International Journal of Pathology and Clinical Research
Atypical Retinal Arterial Macroaneurysm
Hans Hoerauf1*, Philipp Steven2 and Nicolas Feltgen1
1Department of Ophthalmology, University of Göttingen, Germany
2Department of Ophthalmology, University of Cologne, Germany
*Corresponding author:
Hans Hoerauf, Department of Ophthalmology, University of Goettingen, Robert-Koch-Str. 40, 37075 Göttingen, Germany, Tel: + 0551 39 66768, E-mail: hanshoerauf@yahoo.com
Int J Pathol Clin Res, IJPCR-2-037, (Volume 2, Issue 2), Case Report; ISSN: 2469-5807
Received: March 30, 2016 | Accepted: May 20, 2016 | Published: May 25, 2016
Citation: Hoerauf H, Steven P, Feltgen N (2016) Atypical Retinal Arterial Macroaneurysm. Int J Pathol Clin Res 2:037. 10.23937/2469-5807/1510037
Copyright: © 2016 Hoerauf H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A patient with an atypical retinal arterial macroaneurysm masked by a persistent vitreous haemorrhage mimicking a neoplasm is presented. During vitrectomy a pigmented peripapillary tumour located at large vessels with circinate lipid exsudates was detected. Examination of removed tissue revealed haemosiderin-loaded macrophages resulting in pigmentation. The histologic finding of phagocytosis of intraretinal blood remnants allowed to diagnose an atypical retinal arterial macroaneurysm.
Keywords
Vitreous haemorrhage, Retinal arterial macroaneurysm, Pigmented tumour, Vitrectomy, Histology
Introduction
Vitreous haemorrhages mainly originate from ocular blood vessels involved in various pathologies such as proliferative diabetic retinopathy, neovascular complications in retinal vein occlusion, retinal tears, arterial macroaneurysms, trauma, intraocular tumour and others. Pathognomonic is the inability to visualize the cause of the haemorrhage by indirect ophthalmoscopy. The use of ultrasound is a useful tool to exclude an underlying retinal detachment but is not sensitive enough for differential diagnosis. Here we present a patient with a persistent vitreous haemorrhage based on an atypical arterial macroaneurysm that caused difficulties in intra- and post-operative diagnosis.
Patient
A 51-year-old female patient presented with a dense vitreous haemorrhage of her right eye. Visual acuity of the right eye was handmotions, visual acuity of the left eye was 20/20). The haemorrhage had persisted for 5 months without any signs of spontaneous resolution. General anamnesis revealed a suspected von-willebrand syndrome and dysfibrinemia that could not be confirmed by a current laboratory testing, no arterial hypertension or other systemic disease. Slit lamp investigation showed iris heterochromia with right eye involvement but no signs of inflammation, no rubeosis, a clear lens and red blood cells in the right vitreous. Indirect ophthalmoscopy of the left eye was unremarkable but was not possible on the right eye due to the dense vitreous haemorrhage. Ultrasound-B of the right eye disclosed a small tumour at the posterior pole close to the optic nerve, no retinal detachment. A pars plana vitrectomy was performed and during surgery a dark pigmented tumour was found at the upper arcade of the retinal blood vessels surrounded by a lipid circinate area extending towards the macula (Figure 1a and Figure 1b). Pigmented membranes were peeled of and prepared for histological examination. Light microscopy showed dense connective tissue strands with haemosiderin-loaded macrophages, the Berlin-blue demonstrated siderophages (Figure 2).
.
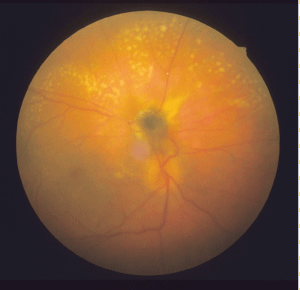
Figure 1a: Postoperative fundus photography of the right eye one week after vitrectomy due to vitreous haemorrhage showing a pigmented juxtapapillary tumour with associated epiretinal membrane, distortion of the upper vascular arcade and surrounding lipid exudates.
