International Journal of Oral and Dental Health
Unusual Necrosis of the Lower Lip Following a Varicella Zoster Recurrence
Adam P McCormick1, Robert J Kanas2*, Mark Orton3 and Ted Rice4
1Private Practice Oral and Maxillofacial Surgeons of Utah, Layton, Utah, USA
2Private Practice, Bay City, Michigan, USA
3Staff Pathologist, Associates of Pathology, Ogden, Utah, USA
4University of Mississippi School of Dentistry, Jackson, Miss, USA
*Corresponding author:
Robert J. Kanas, DDS, Private Practice, Bay City, Michigan, 368 Cantley St., Lakeville, MI 48366-0432, USA, Tel: 248-763-4447, E-mail: rjkanas@gmail.com
Int J Oral Dent Health, IJODH-2-026, (Volume 2, Issue 1), Case Report; ISSN: 2469-5734
Received: February 09, 2016 | Accepted: March 21, 2016 | Published: March 24, 2016
Citation: McCormick AP, Kanas RJ, Orton M, Rice T (2016) Unusual Necrosis of the Lower Lip Following a Varicella Zoster Recurrence. Int J Oral Dent Health 2:026. 10.23937/2469-5734/1510026
Copyright: © 2016 McCormick AP, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Recurrence of varicella-zoster virus (VZV) or herpes zoster (HZ) is a relatively common cutaneous eruption among the elderly (> 60 yrs.) or immunocompromised patients. It usually presents as an exanthematous pruritic rash that becomes vesicular, pustular or ulcerative. HZ commonly involves a unilateral thoracic dermatome. When the trigeminal nerve is involved, a unilateral eruption in the oral cavity and ipsilateral side of the face may occur following a division of the trigeminal nerve. In rare cases, prolonged infection may lead to a localized vasculitis with resultant extensive necrosis of the surrounding tissue.
Case Report: This report is a description of extensive lower lip necrosis following a recurrent VZV infection with concomitant herpes simplex-1 infection in a young adult female patient. Differential diagnosis along with reconstruction of the lower lip is illustrated with excellent post-operative esthetic and functional outcomes.
Conclusion: Reactivated VZV should be considered as a potential cause of unusual, large necrotizing ulcers of the orofacial structures in immunocompetent patients.
Keywords
Varicella-zoster virus (VZV), Herpes-simples-1 virus (HSV-1), Lip, Vasculitis, Necrosis, Infarction
Introduction
Varicella Zoster virus (VZV) is the causal agent of varicella (chickenpox) and recurrences of the virus is referred to as herpes zoster (shingles). Primary VZV infection is a common childhood disease in non-vaccinated populations. The primary VZV infection is characterized by fever, malaise and an exanthematous vesicular rash involving the face and trunk followed by involvement of the extremities. The rash usually progresses through stages of pruritic exanthem, vesiculation, pustulation and crusting [1]. In immunocompetent individuals, the infection is self-limiting and resolves in 10-14 days.
During the initial varicella infection, virus is transported to sensory nerves and establishes latency in the dorsal spinal ganglia. Herpes zoster (HZ) presents as a cutaneous vesicular eruption in a unilateral dermatome innervated by the affected sensory nerve upon reactivation of latent VZV [2]. Recurrences usually affect the thoracic dermatomes in about two-thirds of the cases. The lesions are usually preceded by days of tingling, burning and itching followed by a painful vesicular eruption in the skin within the distribution of the sensory nerve, usually in a characteristic, unilateral fashion rarely crossing the midline. Clinical presentation consists of clusters of vesicles on an erythematous base that become pustular, ulcerate and then crust with resolution in 2-3 weeks in otherwise healthy individuals [3].
VZV may also be dormant in the trigeminal ganglia and when reactivated, lesions may appear on the face, lips, mouth or eye, or along any of the divisions of the trigeminal nerve [3]. The oral lesions are usually unilateral and extend to the midline and frequently present in conjunction with overlying facial skin involvement. The oral lesions usually consist of small vesicles that rupture quickly to form shallow painful ulcers. These also resolve in 2-3 weeks in immunocompetent patients.
