International Journal of Pathology and Clinical Research
A Battle against the Odds: Intensive Therapy in Thrombotic Storm
Priyanka Raheja1, Pável Olivera1, Verónica Pons1, Mercedes Pérez1, Joan Balcells2, Romy Rossich2 and Amparo Santamaría1*
1Department of Hematology, Vall d'Hebron University Hospital, Spain
2Department of Pediatric Critical Care, Vall d'Hebron University Hospital, Spain
*Corresponding author:
Amparo Santamaría Ortíz, Hemostasis and Thrombosis Unit, Department of Hematology, Hospital Universitari Vall d'Hebrón, Passeig Vall d'Hebron 109-119, 08035 Barcelona, Spain, Tel: +34-9327-46061, E-mail: asantamaria@vhebron.net
Int J Pathol Clin Res, IJPCR-2-048, (Volume 2, Issue 4), Case Report; ISSN: 2469-5807
Received: September 26, 2016 | Accepted: October 28, 2016 | Published: October 31, 2016
Citation: Raheja P, Olivera P, Pons V, Pérez M, Balcells J, et al. (2016) A Battle against the Odds: Intensive Therapy in Thrombotic Storm. Int J Pathol Clin Res 2:048. 10.23937/2469-5807/1510048
Copyright: © 2016 Raheja P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Thrombotic storm (TS) is a rare life-threatening entity that is characterized by multiple thrombotic events affecting diverse vascular sites occurring over a short period of time (days to weeks). We describe a case of a young boy who developed extensive and rapidly progressive thrombosis which required intensive treatment that included the use of triple antithrombotic therapy, pharmacomechanical thrombectomy, systemic thrombolytic therapy, and the combined use of plasmapheresis and immunosuppression. Our case highlights the use of aggressive therapy in a hematological emergency involving reduced blood flow to essential organs. We emphasize the need for a broad initial diagnostic approach to recurrent thromboembolism in young patients. We also discuss a novel treatment using the Trellis Thrombectomy system (Trellis-8™ system Covidien, Mansfield, MA), which in our patient had excellent efficacy and a positive outcome, without side effects.
Abbreviations
TS: Thrombotic Storm; DVT: Deep Vein Thrombosis; PE: Pulmonary Embolism; IVC: Inferior Vena Cava; LMWH: Low Molecular Weight Heparin; ATIII: Antithrombin III; PICU: Pediatric Intensive Care Unit; UFH: Unfractionated Heparin; HITT: Heparin Induced Thrombocytopenia and Thrombosis; PNH: Paroxysmal Nocturnal Hemoglobinuria
Introduction
Thrombotic storm (TS) is a rare life-threatening entity that is characterized by multiple thrombotic events affecting diverse vascular sites occurring over a short period of time (days to weeks). Patients are typically younger, usually have no prior history of thromboembolism and in most cases family history is negative. Just like in the general population, the most common thrombotic events sustained by these patients include deep vein thrombosis (DVT) and pulmonary embolism (PE). However, they also present thrombosis in unusual locations, including involvement of arterial and microvascular circulation and are often difficult to treat [1-4]. We describe a case of a young boy who developed extensive and rapidly progressive thrombosis which required intensive treatment that included the use of triple antithrombotic therapy, pharmacomechanical thrombectomy, systemic thrombolytic therapy, and the combined use of plasmapheresis and immunosuppression.
