International Journal of Pathology and Clinical Research
Orbital Necrobiotic Xanthogranuloma: A Case Report
Hind M. Alkatan1* and Abdul Elah A. Al-Abdullah2
1King Saud University, College of Medicine, Department of Ophthalmology, Saudi Arabia
2King Khaled Eye Specialist Hospital, Uveitis Division, Saudi Arabia
*Corresponding author:
Dr. Hind Alkatan, Assistant Professor, Director of KSU Post Graduate Residency and Fellowship Training Programs in Ophthalmology, Ophthalmology Department, College of Medicine, King Saud University, Saudi Arabia, Tel: No: +966 504492399, Fax: +966112052740, E-mail: hindkatan@yahoo.com, hkatan@ksu.edu.sa
Int J Pathol Clin Res, IJPCR-1-016, (Volume 1, Issue 1), Case Report; ISSN: 2469-5807
Received: November 02, 2015 | Accepted: December 21, 2015 | Published: December 24, 2015
Citation: Alkatan HM, Al-Abdullah AEA (2015) Orbital Necrobiotic Xanthogranuloma: A Case Report. Int J Pathol Clin Res 1:016. 10.23937/2469-5807/1510016
Copyright: © 2015 Alkatan HM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Xanthogranulomatous ocular and periocular lesions in adults have been reported in 3 main forms: adult-onset xanthogranuloma (AXG), necrobiotic xanthogranuloma (NXG), and Erdheim-Chester disease. The three forms differ in regards to laterality, systemic associations, and prognosis. NXG is a rare chronic progressive disease considered to be systemic with mostly asymptomatic internal organ involvement. Ophthalmic manifestations include conjunctival, corneal and scleral involvement. We are presenting a case of NXG with initial presentation as bilateral scleritis and eventual posterior eye and orbital involvement resulting in loss of vision and exenteration. The diagnosis of NXG was not made until 28 years following her initial presentation.
Keywords
Scleritis, Necrobiotic xanthogranuloma, Wegener's Granulomatosis
Abbreviations
AXG: adult onset xanthogranuloma, NXG: necrobiotic xanthogranuloma, WG: Wegener's granulomatosis, TB: Tuberculosis, ANA: Anti-nuclear antibody, ANCA: Anti-neutrophil cytoplasmic antibody
Introduction
Xanthogranulomatous lesions can affect adults under 3 conditions: (1) AXG, which is often associated with hematological disorders (such as anemia, thrombocytopenia, or eosinophilia) and can present with unilateral ocular/periocular involvement, (2) NXG, which is often associated with paraproteinemia, myeloma, or lymphoproliferative disorders and shows bilateral ocular/periocular involvement, and (3) Erdheim-Chester disease, which is associated with wider systemic involvement including vital organs resulting in death and typically shows posterior orbital involvement [1].
We are presenting a unique case that initially presented with bilateral necrotizing scleritis and mild left upper lid swelling. The disease progressed despite her treatment to involve the posterior aspect of the left globe and orbit within 1 year. The patient eventually lost vision in that eye and her exenteration specimen was diagnosed as Wegener's Granulomatosis (WG). The final accurate diagnosis of NXG was made upon the review of her clinical and histopathological features 28 years later.
The case
A 50-year-old female patient presented in June 1987 with bilateral redness in her eyes of uncertain duration. Ophthalmic examination at that time showed visual acuity (VA) of 20/100 on the right and 20/60 on the left. Her intraocular pressure (IOP) was normal in both eyes (15 mmHg on the right and 12 mmHg on the left). Anterior segment examination showed bilateral conjunctival injection, peripheral thinning of both corneas with no evidence of infiltrate, scleral thinning with active necrosis, and focal areas of uveal show. The anterior chamber in both eyes was deep and quiet with normal iris and equal pupils. The lens showed + 2 nuclear sclerosis in both eyes. External examination was normal on the right and only showed mild upper lid swelling on the left. No skin lesions were observed at that time. Fundus examination was normal in both eyes with flat retina and healthy optic disc.