The most common complication of HZ is postherpetic neuralgia. It usually manifests as an intense, sharp, stabbing pain that may last for more than three months following a VZV reactivation [1,4]. Other complications include facial nerve motor palsy [5], optic neuropathy leading to blindness [6] and involvement of the maxillary or mandibular divisions of the trigeminal nerve may lead to devitalization of teeth and root resorption [7].
Extensive tissue necrosis has been previously reported with HZ. Although rare, extensive osteonecrosis of either the maxilla or mandible with spontaneous exfoliation of teeth have been reported either concurrently or following a recurrent VZV eruption of the trigeminal nerve [2]. Also, there have been rare reports of extensive skin or nose necrosis following a reactivated VZV eruption [8]. The following case report may be the first description of extensive unilateral necrosis of the lower lip following a recurrent VZV infection in a young female patient.
Case Report
A 23-year-old female presented initially to the emergency department (ED) at McKay Dee Hospital in Ogden, Utah for a large lip ulceration. A bacterial culture was taken and Augmentin along with analgesics were prescribed. She was then referred for follow-up the next day as an outpatient to Oral and Maxillofacial Surgeons of Utah (Bountiful, Layton, Ogden, Pleasant View, Utah).
Her chief complaint was "I pulled my lip off". Her history of present illness consisted of having "fever blisters" off and on for the past 3 months. Approximately one week prior to her presentation in the ED she stated, "My lower lip started to scab over from "fever blisters" and then subsequently lifted off. She reported a history of pregnancy x 1 (vaginal), vasovagal syncope, gastroesophageal reflux disease, migraines, snoring, cholelithiasis, bruising and cold sores. She reported a 5 pack year history of tobacco use. She denied illicit drug use. There was no previous history of surgeries, allergies or medication reactions. She had not visited the dentist recently nor received any local anesthetic. She denied any trauma or self-mutilation to the lips. She was prescribed in the ED Augmentin 500 mg and analgesics.
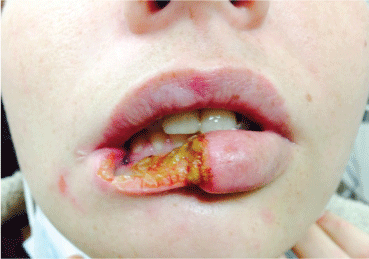
Clinical examination revealed a large, red, necrotic, trapezoidal defect of the lower right lip that was covered with yellow exudate and extended 0.5 cm medial of the right commissure and terminated at the midline (Figure 1). There appeared to be extensive loss of supporting lip tissue similar to an infarct. It measured 3.0 cm × 1.5 cm. There were also two areas of erythema measuring 0.5 cm each in the upper lip and in the skin below the right lip commissure (arrows). These appeared to represent healing small ulcers. Intraoral lesions were absent. No cervical lymphadenopathy was detected.
.
Figure 1: Large trapezoidal necrotic ulceration of the lower right lip covered with yellow exudate.
View Figure 1
A complete blood count (CBC) was within normal limits and her lymphocytes were 1206 cells/μl (normal range 430-1800 cells/μl). The differential diagnosis included a factitial injury or trauma, methicillin-resistant staphylococcus aureus (MRSA infection), a recurrent VZV infection with extensive tissue necrosis or an anaplastic large T cell lymphoma with a vasculitis component leading to infarction and necrosis. A repeat bacterial culture and sensitivity swab was submitted to rule out MRSA. Both bacterial cultures came back negative. The patient refused to have a tissue biopsy performed at the initial presentation. Therefore, blood serum titers were ordered for VZV, HSV-1, and HSV-2 and empirical treatment was initiated.
The patient was prescribed topical acyclovir 5% (applied 6 times per day) and systemic valacyclovir hydrochloride 500 mg BID × 7 days (because of her history of recurrent "fever blisters." Her Augmentin and analgesics received in the ED were continued. VZV, HSV-1 and HSV-2 serum titers were ordered. HerpeSelect-1 and HerpeSelect-2 (Focus Diagnostics, Inc., Cypress, California) commercial ELISA tests were utilized and have high specificity (92%) with low to no cross reactivity to other herpesviruses. A commercial available ELISA test was utilized for the detection of VZV (Focus Diagnostics, Inc. Cypress, California). The patient was scheduled to return in one week for re-evaluation.
