International Journal of Oral and Dental Health
Trends in Recurrence of Keratocystic Odontogenic Tumor
Ianculovici C, Blinder D and O Peleg*
Department of Oral and Maxillofacial surgery, Sheba Tel Hashomer Medical Center, Israel
*Corresponding author:
Dr. Oren Peleg, Department of Oral and Maxillofacial surgery, Sheba Tel Hashomer Medical Center, Israel, Tel: +972544636691, E-mail: orenpeleg@gmail.com
Int J Oral Dent Health, IJODH-2-031, (Volume 2, Issue 3), Case Series; ISSN: 2469-5734
Received: June 07, 2016 | Accepted: July 09, 2016 | Published: July 12, 2016
Citation: Ianculovici C, Blinder D, Peleg O (2016) Trends in Recurrence of Keratocystic Odontogenic Tumor. Int J Oral Dent Health 2:031. 10.23937/2469-5734/1510031
Copyright: © 2016 Ianculovici C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The recurrence rate of 112 cases of Keratocystic Odontogenic Tumor (KCOT) were analyzed with regard to their location, size, locularity and treatment.
36 patients (32.1%) presented recurrence. Multilocular KCOT measuring more than 3.5 cm presented higher rate of recurrence. When the initial treatment was enucleation with peripheral ostectomy the recurrence was located in the periphery of the initial tumor. When the treatment was marsupialization followed by enucleation and peripheral ostectomy, the recurrence was located in the periphery of the tumor reached after marsupialization, usually in area of adjacent teeth. The addition of Carnoy's solution has slightly reduced recurrence rate.
Introduction
The Keratocystic Odontogenic Tumor (KCOT) is characterized by its high tendency to recur after surgical treatment. This is attributed to its infiltrative growth pattern and to the failure during surgery to remove the epithelial rests of the dental lamina or the daughter cysts [1-4].
The reported recurrence of KCOT in the past literature ranged from 2.5% to 62.5% [3,4]. More commonly recurrence of the tumor is reported as 20% to 30% [2,5,6]. The fluctuations in the recurrence rate are explained by the variation in length of the follow-up period, the treatment modalities, the initial size of the lesion, its locularity, the number of cases included in the study, the pathology of the tumor (presence of orthokeratin or parakeratin), the skill of the surgeon and the association with nevoid basal cell carcinoma syndrome [5,7-14].
The purpose of this study is to review our department experience with the recurrence rate of 112 cases of KCOT treated, with regard to the location, size, locularity, treatment modality and period of follow-up.
Patients and Methods
112 patients, 70 males and 52 females were treated and followed-up for a period of 3-17 years. Patients presenting with small tumors were treated by enucleation and curettage. In cases of large cysts, an incisional biopsy was first performed, and taking into consideration the proximity of the tumor to vital structures that needed to be preserved and the degree of cooperation of the patient, a decision was made regarding the mode of treatment: enucleation with peripheral ostectomy or marsupialization followed by enucleation with peripheral ostectomy in both modalities with or without the use of Carnoy's solution.
Every patient was followed-up postoperatively clinically and radiographically by periapical and panoramic X-ray. If doubt of recurrence existed, a dental scan computer tomography was performed and surgical exploration was considered. All Patients had a follow up period of 3 years and up to 17 years (Mean 6.1 years). Patients either with basal cell nevus syndrome or with a cystic lesion exhibiting any evidence of orthokeratinization on histopathologic examination were excluded from the study.
Of the 112 patients 36 patients (31.1%) presented with recurrence and were analyzed for its initial location, size, locularity, treatment modality and location of recurrence.
