International Journal of Oral and Dental Health
Indications and Frequency of Orthognathic Surgery in Sweden - A Questionnaire Survey
Max Andrup1*, Jesper Elenius2, Eusebio Ramirez3 and Mats Sjöström4
1Public Dental Service, Hudiksvall, Sweden
2Public Dental Service, Skelleftea, Sweden
3Public Dental Service, Kalmar, Sweden
4Oral and Maxillofacial Surgeon, Umeå University, Sweden
*Corresponding author: Max Andrup, DDS, Public Dental Service, Folktandvården Hudiksvall, Skvallertorget 1, 82430 Hudiksvall, Sweden, Tel: +46 708 341587, E-mail: max@andrup.se
Int J Oral Dent Health, IJODH-1-019, (Volume 1, Issue 4), Research Article; ISSN: 2469-5734
Received: September 18, 2015 | Accepted: November 16, 2015 | Published: November 18, 2015
Citation: Andrup M, Elenius J, Ramirez E, Sjöström M (2015) Indications and Frequency of Orthognathic Surgery in Sweden - A Questionnaire Survey. Int J Oral Dent Health 1:019. 10.23937/2469-5734/1510019
Copyright: © 2015 Andrup M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Orthognathic surgery, a standard procedure used to improve intermaxillary relationship, surgically moves either one or both jaws. However, statistics for frequency and indications for orthognathic surgery in Sweden are non-existent. This study examines indications, frequency, and surgical techniques for orthognathic surgery performed in Oral and Maxillofacial Surgery (OMFS) clinics in Sweden. In 2011, a questionnaire survey was sent to all OMFS clinics in Sweden to collect data on gender and age of patients, surgical techniques, indications, frequency of operations, and whether patients underwent one- or two-jaw surgery. Of the 50 OMFS clinics, 47 responded, revealing that 891 patients in 23 clinics were treated with orthognathic surgery, slightly more women than men were treated, and 91% of the patients were 26 years or younger. The results from our survey indicate that functional indication is the most common surgical indication. This is not in line with the literature, which describes the aesthetic component as the most common indication. One explanation could be that the treatment in Sweden is heavily subsidized by federal financial support if certain inclusions criteria are fulfilled. These criteria are mainly based on cephalometric analysis together with dental arch relationship and not on aesthetic components, which are harder to measure. It was also revealed that there was a great discrepancy among the Swedish counties concerning one- vs. two-jaw surgery. A possible reason for this can be differences in surgical experience and custom at each OMFS clinic.
Keywords
Orthognathic surgery, Sweden, Questionnaire, Indications, Frequency
Introduction
Orthognathic surgery
Orthognathic surgery combines both maxillofacial surgery and orthodontics. Discrepancies between dental arches or between maxilla and the mandible can cause functional disorders that affect speech and mastication. More severe discrepancies can also affect the patient's psychological wellbeing. Less severe discrepancies are possible to correct with orthodontics alone. Orthognathic surgery is required when correcting more severe discrepancies as this involves skeletal disharmony in addition to discrepancies between dental arches and discrepancies in interrelations between jaws [1].
Several surgical procedures and techniques can be applied, depending on the indications for orthognathic surgery and the nature of the dentofacial deformity [1-6]. In situations with greater discrepancies and significant risk of relapse, a combination of maxillary and mandibular procedures may be needed due to the relation between the magnitude of the movement and the stability after surgery. A combination of maxillary and mandibular surgery can also be indicated when treating combinations of discrepancies or facial asymmetry. Moving the maxilla up and the mandible forward is the most stable movement. On the other hand, moving the mandible backwards, and widening or moving the maxilla down, are the least stable movements and are associated with a higher risk of relapse [7].
Indications
Malocclusion: Unlike optimum functional occlusion, dental malocclusion is more likely to lead to disease. Malocclusion may cause decreased masticatory function due to less inter-maxillary contact, causing a reduced occlusal contact area. Masticatory function after malocclusion treatment (e.g., orthognathic surgery) often remains inferior, with no significant improvement after surgery [8]. It seems that masticatory muscle function is decreased after surgery due to the adaption of the muscles to the new bone position and the stretching of the muscular fibres. After five years, studies have shown significant increase in masticatory function [8]. The impact of malocclusion on speech has been discussed, and a few studies have found that some types of malocclusion result in miss-articulations in speech [9]. However, there is no clear evidence that orthognathic surgery or malocclusion affects speech, but more studies are needed before a determination can be made [10]. Despite an alternative occlusal configuration, if the masticatory system is physiologically and is without pathology, there is no need to correct unless there is another indication [11].
