International Journal of Respiratory and Pulmonary Medicine
Left Hemi-Diaphragmatic Hydatid Cyst - A Rare Presentation and Diagnostic Challenge
Haris Hakeem1, Ghulam Fareed1, Muhammad Irfan1* and Saulat Fatmi2
1Department of Medicine, Aga Khan University, Pakistan
2Department of Cardiothoracic Surgery, Aga Khan University, Pakistan
*Corresponding author: Dr. Muhammad Irfan, FCPS (Medicine), FCPS (Pulmonology), Associate Professor, Section of Pulmonary and Critical Care Medicine, Department of Medicine, Aga Khan University, Stadium Road Karachi, Pakistan, Tel: + 92 21 34864664, E-mail: muhammad.irfan@aku.edu
Int J Respir Pulm Med, IJRPM-3-046, (Volume 3, Issue 2), Case Report; ISSN: 2378-3516
Received: April 17, 2015 | Accepted: April 19, 2016 | Published: April 22, 2016
Citation: Hakeem H, Fareed G, Irfan M, Fatmi S (2016) Left Hemi-Diaphragmatic Hydatid Cyst - A Rare Presentation and Diagnostic Challenge. Int J Respir Pulm Med 3:046. 10.23937/2378-3516/1410046
Copyright: © 2016 Hakeem H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Echinococcosis or hydatid cyst disease is among the oldest diseases known to man. Common presentations include involvement of liver and lungs. Hydatid cyst in diaphragm without hepatic involvement is rare and less than 100 cases are reported in literature. We are describing a case of a young female who presented with cough anddyspnea secondary to large cysts that appeared to involve the right lung and spleen on initial imaging studies. Peroperatively, however, the presumed spleenic cystwas surprisingly found to be lying within left hemidiaphragm. Complete surgical resection of the cysts was performed with uneventful post-operative recovery.
Keywords
Hydatid cyst, Diaphragm, Echinococcus
Introduction
Hydatid Cyst (HCs) is a zoonosis caused by cestode Echinococcus granulosus and is endemic in many parts of the world. The most common organs that are affected by E. granulosus are liver and lungs (78%) [1]. Diaphragmatic localization is very rare with the incidence of around 1%, and most of these are generally associated with hepatic hydatid cysts [2]. According to Kjosseve all, less than 100 cases of diaphragmatic HCs have been reported in the international literature so far and most of them had concomitant involvement of right hemidiaphragm [1]. Herein, the authors report a case of a young female who presented with cough and dyspnea. Initial imaging studies showed large hydatid cysts involving the right lung and spleen. Peroperatively , however, the presumed spleenic cyst was surprisingly found to be lying within left hemidiaphragm.
Case History
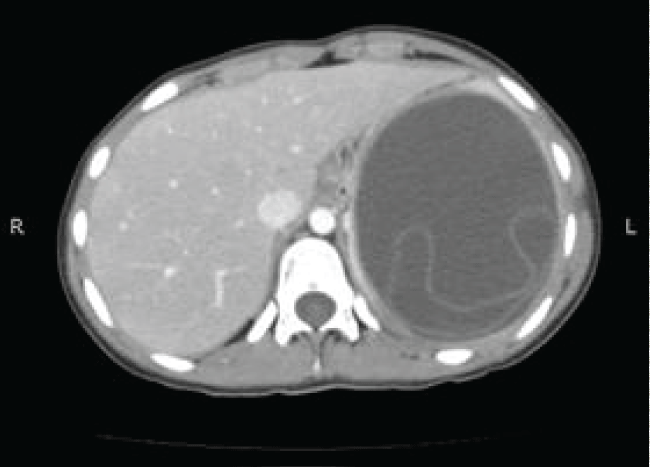
A 16 years old girl presented with cough, dyspnea and pain in left hypochondrium for 15 days. She denied history of fever, weight loss and hemoptysis. Her past and family history was negative for congenital or hereditary diseases. General physical examination was unremarkable. Her respiratory system examination revealed dull percussion note and absent breath sounds in right mid and lower chest. A mass was palpable in the left hypochondrium which was interpreted as splenomegaly. Her ultrasound abdomen revealed large cystic hypo echoic lesions in right lower lung and spleen suggestive of HCs. CT scan was done which showed a well-defined 9.9 × 9 × 10 cm hypodense cyst involving the middle and lower lobes of right lung. It had thick enhancing walls and caused mild pleural effusion with adjacent atelectasis. A similar thick walled 11.2 × 9.9 × 10.5 cm hypodense cyst with enhancing walls and internal floating membranes was also seen, reported to be within spleen (Figure 1 and Figure 2). These cysts were causing displacement of surrounding vessels and adjacent viscera. No evidence of focal lesion was identified in liver parenchyma. Complete blood count, serum creatinine and liver function tests were within normal limits. Serology for echinococcus antibodies was negative. The patient was referred to cardiothoracic surgeon for further management. Thoracotomy was performed and right lower lobe cyst was removed. On the left side, however, presumed splenic cyst was surprisingly found to be lying within the diaphragm. It was successfully excised and the cavity was washed with hypertonic saline. Tissue diagnosis of HCs was confirmed in both specimens (Figure 3). Postoperative recovery was uneventful and the patient was subsequently discharged on Albendazole (10 mg/kg body weight). On her last follow up visit, 2 months after surgery, patient was disease free and doing well.
