International Journal of Respiratory and Pulmonary Medicine
Spontaneous Bacterial Pleuritis from Respiratory Source and High Adenosine Deaminase Level
Alberto Garcia-Zamalloa1*, Mar Zabalo2, Milagros Berruete3, Elena Telleria4, and Arantza Moyua5
1Internal Medicine Service, Policlinica Gipuzkoa, Basque Country, Spain
2Intensive Care Unit, Policlinica Gipuzkoa, Basque Country, Spain
3Biochemistry Laboratory, Policlinica Gipuzkoa, Basque Country, Spain
4Department of Emergencies, Policlinica Gipuzkoa, Basque Country, Spain
5Radiology Service, Policlinica Gipuzkoa, Basque Country, Spain
*Corresponding author: Alberto Garcia-Zamalloa MD, Internal Medicine Service, Policlinica Gipuzkoa, 20009 Gipuzkoa, Spain, Tel: 34-943.002800, E-mail: alberto.garciazamalloa@gmail.com
Int J Respir Pulm Med, IJRPM-2-020, (Volume 2, Issue 2), Case Report; ISSN: 2378-3516
Received: March 04, 2015 | Accepted: April 04, 2015 | Published: April 08, 2015
Citation: Garcia-Zamalloa A, Zabalo M, Berruete M, Telleria E, Moyua A (2015) Spontaneous Bacterial Pleuritis from Respiratory Source and High Adenosine Deaminase Level. Int J Respir Pulm Med 2:020. 10.23937/2378-3516/1410020
Copyright: © 2015 Garcia-Zamalloa A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Spontaneous Bacterial Pleuritis (SBP) is defined as spontaneous infection of a preexisting hepatic hydrothorax [1]. Although spontaneous bacterial peritonitis and SBP are closely related, the latter has seldom been reported and its pathogenesis remains unclear [2]. We present a case of SBP from a respiratory source and which showed an elevated level of Adenosine deaminase (ADA) value in pleural fluid, not previously described in medical literature.
Case Report
An obese 85 year-old woman was admitted to the hospital because of extreme dyspnoea after one week with fever and cough. She had been previously diagnosed with myelodysplastic syndrome, chronic renal failure with creatinine 2 mg/dl, glomerular filtrate 25 ml/min; and cirrhosis with moderate persistent ascites despite diuretic treatment and mild pleural effusion reaching a fifth of the right hemithorax.
On examination the temperature was 37.9�C, the blood pressure 110/70 and pulse rate 110 beats per minute. She was somnolent but arousable with verbal stimuli. Flapping was not evident. Hypophonesis on the right hemithorax was evident on auscultation. There were no clinical signs of ascites or peripheral edema.
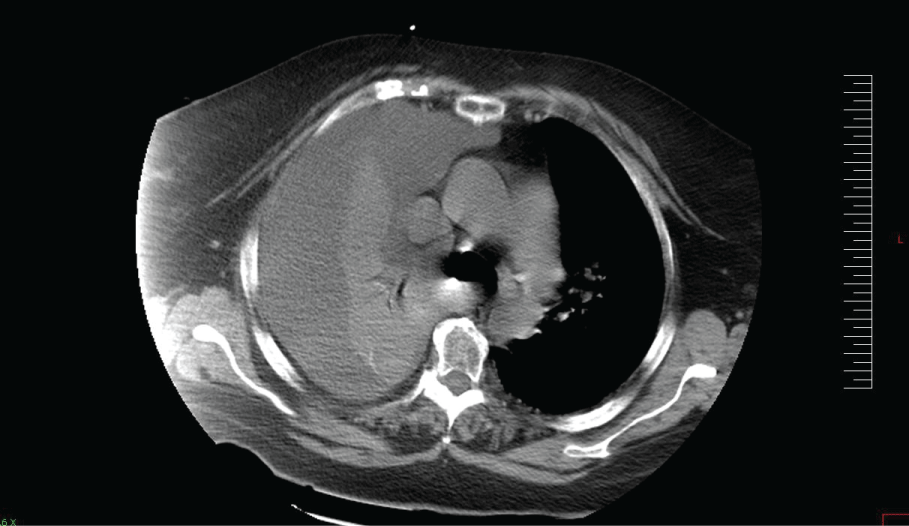
Blood tests showed on admission a remarkable white cell count of 16,600 per mm3 (90% neutrophils), hemoglobin 10.2g/dl, 110.000 platelets per mm3; urea nitrogen 211mg/dl, creatinine 3.56mg/dl, glomerular filtrate 13ml/min/kg, albumin 2.9g/dl, total bilirrubin 1.9mg/dl, prothrombine rate 11 sec. Sputum culture grew Streptococcus pneumoniae. Arterial blood gas examination showed PO2 56, PCO2 61 pH 7.36 BIC 38 and Saturation 88%. Pleural fluid values were as follows: pH 7.37, glucose 110mg/dl, total protein 1.9mg/dl, LDH 1490U/l and 2,240 leukocytes per mm3, 60% neutrophils (1,344 per mm3). ADA value was 56U/l (we tend to include ADA value in routine analysis in pleural fluid due to historical endemic tuberculosis). Pleural and blood cultures were negative. Thoracic and abdominal computed tomography showed a right sided pleural effusion occupying the whole right hemithorax and mild ascites, with no evidence of pneumonia (Figure 1).