View Figure 1a
.
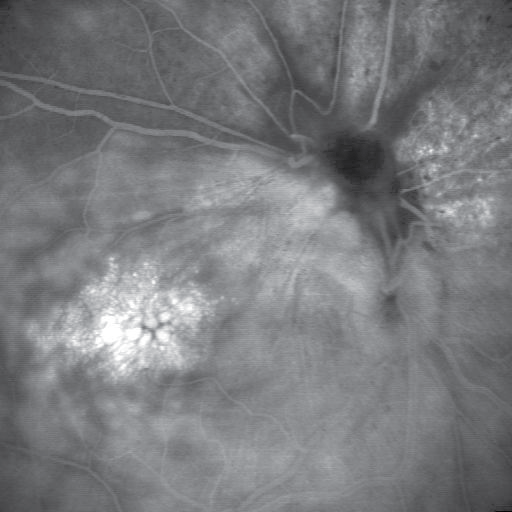
Figure 1b: Fluorescein angiography (late phase) demonstrates cystoid macular edema.
View Figure 1b
No other surgical maneuver was necessary. Postoperatively, fluorescein angiography was performed revealing a pigment-and exudate-related blockage and a distinct macular edema originating from the retinal tumour. No retinal telangiectasia were identified. Within a follow-up period of 12 months, the exudates resolved without further therapy and cystoid edema regressed slowly (Figure 3). The "tumour" showed no changes apart from a slight reduction in size and rounding regarding to size and location. VA increased to 20/60 at last follow up visit. Our patient refused further treatment to reduce macular edema.
.
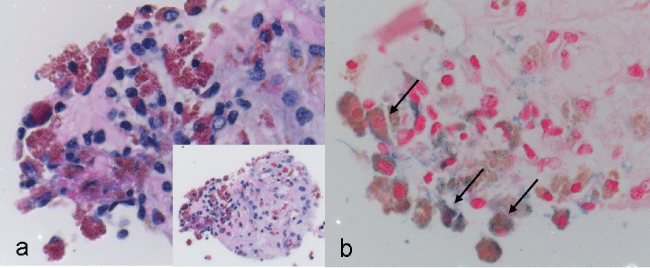
Figure 2a: Light microscopy (original magnification x40, PAS-staining) of the intraoperative specimen revealing macrophages that are loaded with haemosiderin (siderophages), fibroblasts, lymphocytes and connective tissue; Inset: overview (original magnification x20, PAS-staining), b: Berlin-blue reaction (original magnification x40) demonstrating siderophages (arrows).
View Figure 2
.
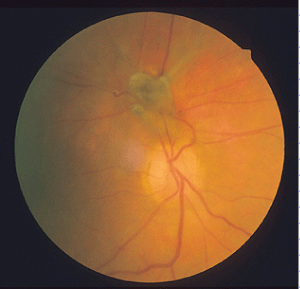
Figure 3: Postoperative fundus photography 12 months after vitrectomy (VA 20/60) with complete resolution of lipid exudates, the size and extent of pigmented lesion appearing unchanged.
View Figure 3
Discussion of Differential Diagnoses
Pigmented juxtapapillary tumours can cause difficulties in differential diagnosis and planning of the appropriate treatment. In particular the differentiation between benign and malignant pathologies is crucial. Benign pigmented retinal tumours include melanocytoma, reactive juxtapapillary proliferations of the pigment-epithelium and combined hamartoma of the retinal pigment epithelium [1]. Melanocytoma, are deeply pigmented hamartoma, that may grow extremely slow and rarely transform to malignant tumours. Typically, fluorescein angiography demonstrates a permanent hypofluorescence. Furthermore, the occurrence of vitreous haemorrhages is atypical. Reactive juxtapapillary proliferations of the retinal pigment epithelium (RPE) reveal finger-like processes along nerve fibers, grayish pigmentations and often an associated epiretinal membrane, but no exsudates. Often, recurrent inflammation or previous trauma is associated with juxtapapillary proliferation of the RPE. In combined hamartoma, peripapillary and in particular submacular RPE, the sensory retina and the adjacent vitreous are affected. Traction by the tumour leads to tortuositas of retinal blood vessels and puckering of the surrounding retina [1]. The tumour reveals a typical blue-greenish pigmentation, leakage from atypical capillaries in fluorescein angiography and proliferation of the RPE. In the presented case only vascular tortuositas and puckering of the retina was observed, but none of the other specific features were present.