The diagnosis of bilateral necrotizing scleritis was made and she was started on topical medications in the form of lubricating eye drops, and prednisolone acetate eye drops, OU. Systemic medications included: oral Prednisone 60 mg once daily and Chlorambucil 4 mg once daily. 6 months later, she started to show bilateral limbal infiltrate with non-resolving scleral necrosis and melting.
She was kept on oral Prednisolone maintenance dose of 5 mg once daily, Cyclosporine 70 mg twice a day, and Indomethacin 25 mg 3 times daily in addition to topical corticosteroid drops. She was suspected clinically to have WG. In December 1988, the patient presented with gradual deterioration of her vision to counting fingers near the face on the left. The examination of that eye showed significant increase in her cataractous lens changes, exudative retinal detachment involving the macula, and choroidal effusion. She also had 4 mm of axial proptosis on the left (measured by Hertel exophthalmometer at base of 100) and limitation of extra ocular motility. The left eye later showed hypotony with further reduction of vision to light perception despite treatment with cyclophosphamide. The eye was enucleated with reconstruction of her left socket using skin flap. Further investigations, revealed negative ANA, rheumatoid factor, TB/syphilis screening, and positive ANCA. She was treated with cyclophosphamide pulse therapy 15 mg per kg (1 g IV). The patient developed staph epidermidis infection of her left socket with necrosis of the skin flap. She eventually underwent left exenteration in July 1993 with the histopathological diagnosis of WG. Her right eye was stabilized, underwent cataract extraction with 10L implantation, and had uncorrected VA of 20/125.
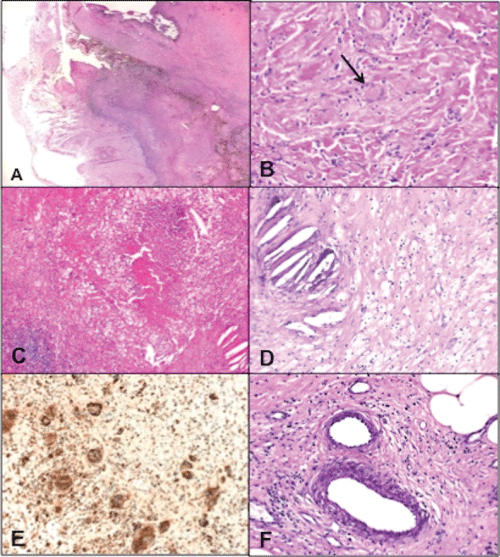
The enucleation and the exenteration histopathological slides were reviewed in 2015 as part of a retrospective project on WG. The skin and orbital tissue showed granulomatous reaction consisting of epithelioid cells, and several multi-nucleated giant cells including both foreign-body type as well as rare Touton giant cells. Areas of lymphocytic infiltrate with occasional germinal centers were also present. Broad zones of sclerotic necrobiosis and cholesterol clefts were observed. The macrophages were CD68 positive while negative to S-100 protein and CD1a stain (Figure 1).
.
Figure 1: (A) Histopathologic appearance of the enucleated blind globe showing posterior scleritis and retinal detachment (Original magnificationX25 Hematoxylin & Eosin); (B) Touton giant cell (black arrow) in the retrobulbar tissue of the enucleation specimen (Original magnificationX400 Hematoxylin & Eosin); (C) Area of necrobiosis, foamy histiocytes & giant cells in the exenteration orbital tissue (Original magnificationX100 Hematoxylin & Eosin); (D) Higher power of the same area showing cholesterol clefts and foamy histiocytes (Original magnificationX200 Hematoxylin & Eosin); (E) Orbital Granulomatous inflammation with histiocytes and Giant cells (Original magnification X400 CD68); (F) Example of a blood vessel with no evidence of true vasculitis (Original magnificationX400 Hematoxylin & Eosin).
View Figure 1
The diagnosis of NXG was made and the patient's clinical course was reviewed. However, we were unable to get information apart from the fact that she passed away in 1994 with no available details on the direct cause of her death at the time of this report.
