International Journal of Respiratory and Pulmonary Medicine
Primary Mediastinal Goiter Resected via Cervical Approach
Benito Vargas-Abrego, Pablo Alvarez-Maldonado*, Rosa M Alcázar-López, Francisco C Lorente-Ludlow and Carlos Núñez-Pérez Redondo
Servicio de Neumología y Cirugía de Tórax, Hospital General de México "Dr. Eduardo Liceaga", D.F.
*Corresponding author: Dr. Pablo Alvarez Maldonado, Servicio de Neumología y Cirugía de Tórax, Hospital General de México "Dr. Eduardo Liceaga",México D.F., Tel/Fax: 052-55-27892000, E-mail: pamyacs@yahoo.com
Int J Respir Pulm Med, IJRPM-2-015, (Volume 2, Issue 1), Case Report; ISSN: 2378-3516
Received: January 16, 2015 | Accepted: February 21, 2015 | Published: February 24, 2015
Citation: Vargas-Abrego B, Alvarez-Maldonado P, Alcazar-Lopez RM, Lorente-Ludlow FC, Redondo CNP (2015) Primary Mediastinal Goiter Resected via Cervical Approach Int J Respir Pulm Med 2:015. 10.23937/2378-3516/1410015
Copyright: © 2015 Vargas-Abrego B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Primary mediastinal goiter is a rare entity. In most cases their finding is incidental. Excision is mandatory because of the risk of compression of vital structures within the chest. We report the case of a primary posterior mediastinal goiter that was resected through a cervical approach.
Keywords
Primary goiter, Aberrant goiter, Ectopic goiter, Mediastinum, Cervical approach, Thoracic surgery
Introduction
Primary Mediastinal Goiter (PMG), also known as intra-thoracic aberrant thyroid [1] or ectopic mediastinal goiter [2], is a rare entity with few cases reported in the literature. By definition it is a benign condition, but there have been cases of malignant primary intra-thoracic goitre [3]. Open thoracic surgery is recommended to safely remove the tumor identifying its intra-thoracic vascular supply. We report a case of primary posterior mediastinal goiter that was successfully resected through a cervical incision.
Case Presentation
A 66-year-old female was admitted to the hospital with complaints of dysphagia and cough of six months. She had history of rheumatoid arthritis of 15 years of diagnosis. Pancytopenia was evidenced secondary to methotrexate treatment for rheumatoid arthritis. Chest plain roentgenograms were taken (Figure 1). A minor enlargement of the superior mediastinal shadow was evidenced in frontal PA film. Lateral film showed an opacity displacing the trachea forward. An oral contrast film showed an opacity compressing the esophagus in its upper third. Computed tomography of the thorax showed a heterogeneous tumor in the posterior mediastinum, with well-defined edges and calcifications in its interior, adhered to the trachea, the esophagus and the vertebral column (Figure 2). She underwent transesophageal endoscopic ultrasound-guided fine-needle aspiration (EUS-FNA) obtaining the histopathological report of benign thyroid tissue. Thyroid function tests were normal. Methotrexate was suspended and pancytopenia improved. Before being discharged she received a thoracic surgery consultation for tumor resection. Two months after discharge she was hospitalized again for surgery. A cervical surgical approach with the intention to convert to thoracotomy was planned. Through a standard collar incision, digital exploration and tumor dissection was made that properly surround it in its entirety surface with no evidence of adherences to any intrathoracic structure. The goiter had its blood supply from a branch of esophageal arteries at its cranial edge, which was identified and ligated. The surgical specimen was then removed with a clamp getting scarce bleeding at the surgical bed. Hemostasis was verified leaving a closed drainage that was later withdrawn. The cervical thyroid gland was explored during surgery with no abnormalities found. There were no intraoperative or postoperative complications and the patient was discharged from the hospital three days after surgery.
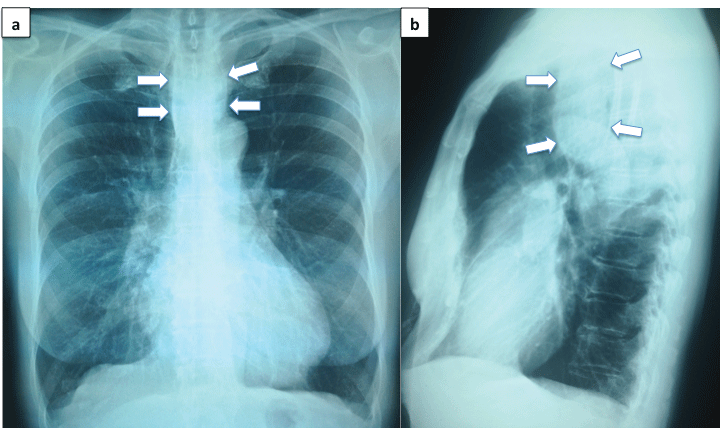
Figure 1: (a) Chest X-ray showing a slight widening of the upper mediastinal shadow (arrows). (b) Lateral film showing a displacement of the tracheal air column forward because of a rounded opacity (arrows).
