International Journal of Respiratory and Pulmonary Medicine
A Case Report of Endobronchial Ultrasound Needle Fracture
Som N Chalise, Craig Brown and Mark R Bowling*
Department of Pulmonary and Critical Care Medicine, East Carolina University School of Medicine, USA
*Corresponding author: Mark R Bowling, MD, Pulmonary and Critical Care Medicine, Associate Professor of Medicine, East Carolina University School of Medicine and Vidant Health, Director of Interventional Pulmonology and Pulmonary Diagnostic Services, Division Chief of Pulmonary and Critical Care Medicine and Vice Chair of Internal Medicine for Clinical Affairs, Consultant for Medtronic Corportation, USA, Tel: 252-744-4650, E-mail: bowlingm@ecu.edu
Int J Respir Pulm Med, IJRPM-3-040, (Volume 3, Issue 1), Case Report; ISSN: 2378-3516
Received: January 18, 2016 | Accepted: February 18, 2016 | Published: February 22, 2016
Citation: Chalise SN, Brown C, Bowling MR (2016) A Case Report of Endobronchial Ultrasound Needle Fracture. Int J Respir Pulm Med 3:040. 10.23937/2378-3516/1410040
Copyright: © 2016 Chalise SN, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA) has many potential complications though most occur infrequently. We encountered a case in which the EBUS needle broke during TBNA. The patient was a 65 year old man who underwent EBUS-TBNA for right paratracheal lymphadenopathy. During the procedure, the TBNA needle was found to be broken. We were able to completely recover it without any complications to the patient or to the EBUS scope.
Keywords
Endobronchial ultrasound, Transbronchial needle fracture
Introduction
EBUS-TBNA has gained popularity within the last decade. Compared to mediastinoscopy and biopsy, EBUS-TBNA boasts comparable results in terms of diagnosing and staging of lung cancer [1]. It is generally safe and minimally invasive. It is also used to diagnose benign causes of mediastinal adenopathy. The potential (albeit rare) complications from EBUS-TBNA include vascular puncture with mediastinal hemorrhage, air embolism, mediastinitis, bleeding into the airway [2-4]. Here we present a rare complication of equipment failure where an EBUS needle breakage occurred during the procedure. We perform EBUS-TBNA routinely at our institution and this is the first time we have observed this type of complication.
Case Report
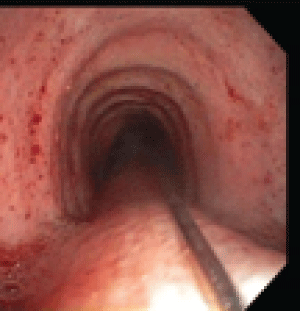
A 65 year old man with multiple medical problems including coronary artery disease status post coronary artery bypass graft, chronic atrial fibrillation, congestive heart failure, diabetes mellitus, rheumatoid arthritis, peripheral arterial disease was sent to the bronchoscopy lab to evaluate for the increasing size of his right paratracheal lymph node. At the time of his procedure, the size of this 4R station lymph node was 2.3 × 2.2 cm. The lymph node was located by EBUS. Three fine needle aspiration (FNA) samples were taken. On the third pass, the needle handle became extremely loose and felt very unusual to the operator. At this time the needle system was removed from the EBUS bronchoscope. The EBUS bronchoscope was pulled back in the trachea and the operator noticed that the needle was still inserted in the right para tracheal position. The EBUS scope was removed and the guidewire connected to the needle was seen extending through the entire trachea, through the vocal cords and out of the mouth (Figure 1). The patient remained stable. A standard flexible video bronchoscope was inserted into trachea.
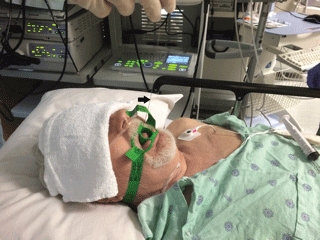
.
Figure 1: Guidewire is seen coming out of the mouth after EBUS scope was removed. Arrow points to the guidewire.
View Figure 1
The guidewire and needle were clearly seen, with the needle protruding from the right paratracheal area approximately 2 cm from the main carina (Figure 2 and Figure 3). No bleeding was noted. The needle and guidewire were removed intact by pulling on the guidewire protruding from the patients mouth (Figure 1). On inspection, no damage to the bronchial mucosa or upper respiratory tract was noted. No damage to the EBUS scope was noted. The EBUS scope was reinserted and the lymph node displayed no apparent ultrasound abnormalities. Two more FNA samples were obtained using a new needle. Adequate tissue was collected and confirmed by rapid on site evaluation as suspicious for small cell carcinoma. Post procedure chest X-ray did not demonstrate any abnormalities and the final pathology result confirmed small cell carcinoma. Photos were obtained at various points in the procedure and consent for disclosure of events and photographs were obtained after the case was concluded.
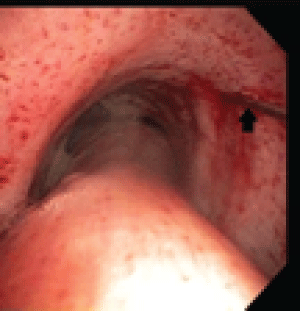
.
Figure 3: Arrow pointing to the distal end of guidewire attached to needle which penetrated the tracheal mucosa at level of the 4R station.
