International Journal of Pathology and Clinical Research
Spontaneous Duodeno-Colic Fistula: A Case Report and Literature Review
Meizhuo Gao1*, Tie Wang2,3, Lining Tian4 and Jinlu Zhao1
1Department of General Surgery, The Forth Affiliated Hospital of Harbin Medical University, China
2Department of Gastrointestinal Surgery, Harbin Medical University Cancer Hospital, Harbin, Heilongjiang Province, China
3Gastrointestinal Research Group, Department of Physiology and Pharmacology, Calvin, Joan and Phoebe Snyder Institute of Chronic Diseases, Cumming School of Medicine, University of Calgary, Calgary, Alberta, Canada
4Department of Continual Education, The First Affiliated Hospital of Harbin Medical University, China
*Corresponding author:
Dr. Meizhuo Gao, Department of General Surgery, The Forth Affiliated Hospital of Harbin Medical University, Nangang, Harbin, China, Tel: +86-451-85939305, E-mail: Dr.MZGao@outlook.com
Int J Pathol Clin Res, IJPCR-2-046, (Volume 2, Issue 4), Case Report and Literature Review; ISSN: 2469-5807
Received: August 29, 2016 | Accepted: October 27, 2016 | Published: October 30, 2016
Citation: Gao M, Wang T, Tian L, Zhao J (2016) Spontaneous Duodeno-Colic Fistula: A Case Report and Literature Review. Int J Pathol Clin Res 2:046. 10.23937/2469-5807/1510046
Copyright: © 2016 Gao M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Duodeno-colic fistula is an unnatural connect between the duodenum and the colon, which occurs rarely with the onset in the middle-aged. This report summarized the clinical manifestation and surgical treatment of the sixth case of spontaneous duodenum-colic fistula and reviewed the published other five cases.
Methods and analysis: The clinical manifestation and course of a 54-year-old female with spontaneous duodeno-colic fistula was reported. The clinical features of all six known cases were also summarized.
Results: The patient agreed and signed the informed consent for the future research and publication. The chief complaint of the patient was chronic diarrhea. The endoscopy procedure and the barium meal examination confirmed the diagnosis of duodeno-colic fistula. The fistula, as well as affiliated duodenum and colonic wall was surgically removed en block. Only unspecific inflammation was observed in the histological exam.
The fistula had normal mucosa and muscularis layer. During a 24-month clinic follow up after surgery until August 2016, the patient remains symptom free.
Conclusion: Once a patient is diagnosed with duodeno-colic fistula, a careful history and physical examination, as well as imaging studies, should be performed to exclude the possibilities of secondary fistula. Non-surgical procedures or low invasive surgeries are recommended to patients with spontaneous duodeno-colic fistula.
Keywords
Duodeno-colic fistula, Congenital, Spontaneous, Surgery
Introduction
Duodeno-colic fistula is an abnormal communication connecting the duodenum and the colon. The main symptoms of duodeno-colic fistula are diarrhea and reflux of colonic content to the duodenum. The aetiology for duodeno-colic fistula could be benign or malignant (resulting from cancer or sarcoma) [1]. A malignant fistula results from tumor arising from the duodenum or the colon. The possible benign causes might be peptic ulceration, duodenum diverticulum, a perforation of typhoid, tuberculosis, ulcerative colitis, acute cholecystitis, pancreatitis, appendicitis or ileitis, complication post gastrectomy, and even the swallowed foreign body [2,3]. However, in some cases of duodeno-colic fistula, no obvious reason can be observed, therefore this situation is regarded as spontaneous or congenital duodeno-colic fistula. In this paper, we report a case of congenital duodeno-colic fistula and discuss the future non-surgical therapeutic options.
Case Report
A 54-year-old female farmer (the case number: ZY010001904807), visited the out-patient clinic of the Forth Affiliated Hospital of Harbin Medical University, with a chief complain of chronic diarrhea for more than ten years. The lady stated to suffer diarrhea more than a decade ago. The frequency of diarrhea was 5 to 6 times daily. She also had lower abdominal pain before the bowel movement, eased by defecation. She had loose stool with undigested food. She stated no blood seen in the stool. Diarrhea often happened 5 to 10 minutes after food intake. Oral administration of antibiotics attenuated the symptoms. The lady lost appetite as well as her body weight. In the previous 6 months before this visit, she lost 2.5 kg in weight. She felt fatigue. She had no nausea, vomit, or belch. She was admitted on August 6th, 2014.
