International Journal of Respiratory and Pulmonary Medicine
A Rare Case of Simultaneously Occurring Pulmonary Fungal Infections
William Li, Bhaskara Madhira* and Michael Kosters
SUNY Upstate Medical University, USA
*Corresponding author:
Bhaskara Madhira, MD, SUNY Upstate Medical University, 750 E. Adams St, Syracuse, NY 13210, USA, Tel: 314.691.8862, E-mail: Reddymab@upstate.edu
Int J Respir Pulm Med, IJRPM-4-068, (Volume 4, Issue 1), Case Report; ISSN: 2378-3516
Received: January 07, 2017 | Accepted: March 07, 2017 | Published: March 09, 2017
Citation: Li W, Madhira B, Kosters M (2017) A Rare Case of Simultaneously Occurring Pulmonary Fungal Infections. Int J Respir Pulm Med 4:068. 10.23937/2378-3516/1410068
Copyright: © 2017 Li W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Endemic infections produce a spectrum of illness ranging from being subclinical to severe progressive disseminated diseases with Immuno compromised individuals being increased risk. In those with an apparently non-improving infection, a simultaneously occurring second infectious source should be considered. Our patient was a 56 year-old immune compromised male with a history of active CML (Chronic Myelocytic Leukemia) undergoing chemotherapy who was receiving doxycycline and fluconazole for actinomycosis and coccidioidomycosis during a recent hospitalization. He presented with persistent non-productive cough, generalized weakness and malaise. A Chest X-Ray suggested worsening reticulonodular opacities and thoracic CT scan exhibited increasing innumerable pulmonary nodules bilaterally with worsening hilar lymphadenopathy. An open lung biopsy by Video Assisted Thoracoscopic Surgery performed revealed suppurative necrotizing granulomas associated with acute organizing bronchopneumonia with fungal organisms consistent with Blastomyces though did not reveal actinomyces. Deeper biopsy sections revealed the presence of spherules both with and without endospores characteristic of Coccidioides immitis concurrently. The patient symptomatically improved with treatment change to amphotericin B from fluconazole. To our knowledge there are no documented instances of co-infection with these particular two organisms. This particular case highlights the need to keep simultaneous endemic infections high in the differential in susceptible individuals who present with unclear findings and an apparently non-improving infectious etiology. The diagnosis of mixed fungal pulmonary infections is a difficult task which requires a high index of suspicion. In the future, cases with questionable mixed fungal infection may be deciphered by techniques different from current diagnostics including broad-range PCR with sequencing and FISH (fluorescence in situ hybridization).
Keywords
Coccidioides, Blastomyces, Fungal, Pulmonary, Infection, Immunocompromised
Introduction
Endemic pulmonary infections produce a spectrum of illness ranging from self-limited pneumonia to severe disseminated systemic disease. Immunocompromised individuals are especially at risk for such an infection and it's most severe complications. However, in those presenting with an apparent non-improving fungal pulmonary infection, a simultaneously occurring second endemic infectious source is an uncommon though serious possibility.
Case
Our patient was a 56-year-old immunocompromised male with a history of active CML (Chronic Myelocytic Leukemia) undergoing chemotherapy who presented with a persistent non-productive cough, generalized weakness and malaise. At the time of presentation he was also undergoing treatment with doxycycline 200 mg/day and fluconazole 400 mg/day for actinomycosis and coccidioidomycosis diagnosed via BAL (bronchoalveolar lavage) and sputum culture respectively during a recent hospitalization two weeks prior. Initial CBC (Complete Blood Count) and vital signs were unremarkable though a CXR (Chest X-Ray) suggested worsening reticulonodular opacities. A subsequent thoracic CT scan exhibited increasing innumerable pulmonary nodules bilaterally with worsening hilar lymphadenopathy in comparison to earlier imaging. An open lung biopsy by VATS (Video Assisted Thoracoscopic Surgery) was then performed revealing suppurative necrotizing granulomas associated with acute organizing bronchopneumonia with fungal organisms consistent with Blastomyces. Histological sections reviewed characteristic pseudoepitheliomatous epidermal hyperplasia, microabscesses within the epidermis and suppurative granulomatous dermal reaction on hematoxylin and eosin (H&E) and methenamine silver stain (Figure 1, Figure 2 and Figure 3). Given the history of coccidioidomycosis however, deeper biopsy sections were examined which revealed the spherules both with and without endospores characteristic of Coccidioides immitis concurrently. Because the patient continued exhibiting his non-productive cough and intermittent oxygen desaturation, treatment with amphotericin B 5 mg/kg daily was started and fluconazole was discontinued. The patient symptomatically improved over a three week period. Upon discharge, treatment was planned to continue for duration of at least 3 to 6 months. Since being discharged he has remained stable after three months of frequent outpatient follow-up appointments and associated interval improvement of reticulonodular opacities on CXR.