Case Presentation
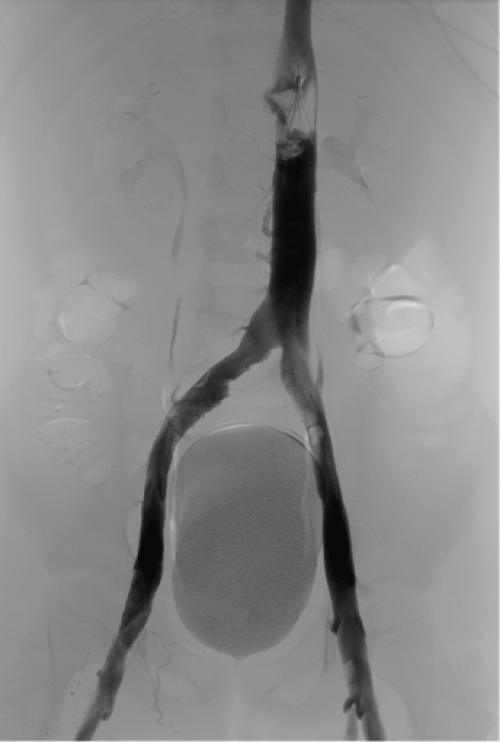
An 8-year-old Caucasian boy, whose only medical history consisted of a traumatic tendon injury requiring surgical repair at the age of 6 and without family history of thrombotic events, was admitted to a small hospital for community acquired pneumonia of unknown etiology, with right pleural effusion. On his seventh day of hospitalization, he presented with left leg swelling, whereby popliteal-femoro-iliac DVT with extension to inferior vena cava (IVC) was diagnosed. Initial laboratory test results revealed: hemoglobin 10.9 g/dL, platelet count 204000/mm3, white cell count 16710/mm3, a PTT ratio 1.2, prothrombin ratio 1.3, fibrinogen 328 mg/dL, quantitative D-dimer 16900 ng/mL, creatinine 0.42 mg/dL and C-reactive protein 15 mg/dL. Low molecular weight heparin (LMWH) therapy with 1 mg/kg/12 h of enoxaparin was initiated and he was referred to our tertiary teaching hospital. During his first week, an extensive diagnostic panel for thrombophilia, including testing for lupus anticoagulant, antiphospholipid syndrome and antithrombin III (ATIII) deficiency was performed, all laboratory testing being negative. On his tenth day in our center, despite the aforementioned anticoagulation, he developed shortness of breath and chest pain. Therefore, CT-angiography was ordered which showed acute PE, as well as a floating thrombus in IVC (Figure 1).
.
Figure 1: CT-Angiography shows thrombosis in both iliac veins and IVC before thrombectomy.
View Figure 1
Outcome
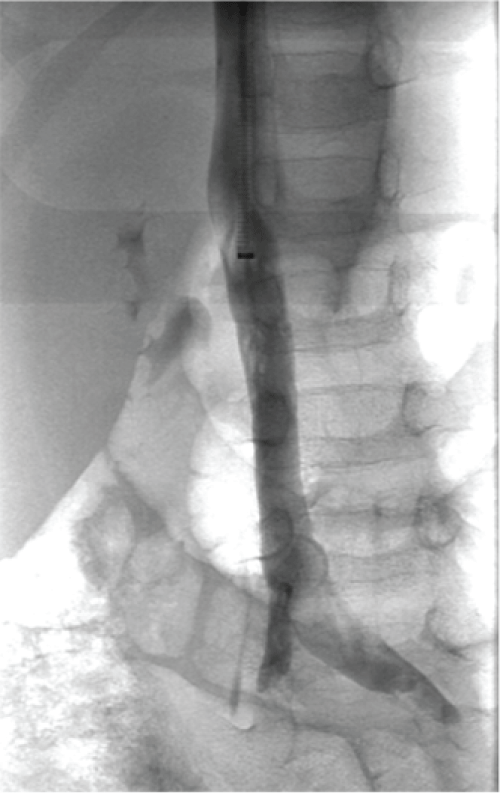
Due to the life threatening nature of his condition, a decision was made by a multidisciplinary team to proceed to pharmacomechanical thrombectomy and to intensify anticoagulant treatment with adjustment of the LMWH dose to achieve anti-Xa levels of 1.0-1.2 IU/mL (therapeutic range for anti-Xa activity 4 hours after enoxaparin administration is 0.8-1.2 U/ml). Although the Trellis thrombectomy system (Trellis-8™ system Covidien, Mansfield, MA) had not been tested on children, the benefit outweighed the risk and its use resulted in an almost complete aspiration of the thrombus (Figure 2). Additionally, an IVC filter was placed to prevent further PE, after which the patient was transferred to the pediatric intensive care unit (PICU), where a continuous infusion of unfractionated heparin (UFH) was initiated.
.
Figure 2: Pharmacomechanical thrombectomy being performed using Trellis system. The image shows inflation of balloons on either end of the thrombus before thrombectomy.
View Figure 2
Simultaneously, further testing to rule out malignancy, coagulation and autoimmune disorders and infectious diseases were ordered. While UFH was monitored with a PTT, anti-Xa assay (between a range of 0.3 to 0.7 UI) and thromboelastography (TEG 5000 Thrombelastograph® Hemostasis Analyzer System, Braintree, MA, USA).
