International Journal of Oral and Dental Health
Early Prosthetic Treatment of Children with Hypohidrotic Ectodermal Dysplasia: Six Case Reports
Sijie Li†, Xue Xiao†, Ruixue Wu, Binghui Zeng, Dongsheng Yu* and Wei Zhao*
Guanghua School and Hospital of Stomatology, Guangdong Provincial Key Laboratory of Stomatology, Sun Yat-sen University, Guangzhou, China
†These authors contributed equally to this work
*Corresponding author:
Dong-sheng Yu and Wei Zhao, Guanghua School and Hospital of Stomatology, Guangdong Provincial Key Laboratory of Stomatology, Sun Yat-sen University, Ling Yuan Road West No. 56, Guangzhou, Guangdong Province 510055, China, Tel: +86-20-8386-2543, +86-20-8386-2553, Fax: +86-20-8382-2807, E-mails: yudsh@mail.sysu.edu.cn; zhaowei3@mail.sysu.edu.cn
Int J Oral Dent Health, IJODH-3-039, (Volume 3, Issue 1), Research Article; ISSN: 2469-5734
Received: October 09, 2016 | Accepted: February 10, 2017 | Published: February 14, 2017
Citation: Li S, Xiao X, Wu R, Zeng B, Yu D, et al. (2017) Early Prosthetic Treatment of Children with Hypohidrotic Ectodermal Dysplasia: Six Case Reports. Int J Oral Dent Health 3:039. 10.23937/2469-5734/1510039
Copyright: © 2017 Li S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Hypohidrotic ectodermal dysplasia (HED) is a rare hereditary disorder characterized by defects of two or more ectodermal structures. Partial or complete absence of deciduous and permanent dentition is one of the more frequently occurring oral symptoms; a few teeth may be present but with conical shape. Other oral symptoms include decreased salivary secretion and atrophic alveolar ridge. Thus, the prosthetic treatment of HED, especially for the young kids is still a big challenge for the pediatric dentists. Here we described a series of the prosthetic treatments of six young boys (aging from 4 to 8 years) with HED using removable partial dentures and complete dentures. The strategy of prosthetic treatment was made on the basis of their age, the development of dentition and jaw. In the removable denture, to promote the partially erupting teeth to erupt, the Intaglio surface of the denture was trimmed out in the path of teeth's eruption. The soft liner materials were inserted into the denture with a thickness of one millimeter to reduce the growth inhibition of the jaw and increase the retention and stability of denture. And all children were followed up in our clinic every three months to modifications and/or replace the denture to avoid possible complications might resulting from the jaw growth. Our four-year experience confirms that a perfect treatment plan helps to promote the vertical dimension, esthetics, functioning of the stomatognathic system and the growth of the jaw, also to improve the speech ability and masticatory efficiency.
Keywords
Early prosthetic treatment, Hypohidrotic ectodermal dysplasia, Anodontia or Oligodontia, Removable prosthesis, Denture liner
Introduction
Ectodermal dysplasia (ED) is a rare hereditary disorder characterized by defects of 2 or more ectodermal structures, including teeth, nails, hair and sweat glands [1,2]. Hypohidrotic ectodermal dysplasia (HED), with a prevalence of approximately one per 100000 births, is the most frequently reported type of ED. HED phenotype is resulted from the mutation in the genes that encode ectodysplasin A (EDA), EDA receptor (EDAR), EDA receptor-associated death domain (EDARADD), and WNT10 and thus it can be inherited in an X-linked (XL) recessive, autosomal recessive (AR), or autosomal dominant (AD) manner [1,3,4]. So far, most cases are X-linked disease and caused by mutations in the gene EDA, which located at Xq12-q13.1 and produces EDA [3,4]. EDA, normally expressed in ectodermal tissues such as keratinocytes, hair follicles, and sweat glands, seems to play an important role as a signaling molecule mainly during fetal and neonatal development. So far, more than 100 mutations in the EDA associated with HED had been reported [1,3]. HED mainly affects males, whereas females are mainly carriers [3,4].