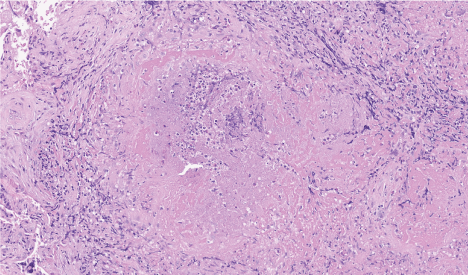
.
Figure 1: Histological sections showing pseudoepitheliomatous epidermal hyperplasia.
20X magnification section on H&E.
View Figure 1
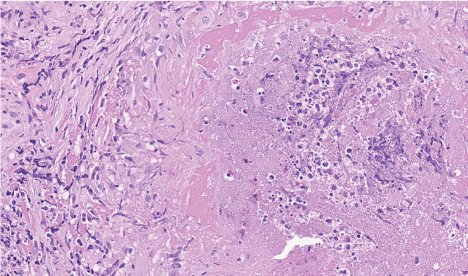
.
Figure 2: Epidermal microabscesses, suppurative granulomatous dermal reaction on hematoxylin and eosin (H&E) stain.
Full resolution section on H&E.
View Figure 2
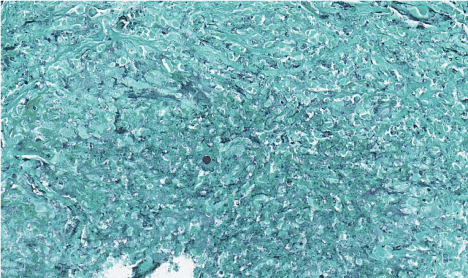
.
Figure 3: Grocott's methanamine silver.
Full resolution section on Grocott's methanamine silver.
View Figure 3
Discussion
Blastomyces dermatitidis and Coccidioides immitis are both dimorphic fungi with the potential to cause significant pulmonary and disseminated complications in immune compromised individuals. Because of this, it is essential to keep both high in the differential when caring for those at risk. The prevalence of each has been well documented with coccidioides being endemic to the southwestern US and Blastomyces to the central/southeastern US and central New York state. This particular case, however, does not follow the classic geographic pattern as the patient did not have any evidence of travel to highly endemic areas in the 6 months prior.
Unfortunately, the clinical manifestations of both are variable ranging from asymptomatic to fatigue, respiratory distress, weight loss or other non-specific complaints which make diagnosis challenging. Kaufman's raises awareness of increased international travel and overlooked historical environmental exposures such as to cotton mills and handling of raw cotton as factors requiring thorough investigation [1].
Dual concurrent fungal pulmonary infections are a seldom reported occurrence. To our knowledge there are no documented instances of co-infection with these particular two organisms. One instance of multiple fungal opportunistic infections did exist albeit in a HIV positive individual. That particular case however isolated each organism within different modalities with Cryptococcus seen in the lymph node biopsy, Pneumocystis jirovecii from the bronchoalveolar lavage and Aspergillus detected from the transbronchial biopsy [2]. Our case demonstrates a strong case for dual infection demonstrated in sections taken from the same sample.
Isolation of dimorphic fungal organisms is an extremely difficult task at times as organisms may have varied morphologic forms and histopathologic reactions. Layton's report of a fatal mixed infection with Blastomyces dermatitidis and Histoplasma capsulatum diagnosed postmortem during autopsy required close cooperation between the pathologist and microbiologist along with investigations under optimum conditions [3]. At present, diagnostic measures include serologic assays to detect fungal antigens or antibodies, though because neither show 100% sensitivity nor specificity, diagnostic cultures and isolation of colonies remain the standard [4]. In the future, cases with questionable mixed fungal infection may be deciphered by techniques including broad-range PCR with sequencing and FISH (fluorescence in situ hybridization) [5]. Also, the Bialek study suggests identification of Coccidioides and Blastomyces isolates are possible via chemi luminescent DNA probes or PCR assays targeting multicopy ribosomal genes in conjunction with sensitivity and specificity of the PCR assays determined by comparative studies using stage-specified clinical specimens [6]. This raises the possibility of more definitive diagnostic strategies when the current standard of care presents inconclusive or questionable findings. This is seen in previous instances where individuals have been misdiagnosed with carcinoma or as one dimorphic organism over another given atypical findings [7].
