International Journal of Respiratory and Pulmonary Medicine
Role of Tissue Doppler, Strain and 3D Echocardiographic Parameters in Pulmonary Hypertension
Marta Afonso Nogueira1*, LuIsa Moura Branco1, Ana Agapito1, Ana Galrinho1, Alexandra Borba2, Ruben Ramos1, Duarte Cacela1 and Rui Cruz Ferreira1
1Department of Cardiology, Santa Marta's Hospital, Portugal
2Department of Pulmonology, Santa Marta's Hospital, Portugal
*Corresponding author: Marta Afonso Nogueira, MD, Serviço de Cardiologia, Hospital de Santa Marta, Rua de Santa Marta, 1169-024, Lisboa, Portugal, E-mail: marta.afonso.nogueira@gmail.com
Int J Respir Pulm Med, IJRPM-3-053, (Volume 3, Issue 3), Original Article; ISSN: 2378-3516
Received: May 20, 2016 | Accepted: August 20, 2016 | Published: August 23, 2016
Citation: Nogueira MA, Branco LM, Agapito A, Galrinho A, Borba A, et al. (2016) Role of Tissue Doppler, Strain and 3D Echocardiographic Parameters in Pulmonary Hypertension. Int J Respir Pulm Med 3:053. 10.23937/2378-3516/1410053
Copyright: © 2016 Nogueira MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction and purpose: Several echocardiographic parameters study right ventricular (RV) function, which has a prognostic impact on pulmonary hypertension (PH). Our goal was to evaluate the correlation between known prognostic markers and standard, as well as advanced echocardiographic parameters, including Tissue Doppler (TDI), strain imaging and three-dimensional (3D) echocardiography.
Methods: 51 patients (pts) with PH were prospectively studied and the following variables (among others) were analysed: Right Atrial Area/Volume and Global Longitudinal Strain (GLS), Tricuspid Annular Plane Systolic Excursion (TAPSE), RV Fractional Area Change, RV GLS, RV Tei Index, Pulmonary Artery Systolic Pressure (PASP), Pulmonary Acceleration Time (PAcT), Tricuspid s'. In 42 pts, the following 3D variables were calculated: RV end-systolic (ES), end-diastolic (ED) volumes (V) and ejection fraction (EF). Data regarding clinical/demographic characteristics, six-minute walk test (6MWT) and brain natriuretic peptide (BNP) were also collected.
Results: There was a statistically significant (p < 0.05) correlation between 6 MWT and RV Tei Index (r = -0.336), PASP (r = -0.388), PAcT (r = 0.661), RVESV (r = -0.380), RVEF (r = 0.381), as well as between BNP and TAPSE (r = -0.332), Tricuspid s' (r = -0.29), PAcT (r = -0.31), RV GLS (r = 0.385), RVESV (r = 0.405), RVEDV (r = 0.445).
Conclusions: In this population with PH, conventional echocardiographic parameters, which have several limitations, but also advanced parameters, particularly RV GLS and EDV/EF obtained by 3D echocardiography, demonstrated an important correlation with prognostic markers well studied, reinforcing the need for a more comprehensive study of RV function.
Keywords
Pulmonary hypertension, Two-dimensional echocardiography, Three-dimensional echocardiography, Longitudinal strain, Right ventricle
Introduction
Pulmonary hypertension (PH) is defined by an increase in mean pulmonary artery pressure (PAP) to a value superior or equal to 25 mm Hg at rest, as determined by right heart catheterization [1].
Although the degree of pulmonary hypertension characterizes this entity, it does not correlate with symptoms or survival [1]. On the other hand, right ventricular (RV) function is a major determinant of clinical presentation and prognosis in pulmonary hypertension [2,3].
Echocardiography is a key screening tool in the complex diagnostic algorithm of PH, providing an estimate of PAP, evaluating the remodeling and function of the RV and being also useful in ruling out secondary causes of PH [4]. Additionally, echocardiography is valuable in evaluating prognosis, treatment options and monitoring the efficacy of specific therapy [5].
Nonetheless, echocardiography is also more affordable for serial testing and more universally available than other cardiac imaging tests such as cardiac magnetic resonance imaging (MRI) [5].
