International Journal of Respiratory and Pulmonary Medicine
Impact of Bariatric Surgery on Obstructive Sleep Apnoea in Morbidly Obese Patients; Single Centre Experience and a Literature Review
Muhammad Ali Karim1, Muhammad Josheel Naveed2, Amir Hussein3 and Abdulmajid Ali1*
1Department of Surgery, University Hospital Ayr, UK
2Department of Chest Medicine, Aintree University Hospital, UK
3Department of General surgery, University Hospital Ayr, UK
*Corresponding author: Mr. Abdulmajid Ali, Consultant Upper GI and Bariatric Surgeon, Department of Surgery, University Hospital Ayr, Ayrshire and Arran, Dalmellington Road, KA6 6DX, UK, E-mail: abdulmajid.ali@aaaht.scot.nhs.uk
Int J Respir Pulm Med, IJRPM-3-055, (Volume 3, Issue 3), Original Article; ISSN: 2378-3516
Received: May 31, 2016 | Accepted: August 26, 2016 | Published: September 01, 2016
Citation: Karim MA, Naveed MJ, Hussein A, Ali A (2016) Impact of Bariatric Surgery on Obstructive Sleep Apnoea in Morbidly Obese Patients; Single Centre Experience and a Literature Review. Int J Respir Pulm Med 3:055. 10.23937/2378-3516/1410055
Copyright: © 2016 Karim MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: Bariatric surgery is an established treatment of morbid obesity and effectively controls symptoms of OSAHS. The aim of this study was to evaluate impact of bariatric surgery on OSAHS.
Methods: Validated Epworth Sleepiness Score (ESS) and STOP-Bang questionnaires were used to assess the impact of bariatric surgery on OSAHS in morbidly obese patient's undergone bariatric surgery from May 2008 to December 2011. Change in ESS, STOP-Bang score, weight and BMI, co-morbidities and CPAP requirement were recorded. EMBASE, MEDLINE and COCHRANE database were searched for relevant literature.
Results: 21 patients were included in the final analysis. There was a significant drop in the overall ESS and STOP-Bang scores of patients (p < 0.05). In 16 patients the symptoms of OSAHS resolved and improved in 1 patient. 89% of the patients did not require CPAP machine post operatively. 20 studies were included in the literature review. It was inferred from the literature review that within 12 months after surgery the reported improvement in OSAHS was up to 78% and between 40 to 60% resolution was reported in the long term follow up (84-144 months).
Conclusion: This study and the available literature strongly support bariatric surgery as an effective treatment of OSAHS. It should be considered in morbidly obese patients alongside other measures.
Keywords
Bariatric surgery, Weight loss surgery, Obstructive sleep apnoea, Gastric bypass, Sleeve gastrectomy
Abbreviations
LAGB: Laparoscopic Adjustable Gastric Banding, RYGB: Roux-en-Y Gastric Bypass, VBG: Vertical Banded Gastroplasty, BPD-DS: Bilio-Pancreatic Diversion-Duodenal Switch, BPD: Bilio-Pancreatic Diversion, ESS: Epworth Sleepiness Score, HG: Horizontal Gastroplasty, NS: Not Specified
Introduction
Obstructive sleep apnoea/hypopnoea syndrome (OSAHS) is a growing concern among the health authorities as its economic, social and health implications are immense. OSAHS is a condition of hypoventilation or obstructive ventilation during sleep causing interruption of sleep to restore breathing. Hence the resultant poor sleep quality eventually gives rise to symptoms like impaired alertness, cognitive impairment, excessive daytime sleepiness, mood and personality changes, loud snoring, choking or gasping during sleep, morning headaches and insomnia [1-3]. These symptoms arising from lack of sleep, if left untreated, have serious consequences causing compromise of quality of life, reduced working capacity, sexual health problems and predispose to medical problems like coronary heart diseases, insulin intolerance and hypertension [4-9].