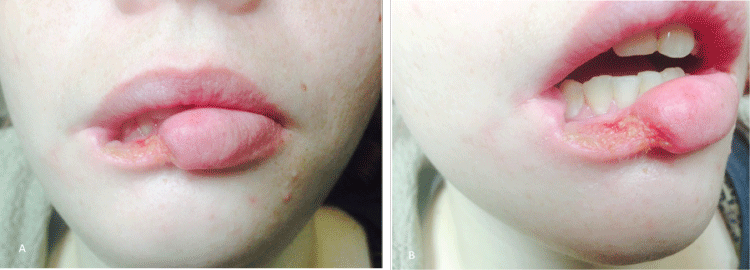
At one week, the lower lip lesion had markedly improved (Figure 2A and Figure 2B). The lesion appeared less red and the beginning of re-epithelialization was evident. There was a small amount of yellow exudate covering the defect. The patient reported less pain and tolerated the medication well. The following immunoglobulin titers were reported at that time; VZV IgG was elevated at 1.81 (normal < 1.09) while the VZV IgM was not elevated at 0.33 (normal < 0.91), HSV-1 IgG was significantly elevated at 7.30 (normal < 0.90) and HSV-2 IgG was 0.09 (normal < 0.90). Based on these laboratory results, unilateral feature of the lip lesion terminating at the midline and response to antiviral therapy, a diagnosis of extensive lip necrosis due to a herpetic vasculitis from reactivation of VZV and/or HSV-1 was determined. Real Time DNA polymerase chain reaction of a swap from the lesion may have offered a means of identifying the specific virus type in this case [9]. Nonetheless, she was continued on the antiviral therapy for additional one week and scheduled to return.
.
Figure 2: Same lip lesion after 1 week of antiviral therapy; Note partial healing, less inflammation and small amount of residual exudate; Front view (A) and lateral view (B).
View Figure 2
After two weeks of antiviral therapy, there remained a large defect in the lower right lip but the inflammation resolved. After consultation with the patient, a reconstructive surgery of the lower lip was decided. The surgery was scheduled 2 weeks later to allow for more resolution of the lip and to see a continued response with only topical acyclovir 5%.
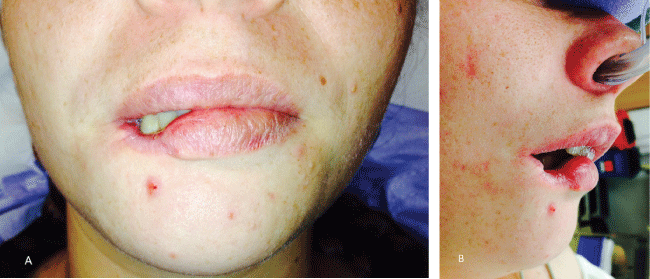
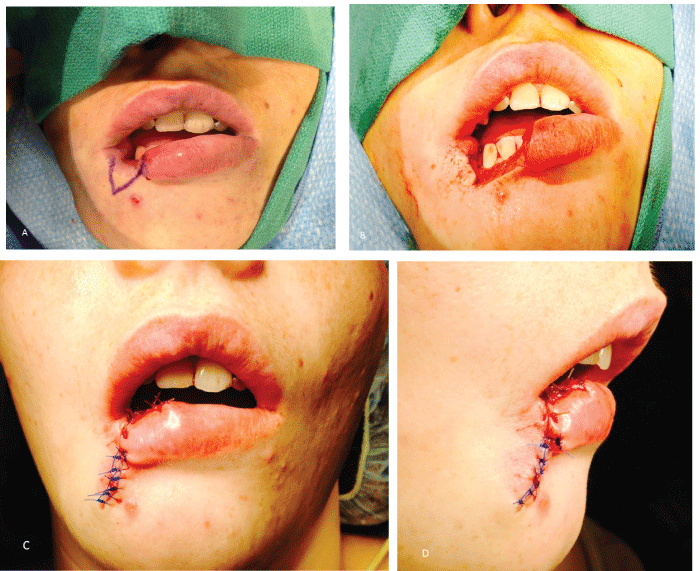
The day of surgery, the lip lesion had completely re-epithelialized (Figure 3A and Figure 3B). The patient was brought to the OR and placed on the operating table in the supine position. She was nasally intubated. The defect was marked with an indelible marker to outline the resection (Figure 4A). A wedge excision was completed with a #15 blade through skin, subcutaneous tissue, muscle and mucosa (Figure 4B). The tissue was submitted for final histopathology. The orbicularis oris muscle was then re-approximated with 4-0 vicryl sutures in an interrupted fashion. The mucosa was then closed with 3-0 chromic gut in a similar fashion. The vermilion was re-approximated and tacked with a 3-0 chromic gut suture while the skin was closed with 5-0 prolene in an interrupted fashion. The 3-0 tacking suture at the vermillion border was then removed and replaced with a 5-0 prolene suture (Figure 4C and Figure 4D). The patient tolerated the procedure well and was discharged to home with follow up for one week later.