Malignant melanoma of the choroid can also be the cause of a vitreous haemorrhage and therefore have to be included in differential diagnosis [2]. Absence of growth during further follow up, as well as the clinical and histological features in the presented case excluded a malignant melanoma.
Adenocarcinomas of the retinal pigment-epithelium are very rare pigmented tumours. Only two case reports have been published, demonstrating the formation of an adenocarcinoma on the basis of a congenital hyperplasia of the retinal pigment-epithelium (CHRPE) [3,4]. Again the clinical and histological findings are different from our case as no malignant cells were found.
Also an undetected foreign body is able to induce a pigmented lesion [5], but no trauma was stated in the case history as mentioned above.
As a further differential diagnosis a parapapillary choroidal neovascularisation (CNV) with vascular leakage has to be considered. A CNV could have caused subretinal bleeding which is able to penetrate through the retina, thereby leading to vitreous haemorrhage. Due to missing age-related changes such as drusen, lack of causes for a secondary CNV and angiographic findings this diagnosis was also unlikely.
The location of the tumour at large retinal blood vessels, lipid circinate exudates and the histological finding with phagocytosis of intraretinal blood remnants by macrophages militate in favour of an retinal arterial macroaneurysm [6]. However, arterial hypertension as a frequent risk factor was not present. Macroaneurysms on the optic disc were reported associated with congenital retinal arterial malformation [7]. Acute rupture of a retinal macroaneurysm with subsequent vitreous haemorrhage is a typical event, sometimes associated with subretinal or intraretinal bleedings or a multilayered haemorrhage [8]. Usually, the macroaneurysm itself can be clearly recognized as a prominent vessel convolute. They may spontaneously regress, leak or bleed. If the fovea is threatened or involved by leakage laser coagulation is a therapeutic option. Pigmented appearance is atypical causing clinical uncertainty in the presented patient.
Conclusion
We present a patient with persistent haemorrhage originating from a pigmented peripapillary tumour. Analysis of histological specimen revealed haemosiderin-loaded macrophages resulting in pigmentation. Thereby, the diagnosis of retinal arterial macroaneurysm was confirmed.
References
-
Laqua H, Wessing A (1979) Congenital retino-pigment epithelial malformation, previously described as hamartoma. Am J Ophthalmol 87: 34-42.
-
Shields CL, Shields JA (2001) Subretinal hemorrhage from a retinal arterial macroaneurysm simulating a choroidal melanoma. Ophthalmic Surg Lasers 32: 86-87.
-
Fan JT, Robertson DM, Campbell RJ (1995) Clinicopathologic correlation of a case of adenocarcinoma of the retinal pigment epithelium. Am J Ophthalmol 119: 243-245.
-
Trichopoulos N, Augsburger JJ, Schneider S (2006) Adenocarcinoma arising from congenital hypertrophy of the retinal pigment epithelium. Graefes Arch Clin Exp Ophthalmol 244: 125-128.
-
Lipper S, Eifrig DE, Peiffer RL, Bagnell CR (1981) Chorioretinal foreign body simulating malignant melanoma. Am J Ophthalmol 92: 202-205.
-
Rabb MF, Gagliano DA, Teske MP (1988) Retinal arterial macroaneurysms. Surv Ophthalmol 33: 73-96.
-
Aumiller MS, Rinehart J (2015) Multi-layered haemorrhage secondary to retinal arterial macroaneurysm: a case report and review. Clin Exp Optom 98: 117-121.
-
Ichibe M, Oya Y, Yoshizawa T, Abe H (2004) Macroaneurysm on the optic disk associated with congenital retinal arterial malformation. Retina 24: 985-986.





