International Journal of Respiratory and Pulmonary Medicine
Sarcoidosis Presenting with Severe Thrombocytopenia
Yusuf Kayar1*, Nuket Bayram Kayar2, Nurcan Unver3 and Iskender Ekinci1
1Department of Internal Medicine, Bezmialem Vakif University, Turkey
2Department of Family Medicine, Bagcilar Education and Research Hospital, Turkey
3Department of Pathology, Bezmialem Vakif University, Turkey
*Corresponding author: Yusuf Kayar, MD, Department of Internal Medicine, Bezmialem Vakif University, Vatan street, Fatih/Istanbul/Turkey 34093, Tel: +90 212 453 1700, Fax: +090 212 3735 000, E-mail: ykayar@yahoo.com
Int J Respir Pulm Med, IJRPM-3-056, (Volume 3, Issue 3), Case Report; ISSN: 2378-3516
Received: July 30, 2016 | Accepted: August 30, 2016 | Published: September 02, 2016
Citation: Kayar Y, Kayar NB, Unver N, Ekinci I (2016) Sarcoidosis Presenting with Severe Thrombocytopenia. Int J Respir Pulm Med 3:056. 10.23937/2378-3516/1410056
Copyright: © 2016 Kayar Y, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Sarcoidosis is a systemic granulomatous disorder of unknown causes. Haematological manifestations in sarcoidosis are uncommon and may include haemolytic anemia, leukopenia, eosinophilia and peripheral lymphopenia, but severe thrombocytopenia is rare. Causes of thrombocytopenia in sarcoidosis were identified a few mechanisms. There are no current guidelines concerning the treatment of thrombocytopenia in sarcoidosis. However, in emergency situations with major thrombocytopenia, it seems reasonable to apply current guidelines recommended forIdiopathic Thrombocytopenic Purpura. We reported a case of sarcoidosis presenting with severe thrombocytopenia, petechial rash and gingival bleeding.
Keywords
Sarcoidosis, Severe thrombocytopenia, Petechial rash
Introduction
Sarcoidosis is a systemic granulomatous disorder of unknown causes.Haematological manifestations in sarcoidosis are uncommon and may include haemolytic anemia, leukopenia, eosinophilia, peripheral lymphopenia and thrombocytopenia, but severe thrombocytopenia is very rare [1,2]. Although thrombocytopenia in sarcoidosis was first described in 1938 by Jersild M [3], its frequency is still unknown, and there is no data available in most sarcoidosis clinical studies. Nevertheless, in retrospective studies thrombocytopenia in sarcoidosis is reported as 1-2% [1,2]. Although quite rare, hemorrhage and thrombocytopenia may be the first presenting signs of sarcoidosis [1]. We reported a case of sarcoidosis presenting with severe thrombocytopenia, petechialrash and gingival bleeding.
Case
A 56-year-old female patient was hospitalized with complaints of coughing and shortness of breath for about two weeks and rash on the legs and gingival bleeding for a week. The patient did not report any chronic illnesses or use of any medications, alcohol or smoking. There were not significant feature in her familial medical history. Physical examination detected maculopapular rash on bilateral legs and petechiae on both legs and arms. Her laboratory results were: Leukocyte: 6.2 × 103/μL, hemoglobin: 12.7 g/dl, platelet: 5.1 × 103/μL, gammaglobulin was 3.1 g/dl; sedimentation 75 mm/hour; and C-reactive protein 4.6 mg/dl. Creatinine, BUN, hepatic function tests, calcium, coagulation tests, fibrinogen, and D-dimer levels were normal. Viral serology was negative. Chest radiography detected bilateral hilar adenopathy. No pathology was observed in abdominal tomography. Pathological lymph nodes were observed at bilateral hilus and mediastinalin the thorax tomography (Figure 1). Respiratory function test and carbon monoxide diffusion test were normal. No pathology other than thrombocytopenia was observed in peripheral smear. Bone marrow biopsy revealed normal myeloid and erythroid series, but increased and hyperplastic megakaryocytes. The patient's quantiferon test was negative, while her level of angiotensin converting enzyme was high at 124 U/ml (16-53 U/ml). The patient was tested for autoantibodies (Antinuclear Antibodies, Anti-Neutrophil Cytoplasmic Antibody, Rheumatoid Factor, Extractable Nuclear Antigen Antibodies) with regards to collagen tissue diseases and vasculitis, and the test result was negative. Serum platelet antibody test was positive (1/128 titrated). Mediastinoscopy was used to sample mediastinal adenopathies. Histopathological examination detected granulomas without necrosis (Figure 2). Based on these findings, the patient was diagnosed with sarcoidosis with mediastinal lymph node and skin involvement, presenting with thrombocytopenia, and was administered treatment with methylprednisolone at a dose of 1 mg/kg/day. The patient was checked three months later and was observed to have an apparent decrease in hilar adenopathy, recovery in skin symptoms, and a platelet count of 125 × 103/μL. The methylprednisolone dose reduced and therapy was continued with low dose methylprednisolone (8 mg/day). The patient followed under treatment with methylprednisolone for about one year. She had not any side effect.