Previous history
The patient had no serious illness. The patient also denied any surgery-related history, abdominal trauma, or history of swallowing any foreign object.
Physical examination
She had an ill-looking general status, which was thin but developed normally. The color of her skin and mucosa was not pale. No edema was observed. Her vital signs were in the normal ranges. There were no abnormalities in the cardiac or respiratory examination. A slight tenderness in the upper right abdomen was palpated, otherwise no pathological signs were found in the abdominal check. The limbs and spine were normal. No abnormal signs were found in neurological system. Rectal examination was normal.
Laboratory Investigation
No evidence for anemia was found in a complete blood count test. A coagulation test at admitting demonstrated the normal results.
Endoscopy examination
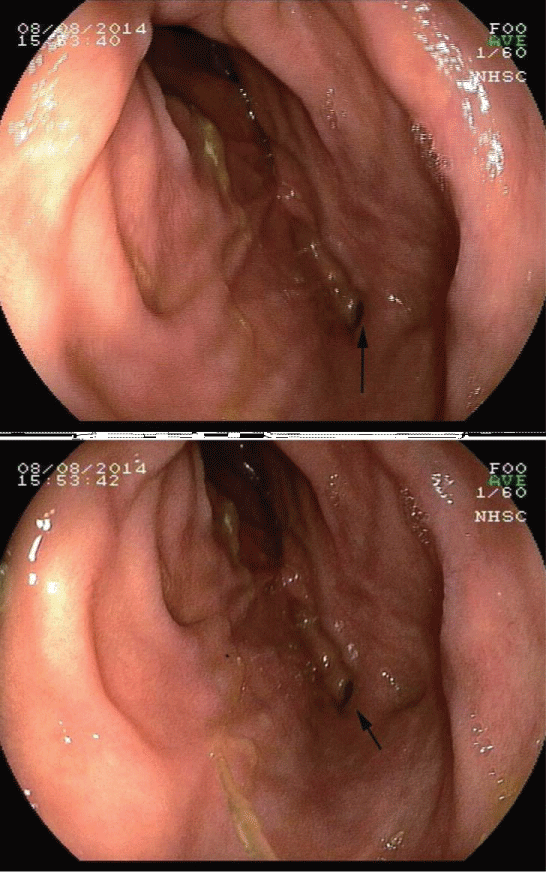
The upper gastrointestinal endoscopy revealed a small polyp in the gastric fundus (Yamada type I [4], 0.4 cm × 0.4 cm) and an opening of a fistula in the second part of the duodenum (Figure 1). The mucosa surrounding the opening had normal appearance. The colonoscopy examination revealed normal mucosa of the entire colon and the rectum.
.
Figure 1: An opening of the fistula was found under the inspection of an upper gastrointestinal endoscopy (black arrows). The opening was located at the second part of the duodenum, and the mucosa around the opening was normal.
View Figure 1
Radiology
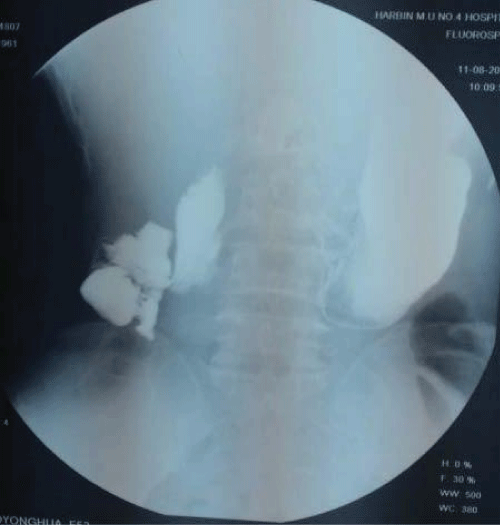
The patient received a barium meal examination on August 11th, 2014. The examination demonstrated a fistula connecting the descending portion of the duodenum and the hepatic flexure of the colon (Figure 2). The diagnosis of duodeno-colic fistula was confirmed by the barium meal examination. No peptic ulcer, duodenum diverticulum, or tumor was observed during the barium meal examination and a following computed tomography scan.
.
Figure 2: The barium meal examination showed the duodeno-colic fistula. Under X-ray, the barium meal came into the hepatic flexure of the colon directly from the duodenum through the fistula, demonstrating the abnormal communication between the second part of the duodenum and the hepatic flexure of the colon.
