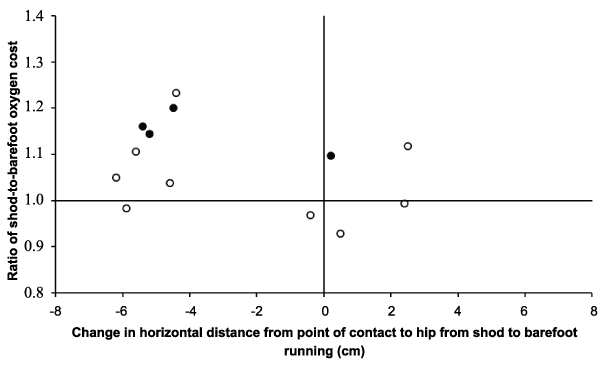
Figure 2 shows that as the change in horizontal distance between point of initial ground contact and the hip reduced, the ratio of shod-to-barefoot oxygen cost increased. A higher ratio represents a greater decrease in oxygen cost from shod to barefoot; ratios above one indicate a reduction in oxygen cost of barefoot compared to shoe running. Values to the left of the vertical line represent a reduction in the distance between initial point of contact and the hip. There was a negative association between the ratio of shod-to-barefoot oxygen cost and the change in horizontal distance between point of initial ground contact and the hip (r=-0.41; 90% CI -0.74 to -0.08; 86% likely negative association), indicating that a decrease in horizontal distance between point of contact and the hip was related to a decrease in oxygen cost of running from shod to barefoot. There was also a negative association between reduction in oxygen cost shod to barefoot and increase in ankle dorsi-flexion angle at mid stance (r=-0.43; 90% CI -0.76 to -0.06; 87% likely negative association) indicating greater ankle dorsi-flexion at mid stance was related to greater reduction in oxygen cost from shod to barefoot running.
.
Figure 2: The ratio of shod-to-barefoot oxygen cost in the final minute of 6-minute treadmill runs at the same relative intensity in well-trained runners (n=13), against reduction in horizontal distance between initial point of contact and the hip. Filled circles indicate runners that changed from heel striking when shod to forefoot striking when barefoot.
View Figure 2
Shoe-mass effect
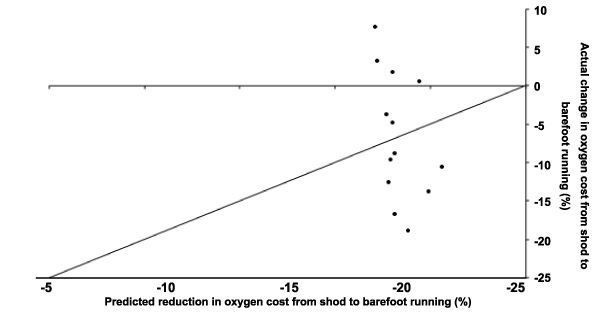
The mean percentage change in actual oxygen cost from shod to barefoot compared to that predicted on the basis of removal of shoe mass were not different but there was substantial individual difference about this mean response (0.0%; 90% CI -4.3 to 4.3%). Despite the actual and predicted mean reductions being similar, figure 3 shows that removing the mass of the shoes did not account for the actual reduction in oxygen cost from shod to barefoot running in any subject as none fell on the line of equality where actual and predicted oxygen uptake were equal. The mean response is therefore misleading.
.
Figure 3: Individual % change in steady-state oxygen cost from shod to barefoot running in well-trained runners (n=13) against the % reduction predicted on the basis of removal of individual shoe mass. The diagonal line of equality represents the position of no difference between actual change and predicted reduction.
View Figure 3
Discussion
The purpose of this study was to investigate the acute effects of removing shoes on gait characteristics and the oxygen cost of steady-state running in well-trained habitually-shod runners with no prior experience of running barefoot. We also aimed to express any change in oxygen cost in the context of a pre-determined practically beneficial magnitude of change.
