International Journal of Respiratory and Pulmonary Medicine
Possible Complication of Marking Hook Wire Entry into the Systemic Circulation during Video-Assisted Thoracoscopic Surgery
Hiromasa Arai1*, Michihiko Tajiri1, Kohei Ando1, Koji Okudela2, Tae Iwasawa3 and Munetaka Masuda4
1Department of General Thoracic Surgery, Kanagawa Cardiovascular and Respiratory Center, Japan
2Department of Pathology, Yokohama City University Graduate School of Medicine, Japan
3Department of Radiology, Kanagawa Cardiovascular and Respiratory Center, Japan
4Departoment of Surgery, Yokohama City University Graduate School of Medicine, Japan
*Corresponding author: Hiromasa Arai, Department of General Thoracic Surgery, Kanagawa Cardiovascular and Respiratory Center, 6-16-1 Tomiokahigashi, Kanazawa-ku, Yokohama, 236-8651, Japan, Tel: +81-45-701-9581, Fax: +81-45-786-4770, E-mail: hiromasa@jg7.so-net.ne.jp
Int J Respir Pulm Med, IJRPM-3-060, (Volume 3, Issue 4), Case Report; ISSN: 2378-3516
Received: July 22, 2016 | Accepted: October 14, 2016 | Published: October 17, 2016
Citation: Arai H, Tajiri M, Ando K, Okudela K, Iwasawa T, et al. (2016) Possible Complication of Marking Hook Wire Entry into the Systemic Circulation during Video-Assisted Thoracoscopic Surgery. Int J Respir Pulm Med 3:060. 10.23937/2378-3516/1410060
Copyright: © 2016 Arai H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A 63-year-old Japanese male suffering from interstitial pneumonia underwent computed tomography (CT) guided tumor localization using a hook wire and a suture system for a small pulmonary nodule suspected of being lung carcinoma. He underwent subsequent video-assisted thoracoscopic surgery. The cut suture connecting to the metal head of the hook wire in the lung parenchyma was visible at the beginning of the procedure. During the surgery, the suture was not able to be visualized. Finally, the patient underwent a left lower lobectomy without the diagnosis of malignancy, based on the possibility of loss of the hook wire into the systemic circulation. Whole body CT under general anesthesia after the surgery, and soft X-ray of the exenterated lung, and intrapulmonary inspection by the pathologist could not detect the hook wire anywhere. The final diagnosis of the tumor was primary lung squamous cell carcinoma; pStage Ia. By reviewing in detail the multi-planner reconstruction CT used to localize the tumor, we found that the hook wire was localized in the peripheral pulmonary vein. We concluded that the hook wire was accidentally inserted into the peripheral pulmonary vein neighboring the tumor. Then, the hook wire proceeded with the blood flow and exited from the lung parenchyma into the systemic circulation via the left atrium. There are some complications of using the CT guided hook wire marking procedure. This is the first report of the rare complication of the hook wire entering the systemic circulation.
Keywords
Computed tomography (CT), Hook wire, Localization, Systemic circulation, Video-assisted thoracoscopic surgery (VATS)
Background
Small lung nodules and pure ground glass opacity (GGO) lesions that cannot be located during surgery are increasingly being discovered due to the development of improved imaging technology and the prevalence of computed tomography (CT) screening for health checkups. The less invasive surgical technique, video-assisted thoracoscopic surgery (VATS), has also been rapidly developed. Detection of a target lesion mainly depends on visual confirmation or finger palpation through the manipulation holes. Thus, it is difficult to confirm these small or indeterminate tumors by palpation with a thoracotomy. There have been some techniques to localize tumors, such as intraoperative ultrasonography, transbronchially marking, and percutaneous marking using either a dye (e.g., methylene blue) or a hook wire and suture system. A CT-guided hook wire and suture system is widely accepted as a standard technique for tumor location. To the best of our knowledge, there are no reports on the complication of entry of the hook wire into the systemic circulation. Herein, we report a case with a missing hook wire, which we concluded had entered the systemic circulation during VATS.
Case Report
A 63-year-old Japanese male suffering from interstitial pneumonia (IP) was referred to our department because of an abnormal shadow in the left lung detected by CT. A small, irregular-shaped tumor that was suspected to be a malignant neoplasm was located in S9b-10b of the left lower lobe (Figure 1). VATS and intraoperative frozen diagnosis were scheduled. The tumor was located in a subpleural region, but was relatively small, at about 20 mm in diameter. Detecting the tumor in VATS was thought to be difficult, and therefore CT-guided tumor localization was scheduled prior to VATS.