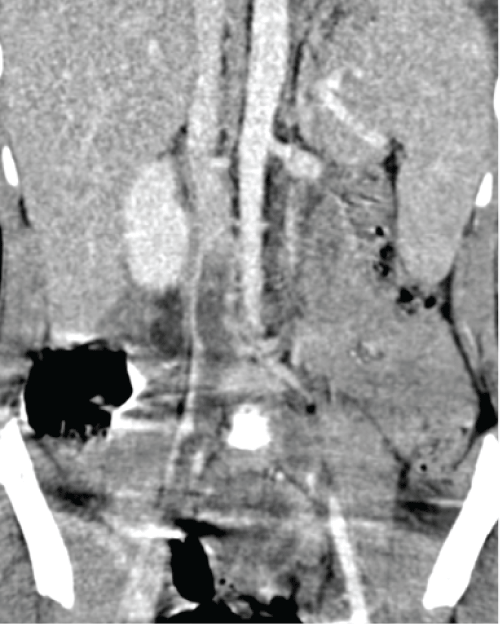
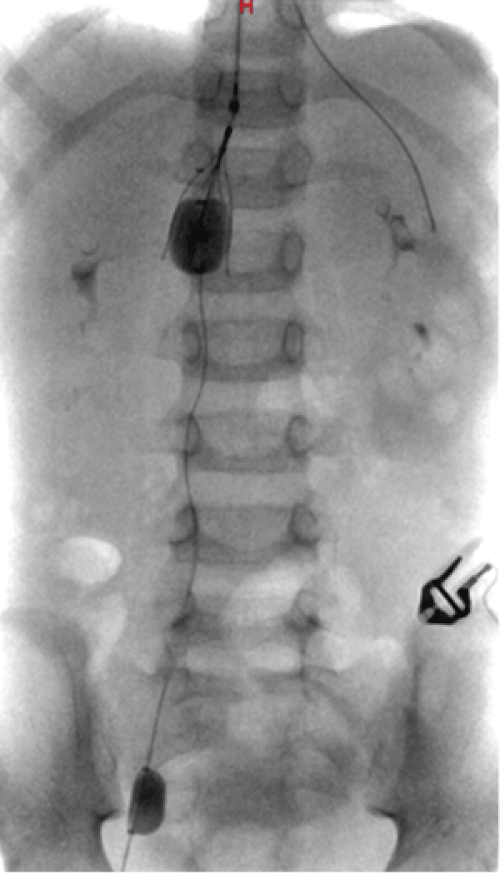
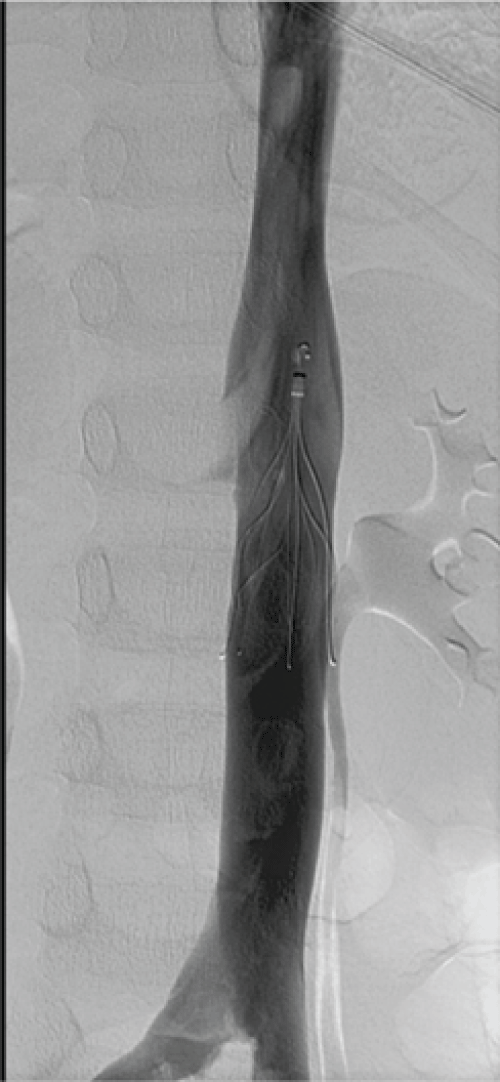
Nevertheless, after three days, he was found to have femoroiliac rethrombosis and IVC filter occlusion (Figure 3). Consensus was reached to implement pharmacomechanical thrombectomy again (Figure 4). The pathology report of the thrombus sample did not find evidence of infectious diseases. At the same time, antithrombotic therapy was intensified by adding ant platelet therapy (aspirin at 5 mg/kg/12h), continuous epoprostenol intravenous infusion and dipyridamole (at 1 mg/kg/8h), while UFH was maintained. In spite of having normal ATIII levels, due to pediatric ICU protocol ATIII was administered, after which systemic fibrinolysis with alteplase at 0.2 mg/kg/h was initiated. Four days later, the IVC filter was removed because of rethrombosis and the Trellis system was used again for thrombus removal (Figure 5).
.