Results
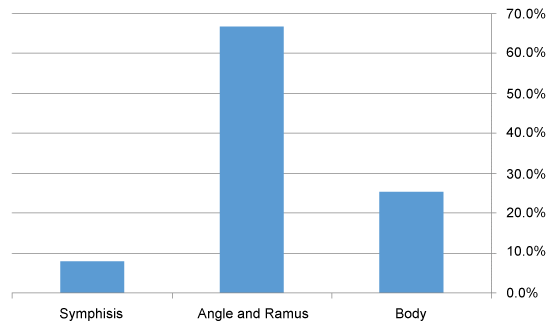
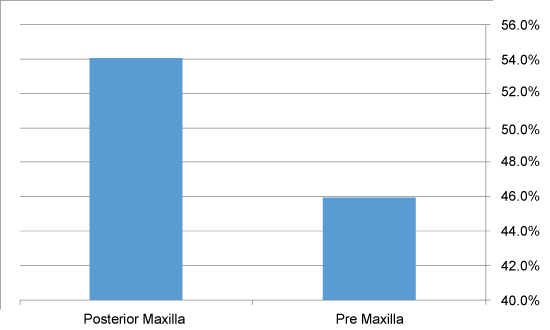
Of the 112 patients with KCOT, 70 were males and 52 females. Their age varied from 10 to 69 years with a mean of 37 years. 75 lesions (66.9%) were located in the mandible (19 in the body, 50 in the angle and the ramus, 6 in the symphysis) as showed in figure 1, and 37 (33.1%) in the maxilla (17 in the pre-maxilla and 20 in the posterior area of the maxilla) as showed in figure 2. 83 (74.1%) were unilocular and 29 (25.9%) were multilocular.
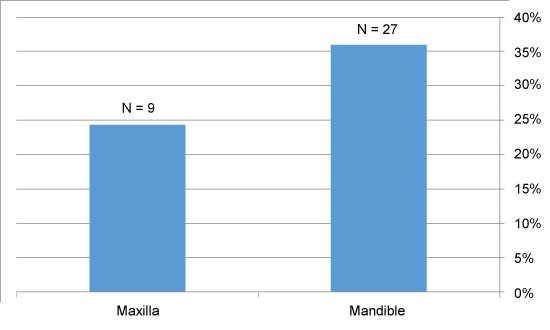
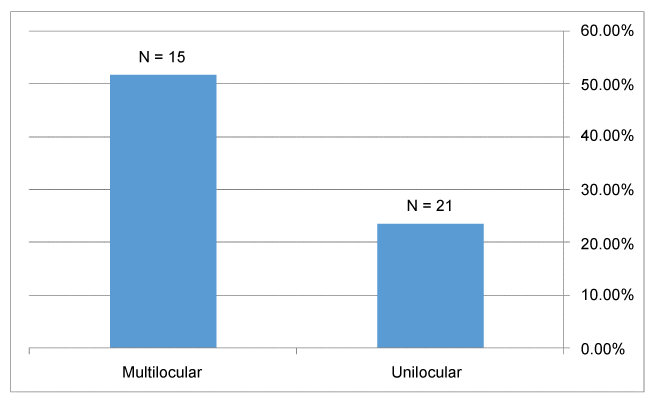
36 patients (32.1%) presented with recurrent KCOT (11 females and 25 males). Their age varied from 14 to 69 years. 27 out of 75 (36%) mandibular lesions recurred and 9 out of 37 (24.3%) maxillary lesions recurred. 21 out of 83 (25.3%) unilocular KCOT recurred. 15 out of 29 (51.7%) multilocular KCOT recurred (Figure 3).