View Figure 2
Clinical Course
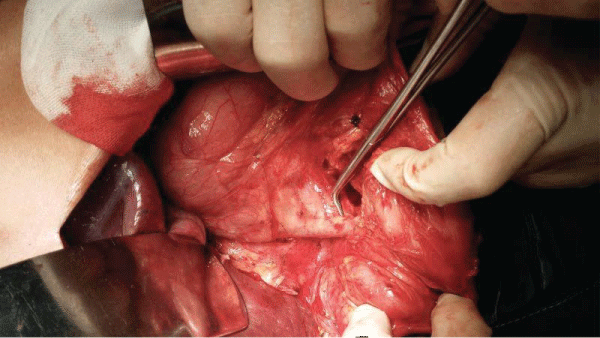
After mechanical and medication preparation of the colon, the patient received an exploratory laparotomy through a right rectus incision on August 13th, 2014. A fistulous track connecting the junction of the second and third parts of the duodenum and the mesenteric edge of hepatic flexure of colon was present (Figure 3). No evidence of inflammation or tumor was observed around the fistula. No other lesion in the peritoneal cavity was observed. A part of the duodenum, as well as the entire fistula and the affiliated colon wall, was removed en block, as the surgical team concerned the possibility of occult neoplasm caused by the potential chronic reflux of the colonic content into the duodenum. The duodeno wall was repaired by the nearby bowel wall. A drainage tube was placed in the duodenum lumen proximally to the fixation (Figure 4). The rapid frozen section during the operation showed no evidence of tumor. At Day 6 post operation, the drainage from the duodenum was 900 ml daily. But, the volume decreased gradually since Day 8 after surgery. At Day 11 after surgery, the drainage tube was removed. The patient remained symptom-free after surgery, and she was discharged two weeks later post operation. The patient has been followed up for 24 months after discharge by clinic visits, during which no abnormal symptoms and signs have been observed.
.
Figure 3: At laparotomy, a fistula connecting the junction of the second and third parts of the duodenum and the hepatic flexure of the colon was found. There was neither inflammation nor neoplasm around the fistula. The peritoneum cavity was clean. No other lesion was found.
View Figure 3
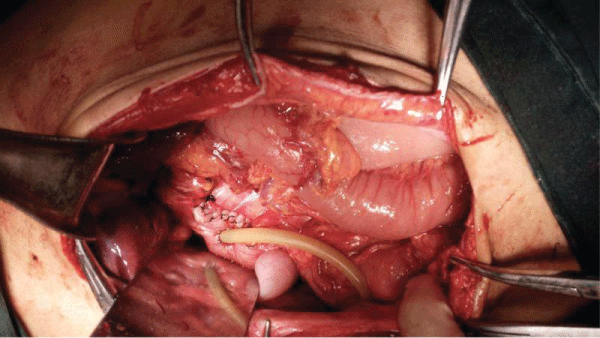
.
Figure 4: A partial duodenum resection was performed, and the fistula and the affiliated colonic wall were resected. The duodeno wall was repaired by the nearby bowel wall. A drainage tube was placed in the duodenum lumen proximally to the fixation.
View Figure 4
Pathology finding
The microscopic examination found neither severe inflammation nor neoplasm in the fistula, the resected section of duodeno, or the colonic wall. Mild unspecific inflammation was seen. The fistula had normal epithelium layer and muscularis layer (Figure 5).