View Figure 1
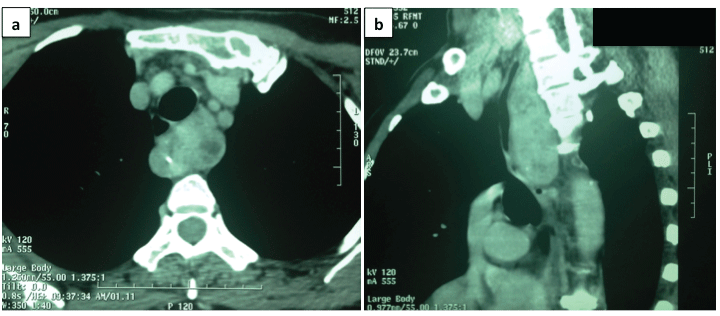
Figure 2: Computed tomography of the chest showing a posterior mediastinal tumor, with well-defined borders and calcifications in its interior. (a) Axial view showing compression of the trachea and esophagus by the tumor. (b) Sagittal view shows compression of the trachea and esophagus and adherence to the front of
the dorsal spine.
View Figure 2
Macroscopically, a tumor of 10 � 5 � 2 cm, with a multi-nodular surface, covered by a thin, translucent full capsule, with reddish brown and yellowish areas was reported (Figure 3a). Its interior was multi-nodular, composed by light brown areas of granular consistency, hemorrhagic areas and yellowish colloid-appearance areas. Indurated consistency areas were not identified. Microscopically (Figure 3b), small follicles of thyroid tissue with no colloid plus dilated cysts with abundant colloid were identified. Foamy macrophages, some with hemosiderin in their cytoplasm, were also reported. There were no findings suggestive of malignancy. Dysphagia and cough disappeared after surgery and the patient remained asymptomatic after 19 months of follow-up.
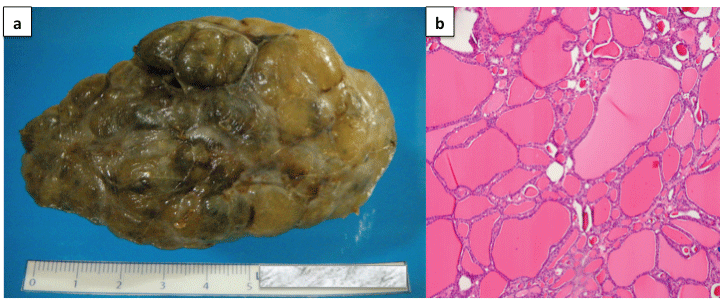
Figure 3: Macroscopic view. (a) A tumor with a multi-nodular surface, covered by a thin, translucent full capsule, with reddish brown and yellowish areas is observed. (b) Microscopically (H&E) small follicles of thyroid tissue with no colloid plus dilated cysts with abundant colloid were identified, with foamy macrophages, some with hemosiderin in their cytoplasm.
View Figure 3
Discussion
PMG, also known as aberrant goiter or ectopic mediastinal goiter implies the presence of intra-thoracic thyroid tissue independent of the cervical thyroid gland; its vascular supply comes from intra-thoracic vessels and is considered a benign entity. It�s localized primarily in the anterior mediastinum (85% of cases). The middle and posterior mediastinum are less frequent locations in 15% of cases [4].
It is a rare condition. Due to thyroid gland migration during embryonic development (between the 3rd and the 8th weeks) the location of primary ectopic goiter may occur from the tongue to the diaphragm. Most are located in the tongue (90%) and the anterior neck, superficial to the hyoid (10%). Are rarer locations the esophagus, trachea, heart and mediastinum. Among intra-thoracic goiters, PMG corresponds to 0.2-1%, affecting more often women [male:female=1:3]. In a review of the literature in 2011, Walz et al. [1] enlisted fourteen reported cases of PMG. Oueriachi et al. [5] found two cases of PMG among 152 cases of intra-thoracic goitre operated in ten years at a single center. Nistor et al. [6] found none in 22 years among 130 cases of cervico-mediastinal masses operated at a single center.
PMG is an incidental finding in most cases since there are no symptoms at the time of diagnosis [5]. When the tumor compresses adjacent structures, as in the case presented, symptoms such as dyspnea, dysphagia, stridor, cough or compression of venous vessels of the thorax could be present.
Simple chest roentgenogram remains a useful initial study, in which an enlargement of mediastinal shadow in more than half of the cases could be seen [7]. Computed tomography of the thorax, in addition to suggest the thyroid origin of the mediastinal mass [multi-cystic appearance with calcifications in its interior], may show a lack of continuity between PMG and the cervical thyroid gland. Magnetic resonance imaging may be useful defining more precisely the relationship of the tumor to adjacent structures. However, the definitive diagnosis is made only by means of histopathological analysis, often achieved only after removing the tumor. In some cases, biopsies can be obtained successfully using CT-guided puncture [1], or as in the case presented by trans-esophageal ultrasound-guided puncture.
Differential diagnoses of a mediastinal mass should be taken into account as lymphadenopathy, arterial aneurysm, neurogenic tumor, thymoma, teratoma, hamartoma, and primary esophageal and tracheal tumors among others.