Figure 4: After the administration of urokinase the thrombosis in the IVC filter dissolves.
View Figure 4
Given the massive acute thrombotic scenario and the poor therapeutic efficacy, other possible diagnoses such as heparin induced thrombocytopenia and thrombosis (HITT) were considered. Despite the low probability of HITT, heparin antibody (anti-platelet factor 4) testing was performed. The aforementioned immunoassay resulted positive although platelet aggregates in functional assays, were negative. Nevertheless, heparin was discontinued while an intravenous infusion of bivalirudin was started. Although, 4 days later, the patient developed massive rethrombosis in lower venous territory up to intrahepatic IVC, in spite of accurate a PTT controls. Therefore, due to the fact that heparin had already been discontinued, that the patient lacked thrombocytopenia or any other criteria suggesting HITT and taking into consideration the immunologic imbalance that takes place in this entity, it was concluded that HITT was not the primary cause of the thrombotic manifestations.
At this point, results for genetic thrombophilia testing, HACEK group serologies, blood cultures, HLAB51 for Behçet's disease and antiphospholipid syndrome antibodies, were all negative. On the other hand, an autoimmune panel was positive for cold agglutinin, antinuclear antibodies (at a titre of 1/80) and anti-Ro antibodies. Despite the inconclusive results, empirical immunomodulator treatment was started on his 19th day, using high-dose intravenous methylprednisolone (30 mg/kg/24h for 3 days and then 2 mg/kg/24h), four sessions of plasmapheresis, high dose immunoglobulins (2 g/kg) and mycophenolate. PET-CT and bone marrow aspiration were performed for cancer screening, although results were unremarkable. Paroxysmal nocturnal hemoglobinuria (PNH) was also ruled out.
On his 26th day in the ICU, there was evidence of IVC rethrombosis. Lower extremity DVT was ruled out using ultrasonography. The IVC filter was replaced by a new filter and a fourth and last pharmacomechanical thrombectomy was performed. As neither heparin nor bivalirudin were effective, after 48 hours of clinical stability, coumarin treatment was started. A week later, ultrasonography showed patency of IVC, iliac and deep femoral vessels, along with partial thrombosis of the left superficial femoral vein. Due to clinical and imaging improvement, the IVC filter was removed. Patient was discharged with oral coumarin, aspirin, oral cortisone, and mycophenolate. After a two year follow up the young boy is healthy and is following long term antiplatelet (aspirin) and antithrombotic (coumarin) therapy with self-managed INR monitoring, without further evidence of thrombotic events.
Discussion
Thrombotic Storm, first described by Kitchens in 1998, is frequently preceded by triggers that initiate the process, such as pregnancy, infection, trauma, surgery and/or inflammatory states [1]. In our patient’s case TS was precipitated by community acquired pneumonia. Although its aetiology is unknown, an extensive thrombophilia workup, malignancy and autoimmune panel should be performed to rule out hypercoagulable conditions (taking special consideration to rule out catastrophic antiphospholipid syndrome). Testing for varicella and group A streptococcus antigens may also be useful. Most patients exhibit evidence for an acute inflammatory state on initial presentation, such as elevated C-reactive protein and erythrocyte sedimentation rate [2].
Although TS is a rare condition, it is essential that it be recognized due to its potentially life-threatening nature. TS diagnosis is established by stereotypical clinical behaviour using a set of criteria devised by the Thrombotic Storm Study Group [3]. Anticoagulant treatment should be initiated immediately at full therapeutic dosing using conventional monitoring goals. If despite anticoagulation, there is rapid progression or development of multifocal thrombosis, then catastrophic antiphospholipid syndrome, heparin-induced thrombocytopenia or thrombotic thrombocytopenic purpura, should be considered [4].
In Manco-Johnson, et al.'s review of 8 case studies, pharmacomechanical thrombolysis via an interventional radiologic approach, local catheter-directed and systemic tPA administration, surgical thrombectomy, or a combination of these modalities were used in each child [5]. In our patient the Trellis Thrombectomy system with urokinase was used. The aforementioned system reduces thrombolytic dose by half and decreases the average necessary infusion period to less than 30 minutes. This device traps the thrombolytic agent between a proximal and a distal balloon, preventing systemic release and restricting the area of thrombolysis. An oscillating wire optimizes dispersal of the thrombolytic agent while the thrombus is mechanically fragmented. The remaining mixture of drug and clot is subsequently aspirated [6].