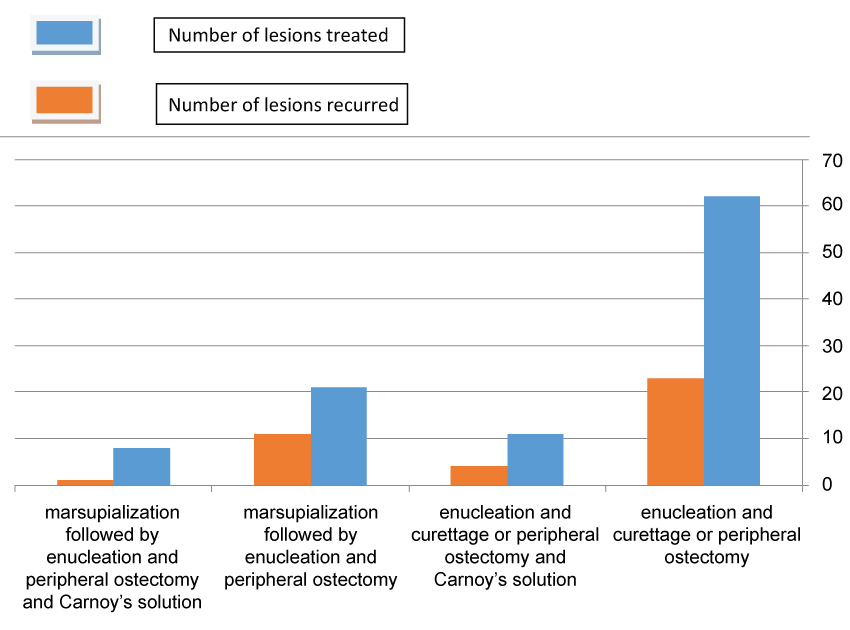
73 out of 112 (65.1%) OKC lesions were treated by initial enucleation and curettage with peripheral ostectomy, with total recurrence of 23 cases (31.5%). 11 of them were also treated chemically using Carnoy's solution with 4 cases of recurrence (36.3%) (Figure 4). The initial size of these 23 recurring lesions was equal or above 1 cm (mean of 4.9 cm).
15 were unilocular and 8 were multilocular (Figure 5). 17 recurred in the mandible (2 in the anterior region and 15 in the body angle and ramus). 6 recurred in the maxilla (3 in the pre maxilla, one recurrence in the piriform area and 2 near adjacent teeth in the posterior maxilla). The recurrence was located at the periphery of the initial lesion and in some cases adjacent to the teeth at the periphery of the lesion. The recurrence was diagnosed from 1 to 5 years after enucleation (mean 2.5 years).
39 out of 112 (34.8%) OKC lesions treated by marsupialization followed by enucleation and peripheral ostectomy, 12 recurred (30.7%). The lesions that recurred had an initial size equal or above 3.5 cm (mean of 3.9 cm). 6 were unilocular and 6 were multilocular. The recurrence was located at the periphery of the tumor after marsupialization and not at its initial periphery. 9 recurred in the mandible (2 in the anterior region and 7 in the angle) and 3 recurred in the maxilla. In all of the cases the recurrence was located at the apices of adjacent teeth. The recurrence was diagnosed after a follow-up period ranging from one to 8 years (mean of 2.9 years). 8 of the above were also treated chemically using Carnoy's solution with only 1 case of recurrence (12.5%).
Over all 19 out of 112 lesions were treated surgically and also chemically by Carnoy's solution, 5 cases (26.3%) recurred. 93 out of 112 lesions were treated only surgically, 31 of them recurred (33.3%).
Discussion
This study reveals that recurrence of KCOT occurred mainly in multilocular lesions greater than 3.5 cm in diameter. The recurrence could be diagnosed only after a year of follow-up because it was difficult to evaluate in the first year the radiographic signs of recurrence or incomplete healing process.
The location of the recurrence depends on the initial treatment of the KCOT. When the lesion was treated by enucleation and curettage or peripheral ostectomy, the recurrence occurred at the periphery of the initial lesion, usually in an area that was difficult to perform a clear enucleation. Use of additional Carnoy's solution in these cases showed similar outcome. Stoelinga in 2001 showed 11% recurrence rate out of 82 KCOTs treated with enucleation, excision of overlying mucosa and applying Carnoy's solution [15]. In our study when the KCOT was treated by marsupialization and later by enucleation with peripheral ostectomy the recurrence was located at the periphery of the lesion that was reached after marsupialization and particularly in areas that were difficult to curette such as apices of adjacent teeth that the surgeon tried to save by this conservative treatment. Addition of Carnoy's solution in these cases showed reduction in number of recurrences but did not change the location of recurrence. The purpose of marsupialization was to save vital adjacent structures such as nerve or teeth or to prevent extensive mutilating surgery even at the cost of possible recurrences. Pogrel and Jorden in 2004, went even further and treated 10 KCOTs by marsupialization alone and had no recurrence. Their study also suggested that the cyst lining may get replaced by normal epithelium during this treatment [16]. In our study, we observed more recurrence in cases treated by marsupialization followed by enucleation and peripheral ostectomy than in cases treated initially by enucleation. However, all these recurrent lesions were enucleated easily by a second minor surgical procedure. Lesions that were treated surgically and chemically recurred a bit less than those lesions that were treated only surgically.