Risk factors of OSAHS include increased age, male gender, family history, diabetes, smoking, alcohol consumption and sedative drugs but the most important of all is obesity [5]. The dramatic increase in the worldwide prevalence of obesity has paralleled the increase in the prevalence of obstructive sleep apnoea [10]. Studies have shown a strong association between increased body mass index (BMI) and the risk of OSAHS [11]. Significant OSAHS is present in 40% of obese individuals and 70% of OSAHS patients are obese [12]. A mere 10% increase in BMI has been shown to increase the individuals risk of developing OSAHS by 500% and weight loss in OSAHS patients significantly decreases apnoea frequency [13].
Conservative management of OSAHS includes lifestyle changes such as losing weight, smoking cessation and limiting alcohol consumption [2,5]. Moderate to severe cases can be treated by using continuous positive airway pressure (CPAP) or intra-oral devices (IODs) and various surgical options are also available [5]. Continuous positive airway pressure (CPAP) is an effective therapy for OSAHS, but compliance to this treatment is low [14]. Bariatric surgery results in sustained weight loss, a decrease of BMI by 45% can occur in the first 12 months, it is therefore is a competitive surgical option for improvement and resolution of moderate to severe sleep apnoea patients [15-18]. In this study we present our experience of impact of bariatric surgery on OSAHS along with a literature review of the impact of bariatric surgery on OSAHS.
Methods
The hospital criteria for referral to bariatric surgery service was; BMI > 35 with NIDDM and/or OSAHS. At the first clinic visit a complete history; initial weight, BMI, height, neck circumference, waist, blood pressure and co-morbidities were recorded. The patients were made to complete an Epworth Sleepiness Score form and if the ESS score was > 11 they were referred to the respiratory physician's team for further assessment and polysomnography. Postoperative patients were routinely seen at 3, 6 and 12 month period initially and then yearly.
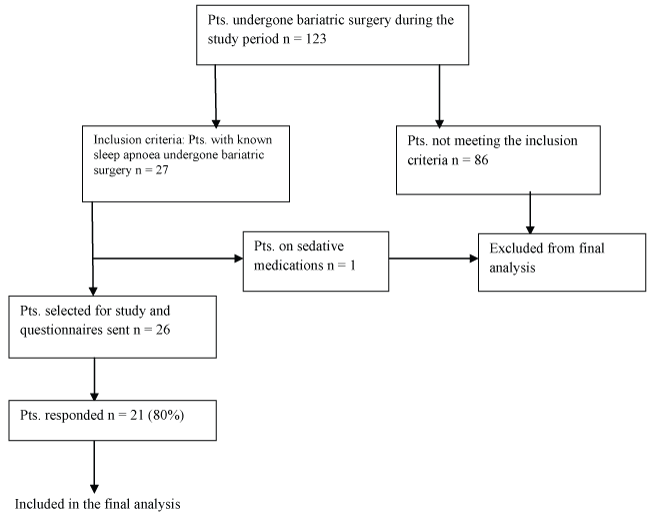
For this study we performed a review of the prospectively maintained data of the patients who underwent bariatric surgery from May 2008 to December 2011. We identified patients who had a documented diagnosis of obstructive sleep apnoea before surgery and included them in the study. Any patients who were on sedative medications were excluded from the study (Figure 1). We recorded the change in ESS, STOP-Bang score, weight and BMI, percentage excess weight loss (EWL) change in co morbidity, CPAP requirement and neck circumference. An ESS score of more than 11 and a STOP-Bang score of more than 3 was considered significant.
Patients were sent two questionnaires by post. Epworth sleepiness scale (ESS) and STOP-Bang questionnaire which are a validated subjective method of assessing sleepiness in a variety of situations [19]. ESS can be used to divide patients in either the normal range (ESS < 11), mild daytime sleepiness (ESS = 11-14), moderate daytime sleepiness (ESS = 15-18) or severe daytime sleepiness (ESS > 18). The STOP-Bang questionnaire is a screening tool for OSAHS, developed and validated to be used for surgical patients [20]. It includes questions about snoring, tiredness, a witnessed episode of stopped breathing during sleep, high blood pressure (HTN), body mass index, age, neck size, and gender.