.
Figure 1: On admission the patient�s thoracic computed tomography showed a right pleural effusion occupying the whole right hemithorax, with no evidence of pneumonia
View Figure 1
Noninvasive mechanical ventilation was initiated and simultaneously 2,300cc of pleural fluid were aspirated. Repeated thoracic computed tomography showed no evidence of pneumonia. Intravenous fluids, ceftriaxone, dopamine and furosemide were administered. Paracentesis was twice attempted without success. Febril defervescence, recovery of consciousness level and improvement of respiratory parameters and renal function were observed. Pleural effusion stabilized at a quarter of the hemithorax. A new thoracentesis six days later yielded a pleural fluid with the following values: pH 7.43, glucose 118 mg/dl, total protein 1.4mg/dl, LDH 207U/l, ADA 32U/l and 950 leukocytes per mm3, 40% neutrophils (380 per mm3). Antibiotics were administered for ten days; the patient recovered her previous clinical status and was finally discharged. Four months later, the patient remained with mild right pleural effusion as prior to admission (Figure 2).
.
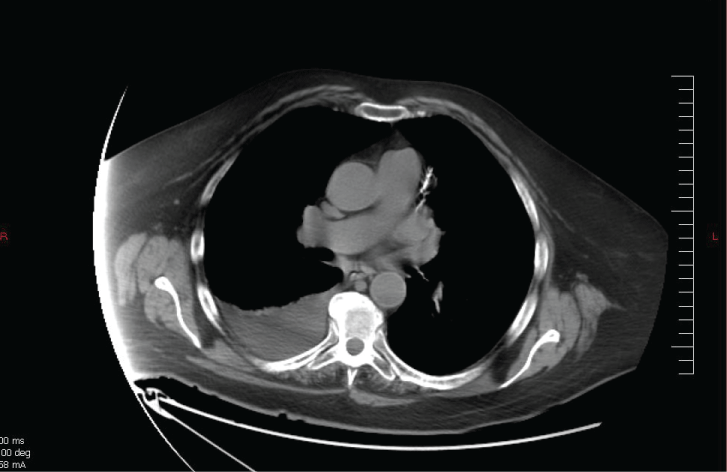
Figure 2: Four months after drainage and antibiotic treatment, the patient remained with mild right pleural effusion.
View Figure 2
Discussion
Spontaneous bacterial pleuritis (SBP) (or spontaneous bacterial empyema according to other authors) is a complication of cirrhotic patients in which a pre-existing pleural effusion becomes infected. Although Chen et al. [3] founded an incidence of 2.4% in cirrhotic patients and 16% in patients with cirrhosis and hydrothorax [3] it is considered to be an underdiagnosed pleural complication of such patients. Spontaneous bacteremia and flowing of infected ascites to pleural cavity are the two most commonly postulated mechanisms [2]. Diagnostic criteria of SBP are enumerated as follows: a) positive pleural fluid culture and polymorphonuclear cell count above 250 cells/mm3, or 2) more than 500 polymorphonuclear cells/mm3 if pleural fluid culture negative; 3) no evidence of pneumonia on chest radiograph or computed tomography, and 4) evidence of pleural effusion before the infectious episode or transudative pleural effusion during infection [4]. Clinical course and management are different from those of empyema secondary to pneumonia: antibiotic treatment to which cultured bacteria is susceptible is the treatment or choice [1], although large effusions involving more than half of the hemithorax constitute an indication for drainage [2].