Temporomandibular disorders (TMD): TMD is an umbrella term that includes multiple disorders (i.e., multiple aetiologies) and therefore multiple treatments are available [12,13]. TMD includes not only the temporomandibular joint (TMJ) as a source of disorder but also the entire masticatory system - the TMJ, the masticatory muscles, the head muscles, and the neck muscles [11]. Approximately 25% of patients in a general population claim to have TMD symptoms, but only about 5% have symptoms severe enough to seek treatment. Epidemiological studies also show that women are over-represented with respect to experiencing symptoms [11,12,14]. TMD can be treated using a variety of treatments, including surgical therapy, an option most often used only after less invasive treatments have been tried [12,13]. The literature describes a wide range (14 - 97%) of orthognathic surgery patients having TMD before surgery [15,16]. A majority of these patients, who had TMD and underwent orthognathic surgery, were women [16,17].
Although little evidence exists that suggests orthognathic surgery cures or prevents TMD, questionnaires indicated that 26% of the men and 46% of the women stated this as a strong motivation for undergoing orthognathic surgery [17]. When it comes to patient satisfaction, a correlation is found between preoperative severity of TMD symptoms and patient satisfaction with postoperative pain levels [16]. Generally, systematic reviews show that after orthognathic surgery TMD symptoms decrease, joint clicking decreases, and joint crepitus remains the same [15,18]. In addition, movement ability often decreases after surgery, but returns to normal within two years. Despite the results, these systematic reviews conclude that the evidence makes it difficult to draw any definitive conclusions because most of the studies are poorly designed and they use different designs, making comparisons between studies impossible. Moreover, the results between the studies vary significantly. A recent, fairly well-designed prospective controlled study draws similar conclusions as the systematic reviews: although the study found significant decreases in myalgia, arthralgia, and disc displacement, the authors concluded that more studies with similar designs are needed [19].
Preprosthethics: Preprosthetic surgery looks for ways to use supportive or retentive mechanisms to make prosthetic rehabilitation possible and thereby achieve a functional dentition and satisfying aesthetics [4]. In the edentulous patient, the resorption pattern of the jaws accentuates the inter-maxillary discrepancy, moving the mandible anteriorly and the maxilla posteriorly from a sagittal direction. This movement can lead to problems reconstructing the teeth and jaws with both fixed and removable prosthodontics [4].
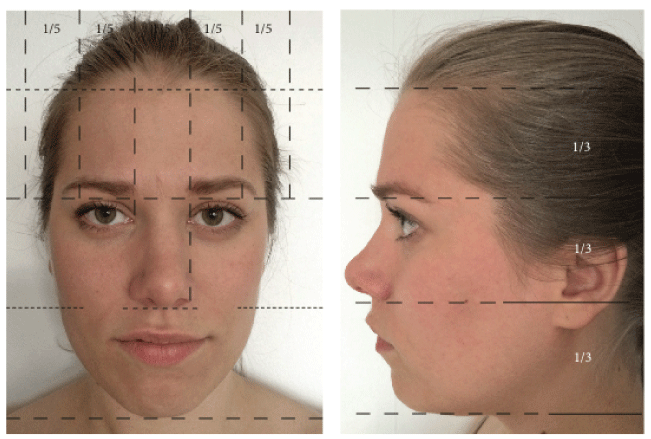
Aesthetics: Aesthetics is one of the main reasons patients choose orthognathic surgery [5,20,21]. Facial aesthetics require considering the importance of facial harmony and symmetry, anteriorly and sagittaly, using, for example, the rule of thirds and the rule of fifths (Figure 1). To reach the functional and aesthetic treatment goals, sliding genioplasty may be needed in addition to orthognathic surgery. Of the genioplasty patients, 90 - 98% are very satisfied with the results after surgery. Therefore, genioplasty should be considered in orthognathic surgery cases with high aesthetic demands [5,22].