.
Figure 3: Pre-operative images showing re-epithelialization of right lip defect (Front view (A) and lateral view (B).
View Figure 3
.
Figure 4: Images taken at time of surgery. Indelible markings (A); V-excision of scarred defect (B); front view of sutured post-operative image (C); lateral view of sutured defect.
View Figure 4
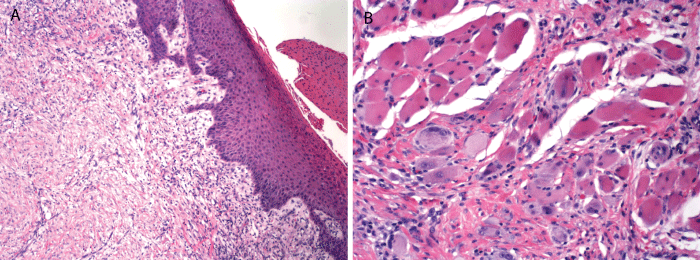
The surgical excision specimen from the reconstructive surgery revealed mild keratosis of the epithelium, submucosal fibrosis and skeletal muscle atrophy consistent with a scarred infarct (Figure 5A and Figure 5B). The patient healed uneventfully and post-op photos were taken at two weeks. The final result from the surgery restored both function and enhanced esthetics to the lower lip (Figure 6).
.
Figure 5: Photomicrograph of surgical biopsy specimen at time of reconstructive surgery. Mild keratosis, fibrosis and atrophy of skeletal muscle consistent with a healed infarct (A) (magnification X 200); Muscle atrophy with clumping of nuclei to form multinucleated skeletal muscle fibers (B) (magnification X 400).
View Figure 5
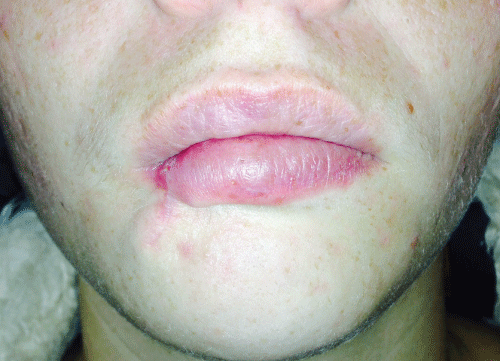
.
Figure 6: Post-operative image at two weeks showing restoration of function and esthetics.
View Figure 6
Discussion
Extensive tissue necrosis of the head and neck area has been previously reported with recurrence of VZV or HZ, although rare. The mechanism involved appears to be a viral induced vasculitis that may originate in the neurovascular bundles of the trigeminal nerve branches that extend to adjacent vessels with persistent infection [3]. This may lead to focal ischemic necrosis of the tissue supplied by the affected artery. In this case, a small division of the inferior branch of the labial artery supplying the right lower lip would most likely been affected.
VZV, unlike HSV-1, is more likely to induce a vasculitis with resultant ischemic necrosis. Even though both viruses are neurotropic, have the ability to remain dormant in the trigeminal ganglia and may reactivate to cause either cutaneous or intraoral vesiculoulcerative lesions, recurrent VZV infection has been associated with tissue necrosis. A co-infection with recurrent HSV-1 may also have occurred in this case by evidence of the high IgG antibody titer and may have contributed to the development of this lip lesion. HSV-1 antibodies may have propagated the VZV infection through a mechanism designated intrinsic antibody-dependent enhancement [10]. However, HSV-1 is less likely to induce this type of ulceration and necrosis except in immunocompromised patients from HIV infection or transplant recipients [11,12]. Large, persistent necrotizing ulcers in both the nonkeratinizing and keratinizing oral mucosa have been reported in immunocompromised patients from HSV-1. In this case, there was no history or documentation of immunosuppression.