For HED patients, partial or complete absence of deciduous and permanent dentition is one of the most frequently occurring oral symptoms, and a few teeth may be present but with conical shape and widely spaced, which contributes to poor masticatory efficiency [3,5,6]. Other oral symptoms include decreased salivary secretion, with the mucous membranes often appearing dry. Common facial manifestations include prominent forehead, "saddle" nose, retrusive maxilla, and protuberant mandible [7-9]. Without the functional stimulation of chewing, the growth of jaw would be impaired, leading to decreased alveolar bone volume and thin alveolar ridge [10].
Based on the literature, 2 to 3 years old is recommended as the ideal timing to undertake early prosthetic treatment for HED patients [11,12]. Early prosthetic treatment in HED patients makes it possible to have good masticatory function, normal temporomandibular joint function, and to avoid social problems, particularly in young patients. However, it is a major challenge for the dental professional to make a treatment plan for HED children.
We present six children with HED aging from 4 to 8 and delineate the progression of the early prosthesis treatment for them, and propose a follow-up protocol to modify the denture and assess changes in the jaw, weight and disposition.
Case Reports
Patients
The patients were referred from the Guanghua School of Stomatology, Sun Yat-sen University, with a chief dental complaint of anodontia or oligodontia at birth. They reported difficulty with mastication and speech due to the presenting complaint. All patients were diagnosed with HED, based on the presence of sparse hair, hypoplasia of sweat gland and anodontia or oligodontia.
Extraoral examinations revealed the remarkable findings, included prominent forehead, "saddle" nose, retrusive maxilla and protuberant mandible and decreased vertical dimension.
Panoramic radiography examination was finished to determine the germ of the tooth, the underdevelopment of residual ridge, crown root ratio (CRR) and root length.
Case 1
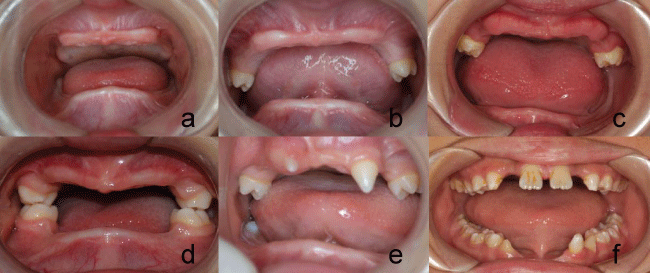
Male, five-years-old, oral examination showed typical features including complete absence of the deciduous teeth (Figure 1a). Panoramic radiograph demonstrated the absence of all germs but the tooth germs of left first molar of the maxilla in the edentulous area (Figure 2a).
.
Figure 1: a) Case 1 Pre-treatment-frontal view; b) Case 2 Pre-treatment-frontal view; c) Case 3 Pre-treatment-frontal view; d) Case 4 Pre-treatment-frontal view; e) Case 5 Pre-treatment-frontal view; f) Case 6 Pre-treatment-frontal view.
View Figure 1
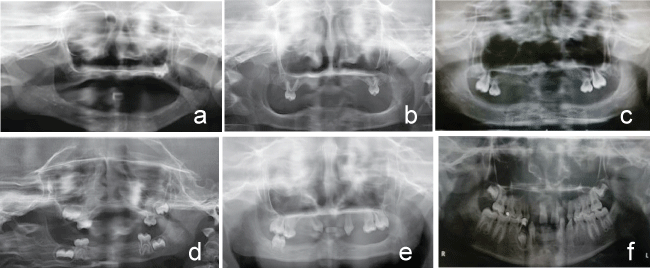
.
Figure 2: a) Case 1 Pre-treatment-panoramic radiograph view; b) Case 2 Pre-treatment-panoramic radiograph view; c) Case 3 Pre-treatment-panoramic radiograph view; d) Case 4 Pre-treatment-panoramic radiograph view; e) Case 5 Pre-treatment-panoramic radiograph view; f) Case 6 Pre-treatment-panoramic radiograph view.
