International Journal of Respiratory and Pulmonary Medicine
An Unusual Case of Recurrent Post-Obstructive Pneumonia from Spontaneous Granulation Tissue Formation
Georges Al-Helou1*, Sripooja Satya2, Brian Senisi2, Robert Maximos3 and Jalil Ahari1
1Pulmonary and Critical Care Division, George Washington University, USA
2Internal Medicine Department, George Washington University, USA
3Pulmonary and Critical Care Division, Veterans' Affairs Medical Center, USA
*Corresponding author: Georges Al-Helou, MD, Pulmonary and Critical Care Division, George Washington University Hospital, 2150 Pennsylvania Ave NW, 8th floor, Washington DC, 20037, USA, Tel: 202-741-2180, Fax: 202-741-2238, E-mail: gre05@email.gwu.edu
Int J Respir Pulm Med, IJRPM-3-050, (Volume 3, Issue 3), Case Report; ISSN: 2378-3516
Received: April 26, 2016 | Accepted: July 08, 2016 | Published: July 11, 2016
Citation: Al-Helou G, Satya S, Senisi B, Maximos R, Ahari J (2016) An Unusual Case of Recurrent Post-Obstructive Pneumonia from Spontaneous Granulation Tissue Formation. Int J Respir Pulm Med 3:050. 10.23937/2378-3516/1410050
Copyright: © 2016 Al-Helou G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Case: A 63-year-old man known to have human immune-deficiency viral (HIV) infection was referred for evaluation following three episodes of left upper lobe pneumonia. He was well controlled on his anti-retroviral medications. Physical exam showed left upper lobe wheezing. No evidence of obstruction could be seen on chest X-ray or computed tomography (CT). Bronchoscopy was done and showed an obstructing lesion that was biopsied then ablated. It was found to be due to a spontaneous formation of granulation tissue with no identifiable cause.
Keywords
Pneumonia, Bronchial obstruction, Human immuno-deficiency virus, Community acquired pneumonia, Spontaneous granulation tissue formation
Discussion
Post-obstructive pneumonia is usually secondary to a blocked, or partially blocked, airway that prevents the mucous clearance and promotes bacterial growth. Granulation tissue formation is commonly seen in post-operative patients or patients that have repetitive trauma from foreign material like retained suture material. However, our patient did not have any of the above mentioned causes and his lesion was deemed to have developed spontaneously. No such cases have been previously published to the best of our knowledge.
A 63-year-old Caucasian male presented to our emergency department with fever, chills, shortness of breath and a cough productive of thick sputum. He is known to have HIV which was diagnosed twenty years ago. He is on anti-retroviral therapy with a recent CD 4 cell count of 530 cells per cubic millimeter. He also has hypothyroidism and well controlled asthma. Over the previous five months, he was hospitalized three times for recurrent bouts of pneumonia and treated with antibiotics.
Further questioning revealed that he had intermittent night sweats along with a ten pound weight loss. He had recently traveled to Western Europe. His home medications included budesonide inhaler, levothyroxine, pantoprazole, and the combination medication Triumeq (abacavir/dolutegravir/lamivudine) for HIV. He lives with his partner, works as a lawyer, consumes 2 alcoholic drinks per day, never smoked, and has no illicit drug use.
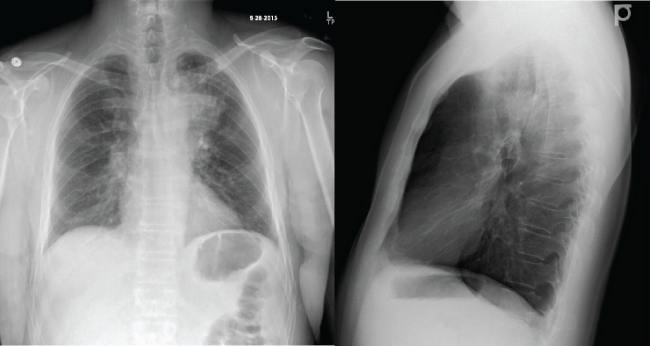
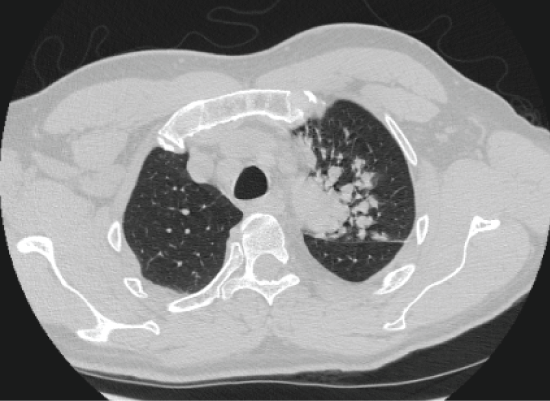
On admission, physical exam revealed tachypnea of 22 breaths per minute and tachycardia of 116 beats per minute. However, patient was afebrile, blood pressure was within normal limits and oxygen saturation was 92%. On auscultation, he had left upper lobe wheezing, he was tachycardic but no murmur was audible. The rest of his physical exam was not remarkable for any abnormality. Chest X-ray (CXR) showed a left upper lobe infiltrate similar to previous admissions (Figure 1). Computed topographic (CT) imaging of the chest revealed enlarged mediastinal and hilar lymph nodes and increased tree-in-bud opacities in left upper lobe with no evidence of an obstructing endo-bronchial lesion (Figure 2). Outpatient records revealed a quantiferon gold that was negative and 3 negative AFB sputum samples.