Osteonecrosis of the maxilla or mandible with spontaneous exfoliation of teeth has been reported in conjunction with reactivated VZV [2,3]. This is an unusual complication of VZV with the exact underlying mechanism undetermined. VZV infection of the periodontal fibers and pulp has been suggested along with a localized vasculitis of the small vessels supplying the periosteum. Nonetheless, the mechanism leading to necrosis of the lip in this case share some common mechanism with VZV associated osteonecrosis.
A review of the literature revealed a paucity of VZV associated necrosis of the skin and perioral structures. Extensive skin necrosis of the nose [8], outer retinal necrosis [6,13] and osteonecrosis of the jaws [2,3,14-16], all associated with reactivated VZV, have been reported previously. In some cases, the patients were either elderly or immunocompromised. However, some case reports were described in younger adults without any identifiable cause for immune suppression as in this case report. VZV has the capacity to potentially cause tissue necrosis as a clinical complication from herpes zoster and should be included in a differential diagnosis of unusual necrotic lesions of the face, neck and mouth.
The differential diagnosis of this lip lesion would include a factitial injury [17,18], impetigo [19], MRSA induced necrosis [20], cutaneous T-cell lymphoma with an angiocentric component [21,22], and VZV associated tissue necrosis. Self-induced trauma or a factitial injury was eliminated based on the history. Self-inflicted trauma is a potential complication from dental therapy and local anesthesia of the inferior alveolar nerve. There is usually a history of a recent dental visit, occurs mainly in children and the severity of lip ulceration is not as extensive as in this case. Impetigo is a contagious cutaneous infection seen mainly in children from either Staphylococcus aureus or group a β-hemolytic streptococci. It often begins as a single macule on the extremities or face which rapidly progresses into a larger, crusted ulceration. Rare reports of necrotizing ulceration have occurred with impetigo [18]. However, a more likely cause of extensive lip necrosis would be a community acquired methicillin- resistant staphylococcus aureus (MRSA) infection [19]. Cultures in this case proved negative for MRSA. An anaplastic large T cell lymphoma occurs in younger adults and may involve blood vessels with a resultant necrotizing vasculitis. It was considered if the lesion did not respond to antiviral therapy.
Treatment of reactivated VZV is directed at the cause and symptoms. Systemic antiviral therapy such as acyclovir (800 mg 5 times daily for 7-10 days), famciclovir (500 mg 3 times daily for 7 days) or valacyclovir (500 mg 3 times daily for 7 days) are some of the approved dosages recommended by the U.S. FDA [23]. Supportive analgesics should be prescribed as needed and include opioids combined with NSAIDs. Gabapentin and pregabalin reduce neurotransmitter release and have shown some efficacy in reducing pain in herpes zoster [23]. Systemic steroids are indicated in the presence of moderate to severe pain or rash with the development of postherpetic neuralgia. However, risks associated with the use of corticosteroids must be carefully evaluated. Medical consultation would be warranted prior to steroid therapy. Even though topical acyclovir was administered in this case, they have proven to be ineffective [23].
A case of extensive lip necrosis resulting in a large tissue defect from a reactivated VZV and possible co-infection with HSV-1 was presented. A differential diagnosis and management of the case was described. Even though reactivated VZV occurs more often in older adults and immunocompromised patients, reactivated VZV needs to be considered when presented with large necrotizing ulcers of the face and mouth in young adults, not otherwise immune compromised.
References
-
LaGuardia JJ, Gilden DH (2001) Varicella-zoster virus: a re-emerging infection. J Investig Dermatol Symp Proc 6: 183-187.
-
Jain MK, Manjunath KS, Jagadish SN (2010) Unusual oral complications of herpes zoster infection: report of a case and review of literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 110: e37-41.
-
Mendieta C, Miranda J, Brunet LI, Gargallo J, Berini L (2005) Alveolar bone necrosis and tooth exfoliation following herpes zoster infection: a review of the literature and case report. J Periodontol 76: 148-153.