On the day of surgery, the patient underwent CT-guided tumor localization using a hook wire (Guiding Marker System®, Hakko, Tokyo, Japan; introducer gauge size 21G and needle length 150 mm). The hook wire consisted of a stainless hook (φ0.28 × 10 mm) and a nylon suture (300 mm). The hook wire was inserted into the left lower lobe adjacent to the tumor under local anesthesia with the patient in a prone position. The procedure was completed without any problems. The patient was then taken directly to the operating room and VATS was started. After the left lung was deflated, the nylon suture connected to the hook wire head was visualized. This suture was cut with sufficient length near the chest wall to serve as a marking material (Figure 2a). As two different needle tumor biopsies adjacent to the wire insertion site for the frozen diagnosis did not identify malignant tissue on frozen section diagnosis, lung wedge resection was planned for frozen diagnosis. At this time, the presence of the shortened suture was confirmed retrospectively (Figure 2b). The lung ligament was dissected to liberate the lower lobe. When the lower lobe was turned to the neutral position, the suture tail could not be seen in the scope.
.
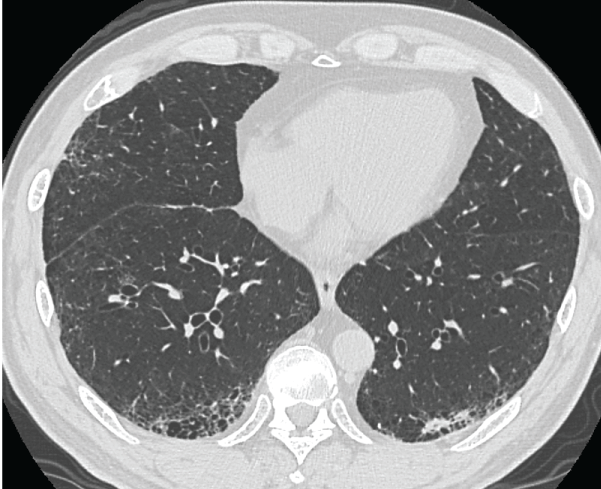
Figure 1 Chest CT showing the shadow of an irregularly-shaped mass neighboring the interstitial pneumonia lesion in the left S9b-S10b region.
View Figure 1
.
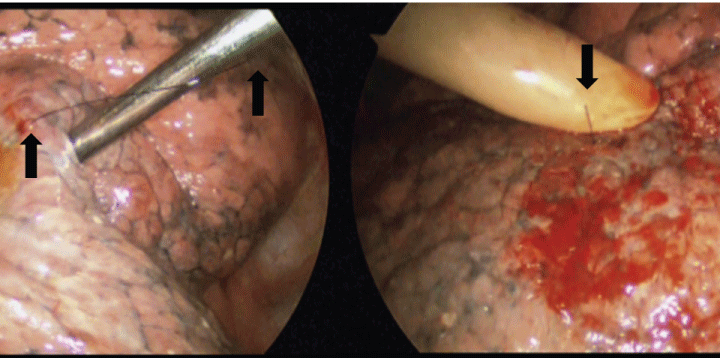
Figure 2 Intraoperative findings. a) The nylon suture was cut with sufficient length as a marking material (arrows); b) The suture had shortened with time (arrow).
View Figure 2
We searched for the suture in the thoracic cavity multiple times, but could not locate it. A portable X-ray was also used, but we were unable to detect the item in the lung or chest wall. The possibility of entry of the hook wire into the peripheral pulmonary vein was considered. A diagnosis of malignancy was not obtained, but the decision was made to perform left lower lobectomy to avoid outflow of the hook wire from the lung parenchyma to the systemic circulation. First, the inferior pulmonary vein was transected, then the pulmonary arteries and the lower lobe bronchus were also dissected using tissue-appropriately sized endo-staplers. Finally, the left lower lobe was extracted from the thoracic cavity using an endo-sack. Thus, left lower lobectomy with VATS (1 window: 30 mm + 3 ports: 5 mm) was completed. Immediately CT imaging and soft X-ray of the exenterated lung were performed with the same type of the hook wire. Intrapulmonary inspection and frozen diagnosis of the tumor were also performed by a pathologist.
After the operation, the patient underwent whole body CT scanning (1 mm slice), including his head, and electrocardiogram (ECG)-gated cardiac CT (1 mm slice) under general anesthesia. In addition, the exenterated lung was dissolved by a medical cleaner containing hypochlorous acid after the permanent pathological examination. Despite these detailed searches by the surgeons, the radiologist, and the pathologist, the hook wire could not be detected anywhere. The final diagnosis was primary lung squamous cell carcinoma pStage IA. His postoperative clinical course was uneventful, and he was discharged from the hospital on the 10th postoperative day without any complications. Whole body CT after 13 months revealed no recurrence of the carcinoma and no foreign body defining the hook wire.