View Figure 2
Case 2
Male, four-years-old, oral examination showed that no deciduous teeth were present except for the second deciduous molars in the upper arch, which were in conical shape (Figure 1b). Panoramic radiograph confirmed the clinical examination and depicted that the CRR of deciduous molars was 2:3 without absorption of root and no other tooth germ existed (Figure 2b).
Case 3
Male, six-years-old, oral examination revealed that only the right first molar and the second deciduous molars were present in the maxilla and that right first molar was only partially erupted (Figure 1c). Panoramic radiograph revealed that the roots of the deciduous molars had absorbed to the midpoint and that the germ of left first molar was in good development (Figure 2c).
Case 4
Male, five-years-old, oral examination showed that only four deciduous second molars were present with normal shape (Figure 1d). Panoramic radiograph noted that the four permanent molar germs were developing well and that the CRR of deciduous molars was 2:3 without absorption of root and no other tooth germ existed (Figure 2d).
Case 5
Male, eight-years-old, oral general examination showed oligodontia characterized by the presence of canines and first molars and second deciduous molars in the maxilla and right first molar in the mandible. The right canine was mesially inclined and partially erupted with only 1/4 of its anatomical crown visible. In addition, all teeth had a conical shape (Figure 1e). Panoramic radiograph shared the partial formation of the roots of permanent teeth and revealed that the CRR of deciduous molars was 2:3 without absorption of root and no other germ existed (Figure 2e).
Case 6
Male, nine-years-old, oral general examination showed the absence of maxillary lateral incisors and mandibular incisor, while all canines and mandibular first left premolar were in conical shape and partially erupted (Figure 1f). Panoramic radiograph showed the tooth germs of second molars in both arches, and the first right premolar in the mandible were in optimal development and no other germ existed (Figure 2f).
Method and Result
A treatment plan was formulated for the children and then each patient was provided with a set of personalized dentures according to the examination. The importance of oral hygiene and follow-up was stressed.
Obtainment of master cast
Preliminary impressions were taken using stock mental trays. They were then used to construct primary study models. Then custom trays were fabricated using self-cure poly methyl methacrylate (PMMA) resin. The master impressions were taken using irreversible hydrocolloid (dental alginate, Heraeus Kulzer). These were then used to construct master casts.
Record of maxillomandibular relationship
Metal frameworks were fabricated to improve the strength of the denture. The molars that were fully erupted bilaterally (as in case 2, 3 and 4) were included in the overall denture design and wire clasps were fitted on to improve the retention of denture.
Since the occlusal vertical dimension (OVD) of cases 4, case 5 and case 6 were normal, no changes were made to their OVD. Instead, the maxillomandibular relationship was duplicated. The optimal OVD of other patients were established by evaluating the height from nose tip to glabellum, swallowing, and phonetics. The record base and record rim were fabricated and used for the maxillomandibular relationship record. Then both casts were oriented on a semi adjustable articulator along with a face bow record.
Teeth arrangement
Artificial teeth should be placed in an accurate position in order to satisfy the aesthetic and functional needs. And functional need is much important when arranged the posterior teeth, while aesthetic need should be considered more when anterior teeth were positioned.
It should be stressed that the artificial teeth should be arranged in the accurate position in the perpendicular direction and horizontal direction to acquire adequate stability. Semianatomic acrylic deciduous teeth (20-degree cusp angle) were fabricated. The buccolingual diameter of the posterior teeth was decreased to reduce the lateral forces. In the horizontal direction, the teeth were set following the Monson curve and Spee's curve to obtain balanced occlusion. The occlusal plane should be parallel to the alveolar ridge and the height of the occlusal plane was kept at the 1/2 to 2/3 of the retromolar pad. In the perpendicular direction, the anteroposterior central groove of the teeth was positioned over a line drawn along the crest or centre of the lower ridge to reduce the lateral forces. What's more, lingualized occlusion was selected to preserve the abutment teeth, minimize lateral forces and create freedom of movement.