Conclusion
Marsupialization followed by enucleation is a conservative treatment which permits to save adjacent vital structures. This treatment modality is chosen only when a possible recurrence will not endanger a vital structure such as base of skull, brain or eyes and when the recurrence will be easily treated. Use of Carnoy's solution slightly reduces the recurrence rate and therefore when possible is recommended especially after marsupialization.
References
-
Nayak MT, Singh A, Singhvi A, Sharma R (2013) Odontogenic keratocyst: What is in the name? J Nat Sci Biol Med 4: 282-285.
-
Philipsen HP (2005) Keratocystic odontogenic tumour. In: Barnes L, Eveson JW, Reichart P, Sidransky D, (eds.) World Health Organization Classification of Tumours. Pathology and genetics. Head and Neck Tumours. IARC Press, Lyon, 306-307.
-
Regezi JA, Sciubba JJ, Jordan RCK (2007) Oral Pathology. Clinical Pathologic Correlations. Saunders, China, 2008, 245-249.
-
Shear M, Speight P (2007) Cysts of the Oral and Maxillofacial Regions (4th edn). Blackwell, Singapore, 6-58.
-
Jafaripozve N, Jafaripozve S, Khorasgani MA (2013) Kerathocyst Odontogenic Tumor: Importance of Selection the Best Treatment Modality and a Periodical Follow-up to Prevent from Recurrence: A Case Report and Literature Review. Int J Prev Med 4: 967-970.
-
Finkelstein MW, Hellstein JW, Lake KS, Vincent SD (2013) Keratocystic odontogenic tumor: a retrospective analysis of genetic, immunohistochemical and therapeutic features. Proposal of a multicenter clinical survey tool. Oral Surg Oral Med Oral Pathol Oral Radiol 116: 75-83.
-
Rajeshkumar BP, Rai KK, Geetha NT, Shivakumar HR, Upasi AP (2013) Carnoy's in Aggressive Lesions: Our Experience. J Maxillofac Oral Surg 12: 42-47.
-
Gao L, Wang XL, Li SM, Liu CY, Chen C, et al. (2014) Decompression as a treatment for odontogenic cystic lesions of the jaw. J Oral Maxillofac Surg 72: 327-333.
-
Kinard BE, Chuang SK, August M, Dodson TB (2013) How well do we manage the odontogenic keratocyst? J Oral Maxillofac Surg 71: 1353-1358.
-
Brauer HU, Diaz C, Manegold-Brauer G (2013) Radiographic assessment of a keratocystic odontogenic tumour using cone-beam computed tomography. Eur Arch Paediatr Dent 14: 173-177.
-
MacDonald D, Gu Y, Zhang L, Poh C (2013) Can clinical and radiological featurespredict recurrence in solitary keratocystic odontogenic tumors? Oral Surg Oral Med Oral Pathol Oral Radiol 115: 263-271.
-
Pogrel MA (2013) The keratocystic odontogenic tumor. Oral Maxillofac Surg Clin North Am 25: 21-30.
-
Sansare K, Raghav M, Mupparapu M, Mundada N, Karjodkar FR, et al. (2013) Keratocystic odontogenic tumor: systematic review with analysis of 72 additional cases from Mumbai, India. Oral Surg Oral Med Oral Pathol Oral Radiol 115: 128-139.
-
Morais de Melo W, Pereira-Santos D, Sonoda CK, Hochuli-Vieira E (2012) Decompression for management of keratocystic odontogenic tumor in the mandible. J Craniofac Surg 23: e639-640.
-
Stoelinga PJ (2001) Long-term follow-up on keratocysts treated according to a defined protocol. Int J Oral Maxillofac Surg 30: 14-25.
-
Pogrel MA, Jordan RC (2004) Marsupialization as a definitive treatment for the odontogenic keratocyst. J Oral Maxillofac Surg 62: 651-655.