Discussion
CT-guided hook wire marking is a useful, safe, reliable and convenient procedure, and is now accepted as the standard approach for small, indeterminate lung tumors and pure GGO lesions [1-5]. However, mild to severe complications have been reported, including pneumothorax (18.6 to 32.1%) [1-3,6], intrapulmonary bleeding (14.9 to 16.3%) [1-3,6], dislodgement/loss of the hook wire (6.4 to 7.0%) [2,5], hemothorax due to accidental puncture of the intercostal vessel (0.6 to 2.3%) [2,3], migration to the chest wall [6], and arterial air embolization [1]. In our institute, CT-guided hook wire marking has been performed in 138 cases in the past 12 years. Five patients (3.6%) had asymptomatic pneumothorax and one (0.7%) had slight intrapulmonary bleeding. In another patient (0.7%), the metal head migrated to the chest wall and was detected by chest CT under general anesthesia and removed. There have been no complications requiring emergency treatment to date.
In the current case, the hook wire was lost during the operation. Several possibilities were considered. First, the hook wire might still have been in the body, but undetectable with imaging. Alternatively, it may have exited the body through accidental insertion into the peripheral bronchus or pulmonary vein. Retrospectively, we performed a detailed review of the preoperative multiplanar reconstruction CT scans used to localize the tumor and found that the hook wire seemed to be located in the peripheral pulmonary vein (Figure 3).
.
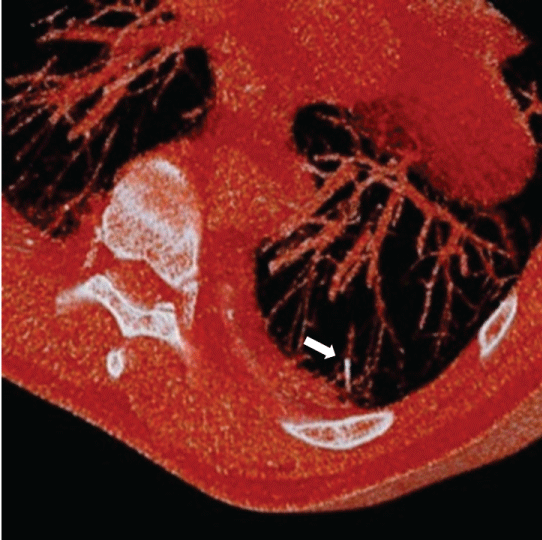
Figure 3 Preoperative multiplanar reconstruction CT. The hook wire seemed to be inserted into the peripheral pulmonary vein (arrow).
View Figure 3
The facts in this case were as follows: a) absence of the hook wire in the thoracic cavity and chest wall, b) shortening of the nylon suture over time in thoracoscopic recordings, c) absence of the hook wire in the exenterated lung on soft X-ray and CT and in the dissolved lung, d) no observation of the hook wire on whole body CT, and e) the possibility of the hook wire entering the peripheral pulmonary vein, as seen on CT. We concluded that the hook wire might have accidentally inserted into the peripheral pulmonary vein neighboring the tumor, moved with the blood flow, and then exited from the lung parenchyma to the systemic circulation via the left atrium. This scenario is somewhat unlikely and difficult to establish with certainty, but it is theoretically possible. To prevent this complication, we now use titanium hemostatic clips to secure the suture tail during VATS (Figure 4).
Our case represents one of the rare but important, possible complications of CT guided hook wire marking. Based on this case, we conclude that surgery must be performed with great care when a hook wire is in the lung parenchyma and the suture should be maintained in the scopic view at all times during VATS.
References
-
Sato K, Miyauchi K, Shikata F, Murakami T, Yoshioka S, et al. (2005) Arterial air embolism during percutaneous pulmonary marking under computed tomography guidance. Jpn J Thorac Cardiovasc Surg 53: 404-406.
-
Chen YR, Yeow KM, Lee JY, Su IH, Chu SY, et al. (2007) CT-guided hook wire localization of subpleural lung lesions for video-assisted thoracoscopic surgery (VATS). J Formos Med Assoc 106: 911-918.
-
Dendo S, Kanazawa S, Ando A, Hyodo T, Kouno Y, et al. (2002) Preoperative localization of small pulmonary lesions with a short hook wire and suture system: experience with 168 procedures. Radiology 225: 511-518.
-
Xu X, Yao Y, Shen Y, Zhang P, Zhou J (2015) Clinical Analysis of Percutaneous Computed Tomography-Guided Hook Wire Localization of 168 Small Pulmonary Nodules. Ann Thorac Surg 100: 1861-1867.
-
Miyoshi K, Toyooka S, Gobara H, Oto T, Miura H, et al. (2009) Clinical outcome of short hook wire and suture marking system in thoracoscopic resection for pulmonary nodules. Eur J Cardiothorac Sur 36: 378-382.
-
Chen X, Wang S, Hao Z, Ma Q (2014) Wire 'missing': a rare presentation of preoperative localization wire system dislocation. J Cardiothorac Surg 9: 162.