Compression of vital structures of the mediastinum and the possibility of malignancy in a PMG [although rare] [3,7] make surgical excision the only treatment option. The specific surgical modality depends on the goiter location, size and relationship to adjacent structures [2,8]. Secondary intra-thoracic goitre are usually resected through an inferior cervical collar incision; nevertheless, extended mediastinal tumors beyond the aortic arch may require additional extra-cervical incisions including sternotomy, clavicular resection, anterior and posterolateral thoracotomy or video-assisted thoracoscopic surgery. When it comes to a PMG, which boundaries are completely within the chest, resection is often achieved through medial sternotomy or thoracotomy to ensure that the vessels supplying the tumor are properly ligated [5,9]. Removing the tumor through the neck can result in uncontrolled bleeding [10]; hence many authors reject this approach [4,5,11]; however, a careful cervical pathway approach leading to the identification and ligation of the feeding vessels of the goiter represents a reasonable alternative in selected cases [1,6]. A cervical video-thoracoscopy approach could be useful for resection, early identification of bleeding and bleeding control, mostly in anterior and middle mediastinum goitre [12,13]. The risks associated with sternotomy and thoracotomy like sternal dehiscence, osteomyelitis, mediastinitis, pneumothorax, bronchopleural fistula among others, besides an increase in postoperative pain and hospital stay [11,14] makes cervical approach a desirable alternative. A wide surgical approach by thoracotomy or sternotomy in large mediastinal masses responsible of tracheal compression is recommended [15] accompanied by close monitoring during surgery when there is compression of the heart, great vessels and/or the airway. The case presented is one of few in which PMG is successfully resected via cervical incision [1].
In conclusion, PMG is an unusual entity. A proper diagnosis approach allows optimal surgical planning for an experienced surgical team. Excision is mandatory because of the risk of compression of vital structures. Its resection via cervical incision with the possibility of converting to thoracotomy or sternotomy is an alternative in selected cases.
References
-
Walz PC, Iwenofu OH, Essig GF (2013) Ectopic mediastinal goiter successfully managed via cervical approach: case report and review of the literature. Head Neck 35: E94-97.
-
Houck WV, Kaplan AJ, Reed CE, Cole DJ (1998) Intrathoracic aberrant thyroid: identification critical for appropriate operative approach. Am Surg 64: 360-362.
-
Kanzaki R, Higashiyama M, Oda K, Okami J, Maeda J, et al. (2012) Surgical management of primary intrathoracic goiters. Gen Thorac Cardiovasc Surg 60: 171-174.
-
Foroulis CN, Rammos KS, Sileli MN, Papakonstantinou C (2009) Primary intrathoracic goiter: a rare and potentially serious entity. Thyroid 19: 213-218.
-
Oueriachi FE, Hammoumi MM, Arsalane A, Slaoui O, Diouri H, et al. (2014) Primary mediastinal goiters. Springerplus 3: 503.
-
Nistor C, Ciuche A, Motas C, Motas N, Bluoss C, et al. (2014) Cervico-mediastinal thyroid masses - our experience. Chirurgia (Bucur) 109: 34-43.
-
Shah BC, Ravichand CS, Juluri S, Agarwal A, Pramesh CS, et al. (2007) Ectopic thyroid cancer. Ann Thorac Cardiovasc Surg 13: 122-124.
-
Chen X, Xu H, Ni Y, Sun K, Li W1 (2013) Complete excision of a giant thyroid goiter in posterior mediastinum. J Cardiothorac Surg 8: 207.
-
Gamblin TC, Jennings GR, Christie DB 3rd, Thompson WM Jr, Dalton ML (2003) Ectopic thyroid. Ann Thorac Surg 75: 1952-1953.
-
Neri S, Chen F, Fujinaga T, Sato K, Sonobe M, et al. (2007) [Mediastinal aberrant goiter; report of a case]. Kyobu Geka 60: 1118-1121.
-
Machado NO, Grant CS, Sharma AK, al Sabti HA, Kolidyan SV, et al. (2011) Large posterior mediastinal retrosternal goiter managed by a transcervical and lateral thoracotomy approach. Gen Thorac Cardiovasc Surg 59: 507-511
-
Arango Tomas E, Baamonde Laborda C, Algar Algar FJ, Salvatierra Velazquez A (2014) Single-port thoracoscopic access for a mediastinal ectopic goiter. Cir Esp.doi: 10.1016/j.ciresp.2013.02.013.
-
Migliore M, Costanzo M, Cannizzaro MA (2010) Cervico-mediastinal goiter: is telescopic exploration of the mediastinum (video mediastinoscopy) useful? Interact Cardiovasc Thorac Surg 10: 439-440.
-
Naraynsingh V, Ramarine I, Cawich SO, Maharaj R, Dan D (2013) Cervical leverage: A new procedure to deliver deep retrosternal goitres without thoracotomy. Int J Surg Case Rep 4: 992-996.
-
Kacprzak G, Karas J, Rzechonek A, Blasiak P (2012) Retrosternal goiter located in the mediastinum: surgical approach and operative difficulties. Interact Cardiovasc Thorac Surg 15: 935-937.