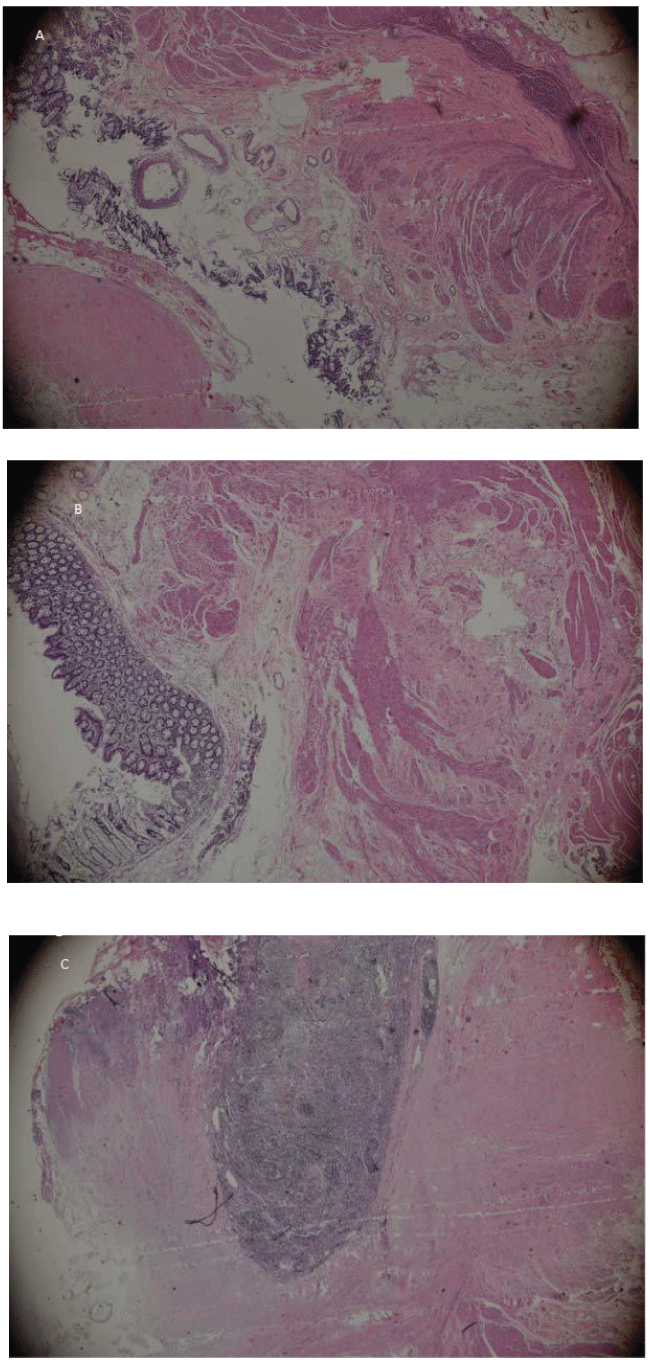
.
Figure 5: Pathology findings. No evidence for inflammation or neoplasm was found under microscopy. The fistula had normal muscularis layer and epithelium layer. A) The lumen of the fistula. Mucosa and muscularis layers are observed around the lumen. 100x; B) The mucosa layer and the muscularis layer of the fistula. 200x; C) Mildly infiltrated immune cells are seen in the wall of the fistula. 200x.
View Figure 5
Literature Review and Discussion
The prevalence of duodeno-colic fistula is very low. The first case of duodeno-colic fistula was reported in 1857 [5], while the first fully documented case, which we can trace now, was published in 1863 [6]. The etiology of duodeno-colic fistula is divided into two major classifications: (1) malignant fistula, which results from cancer or sarcoma; and (2) benign fistula, which is caused by varied benign diseases such as peptic ulcer, duodenum diverticulum, typhoid perforation, tuberculosis lymphadenitis, ulcerative colitis, inflammation of the bile duct system and pancreas, the complication of surgery, and others. But, in this case, no above etiology was observed. We considered this was a case in a new category- spontaneous idiopathic duodeno-colic fistula.
To our best knowledge, this is the sixth reported case of spontaneous duodeno-colic fistula, in addition to the three cases recorded by the team of Dr. Torrance in 1972 [7], one case by Dr. McKelvey and colleagues [8], and another case by Dr. Narula and Dr. McCormick [9]. The features of the published cases have been summarized in table 1. The disease occurs in the middle-aged. It seems that males and females have the similar susceptibility to spontaneous duodeno-colic fistula. The symptoms related to duodeno-colic fistula are diarrhea with or without steatorrhea which is aggravated by food intake, weight loss, and the laboratory findings for anemia, and Vitamin B12 deficiency. Fecal vomiting without the evidence of bowel obstruction has diagnostic value. However, these symptoms are duodeno-colic fistula related, not specific to spontaneous duodeno-colic fistula. In the collected 6 cases, no fecal vomiting was seen. Our opinion is if unexplained diarrhea is present, the possibility of spontaneous duodeno-colic fistula should be considered.
![]()
Table 1: Details of reported cases of spontaneous duodeno-colic fistula.