Nowadays, there are several echocardiographic parameters that evaluate mainly the right ventricular function, from traditional parameters such as right ventricular Tei Index, to more recent parameters, including RV Global Longitudinal Strain, using speckle-tracking imaging or three-dimensional (3D) echocardiography [6-10]. In fact, 3D echocardiography is able to display the complex anatomy of the RV, simultaneously depicting both longitudinal and transverse movements, rendering it superior to conventional two-dimensional (2D) methods in RV function assessment [9,10].
Actually, many echocardiographic laboratories are currently using the conventional measures along with the newer methods for a more comprehensive RV echocardiographic analysis [5]. Therefore, although most of them are not included in the routine echocardiographic evaluation of PH patients, it is important to use different parameters in order to correctly study, non-invasively, RV physiology and its prognostic value.
Methods
In this study, 51 patients with the diagnosis of PH, by right heart catheterization, consecutively observed in either a PH or Congenital Heart Disease Consultation, were prospectively submitted to a transthoracic echocardiogram (TTE), from August 2013 to April 2015.
All echocardiographic studies were obtained from the same operator, using the same echocardiography machine (GE Vivid E9) and workstation (EchoPAC PC Software, version 112).
According to the recommendations of the American Society of Echocardiography and European Association of Cardiovascular Imaging [11], the echocardiographic variables analysed were: Absolute and Indexed Right Atrial (RA) Area and Volume, RA Global Longitudinal Strain (GLS), Tricuspid Annular Plane Systolic Excursion (TAPSE), Right Ventricular Fractional Area Change (RVFAC), RV GLS, RV Tei Index (Index of Myocardial Performance), RV Tei Index by Tissue Doppler Imaging (TDI), Tricuspid e', s' and E/e', Pulmonary Artery Systolic Pressure (PASP), Pulmonary Acceleration Time (PAcT), Aortic Velocity Time Integral (VTI), Cardiac Output (CO), Left Ventricle Eccentricity Index (LVEI) in diastole and systole, Mitral mean e', s' and E/e'.
Regarding GLS, it is important to underline that we have used the same software applied for the study of the left ventricle, as usual.
Nonetheless, we also measured the Peak Isovolumic Myocardial Velocity (IVCv) and the Myocardial Acceleration during Isovolumic Contraction (IVA), which is defined by dividing IVCv by Time to Peak Velocity, using TDI, according to the literature [12,13]. Since IVA is frequency dependent, it was also indexed to the heart rate (divided by √RR [ms]).
Additionally, we calculated the duration of Tricuspid Regurgitation corrected for Heart Rate (TRDc), using the formula: TRDc[ms]/(√RR interval[s]) [14].
The 3D echocardiographic variables - RV end-systolic (ES), end-diastolic (ED) and stroke (SV) volumes (V), as well as RV ejection fraction (EF) - were calculated offline using the software TomTec 4D RV Volume, in 42 patients (in the remaining population it was not possible to obtain due to technical difficulties, mostly related to RV anatomy and suboptimal acoustic window).
Finally, we also collected data regarding demographic characteristics, clinical classification of PH (according to the ESC/ERS Guidelines [15]), clinical status of the patients (New York Heart Association = NYHA functional class), six-minute walk test (6MWT) results and serum levels of brain natriuretic peptide (BNP), in the same period of time of TTE.
Statistical Analysis
The statistical analysis was performed using IBM® SPSS® Statistics, version 21.
Qualitative variables were expressed as absolute frequencies and percentages and quantitative variables were expressed as mean value ± standard deviation. Correlation between data was tested with Pearson's correlation analysis and a p value inferior to 0.05 was accepted as statistically significant.
Results
The majority of patients were female (34 patients = 67%), with a mean age of 54 ± 16 years (range: 26 to 85 years old). Most patients were classified in groups 1 (mainly congenital heart disease and idiopathic) or 4 (Figure 1 and Figure 2) and were in NYHA functional class II or III (Figure 3). The results regarding each echocardiographic parameter are shown in table 1.
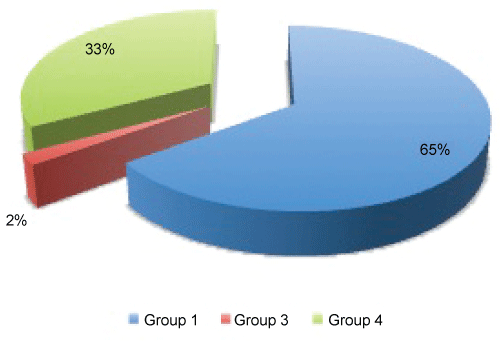
.