.
Figure 1: Rule of thirds and fifths. Left picture, anterior view, demonstrates the rule of thirds and fifths. Right picture, sagittal view, demonstrates the rule of thirds. Pictures published with permission from the model.
View Figure 1
Because dental and facial aesthetics can significantly affect a patient's psychosocial condition and self-image, surgeons and orthodontists should include aesthetic considerations as part of their treatment strategies. During the treatment planning process with respect to aesthetics, surgeons and orthodontists should involve the patient at the same level as when determining clinical end points. For example, in certain cases, patients may be satisfied with achieving functionality and may be less concerned with improving aesthetics, so surgical treatment may not be needed. In these cases, treatment with orthodontic camouflage should be used instead of orthognathic surgery [21].
Although orthognathic surgery is a standard treatment in Sweden, statistics for frequency and indication for orthognathic surgery in Sweden are non-existent. Using a questionnaire survey sent to all oral and maxillofacial surgery (OMFS) clinics in Sweden, this study collected data on gender, age, frequency of patients, surgical techniques, indications, and whether patients underwent one- or two-jaw surgery for orthognathic surgery performed in 2011.
Material and Methods
To identify the current indications and the frequency for orthognathic surgery in Sweden in 2011, a questionnaire survey (Appendix) was sent to all (n = 50) OMFS clinics in Sweden. The clinics were identified on the official website for the Swedish Association of Oral and Maxillofacial Surgeons. The questionnaire asked the respondents to provide information regarding gender and age of the patients, surgical techniques, indications, whether patients had undergone surgery on one or both jaws, and frequency of the operations. The questionnaire was coded and if no response was received, a reminder letter was sent four weeks after the original letter. If still no response, a reminder was sent by e-mail and/or the clinic was contacted by telephone. Collected data were inputted into Microsoft Excel by going through the answers by code and by the way they were distributed in the survey questionnaire.
Results
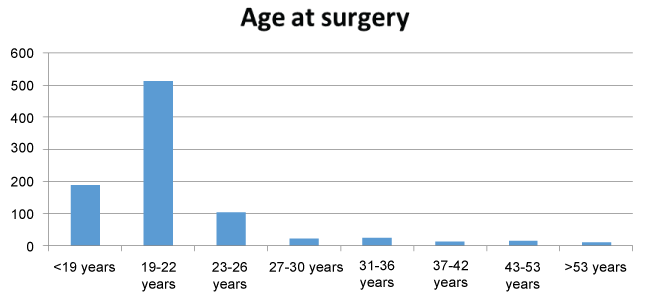
The survey questionnaire was sent to 50 OMFS clinics and 47 clinics responded. Two of the three non-responding clinics had closed by the time the study started and one did not respond. Of the 47 responding clinics, 23 (48.9%) performed 891 orthognathic surgeries in 2011 and these clinics were located in 16 of the 21 Swedish counties. The patients (56.2% were women and 43.8% were men) (Table 1A) represented every age range but most surgeries were performed on patients under 27 years, with most of these in the age range between 19 and 22 years (57.8%), followed by patients younger than 19 years (21.3%) and patients between 23 and 26 years (11.8%) (Figure 2A).
![]()
Table 1A: Table demonstrating frequency of; gender, single jaw/bi-maxillary surgery, main indication for surgery and dentofacial deformity aimed to correct. Answer frequency in parenthesis in the headline.