Adenosine deaminase (ADA) is the most cost-effective pleural fluid marker for the diagnosis of tuberculous pleural effusion [5,6]. Most widely accepted cut-off value is 40U/l, with a sensitivity and specificity of 92% and 90% respectively for the diagnosis of tuberculous pleurisy [7,8] and such high levels in lymphocytic pleural effusions have also been reported in rheumatoid arthritis, lymphoma, bronchoalveolar carcinoma, mesothelioma, systemic lupus erythematosus, and in seldom cases of mycoplasma and chlamydia pneumonia, psitacosis, paragonimiasis, infectious mononucleosis, brucelosis, familial Mediterranean fever , histoplasma and coccidioidomycosis [9] along with this, one-third of cases of uncomplicated pleural effusions and two-thirds of those of complicated pleural effusions and empyema, both neutrophilic, may have an ADA level higher than 40U/l [10]. In an extensive study in our county through ten years and including 472 episodes of pleural effusion, ADA showed a sensitivity of 89% and specificity of 92% when used alone for the diagnosis of pleural tuberculosis; PPV and NPV values were 69% and 97%, but when combined with lymphocyte proportion higher than 50% specificity and PPV increased to 98% and 90% respectively. Seventy eight out of the 472 episodes (16%) were pleural effusions of miscellaneous origin, and the mean ADA value in pleural fluid in this group was 19U/l, with a standard deviation of 18U/l. Simultaneously, uncomplicated parapneumonic effusion was diagnosed in 92 cases (19%), with a mean ADA value in pleural fluid of 21U/l and a standard deviation of 10U/l [10].
Our patient developed a pleural effusion which fulfilled diagnostic criteria of SBP: within a previous hydrothorax, quickly increasing pleural effusion with more than 500 polymorphonuclear cells/mm3 was objectived, transiently exudative and without evidence of pneumonia on computed tomography. The clinical symptoms with fever and cough and the growth of Streptococcus pneumoniae in sputum culture make reasonable the hypothesis that the source was the respiratory tract; and accidentally we found that ADA level in pleural fluid was increased, which is not previously reported in this type of pleural effusions. It seems rational that pathogenesis of spontaneous bacterial pleuritis from respiratory source and parapneumonic effusion might sometimes be similar, with moving of fluid and cells across the adjacent visceral pleural membrane from the lung; and we might so suggest including SBP within the limited group of pleural effusions which may evolve with a high ADA level.
References
-
Light RW (2013) Pleural Diseases. (6th edn) Lippincot, Williams and Wilkins, Baltimore, USA: 144-147.
-
Tu CY, Chen CH (2012) Spontaneous bacterial empyema. Curr Opin Pulm Med 18: 355-358.
-
Chen CH, Shih CM, Chou JW, Liu YH, Hang LW, et al. (2011) Outcome predictors of cirrhotic patients with spontaneous bacterial empyema. Liver Int 31: 417-424.
-
Xiol X, Castellote J, Baliellas C, Ariza J, Gimenez Roca A, et al. (1990) Spontaneous bacterial empyema in cirrhotic patients: analysis of eleven cases. Hepatology 11: 365-370.
-
Porcel JM (2009) Tuberculous pleural effusion. Lung 187: 263-270.
-
Krenke R, Korczynski P. (2010) Use of pleural fluid levels of adenosine deaminase and interferon gamma in the diagnosis of tuberculous pleuritis. Curr Opin Pulm Med 16: 367-375.
-
Greco S, Girardi E, Masciangelo R, Capoccetta GB, Saltini C (2003) Adenosine deaminase and interferon gamma measurements for the diagnosis of tuberculous pleurisy: a meta-analysis. Int J Tuberc Lung Dis 7: 777-786.
-
Liang QL, Shi HZ, Wang K, Qin SM, Qin XJ (2008) Diagnostic accuracy of adenosine deaminase in tuberculous pleurisy: a meta-analysis. Respir Med 102: 744-754.
-
Gopi A, Madhavan SM, Sharma SK, Sahn SA (2007) Diagnosis and treatment of tuberculous pleural effusion in 2006. Chest 131: 880-889.
-
Garcia-Zamalloa A, Taboada-Gomez J (2012) Diagnostic accuracy of adenosine deaminase and lymphocyte proportion in pleural fluid for tuberculous pleurisy in different prevalence scenarios. PLoS One 7: e38729.