Figure 1 Distribution according to clinical classification of pulmonary hypertension. 65% = 33 patients; 33% = 17 patients; 2% = 1 patient.
View Figure 1
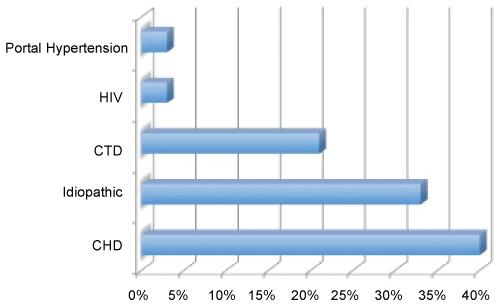
.
Figure 2: Subgroups of patients with pulmonary arterial hypertension (Group 1).
CHD: Congenital Heart Disease; CTD: Connective Tissue Disease; HIV: Human Immunodeficiency Virus Infection
View Figure 2
![]()
Table 1: Results regarding all echocardiographic parameters analysed.
View Table 1
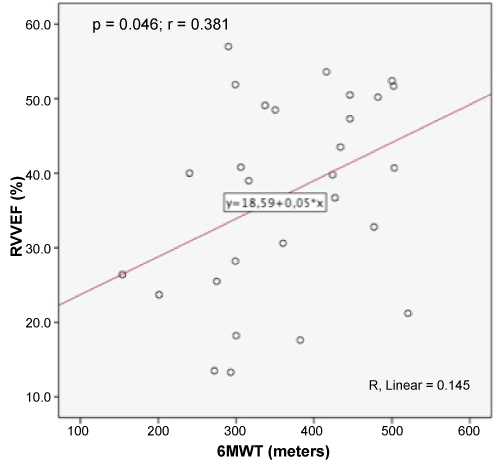
In this population, there was a statistically significant correlation between 6MWT and the following variables: RV Tei Index, with p = 0.048 and r = -0.336 (Figure 4); PASP, with p = 0.021 and r = -0.388; PAcT, with p = 0.0001 and r = 0.661; RVESV, with p = 0.046 and r = -0.380 and RVEF (Figure 5 and Video 1), with p = 0.046 and r = 0.381.
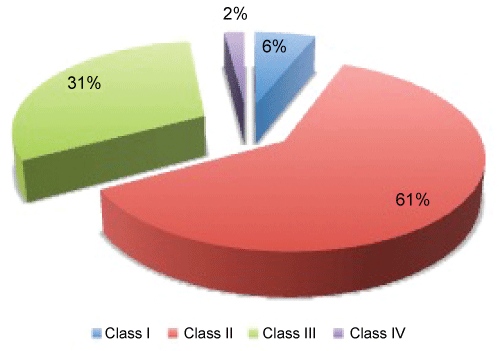
.
Figure 3: Distribution according to functional class of the New York Heart Association (NYHA).
View Figure 3
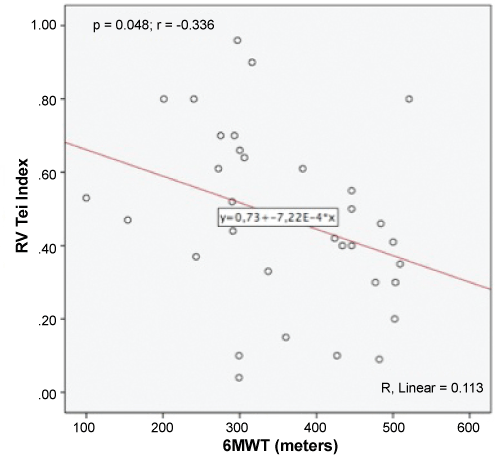
.
Figure 4: Correlation between 6MWT (Six-Minute Walk Test) and RV (Right Ventricular) Tei Index.