Relining of denture
To improve the stability and comfort of the denture, soft liner materials were implemented to reline the denture. Usually, the upper and lower dentures should be relined separately. Firstly, approximately 1 mm thickness of materials were relieved from the Intaglio surface of upper denture base to obtain the space for soft liner materials with exception of the regions ahead of the retromolar pad and canines to provide a vertical stop. The soft liner materials (Silagum comfort soft relining, DMG) were then loaded into the denture and the denture were seated carefully. The materials were then border moulded in rapid succession. Then the patient was asked to keep still in the centric position. When the materials had set, the denture would be removed from the mouth. Then the same procedure was followed for the lower denture (Figure 3).
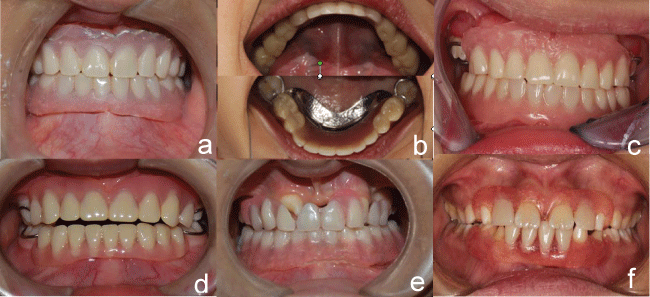
.
Figure 3: a) Case 1 Post-treatment-frontal view; b) Case 2 Post-treatment-occlusal view; c) Case 3 Post-treatment-frontal view; d) Case 4 Post-treatment-frontal view; e) Case 5 Post-treatment-frontal view; f) Case 6 Post-treatment-frontal view.
View Figure 3
Special procedure for case 5
For case 5, special procedure was carried out by trimming the Intaglio surface of the denture in the path of teeth's eruption (Figure 3e).
Final procedure
The buccal side of polished surface was covered with a thin layer of PMMA resin to improve the smoothness and to increase the adhesion area. Occlusal errors were then identified and corrected by selective grind. The tissue surface was finished and polished thoroughly. Then, the dentures were inserted.
Postoperative preparation
Fluoride therapy was given to protect the remaining dentition.
Follow-up
The denture may make the child feel sick, if it did happen, the parents or guardians were taught to learn to keep the denture in the mouth for a short time at first and extend the time gradually or wear the upper denture only and wear both dentures later on. The parents or the guardians were recommended to take day-to-day childcare and make a return visit whenever the child felt uncomfortable.
We relined or remade the denture regularly. The relining of denture was determined by the growth of jaw, the development of the tooth and the property of soft liner materials. Usually, the denture was relined every six months. Also, in order to not restrict the eruption of the teeth, the denture would be relined or remade if there were any partially erupted teeth.
All patients were followed-up in our clinic every three months. During the follow-up period, patients and their parents or guardians responded positively by stating the denture is comfortable and the masticatory efficiency was significantly enhanced. To date, the patient has worn the denture for 1-4 years and reported no complications.
Other medical orders
1. Stay in the cool environment in the daily life, and avoid high-level physical activity.
2. Drink more water.
3. Daily bathing with "superfatted" soap followed by the use of moisturizing lotions/creams.
4. Use sunscreen with a moisturizing base when exposed to the sun.
Discussion
For HED patients, partial or complete absence of deciduous and permanent dentition is one of the most frequently occurring oral symptoms. Early prosthetic treatment in HED patients makes it possible to obtain satisfactory masticatory function, normal temporomandibular joint function, and to avoid social problems, particularly in young patients. Therefore, it is recommended that early prosthetic treatment for HED patients should be carried out when the patient is 2 to 3 years old [12]. And for those who are not able to cope with the procedure, some researchers have advocated that the treatment should be fulfilled under general anaesthetic or sedation. However, others argue that the emotion of the patient must be taken into consideration during the entire procedure and that the success of the treatment depends mainly on the patient's cooperation in daily life rather than in the clinic [13]. In our study, the patients' ages ranged from 4 to 8 years old when they visited our clinic and hence missed the best treatment timing. It may be because that most parents didn't have an idea about the importance of the early prosthetic treatment.