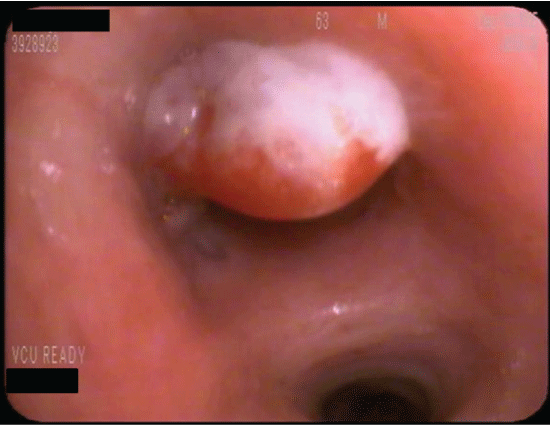
Due to his recurrent pneumonias, he was referred for bronchoscopy to further evaluate the presence of an airway obstruction as the cause of his recurrent illnesses. The bronchoscopy revealed an endobronchial pedunculated lesion obstructing the left upper lobe bronchus. This was biopsied and ablated via Nd: Yap laser (Figure 3). Careful inspection of the airway and the lesion showed no evidence of foreign body. After the bronchoscopy, he developed worsening cough, shortness of breath, and wheezing. His symptoms improved significantly with nebulizer treatment and were thought to be due to bronchial irritation from the ablation.
.
Figure 3: Bronchoscopic view of the obstructing lesion in the left upper lobe bronchus. The lesion was removed via laser therapy.
View Figure 3
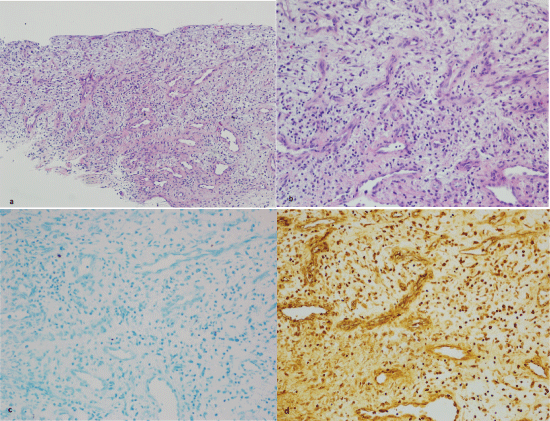
Bronchio-alveolar lavage was negative for acid fast bacilli, P. jirovecii, and other organisms by gram stain. Culture grew normal respiratory flora. Blood cultures were without growth, urine Streptococcus pneumoniae and legionella antigens were also negative. Specimen were sent for pathology. Hematoxylin and eosin (H&E) showed minimal inflammation and granulation tissue formation, no granulomas seen (Figure 4a and Figure 4b). Acid fast staining was negative for mycobacterium (Figure 4c). Wharthin-Starry stain was negative for spirochetes (Figure 4d) which made bacillary angiomatosis less likely.
.
Figure 4: a,b) Pathology showed: minimal inflammation and evidence of granulation tissue formation on H&E;
c) No mycobacteria seen on AFB; d) No evidence of organisms on Wharthin-Starry stain.
View Figure 4
He was discharged home to finish a course of oral moxifloxacin for his pneumonia. Follow up pulmonary function tests (PFT) showed normal flows, volumes and slightly decreased diffusing capacity. A repeat CXR two months later showed resolution of the left upper lobe opacities.