Our results suggest that an average reduction in the steady-state oxygen cost of running, of a magnitude resulting from targeted training of 6-8 weeks that also improved performance [30,31], can be gained immediately by removal of shoes in well-trained runners. The likely oxygen cost reduction (-3% to -11%) included the values reported by two previous studies finding statistically significant reductions in oxygen cost with barefoot compared to shod running [15,16]. The likely range marginally excluded the statistically significant reduction (2.4%) recently reported by other authors comparing minimally-shod running to cushioned-shoe running, while accounting for shoe mass and controlling for foot strike pattern [17]. It has been argued that any benefits observed from shoe removal can be explained by the removal of shoe mass [18]. However, in light of significant reductions after controlling for mass and other confounds such as strike type, it has also been argued that altered gait patterns could explain reductions in oxygen cost [17]. The latter suggestion was supported by observed increases in arch strain and Achilles tendon Tricep-Surae Complex length (a proxy for strain energy storage in these structures) [17]. The mean reduction we observed (6.6%) could be explained by the removal of the mean shoe mass (660 g) as suggested by the 1%-per-100 g relationship [18,19]. However, the variability in response we observed (19% reduction to 8% increase in oxygen cost) was large and the 1% rule did not hold true for any of our subjects. The apparent similarity in means is simply an artefact of substantial reductions in excess of those predicted being cancelled out by some equally substantial increases in oxygen cost of barefoot compared to shod running opposing a predicted reduction. It is notable that subjects showing the greatest reduction in oxygen cost when barefoot (far greater than predicted by shoe-mass removal) were also those who switched foot strike pattern from a heel strike in shoes to a forefoot strike when barefoot. The number of those switching strike types was insufficient for a statistical comparison with those that did not. Nonetheless, such variability has also been reported elsewhere [17] and suggests that individual differences in technique alteration when switching from shod to barefoot running could be an important factor that has received little attention to date. It further suggests that changes in technique could result in oxygen cost reductions much larger than can be explained by shoe mass removal. Future work might consider examining less experienced runners to see if similar variability in first-time responses exists. Regardless of the mechanisms explaining the observed mean reductions in the oxygen cost of running, our data suggest that a meaningful reduction, previously linked to improved running performance, can be gained rapidly in some well-trained runners for whom running barefoot is novel. To our knowledge, this is the first study placing oxygen cost changes between shod and barefoot or minimally-shod running into a performance context. However, in light of the large variability in response (some subjects were less economical barefoot), care must be taken in assuming the mean response will apply to all runners.
Our primary aim was to examine acute responses in subjects new to running barefoot to assess changes expected from the plantar-sensory feedback hypothesis, so we did not control for factors such as stride rate, strike type or shoe mass necessary for clear examination of mechanistic explanations. However, we did measure gait variables to characterise the typical-acute alterations. Changes in stride characteristics from shod to barefoot were in agreement with previous studies, namely reduced stride length, increased stride rate and decreased contact time [6-9]. Though the observed average flight time was reduced, it was more variable than other measures resulting in an unclear estimate of the true population effect. In addition, we found leg and vertical stiffness, ankle dorsi-flexion angle and knee-flexion angle at mid stance to be increased in the barefoot condition, and the distance between initial point of ground contact and the hip to be reduced.
It has been suggested that changes in stride characteristics when barefoot arise as a strategy to avoid or to reduce impact force, loading rate and the discomfort associated with both [6]. The changes we and others have reported could be viewed as impact-avoidance strategies. These changes occurred without any prior familiarity with barefoot running, and over a relatively short time course of six minutes, suggesting that plantar-sensory feedback from the bare sole might be an important mediator of the running technique adopted at a fixed-submaximal speed. This lends support to the plantar-sensory feedback hypothesis [2]. Our design could not quantify the time course of such gait change. This will require studies to examine the change in gait characteristics from the beginning and throughout the time course of activity.