To avoid restricting the development of the jaw and the dentition, removable denture, including complete denture (CD), removable partial denture (RPD) and overlay denture, were selected as a chief method. And the remaining teeth are important factors to consider as there is an obvious relationship between the retention and stability of denture and remaining teeth [14]. In this study, the extraction of the malformed tooth (permanent tooth and deciduous tooth) is not approved unless the tooth is worthless. Compare to the tooth extraction, a well-prepared tooth could decreases the resorption of residual ridges and makes the RPD or overlay denture possible, which is considered as prior choice [15,16]. Moreover, the present study indicated that the deciduous teeth which without replaced permanent teeth had a tendency to stay more than 30 years. Although multiple of teeth are of conical shape and in ectopic eruption, much treatments can still be done to make good use of them, such as orthodontic and crown restoration [17]. On the other hand, as much as the research has mentioned, the loss of the abutment teeth were mainly due to the caries and the periodontal diseases, which will seriously affect the retention of the RPD [18]. Whilst the salivary secretory levels decrease, the risk of caries may increase after the denture use. Thus, fluoride therapy was much important to protect the remaining teeth. In this study, considering the cooperation of kid patients, no crown restoration or orthodontic was made, instead, fluoride therapy was selected to protect the patients' teeth.
The property of weak flexural strength is often the reason that caused the PMMA not fitting well with the oral tissue, which may result in the poor distribution5 of the masticatory force. And it is associated with local tenderness and thus may accelerate the resorption of the residual ridge [19]. Thus, in this study, we chose the silicone-based materials, one kind of relining materials to reline the denture. As we know, compared with PMMA, soft liner materials can theoretically distribute and absorb forces on the denture bearing area with a cushioning effect and improve denture stability and comfort, thus enhancing masticatory function [19-21]. It also has a healing effect to the mucosa and as a result, gives comfort to the patients [22]. There are two kinds of soft liner materials that had been frequently used to reline the denture, included the soft acrylic materials and the silicone-based materials. The soft acrylic materials show viscoelastic behaviour and may become hard as time passes by, so it is usually recommended as treatment liner [23,24]. While silicone-based materials show elastic behaviour and had no cytotoxic effects on the epithelial cells or gingival fibroblasts, so it is more likely to be used as permanent liner [23,25].
Although some research indicated that a thickness of 2 mm of soft lining materials would be beneficial to patients with a thin residual ridge in maintaining retention and stability [26,27]. Other research indicated that a thickness of silicone soft liner varying from 0.5 mm to 2 mm does not influent the rate of adhesive failure between the denture base resin and the silicone soft liner [28]. Since the dentures in our patients are smaller than adults, the thickness of the denture that had been trimmed was about 1 mm.
Bond strength is another reason that causes adhesive failures, therefore, give a chance for microorganism to gather together [26]. In order to prevent it from happening, the adhesive area should be increased. Some reports have suspected that soft liner materials may increase the risk of denture stomatitis, which was believed most likely due to the accumulation of C. albicans. Statistically significant differences were observed between rough surfaces and smooth surfaces, implying that smooth surfaces are an essential factor to avoid denture stomatitis [29]. Therefore,we especially stressed the importance of finishing the denture. Regular follow-ups also decrease the risk of denture stomatitis. The soft liner materials were replaced every six months, in order to maintain the good properties of the materials.