Patients were given two weeks to respond to the questionnaire and then a reminder was sent to the patients and an additional two weeks given to wait for the response. A high response rate was expected, as patients were regularly followed up as part of continued weight loss programme in the hospital. Primary outcomes of this study were changes in the ESS and STOP-Bang scores of patients and improvement or resolution of sleep apnoea after bariatric surgery. Secondary outcomes were change in BMI and percentage excess weight loss (EWL) at 6 and 12 months after bariatric surgery.
Literature review
EMBASE, MEDLINE and COCHRANE databases were searched for available literature on the subject, from 1988 to 2012, using the words synonymous with obstructive sleep apnoea and bariatric surgery (Sleep apnoea, Hypoventilation syndrome, Hypopnoea and Bariatric surgery, Gastric bypass, Sleeve gastrectomy, Gastric band, LAGB, Weight loss surgery). The databases were searched for all relevant articles written in English language that mentioned impact of bariatric surgery on OSAHS in adult populations (age ≥ 18 yrs). Both laparoscopic and open bariatric procedures were included. All prospective cohort studies, retrospective cohort studies were included. Full articles were retrieved applying the selection criteria to the abstracts and titles. Non English publications, studies on animals, studies on obesity in children, studies without clear outcome on impact of bariatric surgery on OSAHS, studies with only abstracts or conference presentations and literature reviews were excluded from the review. Articles were then read and scanned manually by two reviewers. Any conflicts were resolved at each stage. Initially 73 studies were identified based on the inclusion criteria. After applying the exclusion criteria 20 studies were included in the analysis. This process was carried out by two reviewers and all conflicts were resolved at each stage.
Data collection and statistical analysis
Data was entered on Microsoft Office Excel 2007, statistical analysis was carried out using SPSS software (version 16, SPSS Inc., Chicago, IL, USA). Continuous data was compared using parametric paired student t-test and Wilcoxon signed-rank test was used for non-parametric data. p-values of less than 0.05 were considered statistically significant.
Results
123 bariatric surgery procedures were performed during the period reviewed. All procedures were completed laparoscopically. 27 patients had obstructive sleep apnoea. Out of these18 patients were previously diagnosed to have OSAHS while nine patients with an ESS of more than 11 were referred for a sleep study which confirmed OSAHS. One patient was on sedative medications and was therefore excluded from the study (Figure1). The response rate for the survey was 81% (21/26). The details of these patients are shown in table 1. The follow up period was 8-34 months.
There was a significant drop 61% in the overall ESS of patients undergoing bariatric surgery. The STOP-Bang score decreased similarly from a mean pre-operative value of 5 to 1.76 post-operatively (p < 0.05) (Table 2). OSAHS resolved in 76% of the patients, 8/9 patients stopped using the CPAP machine (Table 2). Mean BMI decreased by 29% (EWL 57.5%) in the first 6 months and 34% (EWL 70%) by 12 months (Table 1).
![]()
Table 1: Details of patients included in the study & weight loss induced by bariatric surgery.
View Table 1
![]()
Table 2: ESS, STOP-Bang scores and clinical conditions of patients, before and after bariatric surgery.
View Table 2
Results of the literature review
20 studies were included in the literature review. 3 studies were based on questionnaires, and 17 were based on sleep study ± a questionnaire. The most commonly used questionnaire was ESS. Total of 828 patients were studied. The follow up period ranged from 4 to 144 months. At 12 months the reported improvement in OSAHS was up to 78% and between 40 to 60% resolution was reported in the long term follow up (84-144 months). One study reported 4% resolution of OSAHS after bariatric surgery.