In regards to treatment effectiveness, Chapman's review on blastomycosis management guidelines suggests amphotericin B to be most effective option with an 86.5% cure rate and only 3.9% relapse rate in one large retrospective series. The same review also reported only a 65% cure rate in a one particular pilot study with 200-400 mg/d of fluconazole being the treatment of choice [8]. They did, however, note higher efficacy in a separate larger multicenter randomized open-label study where higher dosages (400-800 mg/d) of fluconazole were use [9]. In regards to coccidioidomycosis, the infectious diseases society currently recommends fluconazole and itraconazole as first line agents with amphotericin B being reserved for patients with respiratory failure due to the infection, those with rapidly progressing infection or infected women during pregnancy though efficacy remains comparable [10]. Our patient seemingly was non-improving despite three weeks of appropriately dosed fluconazole while appearing to improve with amphotericin B. The basis for success of the latter treatment is arguably twofold given amphotericin B's indication in those with worsening respiratory disease in coccidioidomycosis and also being the treatment of choice for the newly diagnosed blastomycosis.
Conclusion
The diagnosis of mixed fungal pulmonary infections is a difficult task which requires a high index of suspicion. The current standard of care for definitive diagnosis consists of bronchoscopy with biopsy and analysis of sections. However, as in the case of our patient, mixed infection with more than one endemic organism is a diagnosis that should not be overlooked especially in the non-improving patient. This case also raises the need to consider alternative diagnostic tools such as PCR with sequencing and FISH in the future in order to improve morbidity and mortality for at risk individuals in such a rare occurring medical dilemma.
References
-
Kaufman L, Valero G, Padhye AA (1998) Misleading manifestations of Coccidioides immitis in vivo. J Clin Microbiol 36: 3721-3723.
-
Mihon C, Alexandre T, Pereira A (2013) Clinical experience in invasive fungal infections: multiple fungal infection as the first presentation of HIV. Clin Drug Investig 1: 37-40.
-
Layton JM, Mckee AP, Stamler FW (1953) Dual infection with Blastomyces dermatitidis and Histoplasma capsulatum; report of a fatal case in man. Am J Clin Pathol 23: 904-913.
-
Pounder JI, Hansen D, Woods GL (2006) Identification of Histoplasma capsulatum, Blastomyces dermatitidis, and Coccidioides Species by Repetitive-Sequence-Based PCR. J Clin Microbiol 44: 2977-2982.
-
Rickerts V, McCormick Smith I, Mousset S, Kommedal O, Fredricks DN (2013) Deciphering the aetiology of a mixed fungal infection by broad-range PCR with sequencing and fluorescence in situ hybridisation. Mycoses 56: 681-686.
-
Bialek R, González GM, Begerow D, Zelck UE (2005) Coccidioidomycosis and blastomycosis: Advances in molecular diagnosis. FEMS Immunol Med Microbiol 45: 355-360.
-
Lee CH, Wilcox L, Chorneyko K, McIvor A (2008) Coccidioides immitis: two cases of misidentified mycosis. Can Respir J 15: 377-379.
-
Chapman SW, Bradsher RW Jr, Campbell GD Jr, Pappas PG, Kauffman CA (2000) Practice guidelines for the management of patients with blastomycosis. Infectious Diseases Society of America. Clin Infect Dis 30: 679-683.
-
Pappas PG, Bradsher RW, Kauffman CA, Cloud GA, Thomas CJ, et al. (1997) Treatment of blastomycosis with higher doses of fluconazole. The National Institute of Allergy and Infectious Diseases Mycoses Study Group. Clin Infect Dis 25: 200-205.
-
Galgiani JN, Ampel NM, Blair JE, Catanzaro A, Geertsma F (2016) 2016 Infectious Diseases Society of America (IDSA) Clinical Practice Guideline for the Treatment of Coccidioidomycosis. Clin Infect Dis 63: e112-e146.