View Table 1A
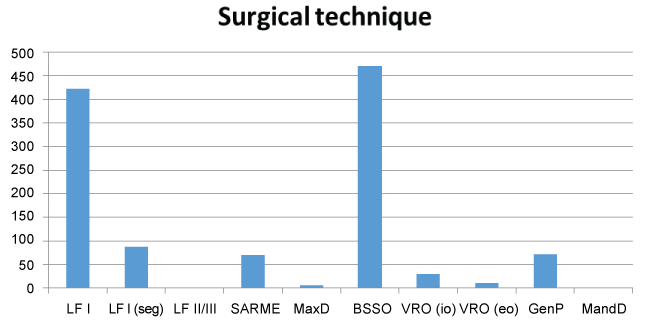
A slight majority of the surgeries were performed on a single jaw (55.2%) and bi-maxillary surgery was performed in 44.8% of the cases, although a large spread in distribution between the clinics and the counties was observed (Table 1B). The two largest counties in Sweden, Skåne and Stockholm, presented different result concerning single jaw and bi-maxillary surgery. The majority of surgical procedures in Stockholm county were bi-maxillary (62.7%), compared to Skåne county where the majority of surgical procedures were performed in one jaw (61.4%). In addition to traditional orthognathic surgery, genioplasty was performed in 8.8% of the cases. Respondents noted two procedures that were not alternatives on the survey: subapical mandibular osteotomy (two cases) and alloplastic chin augmentation (one case). For more detailed information concerning the specific surgical procedures (Figure 2B).
.
Figure 2B: Bar chart demonstrating the frequency regarding surgical procedures.
Explanations
LF 1 (1-piece) Le Fort 1 (1-piece)
LF 1 (seg.) Le Fort 1 (segmental)
LF 2/3 Le Fort 2/3
SARME Surgical assisted rapid maxillary expansion
MaxD Maxillary Distraction
BSSO Bilateral Sagittal Split Osteotomy
VRO(i) Intraoral Vertical Ramus Osteotomy
VRO(e) Extraoral Vertical Ramus Osteotomy
GenP Genioplasty
ManD Mandibular Distraction
View Figure 2B
The main indication for performing orthognathic surgery was functional (89.3%), followed by aesthetic/psychological (9.8%). Few of the surgeries were performed on pre-prosthetic indication (1.0%). Concerning the correction of the main jaw discrepancies, the most frequent discrepancy was of sagittal nature (46.9%). Correcting vertical jaw discrepancies was the main aim in 13.0% and correcting transversal jaw discrepancies was the main aim in 9.9% of the surgeries. In 30.2% of the cases, the aim was to correct a combination of different discrepancies.
In Sweden, the incidence of orthognathic surgery was 0.0094% in 2011 (calculation based on a population of 9,482,855 inhabitants in 2011 according to Statistics Sweden). There was a wide spread between the counties regarding incidence: the highest incidence was 0.0163% and the lowest incidence was 0.0053% (calculations based on the OMFS clinics' approximation of the population in their catchment area). For further detailed information of the incidence in each county (Table 1B).
![]()
Table 1B: Table demonstrating distribution of patients undergoing surgery, distribution of single jaw surgery/bi-maxillary surgery and incidence in Sweden and in each county separately. Incidence calculated on the clinics self-reported catchment area.
View Table 1B
Discussion
The aim of the study was to gather data on orthognathic surgery performed in Sweden 2011. No previous studies were found describing the incidence as well as the surgical techniques associated with orthognathic surgery in a specific country. As 47 of 50 clinics completed the survey, the data are representative for Sweden. However, as in all survey questionnaires, it is difficult to verify the accuracy of the respondents' answers and how the respondents interpreted the questions.
The gender distribution, with a small majority towards female patients, was expected and is described in several other studies [23]. A majority of the patients went through the surgery in the age range of 19 - 22. Facial growth is mostly finished around this age giving a stable skeletal situation [24]. When it comes to performing surgery in one or two jaws, the large distribution of results is interesting. It is well known that the risk of relapse increase with larger surgical movements. In a situation where a large magnitude of movement is needed in one jaw, the risk of relapse can be minimized if the movement is divided between both maxilla and the mandible. Yet, surgery in both jaws means two surgical interventions and a higher risk of neural and vascular complications. One possible explanation for this difference in surgical approach between counties in Sweden could be differences in clinical experience and custom at each OMFS clinic.
Our results show that functional indication by far is the main indication for performing orthognathic surgery in Sweden. Although aesthetics have been noted as one of the primary motivations for surgery for patients [5,20,21], only in 9.8% of the surgeries were aesthetics given as the main indication. In Sweden orthognathic surgery is made possible by federal financial support. The evaluation for the individual patient is based on treatment needs where cephalometric analysis and dental arch relationship are the basis for decisions on financial support. The result might also indicate discrepancies between the patient's expectations and the surgeon's aim, an incongruence that may lead to a result that does not fulfil the patient's expectations. For example, genioplasty, despite being a proven and safe procedure with high patient satisfaction, was performed less often than we expected. This result may have been due to miss-communication between surgeons and patients or by the fact that the question regarding the main indication in our survey could be interpreted in several ways, depending on the surgeons' perspectives and the patients' ability to accurately express their reasons for undergoing surgery.