-
Nagel MA, Gilden DH (2007) The protean neurologic manifestations of varicella-zoster virus infection. Cleve Clin J Med 74: 489-494.
-
Sun WL, Yan JL, Chen LL (2011) Ramsay Hunt syndrome with unilateral polyneuropathy involving cranial nerves V, VII, VIII, and XII in a diabetic patient. Quintessence Int 42: 873-877.
-
Moorthy RS, Weinberg DV, Teich SA, Berger BB, Minturn JT, et al. (1997) Management of varicella zoster virus retinitis in AIDS. Br J Ophthalmol 81: 189-194.
-
Kanas RJ, Kanas SJ (2011) Dental root resorption: a review of the literature and a proposed new classification. Compend Contin Educ Dent 32: e38-52.
-
Snel BJ, Visconti G, Grabietz PD, Werker PM (2010) Necrosis of nose skin after varicella zoster infection: a case report. J Plast Reconstr Aesthet Surg 63: e445-447.
-
LeGoff J, Péré H, Bélec L (2014) Diagnosis of genital herpes simplex virus infection in the clinical laboratory. Virol J 11: 83.
-
Ubol S, Halstead SB (2010) How innate immune mechanisms contribute to antibody-enhanced viral infections. Clin Vaccine Immunol 17: 1829-1835.
-
Jensen JL, Kanas RJ, DeBoom GW (1987) Multiple oral and labial ulcers in an immunocompromised patient. J Am Dent Assoc 114: 235-236.
-
Arduino PG, Porter SR (2006) Oral and perioral herpes simplex virus type 1 (HSV-1) infection: review of its management. Oral Dis 12: 254-270.
-
Gnann JW Jr (2002) Varicella-zoster virus: atypical presentations and unusual complications. J Infect Dis 186 Suppl 1: S91-98.
-
Pushpanshu K, Kaushik R, Srivastava S, Punyani SR (2013) An unusual complication of tooth exfoliation and osteonecrosis following herpes zoster infection of trigeminal nerve: a case report and literature review. Minerva Stomatol 62: 241-245.
-
Pillai KG, Nayar K, Rawal YB (2006) Spontaneous tooth exfoliation, maxillary osteomyelitis and facial scarring following trigeminal herpes zoster infection. Prim Dent Care 13: 114-116.
-
Lambade P, Lambade D, Saha TK, Dolas RS, Pandilwar PK (2012) Maxillary osteonecrosis and spontaneous teeth exfoliation following herpes zoster. Oral Maxillofac Surg 16: 369-372.
-
Chi D, Kanellis M, Himadi E, Asselin ME (2008) Lip biting in a pediatric dental patient after dental local anesthesia: a case report. J Pediatr Nurs 23: 490-493.
-
Bendgude V, Akkareddy B, Jawale BA, Chaudhary S (2011) An unusual pattern of self-inflicted injury after dental local anesthesia: a report of 2 cases. J Contemp Dent Pract 12: 404-407.
-
Ghafoor M, Halsnad M, Fowell C, Millar BG (2012) Impetigo presenting as an acute necrotizing swelling of the lower lip in an adult patient. Oral Surg Oral Med Oral Pathol Oral Radiol 113: e22-24.
-
Bruno GJ, Bruno JM, Miyake AA (2007) Community-acquired methicillin-resistant Staphylococcus aureus infection with fatal necrotizing pneumonia from lip abscess: a case report. J Oral Maxillofac Surg 65: 2350-2353.
-
Ferreri AJ, Govi S, Pileri SA, Savage KJ (2012) Anaplastic large cell lymphoma, ALK-positive. Crit Rev Oncol Hematol 83: 293-302.
-
Nambudiri VE, Aboutalebi A, Granter SR, Saavedra A (2013) Recurrent ALK-negative anaplastic large T-cell lymphoma presenting as necrotizing vasculitis. Am J Dermatopathol 35: 512-516.
-
Dworkin RH, Johnson RW, Breuer J, Gnann JW, Levin MJ, et al. (2007) Recommendations for the management of herpes zoster. Clin Infect Dis 44 Suppl 1: S1-26.