View Figure 4
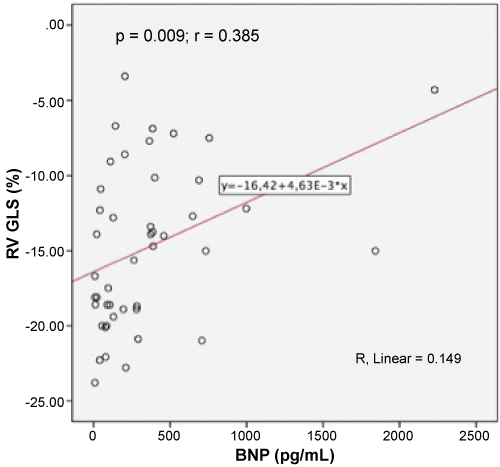
There was also a statistically significant correlation between BNP levels and the following variables: TAPSE, with p = 0.022 and r = -0.332; RV GLS (Figure 6 and Video 2), with p = 0.009 and r = 0.385; Tricuspid s', with p = 0.046 and r = -0.29; PAcT, with p = 0.043 and r = -0.31; RVESV (Video 1), with p = 0.011 and r = 0.405 and RVEDV (Video 1), with p = 0.005 and r = 0.445.
.
Figure 5: Correlation between 6MWT (Six-Minute Walk Test) and RVEF (Right Ventricular Ejection Fraction).
View Figure 5
.
Figure 6: Correlation between BNP (Brain Natriuretic Peptide) and RV GLS (Right Ventricular Global Longitudinal Strain).
View Figure 6
Discussion
This study involved a prospective analysis of several echocardiographic parameters in a heterogeneous population of patients with PH, mainly from groups 1 and 4.
Recently, the ESC/ERS Guidelines have been updated considering only the right atrial area and the presence of pericardial effusion as the two main echocardiographic prognostic markers in patients with pulmonary arterial hypertension (group 1) [15].
Nonetheless, to evaluate in a more comprehensive way the right ventricular function, it is important to consider many other echocardiographic parameters. Considering the conventional parameters with a statistically significant correlation with two well studied prognostic markers (6MWT and BNP), namely RV Tei Index, PAcT, PASP, TAPSE, they correspond to well-known and easily performed parameters. However, there are limitations in their use: conventional velocity and displacement based analyses can be affected by translational motion of the heart and respiratory variation [6].
In fact, there is a relatively weak performance of older 2-dimensional (2D) echocardiographic indices of RV performance including fractional area change and tricuspid annular plane systolic excursion in the setting of pulmonary hypertension due mainly to the complex RV shape and the thinness of its free wall [8]. Nonetheless, TAPSE correlated with BNP but not with 6MWT, which may be explained by the numerous factors that influence this test, besides RV function, such as respiratory or muscular performance.
Regarding RV GLS, which in this study also had a statistically significant correlation with BNP, it enables quantification of global myocardial function in a simple and angle-independent manner, giving a more direct assessment of RV mechanics [6].
Moreover, RV GLS showed a strong association (stronger than that of other echocardiographic indices) with all-cause mortality, cardiopulmonary mortality and cardiopulmonary events in a study held at the Mayo Clinic in 575 patients (although it was a retrospective study in patients with both known or suspected PH) [16].
Additionally, the fact that GLS correlated with BNP and 3D echocardiographic variables correlated with 6MWT and BNP, whilst RVFAC did not, may indicate that those advanced parameters are more sensitive and potentially constitute early markers of RV dysfunction. Accordingly, although based on a significant correlation with prognostic markers, our study corroborates the potential usefulness of RV GLS and especially 3D echocardiographic variables as add-on tools in the characterization of patients with PH and we believe that these parameters will be used more often in the future, as soon as more studies are published in this setting.
However, it is also important to notice that albeit an isolated change in one echocardiographic variable is not meaningful per se, multiple variable modifications provide more accurate information, with clinical impact. In this regard, the multivariable approach should be the rule, combining different parameters, including the above-mentioned advanced variables. Despite this study having a relatively small population, the data were collected prospectively and included patients from different groups, reflecting the heterogeneity of PH in real world scenario.
Nevertheless, given the dimension of the population analyzed, there will be needed further studies in order to confirm the incremental value of the more recent echocardiographic parameters on the prognostic stratification of this clinical entity.
Conclusions
In this cohort of patients with PH, not only conventional echocardiographic parameters such as right ventricular Tei Index, which have several limitations, but also more advanced parameters, particularly right ventricular global longitudinal strain and 3D functional/volumetric assessment, demonstrated an important correlation with prognostic markers well studied (six-minute walk test and serum levels of brain natriuretic peptide), reinforcing the need for a more comprehensive study of right ventricular function, in this clinical entity.
Acknowledgement
The authors would like to thank to all the technicians that work in the echocardiography laboratory for their valuable help.