Implant supported denture have been recommended as the best method to restore the dentition. However, higher risk has also been authenticated in early implant, as the implants placed in growing alveolar ridge have a tendency to stay still and remain ankylosed or become submerged with the sustained growth of the alveolar ridge and the continued eruption of neighbouring natural teeth [13,30]. The implant can also have a negative effect on children's craniofacial growth [12]. The combination of the rigid body of implant and rigid prosthesis may further restrict the development of the jaw, especially when the rigid prosthesis is positioned across the midline [30]. Therefore, it is recommended to wait until the cessation of growth. In recent years, some investigators have advocated to implant at 14-15 years old for girls and 16-years-old for boys or later [13].
Conclusion
HED patients often exhibit problems such as physical appearance, mastication and speech, all of which contribute to poor self-image. And the prosthetic treatment in HED children is challenging. Our four-year experience with the use of removal partial and complete dentures confirms that a perfect treatment plan should consider the child's age, the development of the stomatognathic system, degree of malformation of teeth, especially those that were partially erupting, as well as the property of the materials. Early prosthetic treatment is a chance to improve the esthetics, the function of the stomatognathic system and optimizes social integration.
Funding Support
Source of funding: This research is supported by the National Natural Sciences Foundation of China (No. 81472526) and by the Natural Sciences Foundation of Guangdong, China (No. 2014A030313126) and by the Science and Technology Program of Guangzhou, China (No.201609010015). The authors declare no potential conflicts of interest with respect to the authorship and/or publication of this article.
References
-
Cluzeau C, Hadj-Rabia S, Jambou M, Mansour S, Guigue P, et al. (2011) Only four genes (EDA1, EDAR, EDARADD, and WNT10A) account for 90% of hypohidrotic/anhidrotic ectodermal dysplasia cases. Hum Mutat 32: 70-72.
-
Itin PH (2014) Etiology and pathogenesis of ectodermal dysplasias. Am J Med Genet A 164A: 2472-2477.
-
Pozo-Molina G, Reyes-Reali J, Mendoza-Ramos MI, Villalobos-Molina R, Garrido-Guerrero E, et al. (2015) Novel missense mutation in the EDA1 gene identified in a family with hypohidrotic ectodermal dysplasia. Int J Dermatol 54: 790-794.
-
Khabour OF, Mesmar FS, Al-Tamimi F, Al-Batayneh OB, Owais AI (2010) Missense mutation of the EDA gene in a Jordanian family with X-linked hypohidrotic ectodermal dysplasia: phenotypic appearance and speech problems. Genet Mol Res 9: 941-948.
-
Lamartine J (2003) Towards a new classification of ectodermal dysplasias. Clin Exp Dermatol 28: 351-355.
-
Salas-Alanis JC, Wozniak E, Mein CA, Duran Mckinster CC, Ocampo-Candiani J, et al. (2015) Mutations in EDA and EDAR Genes in a Large Mexican Hispanic Cohort with Hypohidrotic Ectodermal Dysplasia. Ann Dermatol 27: 474-477.
-
Singer SL, Henry PJ, Liddelow G, Rosenberg I (2012) Long-term follow-up of implant treatment for oligodontia in an actively growing individual: a clinical report. J Prosthet Dent 108: 279-285.
-
Nakayama Y, Baba Y, Tsuji M, Fukuoka H, Ogawa T, et al. (2015) Dentomaxillofacial characteristics of ectodermal dysplasia. Congenit Anom (Kyoto) 55: 42-48.
-
Rad AS, Siadat H, Monzavi A, Mangoli AA (2007) Full mouth rehabilitation of a hypohidrotic ectodermal dysplasia patient with dental implants: a clinical report. J Prosthodont 16: 209-213.
-
Bani M, Tezkirecioglu AM, Akal N, Tuzuner T (2010) Ectodermal dysplasia with anodontia: a report of two cases. Eur J Dent 4: 215-222.
-
Hickey AJ, Vergo TJ Jr (2001) Prosthetic treatments for patients with ectodermal dysplasia. J Prosthet Dent 86: 364-368.