.
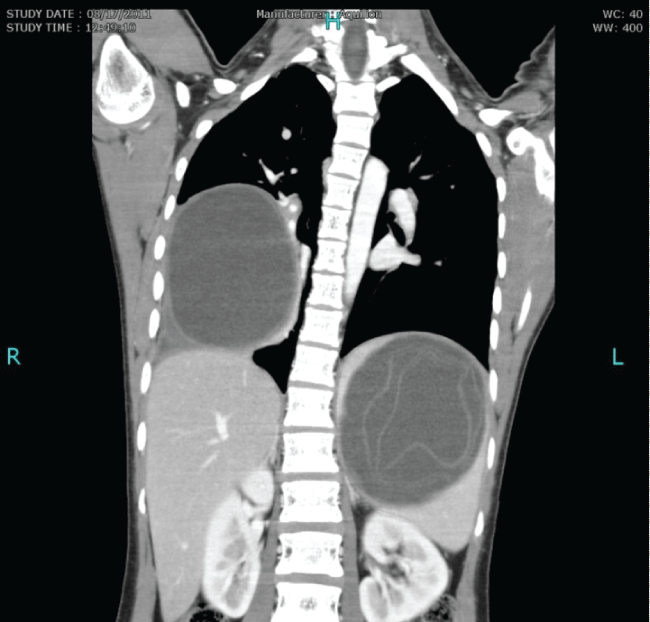
Figure 1: CT scan (coronal view) of bilateral hydatid cysts. One in right lung and the other 'reported' to be within spleen with floating membranes.
View Figure 1
.
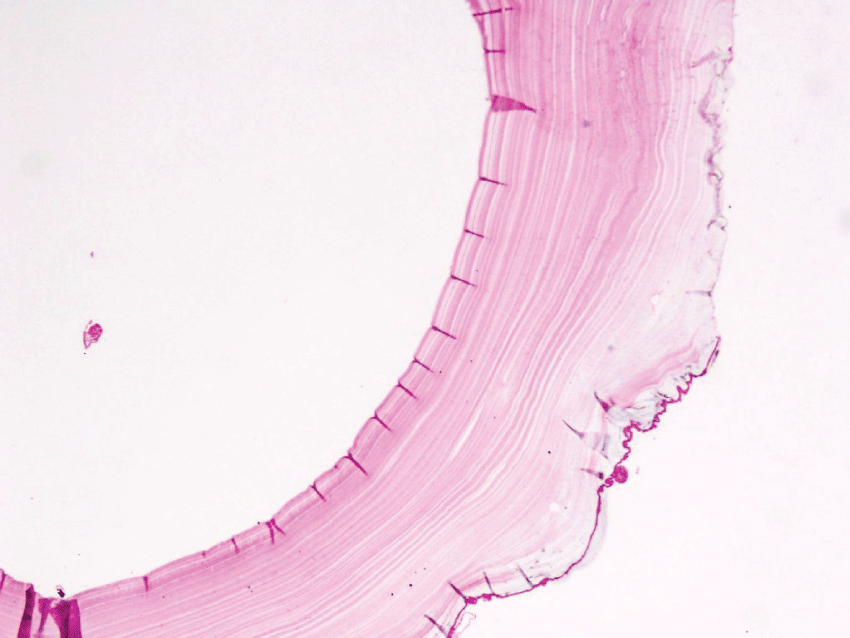
Figure 3: Histopathology section of HC showing thin germinal layer which gives rise to brood capsules.