Discussion
OSAHS is a growing health problem and its prevalence is largely related to the expanding obese population. It has been reported that sleep disordered breathing affects around 9% of middle-aged women and 24% of middle aged men [21]. Mild cases of obstructive sleep apnoea can usually be treated by conservative measures. However moderate to severe conditions are difficult to treat and weight loss is the corner stone for management of OSAHS. Weight loss decreases the intra-abdominal pressure on the diaphragm and the decrease in neck circumference decreases the pressure on the upper airways, hence improving OSAHS. Neck size is an important anthropometric measurement as it is known that patients with OSAHS often have a neck circumference > 17 inches (43 cm) [5]. Weight loss induced by bariatric surgery is sustained for a longer term compared to other non-surgical measures and therefore it is expected that symptoms of sleep apnoea should be controlled over a longer period of time. However there is paucity of published literature on long-term outcome of bariatric surgery on OSAHS.
We performed a literature search on EMBASE, MEDLINE and COCHRANE and identified 20 studies meeting the inclusion criteria (Table 3). Almost all the studies concluded that weight loss induced by bariatric surgery significantly improved OSAHS. The most common method of diagnosing OSAHS was polysomnography and 8 studies used the Epworth sleepiness score (ESS) for screening and follow up. A recent prospective study done in 2010 by Cleophas, et al. [22] involved a patient cohort of 223 which showed a significant decrease in the ESS, by 39%, of patients after bariatric surgery. 46-100% resolution of OSAHS has been reported based on sleep studies before and after bariatric surgery. Improvement in as early as 3 months after surgery has been reported [17] and a study involving a small group of patients showed maintenance resolution for up to 12 years after surgery [18].
![]()
Table 3: Summary of literature review of impact of bariatric surgery on Obstructive Sleep Apnoea (OSA).
View Table 3
Pillar observed in a 7.5 year follow up recurrence of symptoms of OSAHS but could not establish a relation between weight regain and recurrence of symptoms. The lowest reported improvement was 46% in 28 patients after a follow up of 14 months [23]. Interestingly only four studies included more than 50 patients, this only reflects the paucity of data in this area and lays further emphasis on reporting studies on this subject. One prospective study was against the notion that weight loss induced by bariatric surgery resolves OSAHS in the majority of patients [24]; however the study involved 24 patients only. A summary of the literature review is shown in table 3.
An alarming feature of OSAHS is the condition being undiagnosed as daytime sleepiness and declining concentration levels can be attributed to other factors and OSAHS is overlooked. In our experience we observed that nine patients were referred for sleep study on the basis of ESS of more than 11 and were found to have OSAHS. Studies from United States, Europe, Asia, and Australia have shown a high prevalence (80-90%) of un-diagnosed sleep apnoea in adults [25-27]. This gives an account of the problem being undiagnosed widely and as a consequence left untreated.
We conclude from our experience and the literature review that bariatric surgery is a promising option to treat OSAHS. It should be considered in morbidly obese patients alongside other measures. Long term follow up studies are required to further elaborate the impact of bariatric surgery on resolution of OSAHS. We also recommend Epworth Sleepiness Score as a screening tool for assessment of all patients being considered for bariatric surgery. Patients with ESS more than 11 should be referred for sleep study, as it is an effective instrument used to measure average daytime sleepiness. There is a high level of internal consistency between the eight items in the ESS as measured by Cronbach's alpha, ranging from 0.74 to 0.88. Numerous studies using the ESS have supported high validity and reliability.
The authors appreciate that there are a few shortcomings of this study. Firstly a better assessment tool for OSAHS is a sleep study, which should ideally be performed on all patients with sleep apnoea before and after surgery. Secondly, a control group comparing bariatric surgery and non-surgical measures of treating OSAHS would make the results even more reliable. There may also be a selection bias in this cohort of patients as these surgeries were performed at a single centre, where follow up of patients is stringent and some patients failed to return the questionnaire, this may have influenced the questionnaire-based results. The small cohort of patients in this study is comparable other studies in the literature review, however now that bariatric surgery is increasingly being performed and its awareness as a feasible option to treat OSAHS is increasing, there is a potential for future studies.
Conflict of Interest
Mr. Muhammad Ali Karim and co-authors have no conflict of interest.
Source of Funding
None to declare.