Ethical Statement
The authors declare that have followed all the international recommendations regarding clinical investigation (Helsinki Declaration of the World Medical Association).
Video 1
Illustrative example of 3d echocardiographic parameters (ESV = End-systolic Volume; EDV = End-diastolic Volume; EF = Ejection Fraction; SV = Stroke Volume). Video 1
Video 2
Illustrative example of right ventricular global longitudinal strain from a patient of this study. Video 2
References
-
Moceri P, Baudouy D, Chiche O, Cerboni P, Bouvier P, et al. (2014) Imaging in pulmonary hypertension: Focus on the role of echocardiography. Arch Cardiovasc Dis 107: 261-271.
-
Naeije R (2015) Assessment of right ventricular function in pulmonary hypertension. Curr Hypertens Rep 17: 35.
-
Knight DS, Schwaiger JP, Krupickova S, Davar J, Muthurangu V, et al. (2015) Accuracy and Test-Retest Reproducibility of Two-Dimensional Knowledge-Based Volumetric Reconstruction of the Right Ventricle in Pulmonary Hypertension. J Am Soc Echocardiogr 28: 989-998.
-
D'Alto M, Romeo E, Argiento P, Di Salvo G, Badagliacca R, et al. (2015) Pulmonary arterial hypertension: the key role of echocardiography. Echocardiography 32: S23-37.
-
Harrison A, Hatton N, Ryan J (2015) The right ventricle under pressure: evaluating the adaptive and maladaptive changes in the right ventricle in pulmonary arterial hypertension using echocardiography (2013 Grover Conference series). Pulm Circ 5: 29-47.
-
Park JH, Park MM, Farha S, Sharp J, Lundgrin E, et al. (2015) Impaired Global Right Ventricular Longitudinal Strain Predicts Long-Term Adverse Outcomes in Patients with Pulmonary Arterial Hypertension. J Cardiovasc Ultrasound 23: 91-99.
-
Ikeda S, Tsuneto A, Kojima S, Koga S, Nakata T, et al. (2014) Longitudinal strain of right ventricular free wall by 2-dimensional speckle-tracking echocardiography is useful for detecting pulmonary hypertension Life Sci 111: 12-17.
-
Reichek N (2013) Right ventricular strain in pulmonary hypertension: flavor du jour or enduring prognostic index? Circ Cardiovasc Imaging 6: 609-611.
-
Li Y, Wang Y, Zhai Z, Guo X, Yang Y, et al. (2015) Real-Time Three-Dimensional Echocardiography to Assess Right Ventricle Function in Patients with Pulmonary Hypertension. PLoS One 10: e0129557.
-
Knight D, Grasso AE, Quail, MA, Muthurangu V, Taylor AM, et al. (2015) Accuracy and Reproducibility of Right Ventricular Quantification in Patients with Pressure and Volume Overload Using Single-Beat Three-Dimensional Echocardiography. J Am Soc Echocardiogr 28: 363-374.
-
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, et al. (2015) Recommendations for cardiacchamberquantification by echocardiography in adults: an update from the AmericanSociety of Echocardiography and the EuropeanAssociation of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 16: 233-270.
-
Schattke S, Knebel F, Grohmann A, Dreger H, Kmezik F, et al. (2010) Early right ventricular systolic dysfunction in patients with systemic sclerosis without pulmonary hypertension: a Doppler Tissue and Speckle Tracking echocardiography study. Cardiovasc Ultrasound 8: 3.
-
Ernande L, Cottin V, Leroux PY, Girerd N, Huez S, et al. (2013) Right isovolumic contraction velocity predicts survival in pulmonary hypertension. J Am Soc Echocardiogr 26: 297-306.
-
Cho IJ, Oh J, Chang HJ, Park J, Kang KW, et al. (2014) Tricuspid regurgitation duration correlates with cardiovascular magnetic resonance-derived right ventricular ejection fraction and predict prognosis in patients with pulmonary arterial hypertension. Eur Heart J Cardiovasc Imaging 15: 18-23.
-
Galiè N, Humbert M, Vachiery JL, Gibbs S, Lang I, et al. (2015) 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension. Eurheartj.
-
Fine NM, Chen L, Bastiansen PM, Frantz RP, Pellikka PA, et al. (2013) Outcome prediction by quantitative right ventricular function assessment in 575 subjects evaluated for pulmonary hypertension. CircCardiovasc Imaging 6: 711-721.