Discussion
Xanthogranulomatous lesions can involve the ocular and periocular tissue in adults in 3 forms AXG, NXG and Erdheim-Chester disease. The later typically involves the posterior aspect of the orbit and is considered lethal due to widespread systemic involvement of vital organs. On the other hand, AXG and NXG tend to present with eyelids and/or anterior orbital involvement [1]. In a retrospective case series including 6 patients with xanthogranulomatous lesions, it has been emphasized that AXG and NXG are 2 distinct entities. AXG can be unilateral in presentation with no tendency for neoplastic disease while NXG is bilateral and shows necrosis and more profound systemic manifestations [1]. Even in the absence of the typical periocular skin lesions, other ophthalmic manifestations of NXG can occur such as severe scleritis [2].
NXG is a rare chronic progressive multi-organ disease of adults with no sex predilection. The average age of onset is reported to be in sixth decade [2]. It NXG was initially described in 1980 and is now considered a systemic disease with internal organ involvement including spleen, heart, lung, kidney, and central nervous system. This organ involvement is asymptomatic in most cases, and possibly established by post mortem tissue diagnosis [3,4].
The exact pathogenesis of NXG is still unclear, although several theories have been raised relating NXG to increased serum levels of immunoglobulin, presence of monoclonal paraprotein, ischemia, and infection such as Borreliosis [2,5]. Skin lesions on the face (including periorbital areas), extremities, or trunk clinically characterize NXG. Periorbital edema due to xanthomatous inflammation of anterior orbital tissue and sub cutis may also occur [4,6]. This was observed in our patient at her initial presentation but was overlooked due to the absence of the skin lesions.
Ophthalmologic manifestations other than the typical periorbital skin xanthelasma-like lesions are seen in 50-80% of cases including: subconjunctival masses, keratitis, episcleritis, scleritis, and uveitis [4]. Severe scleritis such as in our case has been often reported with posterior involvement [2,7].
In cases of with posterior scleritis, other intraocular manifestations can be observed such as choroidal folds, optic disc edema, retinal striae and subretinal fluid with leakage at the choroidal level [2,7]. Our patient developed choroidal effusion and exudative retinal detachment 18 months following her initial presentation.
The most important systemic associations are the hematologic and lymphoproliferative disorders including lymphomas, leukemia, myelodysplastic syndrome, and macro-globulinemia. Although 80-90% of cases will show monoclonal gammopathy, only 10% will develop multiple myeloma [6]. The development of multiple myeloma has been reported to occur as late as 20 years after the onset of NXG [8].
Clinical correlation is of vast importance to make the diagnosis of NXG, especially, in the absence of periocular skin involvement and tissue diagnosis. The presence of paraproteinemia helps reach the diagnosis [2,3].
The histopathological features help in differentiating NXG from other granulomas and xanthomatous lesions where large broad areas of necrobiosis are observed in addition to the Touton giant cells and the cholesterol clefts [4]. These were all evident in our reviewed histologic slides of the left exenteration specimen. On the other hand, WG is an immune-mediated necrotizing, granulomatous vasculitis that has a clinical predilection to involve the upper airways, lungs, and kidneys. Eye involvement in this condition similarly includes conjunctivitis, episcleritis, scleritis, sclerouveitis, and retro-orbital involvement with the possibility of relapse after systemic control of the disease [9]. The histopathological features include necrotizing granulomatous inflammation and pauci-immune vasculitis in small- and medium-sized blood vessels. The vascular involvement aids in the diagnosis with very characteristic granulomatous vasculitis and disruption of the elastic laminae (in early lesions) and outlining the vessel wall (in advanced lesions), however this is not always present. The diagnostic extra-vascular lesions show necrotizing inflammation and ulceration with occasional multinucleate giant cells. The fully developed palisading granuloma, the hallmark of WG, shows a stellate focus of necrosis with either fibrinoid material or an aggregate of neutrophils and neutrophil debris, surrounded by a palisade of macrophages [8-10].