References
-
(2010) Continuous Positive Airway Pressure for the treatment of Obstructive Sleep Apnoea/Hypopnoea Syndrome. National Institute for Clinical Excellence (NICE).
-
Lee W, Nagubadi S, Kryger MH, Mokhlesi B (2008) Epidemiology of Obstructive Sleep Apnea: a Population-based Perspective. Expert Rev Respir Med 2: 349-364.
-
Tsara V, Amfilochiou A, Papagrigorakis MJ, Georgopoulos D, Liolios E, et al. (2009) Guidelines for diagnosis and treatment of sleep-related breathing disorders in adults and children definition and classification of sleep related breathing disorders in adults. Different types and indications for sleep studies (Part 1). Hippokratia 13: 187-91.
-
(2006) Fact sheet on Sleep apnoea-Lung and Asthma Information Agency (LAIA).
-
(2003) Management of Obstructive Sleep Apnoea/ Hypopnoea Syndrome in Adults. Scottish Intercollegiate Guidelines Network (SIGN).
-
Yang EH, Hla KM, McHorney CA, Havighurst T, Badr MS, et al. (2000) Sleep apnea and quality of life. Sleep 23: 535-541.
-
Motta J, Guilleminault C, Schroeder JS, Dement WC (1978) Tracheostomy and hemodynamic changes in sleep-inducing apnea. Ann Intern Med 89: 454-458.
-
Davies CW, Crosby JH, Mullins RL, Barbour C, Davies RJ, et al. (2000) Case-control study of 24 hour ambulatory blood pressure in patients with obstructive sleep apnoea and normal matched control subjects. Thorax 55: 736-740.
-
Young T, Skatrud J, Peppard PE (2004) Risk factors for obstructive sleep apnea in adults. JAMA 291: 2013-2016.
-
Yu JC, Berger P (2011) Sleep apnea and obesity. S D Med 28-34.
-
Young T, Peppard PE, Taheri S (2005) Excess weight and sleep-disordered breathing. J Appl Physiol (1985) 99: 1592-1599.
-
Vgontzas AN, Tan TL, Bixler EO, Martin LF, Shubert D, et al. (1994) Sleep apnea and sleep disruption in obese patients. Arch Intern Med 154: 1705-1711.
-
Peppard PE, Young T, Palta M, Dempsey J, Skatrud J (2000) Longitudinal study of moderate weight change and sleep-disordered breathing. JAMA 284: 3015-3021.
-
Weaver TE, Grunstein RR (2008) Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc 5: 173-178.
-
Summers CL, Stradling JR, Baddeley RM (1990) Treatment of sleep apnoea by vertical gastroplasty. Br J Surg 77: 1271-1272.
-
Guardiano SA, Scott JA, Ware JC, Schechner SA (2003) The long-term results of gastric bypass on indexes of sleep apnea. Chest 124: 1615-1619.
-
Rasheid S, Banasiak M, Gallagher SF, Lipska A, Kaba S, et al. (2003) Gastric bypass is an effective treatment for obstructive sleep apnea in patients with clinically significant obesity. Obes Surg 13: 58-61.
-
Scheuller M, Weider D (2001) Bariatric surgery for treatment of sleep apnea syndrome in 15 morbidly obese patients: Long-term results. Otolaryngol Head Neck Surg 125: 299-302.
-
Johns MW (1992) Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep 15: 376-381.
-
Chung F, Yegneswaran B, Liao P, Chung SA, Vairavanathan S, et al. (2008) STOP questionnaire: a tool to screen patients for obstructive sleep apnea. Anesthesiology 108: 812-821.
-
Young T, Palta M, Dempsey J, Skatrud J, Weber S, et al. (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328: 1230-1235.
-
Jon-Erik Cleophas Holty, Neeta Parimi, Michael Ballesteros Blackwell T, Cirangle PT, et al. (2011) Does surgically induced weight loss improve daytime sleepiness? Obes Surg 21: 1535-1545.