Most of the current literature advises against the use of an IVC filter in TS, but given that the thrombus was located in the inferior vena cava, an IVC filter was placed for lung protection. Even though later on the filter thrombosed, probably because of the patient’s hypercoagulable state (lower extremity DVT was ruled out), it was still considered necessary to place it before thrombectomy to prevent a massive pulmonary embolism. In children, there is limited clinical data on IVC filters (case reports, small case series and a retrospective review) [7,8]. The most important indication for the use of IVC filters in both adults and children is the prevention of PE in patients with lower limb VTE in whom systemic anticoagulation is contraindicated either on a temporary or long term basis. Other relative indications include failure of anticoagulation, such as recurrent symptomatic PE despite adequate anticoagulant therapy, inability to achieve/maintain adequate anticoagulation and propagation of DVT on therapeutic anticoagulation [8,9].
There are only six cases described in current literature that combine antithrombotic, pharmacomechanical thrombectomy, systemic thrombolysis and immunomodulatory therapies in a short time frame [1-5,10]. Our case highlights the use of aggressive therapy in a hematological emergency involving reduced blood flow to essential organs. We emphasize the need for a broad initial diagnostic approach to recurrent thromboembolism in young patients by ruling out catastrophic APS, congenital thrombophilia, HITT, DIC, TTP, PNH and malignancy. We also discuss a novel treatment using Trellis Thrombectomy system, which in our patient had excellent efficacy and a positive outcome, without side effects. As for patients that survive the storm, long term anticoagulant therapy is recommended, using either LMWH or an oral vitamin K antagonist, since it’s the only way to curtail thrombosis.
Financial Disclosure
The authors have no financial relationships relevant to this article to disclose
Potential Conflicts of Interest
The authors have no conflicts of interest relevant to this article to disclose.
Contributors' Statement
• Priyanka Raheja: Dr. Raheja drafted the case report and approved all corrections made to it, including the final version to be published.
• Pável Olivera, Amparo Santamaría and Verónica Pons: Dr. Olivera, Dr. Santamaría and Dr. Pons critically revised the case report and made substantial corrections to all the drafts.
• Mercedes Pérez: Dr. Perez obtained the images in the case report and critically revised the section on the Trellis thrombectomy system, making a substantial contribution to the final draft.
• Joan Balcells and Romy Rossich: Dr. Balcells and Dr. Rossich critically revised all data pertaining to the patient's time in the pediatric intensive care unit and made important corrections to the initial draft.
All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
References
-
Kitchens CS (1998) Thrombotic storm: when thrombosis begets thrombosis. Am J Med 104: 381-385.
-
Ortel TL, Kitchens CS, Erkan D, Brandão LR, Hahn S, et al. (2012) Clinical causes and treatment of the thrombotic storm. Expert Rev Hematol 5: 653-659.
-
Kitchens C, Erkan D, Brandao L, Hahn S, James A, et al. (2011) Thrombotic Storm Revisited: Preliminary Diagnostic Criteria Suggested by the Thrombotic Storm Study Group. The American Journal of Medicine 124: 290-296.
-
Aryal MR, Badal M, Bhandari N, Bhatt VR (2013) Accelerated arterial and venous clots in a young pregnant woman: a saga of thrombotic storm. BMJ Case Rep 2013.
-
Manco-Johnson MJ, Wang M, Goldenberg NA, Soep J, Gibson E, et al. (2012) Treatment, survival, and thromboembolic outcomes of thrombotic storm in children. J Pediatr 161: 682-688.
-
O'Sullivan G, Lohan D, Gough N, Cronin C, Kee S (2007) Pharmacomechanical Thrombectomy of Acute Deep Vein Thrombosis with the Trellis-8 Isolated Thrombolysis Catheter. Journal of Vascular and Interventional Radiology 18: 715-724.
-
Kukreja KU, Gollamudi J, Patel MN, Johnson ND, Racadio JM (2011) Inferior vena cava filters in children: our experience and suggested guidelines. J Pediatr Hematol Oncol 33: 334-338.
-
Chalmers E, Ganesen V, Liesner R, Maroo S, Nokes T, et al. (2011) Guideline on the investigation, management and prevention of venous thrombosis in children. Br J Haematol 154: 196-207.
-
Monagle P, Chan AK, Goldenberg NA, Ichord RN, Journeycake JM, et al. (2012) Antithrombotic therapy in Neonates and children: Antithrombotic therapy and prevention of thrombosis, 9th ed: American college of chest physicians evidence-based clinical practice guidelines. Chest 141: e737S-801S.
-
Maggi U, Rossi G, Avesani EC, Artoni A, Caprioli F, et al. (2013) Thrombotic storm in a teenager with previously undiagnosed ulcerative colitis. Pediatrics 131: e1288-1291.