The dentofacial deformity behind the surgical procedure was reported from 14 out of 23 counties. Bilateral sagittal split osteotomy (BSSO) was performed in 470 out of 891 procedures while intraoral or extra oral vertical ramusosteomy (IVRO/EVRO) was performed in 41 procedures. Both techniques are used to correct sagittal deformities and have their advantages and disadvantages [2,4]. The questionnaire did not include a report concerning if the sagittal deformity was a pre normal or post normal relation between the maxilla and mandible. One can only speculate but assume that half of the sagittal discrepancies were pre normal and half were post normal. In a situation with a prenormal occlusion the set back of the mandible can be performed with both BSSO and IVRO/EVRO. BSSO were performed ten times more than IVRO/EVRO which indicates that Swedish oral and maxillofacial surgeons prefer the BSSO technique. With BSSO there is no need for intermaxillary fixation and the technique can be used in situations with ramus elongation. On the other hand there is a risk for neurosensory disturbance of the inferior alveolar nerve [25].
Vertical dentofacial deformity was reported in 13 per cent of the patients. The maxillary surgical procedure with a Le Fort I osteotomy (LF I) with posterior impaction will give a possibility to close an anterior open bite [1]. In situations with a transversal deformity due to a narrow maxillary dental arch a segmental Le Fort I or a surgical assisted rapid maxillary expansion (SARME) can be performed [1,6]. Maxillary surgical procedures, Le Fort I/segmental Le Fort I/SARME, were performed in 580 patients. Transversal dentofacial deformities were found in ten per cent of the patients and combinations between different deformities in 30 per cent of the patients. For both deformities bimaxillary surgery can be indicated and explains why the number of surgical procedures exceeded the number of patients.
The incidence of orthognathic surgery in Sweden showed differences among the Swedish counties. This discrepancy could be due to the fact that some counties did not perform orthognathic surgery (five out of 21), but sent their patients to other counties that had larger clinics with greater resources for this type of treatment.
This questionnaire survey concerning orthognathic surgery in Sweden 2011 shows that age and gender distribution are consistent with the literature. The main indication for orthognathic surgery in Sweden is functional. In the literature the main indication is aesthetic and this difference can be due to the fact that if a Swedish patient reaches certain inclusion criteria, mostly based on cephalometric analysis together with dental arch relationship, the treatment is heavily subsidized by federal financial support. Since the aesthetic component isn't as easy to measure, the functional indications have a more dominant role in determining which patients receive financial support. Sagittal anomaly is the most common dentofacial deformity. The main surgical procedures for correction of dentofacial deformities are bilateral sagittal split osteotomy and Le Fort I osteotomy. Differences concerning one vs two jaw surgery could be explained by different surgical experiences and custom at each clinic. The fact that not all OMFS clinics perform orthognathic surgery and sends their patients to a larger clinic in a neighbouring county could explain the difference in incidence between counties in Sweden.
Acknowledgements
We would like to offer a special thanks to the participating Oral and Maxillofacial Surgery clinics, which have made this thesis possible.
Ethical Statements
In the questionnaire study no ethical dilemma was found because no delicate patient data were treated and the patient data had already been processed by the participating clinics so no patients could be identified.
References
-
JP R (2003) Essentials of Orthognathic Surgery. K O'Malley eI (edn) Quintessence publishing co.
-
Ghali GE, Sikes JW Jr (2000) Intraoral vertical ramus osteotomy as the preferred treatment for mandibular prognathism. J Oral Maxillofac surg 58: 313-315.
-
Andersson L KK-E, Progrel MA (2010) Oral and Maxillofacial Surgery. L Anderson K-EK, and MA Progrell (eds). West Sussex: Wiley-Blackwell.
-
Miloro MGG, Larsen P, Waite P (2004) Peterson's Principles of oral and maxillofacial surgery. M Miloro e (ed). Hamilton, Ontario: BC Decker Inc.