-
Bala S, Nikhil M, Chugh A, Narwal A (2012) Prosthetic rehabilitation of a child suffering from hypohidrotic ectodermal dysplasia with complete anodontia. Int J Clin Pediatr Dent 5: 148-150.
-
Pigno MA, Blackman RB, Cronin RJ Jr, Cavazos E (1996) Prosthodontic management of ectodermal dysplasia: a review of the literature. J Prosthet Dent 76: 541-545.
-
Grecchi F, Pagliani L, Mancini GE, Zollino I, Carinci F (2010) Implant treatment in grafted and native bone in patients affected by ectodermal dysplasia. J Craniofac Surg 21: 1776-1780.
-
Tarjan I, Gabris K, Rozsa N (2005) Early prosthetic treatment of patients with ectodermal dysplasia: a clinical report. J Prosthet Dent 93: 419-424.
-
Bayat M, Khobyari MM, Dalband M, Momen-Heravi F (2011) Full mouth implant rehabilitation of a patient with ectodermal dysplasia after orthognathic surgery, sinus and ridge augmentation: a clinical report. J Adv Prosthodont 3: 96-100.
-
Raducanu AM, Pauna M, Feraru IV (2010) A simple prosthetic restorative solution of a single peg-shaped upper central primary incisor in a case of ectodermal dysplasia. Rom J Morphol Embryol 51: 371-374.
-
Dula LJ, Ahmedi EF, Lila-Krasniqi ZD, Shala KSh (2015) Clinical evaluation of removable partial dentures on the periodontal health of abutment teeth: a retrospective study. Open Dent J 9: 132-139.
-
Santawisuk W, Kanchanavasita W, Sirisinha C, arnirattisai C (2010) Dynamic viscoelastic properties of experimental silicone soft lining materials. Dent Mater J 29: 454-460.
-
Pisani MX, Segundo AL, Leite VM, de Souza RF, da Silva MA, et al. (2013) Electromyography of masticatory muscles after denture relining with soft and hard denture liners. J Oral Sci 55: 217-224.
-
Sadr K, Alipour J, Heidary F (2012) Finite Element Analysis of Soft-lined Mandibular Complete Denture and its Supporting Structures. J Dent Res Dent Clin Dent Prospects 6: 37-41.
-
Atsu S, Keskin Y (2013) Effect of silica coating and silane surface treatment on the bond strength of soft denture liner to denture base material. J Appl Oral Sci 21: 300-306.
-
Salloum AM (2014) Creep and stress relaxation behavior of two soft denture liners. J Indian Prosthodont Soc 14: 93-97.
-
Chaves CA, Vergani CE, Thomas D, Young A, Costa CA, et al. (2014) Biological effects of soft denture reline materials on L929 cells in vitro. J Tissue Eng 5: 2041731414540911.
-
Atay A, Bozok Cetintas V, Cal E, Kosova B, Kesercioglu A, et al. (2012) Cytotoxicity of hard and soft denture lining materials. Dent Mater J 31: 1082-1086.
-
Rodrigues S, Shenoy V, Shetty T (2013) Resilient liners: a review. J Indian Prosthodont Soc 13: 155-164.
-
Gupta N, Misra N, Kumar S, Uppal S (2013) Modified technique of soft liner application. BMJ Case Rep 2013.
-
Muralidhar G, Satish Babu CL, Shetty S (2012) Integrity of the interface between denture base and soft liner: a scanning electron microscopic study. J Indian Prosthodont Soc 12: 72-77.
-
Kumari SV, Taruna M, Chittaranjan B, Reddy SM, Reddy KK, et al. (2015) A qualitative analysis to compare the effects of surface machining of conventional denture base resin and two soft liners: a scanning electron microscopic study. J Clin Diagn Res 9: ZC30-34.
-
Kearns G, Sharma A, Perrott D, Schmidt B, Kaban L, et al. (1999) Placement of endosseous implants in children and adolescents with hereditary ectodermal dysplasia. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 88: 5-10.