This patient had a post-obstructive pneumonia from the obstructing granulation tissue formation. Post-obstructive pneumonia is usually secondary to a blocked airway that prevents the mucous clearance and promotes bacterial growth [1]. Infection is usually slow to resolve and recurrent bouts of pneumonia can occur. There are multiple causes for post-obstructive pneumonia with cancer being the most common [2]. No cause was found that explained the formation of the granulation tissue and we think it formed spontaneously. No other cases have been described before.
Bacillary angiomatosis was considered in our differential, but given the absence of organisms on pathology and the resolution of symptoms with no recurrence after excision, the likelihood of the disease was thought to be low. Bacillary angiomatosis is caused by Bartonella quintana and B. henselae which stimulate endothelial cell proliferation and migration resulting in neo-vascular proliferation [3]. This was unlikely in our patient as no organisms were seen and no recurrence occurred after ablation.
The airway epithelium is a continuous cell layer that acts as both a host defense and an environmental barrier. As such, any injury to the airway requires a rapid and reliable healing process [4]. Wound healing is divided into four steps: coagulation and hemostasis, inflammation, proliferation and tissue remodeling [5]. Following an injury, the sub endothelial matrix is exposed leading to an inflammatory reaction followed by a proliferative phase of fibroblast migration. A prolonged inflammatory response in the airway can lead to granulation tissue formation [6]. Even though the exact pathway is still not completely understood, several cytokines have been involved in this prolonged inflammatory response as well as the aberrant tissue healing. These include: Transforming Growth Factor-Beta, Interleukin-1 and Prostaglandin E2 [7]. It is thought that human bronchial epithelial cells help modulate and increase the contraction of fibroblasts and play an important role in normal wound healing [8].
Local trauma or irritation due to surgical or iatrogenic interventions has long been known to trigger the formation of granulation tissue as a result of abnormal wound healing [9]. Foreign bodies including remnants of prior surgeries, such as suture materials, have also been associated with recurrence of granulation. This can present in the immediate post-operative period or years following insult [10]. This is thought to be due to the prolonged irritating effect of the foreign material that is not cleared by the body. In our case, no foreign body was found as a cause of the granulation tissue formation.
In summary, this is a case of a patient with well controlled HIV and asthma with spontaneous formation of granulation tissue and no evident cause. This caused bronchial obstruction with subsequent recurrent post-obstructive pneumonia. The case presented here, to the knowledge of the writers, is the first case of spontaneous formation of localized granulation tissue that has led to endobronchial obstruction.
References
-
Burke M, Fraser R (1988) Obstructive pneumonitis: a pathologic and pathogenetic reappraisal. Radiology 166: 699-704.
-
Mehta RM, Cutaia M (2006) The role of interventional pulmonary procedures in the management of post-obstructive pneumonia. Curr Infect Dis Rep 8: 207-214.
-
Wormser GP (2007) Discovery of new infectious diseases - bartonella species. N Engl J Med 356: 2346-2347.
-
Gill SE, Parks WC (2008) Metalloproteinases and their inhibitors: regulators of wound healing. Int J Biochem Cell Biol 40: 1334-1347.
-
Velnar T, Bailey T, Smrkolj V (2009) The wound healing process: an overview of the cellular and molecular mechanisms. J Int Med Res 37: 1528-1542.
-
Ghosh A, Malaisrie N, Leahy KP, Singhal S, Einhorn E, et al. (2011) Cellular adaptive inflammation mediates airway granulation in a murine model of subglottic stenosis. Otolaryngol Head Neck Surg 144: 927-933.
-
Coker RK, Laurent GJ, Shahzeidi S, Lympany PA, du Bois RM, et al. (1997) Transforming growth factors-beta 1,-beta 2, and-beta 3 stimulate fibroblast procollagen production in vitro but are differentially expressed during bleomycin-induced lung fibrosis. Am J Pathol 150: 981-991.
-
Mio T, Liu XD, Adachi Y, Striz I, Sköld CM, et al. (1998) Human bronchial epithelial cells modulate collagen gel contraction by fibroblasts. Am J Physiol 274: L119-126.
-
Bolognia JL, Jorizzo JL, Schaffer JV (2012) Bolognia Textbook of Dermatology 2313-2325.
-
Watanabe Y, Sasada S, Izumo T, Nakamura Y, Chavez C, et al. (2014) Intractable Obstructive Endobronchial Granulation Caused by Surgical Materials After Sleeve Resection for Tracheal Carcinoma. Ann Thorac Surg 98: 2200-2202.