View Figure 3
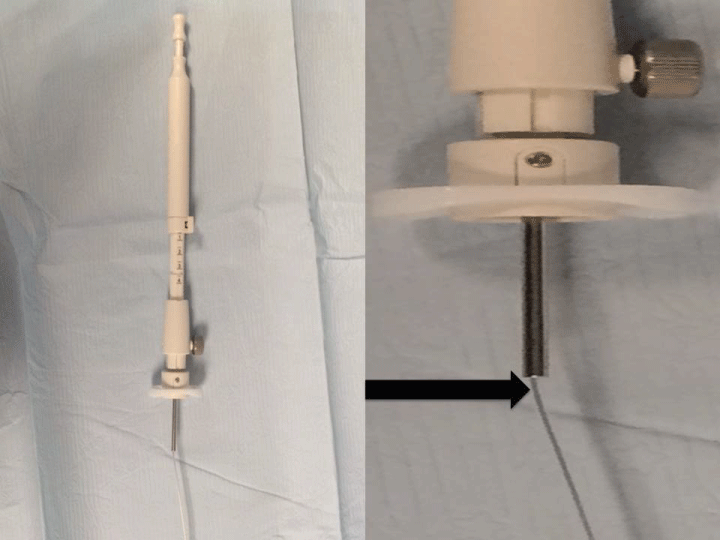
.
Figure 4: An example of the area of the EBUS needle system where the guidewire was fractured. See the arrow.
View Figure 4
Discussion
There has been an emerging use of EBUS-TBNA instead of over mediastinoscopy for biopsy of mediastinal and hilar lymphadenopathy given it is less invasive and of comparable sensitivity. It enables bronchoscopists to both diagnose as well as stage malignancy. EBUS-TBNA is a relatively safe procedure, however, there have been multiple complications reported with its use. According to a large retrospective study in Japan, where a total of 7,345 cases were analyzed, 90 total complications happened (1.23%) [2]. Hemorrhages were the most frequent with 50 cases (0.68%). Infectious complications occurred in 14 cases (0.19%), which included mediastinitis, pneumonia, pericarditis, cyst infection and sepsis. Pneumothorax happened in 2 cases (0.03%), one of which required chest tube drainage. Death occurred in 1 (0.03%) due to severe cerebral infarction. Breakage of the EBUS scope occurred in 98 cases (1.33%) with the puncture of needle through the scope in 15 cases (0.20%). No further details of puncture due to needle could be found.
Our literature search revealed that there are two case reports with EBUS needle breakage. The first case is from Turkey in 2012 where they performed EBUS to evaluate mediastinal lymphadenopathy in a 62 year old man. The first two passes for subcarinal lymph node sample were smooth. During the third pass, the needle tip was not seen on the ultrasonography monitor; hence it was felt that the needle was broken. The EBUS system was removed and it was discovered that 11 mm of the needle was broken. That broken segment was later found in the transverse colon, on an abdominal X-ray taken 3 hours afterwards. It was thought the needle tip was probably expelled from the bronchial system and trachea by EBUS contact or cough and it entered the gastrointestinal tract by swallowing. No further complication noted and felt that the needle tip was probably passed in the feces [3].
Another case, reported in abstract form describes a 52 year old male who underwent EBUS evaluation for left sided hilar mass with associated pleural effusion and mediastinal/hilar lymphadenopathy. The bronchoscopist felt unexpected resistance while advancing the needle through the working channel. The catheter was withdrawn and it was noted that the needle had been inadvertently advanced while still within the working channel. The remainder of the procedure was performed without any complications. During sterilization of the bronchoscope, it was found to be damaged. Several days after the procedure, the patient called in and reported that he had coughed up a spring, which was determined the that spring-like unit was a piece of the single use EBUS-TBNA aspiration needle [4].
Our presented case involved a unique pattern of needle breakage in that it fractured at the point where the catheter enters the handle of the needle apparatus (Figure 4). Similar cases were not reported previously. The needle breakage was discovered immediately, and we removed the broken segment completely without difficulty. The remainder of the procedure went smoothly, a diagnosis was confirmed and no harm came to the patient or to the EBUS scope. In retrospect, it is most likely that the wire that is connected to the needle was kinked as the needle was inserted into the working channel of the bronchoscope. It is believed that this most likely weakened the connecting wire and when the needle was deployed, it fractured at this kinked area.
Conclusion
Although many complications of EBUS-TBNA procedure have been reported, needle breakage is relatively rare. This type of needle breakage with complete recovery has not yet been reported. We recommend that if any segment of the needle apparatus becomes damaged during the procedure, that needle should be discarded and replaced with a new needle system to complete the procedure.
References
-
Yasufuku K, Pierre A, Darling G, de Perrot M, Waddell T, et al. (2011) A prospective controlled trial of endobronchial ultrasound-guided transbronchial needle aspiration compared with mediastinoscopy for mediastinal lymph node staging of lung caner. J Thorac Cardiovasc Surg 142: 1393-1400,e1391.
-
Asano F, Aoe M, Ohsaki Y, Okada Y, Sasada S, et al. (2013) Complications associated with endobronchial ultrasound-guided transbrochial needle aspiration: A nationwide survey by the Japan Society for Respiratory Endoscopy. Respir Res 14: 50.
-
Özgül MA, Çetinkaya E, Tutar N, Özgül G (2014) An unusual complication of endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA): the needle breakage. See comment in PubMed Commons below Ann Thorac Cardiovasc Surg 20 Suppl: 567-569.
-
Moughrabieh M, Zamora F, Dincer H, Podgaetz E, Gibson H (2015) Ebus Needle Breakage Leaving Foreign Body Behind: Thematic Poster Session. Am J Respir Crit Care Med 191: A3097.