Theoretically, the observed gait changes could also serve to reduce the oxygen cost of running. The reduction in contact time could enhance re-utilisation of strain energy stored in the lower leg and longitudinal arch, particularly when viewed in conjunction with the increased leg and vertical stiffness and ankle dorsi-flexion angle we observed at mid stance. The negative relationship we observed between increase in ankle dorsi-flexion angle and reduction of oxygen cost support this suggestion. The reduction in distance between initial point of ground contact and the hip (a strategy that should reduce the likelihood of an impact-force transient) could also theoretically reduce oxygen cost by decreasing braking impulse and joint torques, thus making it less costly to maintain a constant speed. The relationship observed between the change in this distance and the change in oxygen cost supports this suggestion. Together, the two relationships between gait changes and oxygen cost reduction suggest that alteration in running technique could be a factor explaining an acute reduction in oxygen cost of barefoot running. Individual differences in the ability to make acute alterations to technique could indicate an element of skill in initial attempts at running without shoes and provide a possible explanation for the variability in responses that we and others have observed. A recent study reported no differences in economy between running in cushioned shoes and minimal/barefoot shoes at baseline in trained runners, but reported an improvement in economy in the minimal/barefoot shoe compared to the cushioned shoe after training in the minimal shoe for four weeks [32]. This indicates that familiarisation of running in minimal / barefoot shoes might be required and that associated changes in technique over a learning period are important to any improvements in running economy. This supports our suggestion that skill in making technique adjustments to a novel mode of running is an important consideration for future research. It also highlights the importance of examining patterns of variation around mean responses to barefoot running to gain a clearer understanding. Previous studies have tended to overlook this. Future studies might also consider bilateral kinematic analysis as calculation as the centre of mass could add further insight into the effects of gait alteration and its variability.
Perspectives
In well-trained distance runners with no experience of running barefoot, removing the shoes resulted in a reduction in the mean oxygen cost of steady-state running of a magnitude shown to benefit running performance. The mean reduction in oxygen cost was associated with some alterations to gait that could be viewed as impact/pain avoidance strategies in light of increased sense of impact, and are logical extensions of the plantar-sensory feedback hypothesis. However, both oxygen cost and gait changes are variable suggesting an element of skill in adapting to and gaining a benefit from initial attempts at barefoot running. Further research is needed to examine if running barefoot could be tolerated for longer durations and if the observed lab-based effect would transfer to actual improvements in competitive performance. More research is required before this practice would be recommended to habitually-shod runners, particularly in light of individual variation, as switching quickly from shod to barefoot running has been shown to increase injury risk to muscle and other tissues unaccustomed to the demands of running barefoot [33,34].
References
-
Jenkins DW, Cauthon DJ (2011) Barefoot running claims and controversies: a review of the literature. J Am Podiatr Med Assoc 101: 231-246.
-
Robbins SE, Gouw GJ, Hanna AM (1989) Running-related injury prevention through innate impact-moderating behavior. Med Sci Sports Exerc 21: 130-139.
-
Robbins SE, Hanna AM, Gouw GJ (1988) Overload protection: avoidance response to heavy plantar surface loading. Med Sci Sports Exerc 20: 85-92.
-
Robbins SE, Gouw GJ (1991) Athletic footwear: unsafe due to perceptual illusions. Med Sci Sports Exerc 23: 217-224.
-
Robbins SE, Hanna AM (1987) Running-related injury prevention through barefoot adaptations. Med Sci Sports Exerc 19: 148-156.
-
Lieberman DE, Venkadesan M, Werbel WA, Daoud AI, D'Andrea S, et al. (2010) Foot strike patterns and collision forces in habitually barefoot versus shod runners. Nature 463: 531-535.
-
Divert C, Mornieux G, Baur H, Mayer F, Belli A (2005) Mechanical comparison of barefoot and shod running. Int J Sports Med 26: 593-598.
-
De Wit B, De Clercq D, Aerts P (2000) Biomechanical analysis of the stance phase during barefoot and shod running. J Biomech 33: 269-278.
-
Squadrone R, Gallozzi C (2009) Biomechanical and physiological comparison of barefoot and two shod conditions in experienced barefoot runners. J Sports Med Phys Fitness 49: 6-13.
-
Burkett LN, Kohrt WM, Buchbinder R (1985) Effects of shoes and foot orthotics on VO2 and selected frontal plane knee kinematics. Med Sci Sports Exerc 17: 158-163.
-
Catlin MJ, Dressendorfer RH (1979) Effect of shoe weight on the energy cost of running. Medicine and Science in Sports and Exercise 11: 80.
-
Conley DL, Krahenbuhl GS (1980) Running economy and distance running performance of highly trained athletes. Med Sci Sports Exerc 12: 357-360.