-
Valencia-Flores M, Orea A, Herrera M, Santiago V, Rebollar V, et al. (2004) Effect of bariatric surgery on obstructive sleep apnea and hypopnea syndrome, electrocardiogram, and pulmonary arterial pressure. Obes Surg 14: 755-762.
-
Lettieri CJ, Eliasson AH, Greenburg DL (2008) Persistence of obstructive sleep apnea after surgical weight loss. J Clin Sleep Med 4: 333-338.
-
Young T, Peppard PE, Gottlieb DJ (2002) Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med 165: 1217-1239.
-
Young T, Evans L, Finn L, Palta M (1997) Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep 20: 705-706.
-
Lee W, Nagubadi S, Kryger MH, Mokhlesi B (2008) Epidemiology of Obstructive Sleep Apnea: a Population-based Perspective. Expert Rev Respir Med 2: 349-364.
-
Rao A, Tey BH, Ramalingam G, Poh AG (2009) Obstructive Sleep apnoea (OSA) patterns in bariatric surgical practice and response of OSA to weight loss after laparoscopic adjustable gastric banding (LAGB). Ann Acad Med Singapore 38: 587-597.
-
Charuzi I, Lavie P, Peiser J, Peled R (1992) Bariatric surgery in morbidly obese sleep-apnea patients: short- and long-term follow-up. Am J Clin Nutr 55: 594S-596S.
-
Poitou C, Coupaye M, Laaban JP, Coussieu C, Bedel JF, et al. (2006) Serum amyloid A and obstructive sleep apnea syndrome before and after surgically-induced weight loss in morbidly obese subjects. Obes Surg 16: 1475-1481.
-
Cleator IG, Birmingham CL, Kovacevic S, Cleator MM, Gritzner S (2006) Long-term effect of ileogastrostomy surgery for morbid obesity on diabetes mellitus and sleep apnea. Obes Surg 16: 1337-1341.
-
Dixon JB, Schachter LM, O'Brien PE (2005) Polysomnography before and after weight loss in obese patients with severe sleep apnea. Int J Obes (Lond) 29: 1048-1054.
-
Pillar G, Peled R, Lavie P (1994) Recurrence of Sleep Apnea Without Concomitant Weight Increase 7.5 Years After Weight Reduction Surgery. Chest 106: 1702-1704.
-
Haines KL, Nelson LG, Gonzalez R, Torrella T, Martin T, et al. (2007) Objective evidence that bariatric surgery improves obesity-related obstructive sleep apnea. Surgery 141: 354-358.
-
Kalra M, Mannaa M, Fitz K, Kumar S, Chakraborty R, et al. (2008) Effect of surgical weight loss on sleep architecture in adolescents with severe obesity. Obes Surg 18: 675-679.
-
Lankford DA, Proctor CD, Richard R (2005) Continuous Positive Airway Pressure (CPAP) Changes in Bariatric Surgery Patients Undergoing Rapid Weight Loss. Obes Surg 15: 336-341.
-
Fritscher LG, Canani S, Mottin CC, Fritscher CC, Berleze D (2007) Bariatric Surgery in the Treatment of Obstructive Sleep Apnea in Morbidly Obese Patients. Respiration 74: 647-652.
-
Martí-Valeri C, Sabaté A, Masdevall C, Dalmau A (2007) Improvement of Associated Respiratory Problems in Morbidly Obese Patients after Open Roux-en-Y Gastric Bypass. Obes Surg 17: 1102-1110.
-
Simard B, Turcotte H, Marceau P, Biron S, Hould FS, et al. (2004) Asthma and Sleep Apnea in Patients with Morbid Obesity: Outcome after Bariatric Surgery. Obes Surg 14: 1381-1388.
-
Sugerman HJ, Fairman RP, Sood RK, Engle K, Wolfe L, et al. (1992) Long-term effects of gastric surgery for treating respiratory insufficiency of obesity. Am J Clin Nutr 55: 597S-601S.
-
Varela JE, Hinojosa MW, Nguyen NT (2007) Resolution of Obstructive Sleep Apnea after Laparoscopic Gastric Bypass. Obes Surg 17: 1279-1282.