View Table 1
In agreement with Dr. Torrance, the etiology of spontaneous duodeno-colic fistula might be congenital and embryological, since the fistula has a similarly normal histological appearance which is between that of the duodenum and the colon [7]. The case in this current study also showed nearly normal histological appearance of the fistula, which had mucosa layer and muscularis layer. However, the precise pathogenesis of spontaneous duodeno-colic fistula remains unknown.
Surgical resection of ligation of the fistula is a curative therapy for spontaneous duodeno-colic fistula. We performed the resection of a segment of duodenum, the fistula and the affiliated colonic wall for our patient. During the laparotomy, we did not observe any signs for inflammation or tumor. But, we were concerning the long-term colonic reflux to the duodenum might cause potential neoplasm, so we performed the partial duodenum resection.
Treatment Suggestion
As the lack of awareness of this disease at the time of surgery, we performed a major abdominal procedure with high risks. Once spontaneous duodeno-colic fistula is introduced, conservative therapeutic strategies should be applied based on the benign nature of this disease. Low invasive procedures, for instance the closure of fistula by laparoscopy, could also be considered. The covered self-expending metal stents (SEMS), which have been reported to be placed by endoscopy for the treatment of malignant duodeno-colic fistula [10], might be a potential therapeutic option for spontaneous duodeno-colic fistula, especially for the old patients with other concurrent medical conditions. After a careful assessment of the abdomen and the entire gastrointestinal tract, the benefit and the risk (especially the possibility of tumor) of the endoscopic placement of SEMs should be balanced by the health care team including surgeons, gastroenterologists and nurses. So far, the therapeutic value of open surgical procedure (maybe include laparoscopic techniques) is definite.
Conclusion
In brief, spontaneous duodeno-colic fistula is a benign disease. If a patient obtains a diagnosis of duodeno-colic fistula, a careful medical history and physical examination, as well as imaging studies, are recommended to exclude the causes for fistula. Once a spontaneous duodeno-colic fistula exits, non-surgical procedures or low invasive surgeries should be considered prior to an open surgery.
Author Contribution
Dr. Meizhuo Gao, M.D. PhD., the chief surgeon, the head of the Department of General Surgery, saw the patient in the clinic. Dr. Gao made the diagnosis of the disease, and also performed the operation. Dr. Gao organized the process of collecting literatures and writing the report. Dr. Gao is the corresponding author of the report, and responsible for all the process of the report. Dr. Tie Wang, M.D, PhD. Student, the attending surgeon, attended the consultation. Dr. Wang composed the manuscript.
Dr. Lining Tian, M.D., attended the consultation, and searched the published literatures. Dr. Jinlong Zhao M.D., the assistant of Dr. Gao, attended the operation and was responsible for peri-operative management and the follow-up.
Funding Source
This work was not supported by any funding.
Conflicts of Interest
The authors claim no competing interests.
References
-
Hopkins JD (1965) Duodeno-colic fistula. A case report. J Natl Med Assoc 57: 231-232.
-
Schreiber S, Rosenstiel P, Albrecht M, Hampe J, Krawczak M (2005) Genetics of Crohn disease, an archetypal inflammatory barrier disease. Nature reviews Genetics 6: 376-388.
-
Hoshi N, Schenten D, Nish SA (2012) MyD88 signalling in colonic mononuclear phagocytes drives colitis in IL-10-deficient mice. Nat Commun 3: 1120.
-
Yamada T, Ichikawa H (1974) X-ray diagnosis of elevated lesions of the stomach. Radiology 110: 79-83.
-
Murchison C (1857) Cases of gastrocolic fistula with observations on its pathology, diagnosis, etc. Edin Med J 3: 4-21.
-
Sanderson F (1863) Duodenocolic fistula. Trans Path Soc Lond 14: 173-175.
-
Torrance B, Jones C (1972) Three cases of spontaneous duodeno-colic fistula. Gut 13: 627-630.
-
McKelvey ST, Carr D, Lesna M, Johnston ID (1975) Spontaneous duodenocolic fistula. J R Coll Surg Edinb 20: 54-57.
-
Narula A, McCormick JS (1990) Spontaneous duodenocolic fistula. J R Coll Surg Edinb 35: 253-254.
-
Sharma VK, Xie QY, Hassan HA, Howden CW (2002) Placement of a covered metal stent via gastrostomy for management of malignant duodenocolic fistula with duodenal obstruction. Gastrointest Endosc 55: 937-940.