-
Hanson NJ, Berg K, Deka P, Meendering JR, Ryan C (2011) Oxygen cost of running barefoot vs. running shod. Int J Sports Med 32: 401-406.
-
Frederick EC (1984) Physiological and ergonomics factors in running shoe design. Appl Ergon 15: 281-287.
-
Flaherty RF (1994) Running economy and kinematic differences among running with the foot shod, with the foot bare, and with the foot equated for weight. MSc, Springfield College.
-
Divert C, Mornieux G, Freychat P, Baly L, Mayer F, et al. (2008) Barefoot-shod running differences: shoe or mass effect? Int J Sports Med 29: 512-518.
-
Perl DP, Daoud AI, Lieberman DE (2012) Effects of footwear and strike type on running economy. Med Sci Sports Exerc 44: 1335-1343.
-
Franz JR, Wierzbinski CM, Kram R (2012) Metabolic cost of running barefoot versus shod: is lighter better? Med Sci Sports Exerc 44: 1519-1525.
-
Frederick E, Daniels JT, Hayes JW (1984) The effect of shoe weight on the aerobic demands of running. In: Bachl N, Prokop L, Suckert R. Current topics in sports medicine. Urban & Schwarzenberg, Vienna: 616-625.
-
Ker RF, Bennett MB, Bibby SR, Kester RC, Alexander RM (1987) The spring in the arch of the human foot. Nature 325: 147-149.
-
Alexander R, Goldspink G (1977) Mechanics and energetics of animal locomotion. Chapman and Hall Ltd: London.
-
Moore IS, Jones AM, Dixon S (2014) The pursuit of improved running performance: Can changes in cushioning and somatosensory feedback influence running economy and injury risk. Footwear Science 6: 1-11.
-
Jones AM, Doust JH (1996) A 1% treadmill grade most accurately reflects the energetic cost of outdoor running. J Sports Sci 14: 321-327.
-
Jones AM (2007) Middle- and long-distance running. In: Winter EM, Jones AM, Davison RC, Bromley PD, Mercer TH. Sport and exercise physiology testing guidelines: The british association of sport and exercise sciences guide, volume 1 - sport testing. Routledge: Oxford: 147-154.
-
Cooke CB (1996) Maximal oxygen uptake, economy and efficiency. In: Eston R, Reilly T. Kinanthropometry and exercise physiology laboratory manual: Tests, procedures and data, volume 2 - exercise physiology. Routledge, London: 161-193.
-
Hayes PR, French DN, Thomas K (2011) The effect of muscular endurance on running economy. J Strength Cond Res 25: 2464-2469.
-
Morin JB, Dalleau G, Kyr�l�inen H, Jeannin T, Belli A (2005) A simple method for measuring stiffness during running. J Appl Biomech 21: 167-180.
-
Gruber AH, Freedman Silvernail J, Brueggemann P, Rohr E, Hamill J (2013) Footfall patterns during barefoot running on harder and softer surfaces. Footwear Science 5: 39-44.
-
Batterham AM, Hopkins WG (2006) Making meaningful inferences about magnitudes. Int J Sports Physiol Perform 1: 50-57.
-
Saunders PU, Telford RD, Pyne DB, Peltola EM, Cunningham RB, et al. (2006) Short-term plyometric training improves running economy in highly trained middle and long distance runners. J Strength Cond Res 20: 947-954.
-
Spurrs RW, Murphy AJ, Watsford ML (2003) The effect of plyometric training on distance running performance. Eur J Appl Physiol 89: 1-7.
-
Warne JP, Warrington GD (2014) Four-week habituation to simulated barefoot running improves running economy when compared with shod running. Scand J Med Sci Sports 24: 563-568.
-
Ridge ST, Johnson AW, Mitchell UH, Hunter I, Robinson E, et al. (2013) Foot bone marrow edema after a 10-wk transition to minimalist running shoes. Med Sci Sports Exerc 45: 1363-1368.
-
Ryan M, Elashi M, Newsham-West R, Taunton J (2014) Examining injury risk and pain perception in runners using minimalist footwear. Br J Sports Med 48: 1257-1262.