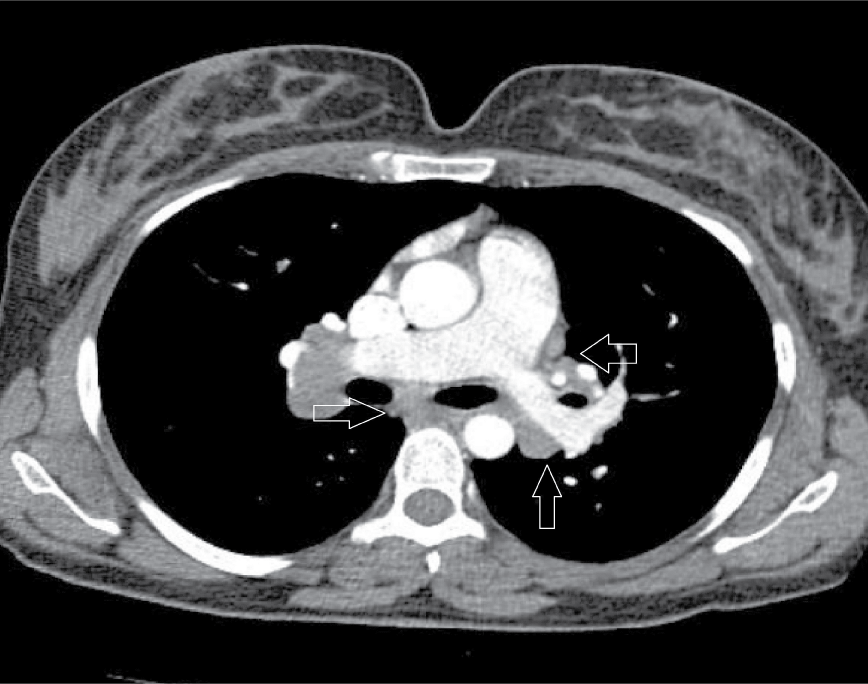
.
Figure 1 Pathological lymph nodes were observed at bilateral hilus and mediastinal in the thorax tomography.
View Figure 1
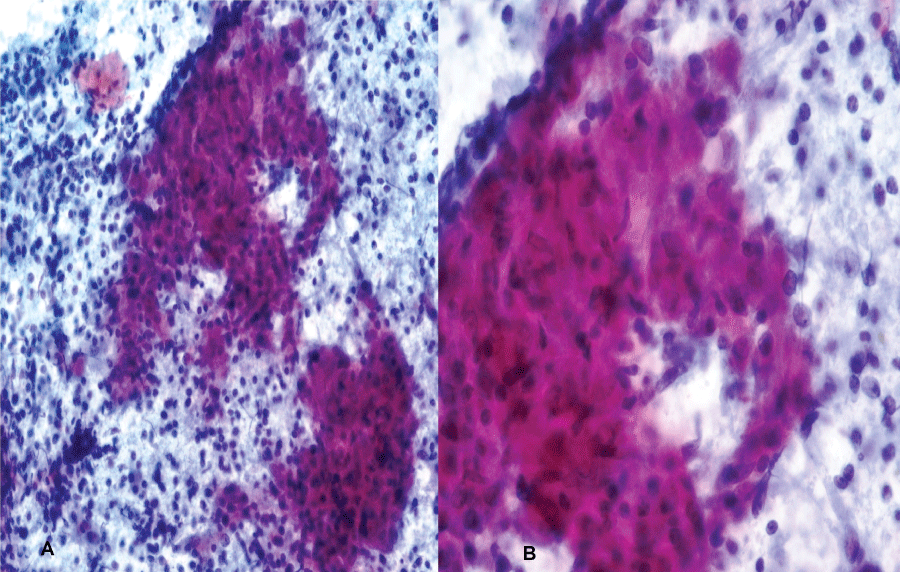
.
Figure 2: Granuloma-like structure (communities of eosinophilic syncytial epithelioid histiocytes) and mixed type mononuclear inflammatory cells in the granular surface. (A): PAP stain × 200; (B): PAP stain × 400 (PAP stain).
View Figure 2
Discussion
Although rare, the association of thrombocytopenia with sarcoidosis has been fully documented. A review of 381 cases of thrombocytopenic purpura showed five patients with sarcoidosis (1%) and in a series of 324 patients with sarcoidosis, 2% had thrombocytopenia defined as a platelet count of less than 100 × 103/μL [2]. Moulis, et al. reported that; sarkoidosis constitutes 0.62% of all immune thrombocytopenia (ITP) patients and 3.47% of secondary ITP patients [4].