-
Chang EW, Lam SM, Karen M, Donlevy JL (2001) Sliding genioplasty for correction of chin abnormalities. Arch Facial Plast Surg 3: 8-15.
-
Koudstaal MJ, Poort LJ, van der Wal KG, Wolvius EB, Prahl-Andersen B, et al. (2005) Surgically assisted rapid maxillary expansion (SARME): a review of the literature. Int J Oral Maxillofac Surg 34: 709-714.
-
Proffit WR, Turvey TA, Phillips C (2007) The hierarchy of stability and predictability in orthognathic surgery with rigid fixation: an update and extension. Head Face Med 3: 21.
-
Magalhaes IB, Pereira LJ, Marques LS, Gameiro GH (2010) The influence of malocclusion on masticatory performance. A systematic review. Angle Orthod 80: 981-987.
-
Chua HD, Whitehill TL, Samman N, Cheung LK (2010) Maxillary distraction versus orthognathic surgery in cleft lip and palate patients: effects on speech and velopharyngeal function. Int J Oral Maxillofac Surg 39: 633-640.
-
Hassan T, Naini FB, Gill DS (2007) The effects of orthognathic surgery on speech: a review. J Oral Maxillofac Surg 65: 2536-2543.
-
JP O (2008) Management of Temporomandibular Disorders and Occlusion. J Dolan (ed) Lexington: Mosby Elsevier.
-
K P (2003) Correction of dentofacial deformities with orthognathic surgery: Oulu.
-
List T, Axelsson S (2010) Management of TMD: evidence from systematic reviews and meta-analyses. J Oral Rehabil 37: 430-451.
-
Magnusson T, Carlsson GE, Egermark I (1993) Changes in subjective symptoms of craniomandibular disorders in children and adolescents during a 10-year period. J Orofac Pain 7: 76-82.
-
Al-Riyami S, Cunningham SJ, Moles DR (2009) Orthognathic treatment and temporomandibular disorders: a systematic review. Part 2. Signs and symptoms and meta-analyses. Am J Orthod Dentofacial Orthop 136: 626 e1-16.
-
Fujimura K, Segami N, Sato J, Kanayama K, Nishimura M, Demura N (2004) Advantages of intraoral verticosagittal ramus osteotomy in skeletofacial deformity patients with temporomandibular joint disorders. J Oral Maxillofac Surg 62: 1246-1252.
-
Phillips C, Broder HL, Bennett ME (1997) Dentofacial disharmony: motivations for seeking treatment. Int J Adult Orthodon Orthognath Surg 12: 7-15.
-
Cascone P, Di Paolo C, Leonardi R, Pedulla E (2008) Temporomandibular disorders and orthognathic surgery. J Craniofac Surg 19: 687-692.
-
Abrahamsson C, Henrikson T, Nilner M, Sunzel B, Bondemark L, et al. (2013) TMD before and after correction of dentofacial deformities by orthodontic and orthognathic treatment. Int J Oral Maxillofac Surg 42: 752-758.
-
Elsalanty ME, Genecov DG, Genecov JS (2007) Functional and aesthetic endpoints in orthognathic surgery. J Craniofac Surg 18: 725-733.
-
Tucker MR (1995) Orthodontic camouflage versus orthognathic surgery in the treatment of mandibular deficiency J Oral Maxillofac Surg 53: 579-587.
-
Guyuron B, Raszewski RL (1990) A critical comparison of osteoplastic and alloplastic augmentation genioplasty. Aesthetic Plast Surg 14: 199-206.
-
Proffit WR, Jackson TH, Turvey TA (2013) Changes in the pattern of patients receiving surgical-orthodontic treatment. Am J Orthod Dentofacial Orthop 143: 793-798.
-
Birgit Thilander OR (1995) Introduction to Orthodontics. 2nd (edn): Gothia.
-
Bruckmoser E, Bulla M, Alacamlioglu Y, Steiner I, Watzke IM (2013) Factors influencing neurosensory disturbance after bilateral sagittal split osteotomy: retrospective analysis after 6 and 12 months. Oral Surg Oral Med Oral Pathol Oral Radiol 115: 473-482.