View Figure 3
Discussion
Hydatidosis is included in the differential diagnosis of space-occupying lesions. Although hydatid disease may affect any organ or soft tissue, the favoured sites of involvement include liver (70-75%) and lungs (20-25%) either alone or concomitantly (18%) followed by peritoneal cavity (10-16%). Less commonly, HCs may involve kidneys (1.5-4%), spleen (3%), brain (3%), musculoskeletal system (0.5-4%), heart (2 %), and retroperitoneum (1%). The HCs of the diaphragm is very rare [1]. In a review of 1,619 patients with thoracic hydatidosis, Jayashankar N et al. present the frequency of the intrapulmonary and extra pulmonary HCs as 94.6% and 5.62% cases respectively [3].
The symptoms of thoracic hydatidosis depend on the size and the site of the lesion. Thus, slowly growing HCs are generally asymptomatic until they are large enough to cause mass effect in an involved organ [3]. As in our case, the common presenting symptoms are cough, chest pain, and breathlessness [3].
More than one pathway has been proposed to explain the development of intrathoracic HCs. It is thought that small sized embryos (< 0.3 mm) initially gain access to the systemic venous system, as they can't be filtered out from the portal blood by virtue of their small size, and thereafter get pumped to all parts of body. Another proposed mechanism presumes that embryos gain access into the systemic circulation via intestinal lymphatics. Some researchers have supported a third pathway that involves direct exposure to lungs through inhalation of contaminated air [4]. After gaining access to the systemic circulation, further voyage to the diaphragm may involve pulmonary-bronchial anastomosis, arterial channels from the phrenic artery and branches from the intercostal arteries [1]. Left hemidiaphragmatic cyst in our case can be explained with the embryos bypassing the two filters i.e. liver and lungs.
Serological tests for hydatid disease have low sensitivity (64-87%) and imaging modalities are the mainstay for diagnosis [5]. Both sonography and CT scan have their pros in the form of cost and widespread availability but when it comes to cysts with atypical appearance on CT scan and peridiaphragmatic location, MRI is a better imaging modality due to its superiority in defining anatomical relationships and better chest wall and diaphragm delineation [1,6]. MRI may have helped in making correct localization of the cyst within the left hemidiaphragm. Eren et al. and Mekki et al. have also proposed MRI as a superior imaging modality in comparison with CT scan for evaluation of complex giant hydatid cysts, their topographical relationships and suspected diaphragmatic and hepatic involvement [2,7].
Conclusion
Hydatid cysts of diaphragm should be considered in patients with preoperative imaging data indicating cystic lesions adjacent to the diaphragm. MRI should be done if the cyst is found to be in close proximity of diaphragm, or elsewhere if in doubt, to determine accurate soft tissue relationship preoperatively.
References
-
K Kjossev, J Losanoff, N Velitchkov, E Belokonski (2003) Hydatid Cyst of The Diaphragm: A Case Report And Review of The Literature. Internet Journal of Thoracic and Cardiovascular Surgery 6: 1.
-
Eren S, Ulku R, Tanrikulu AC, Eren MN (2004) Primary giant hydatid cyst of the diaphragm. Ann Thorac Cardiovasc Surg 10: 118-119.
-
Marla NJ, Marla J, Kamath M, Tantri G, Jayaprakash C (2012) Primary hydatid cyst of the lung: a review of the literature. Journal of Clinical and Diagnostic Research 6: 1313-1315.
-
Atoini F, Ouarssani A, Hachimi MA, Aitlhou F, Rguibi MI, et al. (2012) Intrathoracic extrapulmonary hydatid cysts. Pan Afr Med J 13: 7.
-
Jarboui S, Hlel A, Daghfous A, Bakkey MA, Sboui I (2012) Unusual location of primary hydatid cyst: soft tissue mass in the supraclavicular region of the neck. Case Rep Med 2012: 484638.
-
Ettorre GM, Vennarecci G, Santoro R, Laurenzi A, Ceribelli C, et al. (2012) Giant hydatid cyst of the liver with a retroperitoneal growth: a case report. J Med Case Rep 6: 298.
-
Alouini Mekki R, Mhiri Souei M, Allani M, Bahri M, Arifa N, et al. (2005) Hydatid cyst of soft tissues: MR imaging findings (Report of three cases). J Radiol 86: 421-425.