Causes of thrombocytopenia in sarcoidosis were identified as three main mechanisms. Many mechanisms may be implicated in the same patient. The first physiopathological hypothesis of thrombocytopenia in sarcoidosis is related to hypersplenism and splenomegaly. Splenomegaly prevalence was assessed at 10% by Fordice, et al., collected 6,074 cases of sarcoidosis in 29 publications [5]. Autopsy series detected spleen granulomas among 60% of cases [5]. Sequestration in the spleen leads to platelet destruction. In few cases, splenomegaly is associated with hypersplenism secondary to portal hypertension and peripheral pancytopenia. Moreover, moderate splenomegaly is also compatible with an autoimmune mechanism, which leads to a peripheral destruction of platelets. Nevertheless, thrombocytopenia related to hypersplenism in sarcoidosis must always be suspected in a patient with splenomegaly and varying degrees of cytopenia (leukopenia, anaemia, thrombocytopenia) [1]. Bone marrow involvement is the second mechanism. Bone marrow granulomatous infiltration in sarcoidosis seems to be rare and not clearly associated with thrombocytopenia. In the Access Research Group Study, 29 (3.9%) of the 736 patients presented with granulomas in bone marrow, but blood cell count modifications were not reported [6]. The third mechanism is autoimmunity. Many immunological aberrations in sarcoidosis have been observed, including the T helper 1 driven granulomatous response and an effusive humoral immune reaction. Autoimmune haemolytic anaemia and idiopathic thrombocytopenic purpura (ITP) have been reported in sarcoidosis. In 1985, Lawrence found an elevation of platelet associated IgG in a patient with thrombocytopenia and sarcoidosis and speculated an antibody mediated destruction of the platelets [7]. Many immunological abnormalities are described in sarcoidosis. Peripheral lymphopenia contrasts with recruitment of T helper cells at sites of active disease. Proliferation of B cells stimulated by activated T cells is reflected by the polyclonal hypergamaglobulinaemia that is so characteristic of sarcoidosis. Lawrence and Greenberg speculated that the non-specific B cell activation may occasionally lead to production of antibodies to platelet antigens and thus cause severe thrombocytopenia [2,7]. The presence of megakaryocytic hyperplasia in the bone marrow and a good response to corticosteroid therapy suggest that the thrombocytopenia was due to immune destruction in our patient.
There are no current guidelines concerning the treatment of thrombocytopenia in sarcoidosis. In the literature, steroids may be recommended in the first intention and could act in all physiopathological mechanisms involved (granulomas in bone marrow, splenomegaly and autoimmune process). However, in emergency situations with major thrombocytopenia, it seems reasonable to apply current guidelines recommended for ITP. These require intensive therapy: methylprednisolone (1 g/day for two days) or/and intravenous immunglobulin (IG-Iv) (1 g/kg per day for 3 days) and whenever needed, platelet transfusions. Splenectomy should be reserved for patients whose thrombocytopenia is not controlled by steroid or IG-Iv therapy. Also aziathioprine, cyclophosphamide, vincristine and adalimubab, rituximab might be used [1].
In conclusion thrombocytopenia in sarcoidosis is a rare event. Different physiopathological mechanisms are responsible of thrombocytopenia in sarcoidosis. Granulomas in bone marrow or hypersplenism may be involved. ITP must be suspected in all other cases. Steroids remain the most effective treatment and must be proposed in the first intention.
References
-
Mahévas M, Le Page L, Salle V, Lescure FX, Smail A, et al. (2006) Thrombocytopenia in sarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis 23: 229-235.
-
Larner AJ, Dollery CT, Cox TM, Bloom SR, Scadding JG, et al. (1990) Life threatening thrombocytopenia in sarcoidosis. BMJ 300: 317-319.
-
Jersild M (1938) The syndrome of Heerfordt (uveo-parotid fever), a manifestation of Boek's sarcoid. Act Med Scand 97: 322-328.
-
Moulis G, Palmaro A, Montastruc JL, Godeau B, Lapeyre-Mestre M, et al. (2014) Epidemiology of incident immune thrombocytopenia: a nationwide population based study in France. Blood 124: 3308-3315.
-
Fordice J, Katras T, Jackson RE, Cagle PT, Jackson D, et al. (1992) Massive splenomegaly in sarcoidosis. South Med J 85: 775-778.
-
Judson MA, Baughman RP, Teirstein AS, Terrin ML, Yeager H (1999) Defining organ involvement in sarcoidosis: the ACCESS proposed instrument. ACCESS Research Group. A Case Control Etiologic Study of Sarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis 16: 75-86.
-
Lawrence HJ, Greenberg BR (1985) Autoimmune thrombocytopenia in sarcoidosis. Am J Med 79: 761-764.