Treatment of NXG is mainly by systemic alkylating agents such as cyclophosphamide with or without systemic corticosteroid. Systemic chemotherapy for associated hematologic malignancies has beneficial effect even on skin lesions in few cases [11,12]. Intralesional triamcinolone acetonide has been also recommended for eyelid and anterior orbital lesions, with variable effect [1,13]. Tissue diagnosis of suspicious periocular lesions is recommended to establish the diagnosis as early as possible even if the risk of wound complications is increased [13]. Our patient was treated with cyclophosphamide and oral steroids but her scleritis progressed on the left with loss of that eye.
In conclusion, ophthalmologists and ophthalmic pathologists should be aware of the ophthalmological manifestations of NXG and the diagnostic features of this entity to allow the differentiation of this disease from other granulomatous conditions. The early diagnosis will aid in proper tailoring of the treatment plan to avoid loss of vision due to the progressive nature of this disease.
Ethical Statement
This case report is approved by the Research Department at KKESH (Project #: RP-15106-CR). The authors have no conflict of interest or financial issues to be disclosed in relation to this report.
References
-
Elner VM, Mintz R, Demirci H, Hassan AS (2005) Local corticosteroid treatment of eyelid and orbital xanthogranuloma. Trans Am Ophthalmol Soc 103: 69-73.
-
Peyman A, Walsh N, Green P, Dorey MW, Seamone C, et al. (2012) Necrobiotic xanthogranuloma associated with necrotizing scleritis. Am J Dermatopathol 34: 644-647.
-
Kossard S, Winkelmann RK (1980) Necrobiotic xanthogranuloma with paraproteinemia. J Am Acad Dermatol 3: 257-270.
-
Inthasotti S, Wanitphakdeedecha R, Manonukul J (2011) A 7-Year History of Necrobiotic Xanthogranuloma following Asymptomatic Multiple Myeloma: A Case Report. Dermatol Res Pract 2011: 927852.
-
Zelger B, Eisendle K, Mensing C, Zelger B (2007) Detection of spirochetal micro-organisms by focus-floating microscopy in necrobiotic xanthogranuloma. J Am Acad Dermatol 57: 1026-1030.
-
Ugurlu S, Bartley GB, Gibson LE (2000) Necrobiotic xanthogranuloma: long-term outcome of ocular and systemic involvement. Am J Ophthalmol 129: 651-657.
-
Wilhelmus KR, Yen MT, Rice L, Font RL (2006) Necrobiotic xanthogranuloma with posterior scleritis. Arch Ophthalmol 124: 748.
-
Lam K, Brownstein S, Jordan DR, van der Jagt R, Jastrzebski A, et al. (2013) Bilateral necrobiotic xanthogranuloma of the eyelids followed by a diagnosis of multiple myeloma 20 years later. Ophthal Plast Recostr Surg 29: e119-20.
-
Gioacchino LC, Passantino R, Bono L, Tortorici C, Farrantelli A, et al. (2013) Clinical and histological features in Wegener Granulomatosis. American Journal of Medical Sciences and Medicine 1.1: 1-4.
-
Cuende E, Mena AR, Andonegui J, Minguela I, Vesga JC (2001) Ocular involvement in Wegener's granulomatosis responding to intravenous cyclophosphamide. Rheumatology (Oxford) 40: 1066-1068.
-
Mohsenin A, Sinard J, Huang JJ (2012) Necrobiotic xanthogranuloma and chronic lymphocytic leukemia of the conjunctiva masquerading as scleritis and uveitis. Clin Ophthalmol 6: 2045-2047.
-
Robertson DM, Winkelmann RK (1984) Ophthalmic features of necrobiotic xanthogranuloma with paraproteinemia. Am J Ophthalmol 97: 173-183.
-
Codere F, Lee RD, Anderson RL (1983) Necrobiotic xanthogranuloma of the eyelid. Arch Ophthalmol 101: 60-63.





